All published articles of this journal are available on ScienceDirect.
Ten-Year Mortality Trends and Natural Causes of Death in the Iraqi Kurdistan
Abstract
Background:
Mortality and causes of death are among the most important statistics used in assessing the effectiveness of a country’s health system. Several countries do not have information systems for collecting these data, and they must therefore be estimated from surveys.
Objective:
This study analyzes mortality data retrieved from official government databases in Iraqi Kurdistan to describe ten-year trends in natural causes of death.
Methods:
Data for natural causes of death, reported from 2009 to 2018, were extracted from the databases of the Registration Bureau of Births and Deaths and of the Forensic Medicine of the Province of Sulaymaniyah. A sample of 16,433 causes of death was analyzed.
Results:
Causes of death were coded according to the ICD-10 classification. Overall, cardiovascular diseases were the leading cause of mortality (52.6%), followed by neoplasms (17.7%), infectious and parasitic diseases (8.9%), and genitourinary diseases (6.3%). Neonatal conditions, congenital anomalies, and neurological conditions each accounted for less than 1% each. Numbers of natural deaths by cause and cause-specific mortality rates have been estimated for the entire Region of Iraqi Kurdistan. Comparisons with other sources suggest that there is a substantial amount of underreporting, especially in relation to deaths of infants and under-five children.
Conclusion:
Our findings confirm that the region is facing a burden of non-communicable diseases, coupled with high proportions of infectious diseases. However, the lack of effective vital statistics with combined under-reported data collection highlights the need for implementation of health monitoring systems. Advancements in generating high-quality data are essential in improving health and reducing preventable deaths. The establishment of a novel Health Information System is discussed.
1. INTRODUCTION
Timely and reliable health information is one of the six building blocks of any health system [1]. The transformation of raw data into evidence and health intelligence is paramount in guiding public health decision-makers in policy formulation and in allocating resources or mobilizing new ones to improve health and reduce inequalities [2]. There is a direct correlation between well-functioning civil registration and vital statistics systems and social and health development [3]. When they are complete and collected in a timely fashion, vital registrations are the main source for comprehensive monitoring of public health programmes and epidemiological surveillance. They are also the most reliable data source for tracking progress on the achievements of a large number of Sustainable Development Goals [4].
Among vital statistics, mortality (including causes of death) is one of the primary sources used to identify and monitor public health priorities. Ranking causes of death is a crucial factor in differentiating the magnitude of the various health problems [5]. However, despite the recognition of the importance of data for mortality and causes of death, considerable challenges still exist. Many countries are not using the vital statistics potential inherent in civil registration systems, either because registration systems are not implemented at scale or because not all information is recorded [6]. This is even more crucial in countries, like Iraq and its northern region, that have experienced armed conflicts, especially when those conflicts are recurrent and protracted, resulting in enormous challenges in ensuring the recovery of health systems [7]. In such a context, it becomes difficult to generate accurate data on even the most basic mortality indicators, and this applies even more in relation to the quality of cause-of-death statistics. The WHO technical meeting of 2014 stated that only 81 out of 194 countries can report high- or medium-quality data on deaths and causes of death [8]. As an interim measure, information is often estimated through surveys alone, which limits the possibility of conducting systematic evaluations and comprehensive assessments of vital statistics [9, 10].
Iraq is a country that during the 1970s had one of the most advanced health systems in the Middle East [11] but has experienced a progressive and steady decline since the late 1980s, due to recurrent international and communal armed conflicts and fighting [12], namely the Gulf wars of 1991 and 2003 and terrorist activities. In 2014, the rise of the so-called Islamic State (ISIS) and the occupation of vast regions of the country deeply impacted various dimensions of the country's healthcare assets, with health facilities being destroyed, medical staff being killed or forced to flee, and the health system routinely lacking data collection infrastructures [13]. With specific reference to data on mortality, despite Iraq being an upper-middle income country [14], there is still limited knowledge about the actual causes of deaths. According to the latest available WHO dataset, Iraqi death statistics “denote severe quality issues; data have low completeness and/or issues with cause-of-death assignment which likely affect estimated deaths by cause and time trends”. Therefore, the “use of estimates for program evaluation should be done with caution, as improvements in the vital registration system may affect the estimated trends in cause-specific mortality” [15]. Reinforcing health information systems, including those covering civil registration, is thus still a country priority [16].
In the Kurdistan Region of Iraq (KRI), routine data collection is not yet standardized across the governorates and computer technologies are not systematically and fully adopted. Raw data―generally collected on paper rather than electronically―are not readily available or are not in a format that is well suited to analysis or management [17]. The availability of sporadic/approximated/aggregated information reflects the situation of the country as a whole, with the KRI lacking in comprehensive, reliable statistics [18]. Information on vital statistics, which should contribute to developing the Region’s indicators, is available only through surveys’ estimations [19]. When considering mortality, only total numbers of estimated deaths are available, with no specific information about causes of death [20]. The development of an integrated health information system, that offers services at the appropriate level of care has been proposed as an ideal model to help the KRI in addressing many of these challenges, thus supporting policy maker in system management and health regulation compliance [21].
Because of the lack of information about causes of death in the Sulaymaniyah province, the primary aim of this study was to analyze and describe the distribution and frequencies of natural causes of death, offering preliminary information on the health situation and population needs. We, therefore, collected available data on causes of death officially recorded over a timespan of ten years in the city of Sulaymaniyah. Second, our research aimed to identify the principal shortcoming existing in health data collection, specifically in relation to causes of death, and to suggest hypotheses for improving the overall process.
2. MATERIALS & METHODS
2.1. Study Setting
The KRI was recognized by the Iraqi Constitution of 2005 as an autonomous region. The Kurdistan Regional Government (KRG) develops local health policies in coordination with the central government of Iraq. These policies are implemented by the Ministry of Health (MoH). Administratively, the region is divided into four Governorates: Duhok, Erbil, Sulaymaniyah, and Halabja.
In the KRI, health service delivery and health financing are a mix of public-private participation and investments. The Ministry of Health (MoH) of Regional Government is modelled on the basic organizational structure and system of the Iraqi MoH: public sector services are administered by the MoH in Erbil, which owns and operates a large network of primary and secondary health care facilities. These facilities are financed through general revenues and apply traditional line-item budgeting processes. The Ministry of Finance approves an annual allocation for MoH services, and all employees are salaried staff under civil service guidelines. The KRG decides health policies, which are implemented by the MoH, whereas long-term health planning is subjected to the responsibility of the Ministry of Planning (MoP) [22].
All Iraqi Health Directorates include Health and Vital Statistics Departments (HVSD), within the Health Planning Units. Health facilities send information to the HVSD on set dates, in the form of either CDs or hard-copy (paper) tables. There are also Registration Bureaus of Births and Deaths (RBBD) located in the various districts that are responsible for registering death events in their surrounding areas [23]. In Sulaymaniyah, the recording of deaths is based on the following procedures: health facilities send reports for natural causes of death to the RBBD for the Province, while deaths due to external events (i.e. accidents, murders, injuries) are recorded by the Province’s Forensic Medicine Department. According to Iraqi law [24], when a death occurs at home, the body should be transported to the hospital. It should not be buried before a death certificate is obtained and registered by the statistics office. The relatives of the deceased person should then send that certificate to the RBBD. However, this law is often not enforced. Therefore, deaths occurring at home are only rarely reported and, consequently, the cause of death will not be determined. The statistics offices of the RBBD produce monthly reports, which are sent to the Governorate’s Directorate of Health.
The RBBD records deaths reported either by hospitals or by relatives. When a person dies at a hospital, a death certificate is released containing certain information about the deceased person (age, gender) and the possible cause of death, ascertained by a medical doctor. Hospitals record all death events, even where the deceased is not from Sulaymaniyah.
2.2. Data Collection and Analysis
The statistics office in the Sulaymaniyah RBBD recorded a total number of 15,023 deaths in the period 2009-2018. The database included events reported by five hospitals in the city: the Shahid Dr. Hemn General Medical Teaching Hospital, the General Surgical Teaching Hospital, the Specialty Cardiac Hospital, the Maternity Hospital, and the Dr. Jamal Ahmed Rashid Paediatric Hospital.
In cases of sudden death, the natural cause can only be determined after an autopsy. Therefore, we also collected information on a total number of 1,410 deaths from natural causes entered in the database of the Forensic Medicine Departments in Sulaymaniyah in the same reference years.
In both databases, causes of death were not coded or classified but were written as text in either Arabic or Kurdish. There are cases of the same diagnosis being recorded using different terms or definitions. Therefore, each individual record had to be checked and coded according to the WHO International Classification of Diseases (ICD-10) [25]. The information was first collected according to cause and age group, and was then merged by year into a single database, which was finally analyzed.
Rates for causes of death were reported for the most common diseases, classified according to the WHO statistical guidelines [15]: cardiovascular diseases, neoplasms, infectious and parasitic diseases, genitourinary diseases, neurological conditions, neonatal conditions, congenital anomalies, and other causes. Information on the total number of accidents and injuries registered by the Forensic Medicine Departments was used to estimate the proportions of deaths due to external events.
Information was given as trends for overall rates, and then broken down by gender. Age-specific death frequencies were calculated. The proportions of deaths derived from the sample and the total number of natural deaths in Kurdistan [26] were used to estimate the number of deaths by cause and age-group for the whole region in 2018. Estimates are presented as absolute numbers and 95% Confidence Intervals (95% CI). Statistical analyses were performed using SPSS v.23.0 (IBM Corp., Armonk, NY, USA). Only anonymous information was extracted from the database. The study was registered to the Scientific Committee of the Statistics and Informatics Department at the University of Sulaymaniyah, which granted ethical approval.
3. RESULTS
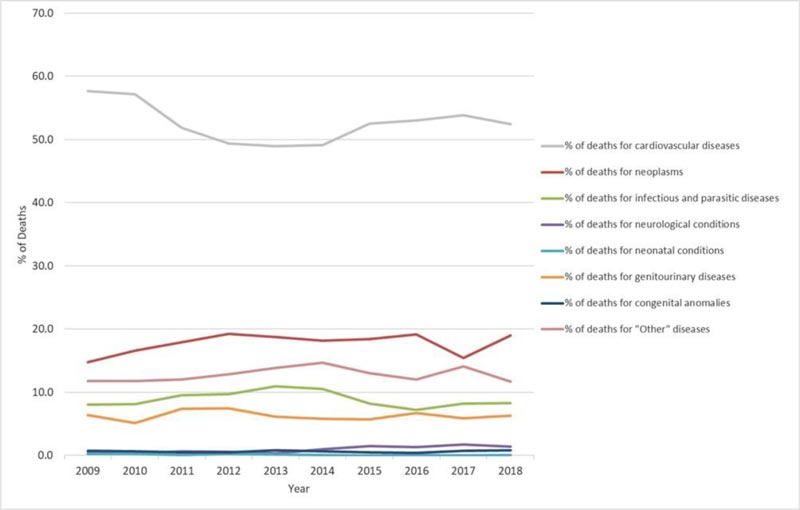
Over ten years (2009-2018), 16,433 deaths from natural causes were officially registered in Sulaymaniyah. Overall, cardiovascular diseases (CVDs) were the main cause of death, accounting for 52.6% of total events, followed by neoplasms (17.7%), infectious and parasitic diseases (8.9%), and genitourinary diseases (6.3%). Neonatal conditions, congenital anomalies and neurological conditions each accounted for less than 1%.
| Year | Deaths from cardiovascular diseases | Deaths from neoplasms | Deaths from infectious and parasitic diseases | Deaths from neurological conditions | Deaths from neonatal conditions | Deaths from genitourinary diseases | Deaths from congenital anomalies | Deaths from “other” diseases | Total numbers of deaths | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | n. | |
| 2009 | 753 | 57.6 | 193 | 14.8 | 105 | 8.1 | 5 | 0.4 | 3 | 0.2 | 83 | 6.4 | 10 | 0.8 | 154 | 11.8 | 1307 |
| 2010 | 800 | 57.2 | 232 | 16.6 | 113 | 8.1 | 5 | 0.4 | 3 | 0.2 | 72 | 5.1 | 9 | 0.6 | 165 | 11.8 | 1400 |
| 2011 | 710 | 51.8 | 246 | 17.9 | 130 | 9.5 | 9 | 0.7 | 1 | 0.1 | 101 | 7.4 | 7 | 0.5 | 165 | 12.1 | 1370 |
| 2012 | 792 | 49.4 | 309 | 19.3 | 155 | 9.7 | 9 | 0.6 | 4 | 0.2 | 120 | 7.5 | 8 | 0.5 | 206 | 12.9 | 1604 |
| 2013 | 736 | 49.0 | 282 | 18.8 | 165 | 11.0 | 5 | 0.3 | 2 | 0.1 | 92 | 6.1 | 13 | 0.9 | 208 | 13.8 | 1503 |
| 2014 | 821 | 49.1 | 304 | 18.2 | 176 | 10.5 | 16 | 1.0 | 1 | 0.1 | 97 | 5.8 | 11 | 0.7 | 246 | 14.7 | 1672 |
| 2015 | 1027 | 52.6 | 360 | 18.4 | 161 | 8.2 | 29 | 1.5 | 0 | 0.0 | 112 | 5.7 | 10 | 0.5 | 255 | 13.1 | 1954 |
| 2016 | 979 | 53.1 | 354 | 19.2 | 133 | 7.2 | 25 | 1.4 | 1 | 0.1 | 124 | 6.7 | 7 | 0.4 | 222 | 12.0 | 1845 |
| 2017 | 1019 | 53.9 | 292 | 15.4 | 156 | 8.2 | 33 | 1.7 | 0 | 0.0 | 111 | 5.9 | 14 | 0.7 | 267 | 14.1 | 1892 |
| 2018 | 989 | 52.4 | 358 | 19.0 | 157 | 8.3 | 26 | 1.4 | 1 | 0.1 | 119 | 6.3 | 15 | 0.8 | 221 | 11.7 | 1886 |
| Tot | 8627 | 52.6 | 2929 | 17.7 | 1452 | 8.9 | 163 | 0.9 | 16 | 0.0 | 1031 | 6.3 | 104 | 0.6 | 2110 | 12.8 | 16433 |
| Deaths from cardiovascular diseases | Deaths from neoplasms | Deaths from infectious and parasitic diseases | Deaths from neurological diseases | Deaths from neonatal diseases | Deaths from genitourinary diseases | Deaths from congenital diseases | Deaths from “other” deseases | Total | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | n. | % | ||
| Age group (0-5) | Tot. | 128 | 16.9 | 80 | 10.5 | 237 | 31.1 | 43 | 5.7 | 15 | 2.0 | 47 | 6.2 | 85 | 11.2 | 126 | 16.5 | 761 | 100.0 |
| Female | 54 | 7.1 | 39 | 5.1 | 93 | 12.2 | 17 | 2.2 | 6 | 0.8 | 21 | 2.8 | 44 | 5.8 | 60 | 7.8 | 333 | 43.8 | |
| Male | 75 | 9.8 | 41 | 5.4 | 144 | 18.9 | 26 | 3.4 | 9 | 1.2 | 26 | 3.4 | 40 | 5.3 | 66 | 8.7 | 427 | 56.1 | |
| Age group (6-20) | Tot. | 138 | 24.5 | 146 | 25.9 | 83 | 14.7 | 42 | 7.4 | 1 | 0.2 | 49 | 8.7 | 12 | 2.1 | 92 | 16.4 | 563 | 100.0 |
| Female | 53 | 9.4 | 56 | 9.9 | 49 | 8.7 | 13 | 2.2 | 1 | 0.2 | 19 | 3.4 | 4 | 0.7 | 44 | 7.9 | 239 | 42.5 | |
| Male | 85 | 15.1 | 90 | 16.0 | 34 | 6.0 | 29 | 5.2 | 0 | 0.0 | 30 | 5.3 | 8 | 1.4 | 48 | 8.5 | 324 | 57.5 | |
| Age group (21-60) | Tot. | 2395 | 47.7 | 1287 | 25.6 | 361 | 7.2 | 49 | 1.0 | 0 | 0.0 | 296 | 5.9 | 2 | 0.0 | 633 | 12.6 | 5023 | 100.0 |
| Female | 747 | 14.9 | 650 | 12.9 | 154 | 3.1 | 23 | 0.5 | 0 | 0.0 | 123 | 2.4 | 1 | 0.0 | 298 | 5.9 | 1995 | 39.7 | |
| Male | 1648 | 32.8 | 637 | 12.7 | 206 | 4.1 | 26 | 0.5 | 0 | 0.0 | 173 | 3.4 | 1 | 0.0 | 335 | 6.7 | 3026 | 60.3 | |
| Age group (60+) | Tot. | 5952 | 59.0 | 1417 | 14.0 | 770 | 7.6 | 29 | 0.3 | 0 | 0.0 | 639 | 6.3 | 5 | 0.0 | 1274 | 12.6 | 10085 | 100.0 |
| Female | 2506 | 24.8 | 495 | 4.9 | 335 | 3.3 | 11 | 0.1 | 0 | 0.0 | 264 | 2.6 | 3 | 0.0 | 585 | 5.8 | 4199 | 41.6 | |
| Male | 3446 | 34.2 | 922 | 9.1 | 435 | 4.3 | 18 | 0.2 | 0 | 0.0 | 375 | 3.7 | 2 | 0.0 | 689 | 6.8 | 5886 | 58.4 | |
Fig. (1) shows the death trends by cause, expressed in percentages, according to a year of registration. A slight reduction in CVDs has been observed over the years: from 57.6% in 2009 to 52.4% in 2018. Conversely, deaths caused by neoplasms increased from 14.8% in 2009 to 19% in 2018. A slight but progressive increase in neurological conditions (from 0.4% to 1.4%) was also observed. Infectious and parasitic diseases, which accounted for 8.1% in 2009, experienced a peak between the years 2013-2014 but returned to 8.3% in 2018. There were no significant changes recorded in the ratio of deaths for genitourinary diseases, congenital anomalies and neonatal conditions, or for other diseases.
To show the results of the analysis more effectively, absolute numbers of events by year, in addition to percentages, have been presented in Table 1.
Generally, mean age of death of 61.1 years (median: 63.5) was recorded for the period of the study as a whole, with an increasing trend noted over the years, from a mean age of 59.8 years (median: 62.8) in 2009 to 63.2 years (median: 64.3). When stratified by age, the highest frequency of events was recorded among the older adults (60-64, 65-69, 70-74 and 75-79 years). Even among adults, age of death increased gradually with age. Deaths among under-five children accounted for 4.5% of all events, while deaths among adolescents were, on the whole, less than 3% (Fig. 2).
The total sample was analyzed by age groups (0-5, 6-20, 21-60, over 60 years), with absolute numbers and percentages presented in Table 2. Under-five children mainly died from infectious and parasitic diseases (31.1%), with the number of deaths due to neonatal diseases being relatively small (2%). The leading causes of mortality in the 6-20 year group were neoplasms (25.9%), followed by CVDs (24.5%), infectious and parasitic diseases (14.7%), and neurological diseases (7.4%). In adults (21-60 years), CVDs (47.7%) and neoplasms (25.6%) accounted for nearly 75% of all deaths, with higher percentages for CVDs among males. Cardiovascular diseases were also the main cause of death among individuals aged over-60, accounting for more than half of events (59%) especially among males, followed by neoplasms (14%).
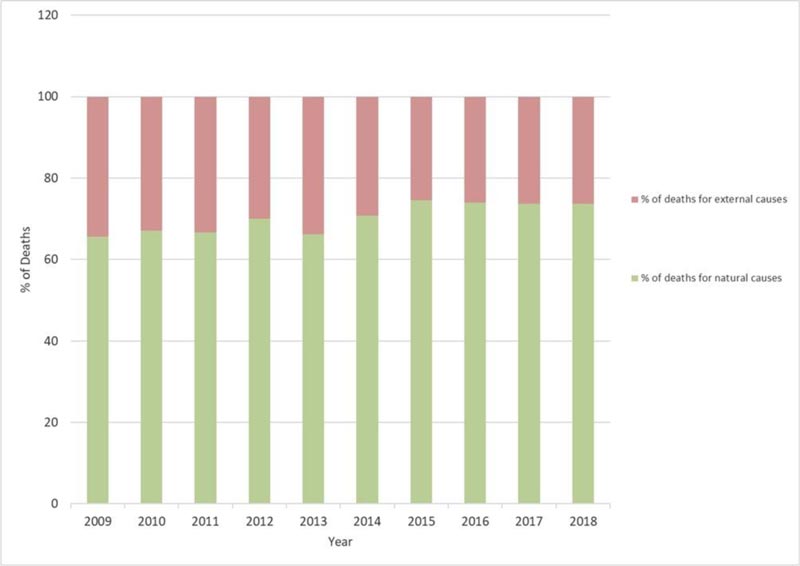
To show the total share of deaths in the province―i.e. natural and external causes- numbers of deaths caused by intentional and unintentional injuries registered during the same period were also included. When natural and external causes of death by year were combined, external events accounted for about one-third of all deaths registered in the city. The share of deaths from external events decreased over the years, from 34.4% in 2009 to 26.4% in 2018. Conversely, the proportion of deaths from natural causes increased, from 65.6% in 2009 to 73.6% in 2018 (Fig. 3).
In addition, based on our proportions, we forecast estimated numbers of the main relevant categories of death from natural causes for the Kurdistan Region. To do so, we used the number of deaths in the Region for 2018, the last available official estimate, i.e. 22,645 deaths [26]. Therefore, for the entire KRI, we estimated 8,776 deaths 2018 from CVDs (95%CI: 8,643-8,909), 2,953 (95%CI: 2,851-3,055) from neoplasms, 1,484 (95%CI: 1,409-1,561) from infectious diseases, and 1,051 (95%CI: 986-1,115) from genitourinary diseases. Consequently, considering an estimated 2018 mid-year population of 5,453,000, the estimated overall cause-specific mortality rate for CVDs was 160.9/100,000 residents, for neoplasms this was 54.2/100,000, for infections, it was 27.2/100,000, and for genitourinary diseases, it was 19.3/100,000. The overall crude mortality rate was 4.2/1,000 population.

In relation to age-group, we estimated, 123 (95% CI: 99-147) deaths from CVDs, 126 (95% CI: 103-149) from neoplasms, and 51 (95% CI: 15-66) from infectious diseases in the 6-20 year group; in adults, 2,332 (95% CI: 2,243-2,421) deaths from CVDs, 1,244 (95% CI: 1,175-1,313) from neoplasms, 267 (95% CI: 233-299) from infectious diseases, and 281 (95% CI: 247-315) from genitourinary diseases. In the over-60, 6,232 (95% CI: 6,103-6,361) deaths from CVDs, 1,501 (95% CI: 1,425-1,577) from neoplasms, 630 (95% CI: 579-681) from infectious diseases, and 692 (95% CI: 639-745) from genitourinary diseases.
4. DISCUSSION
Iraq is suffering from what has been defined as the “single most critical failure of development over the past 30 years” [3], namely the lack of data systems for the collection of data on births, diseases, and causes of death. This situation is due mainly to the limited availability of health-related and epidemiological information, with available data usually being of uncertain quality. Despite the availability of several studies focusing on the impact of conflicts and wars on the public health system of Iraq and of Iraqi Kurdistan [27-29], studies about mortality trends and causes of natural deaths are still limited. In 2012, the WHO requested a rapid assessment of the Iraqi health system. The evaluation showed an inadequately functioning system, especially in relation to the completeness of birth and death registration and cause of death data. Several areas to be improved were identified, and total computerization of the system at various levels was recommended [30].
As for Iraq as a whole, there is limited documented knowledge in the KRI about the current health situation of the population. Information is not routinely collected and used for health planning, and the impact of the care provided is not efficiently monitored or evaluated [31, 32]. These limitations make it impossible to carry out the full range of analyses that politicians and managers would need to guide health policies or monitor health services and/or results [33].
To our knowledge, in recent years, there is only one study focusing on an analysis of mortality in the KRI [34], specifically in the city of Erbil. Therefore, we conducted a similar analysis on the causes of death in the city of Sulaymaniyah. Our findings show that cardiovascular diseases were the main cause of death over the period of ten years, followed by neoplasms, infectious and parasitic diseases and genitourinary diseases. Conversely, infectious and parasitic diseases remained stable over time, being the leading cause of mortality only among under-five children. The general increasing trend in the mean age of death, and the growing share of deaths due to non-communicable diseases [35], combined with high proportions of infectious diseases, confirms a trend observed in other Middle Eastern countries [36].
In terms of differences between the genders, more deaths at younger ages were generally recorded among males, especially in adults and elderly individuals.
We compared our results with the WHO data for Iraq and neighbouring Iran and Saudi Arabia [15], and with a study conducted in Erbil Province [34]. CVDs were confirmed as the leading cause of natural deaths by all sources, despite being higher in our study (38% Iraq, 48% Iran, 44.6% Saudi Arabia, 36% Erbil). Neoplasms were the second leading cause of natural deaths, and our findings were in line with those for Iraq (17%) and Iran (18%), but higher than Erbil (10%) and Saudi Arabia (12%). Infectious and parasitic diseases were double those recorded for Iraq (4%), and more than three times the values found for Iran (3%) and Saudi Arabia (2%). This information was not available for Erbil. Genitourinary diseases almost doubled the numbers calculated for Iraq (3%), Erbil (4%), Iran (3%), but less than those for Saudi Arabia (8%).
On the other hand, congenital anomalies seemed to be under-reported compared to Iraq (4%), Erbil (5%) and Saudi Arabia (3%), although the numbers were similar to those for Iran (1%), while rates for neonatal conditions were significantly lower than all the other sources. Our findings could be a sign of substantial under-registration of deaths among under-five children. In fact, Awqati et al. stated that―in 2002―only 15% of deaths of children aged less than five years under-five were actually registered in Iraq’s vital statistics registration, especially when death occurred at home [37].
When we supplemented our findings with the data on deaths due to external events recorded over the same period of study, we determined that external causes accounted for about one third of total deaths. This proportion was in agreement with overall data for Iraq (28%) and Erbil (29%). While numbers for deaths caused by external events were quite stable, total records of natural deaths fluctuated within the evaluation period, with percentages rising in recent years. This might be due primarily to an under-recording of deaths by the RBBD statistics offices, especially when these occur at home. Furthermore, it is well-documented that, as a result of wars and conflicts in several countries in the Eastern Mediterranean Region, as well as in Iraq, health statistics are often not fully available or reliable, since routine monitoring systems for mortality are not implemented on an appropriate scale [38].
When we compared the estimated cause-specific mortality rate with those for Iraq as for whole [15], which is characterized by an age distribution pattern similar to the KRI, our rates were lower for infections (35.5/100,000 for Iraq) while being quite similar for neoplasms (56.9/100,000) and higher for CVDs (138.7/100,000) and genitourinary diseases (12.9/100,000).
Our analysis confirmed some shortcomings in the efficiency and reliability of the system, such as the completeness of the registration process. In particular, when referring to infant and under-five mortality, our findings highlight the deficiencies in the information reported. To our knowledge, no studies based on officially registered data on causes of child mortality have been yet conducted in the country and epidemiological facts are therefore still needed [37].
Our study points to the need for additional standardized tools to assess causes of death in Iraq, as well as a central system for epidemiological surveillance that is able to combine data from different sources, thus allowing facilities―such as RBBD and Forensic Medicine Departments―to communicate and integrate data. Reliable information on diseases and deaths in the population should be the foundation of any health system, so that health policies developed on the basis of poor evidence can be avoided [39].
In the Eastern Mediterranean Region, the WHO is already working on key initiatives for implementing regional civil registration and vital statistics systems, focusing specifically on a timely and complete registrations of deaths and accurate certifications of the causes of death [40]. Moreover, the WHO supports regional initiatives to develop national health information systems, suggesting the use of platforms that are already available, such as the District Health Information Software 2 (DHIS-2) package [41]. The WHO is also supporting the adoption of the International Classification of Diseases (ICD) as the basic standard for data reporting on mortality and morbidity [42]. In line with this approach, the University of Rome Tor Vergata (Italy) and the KRI Ministry of Health ―with the financial support of the Italian Agency for Development and Cooperation―have initiated a cooperation project to establish the first Health Information System in the KRI, aimed at gathering data on health determinants, births, deaths and health service performance. This project was commenced in 2015 through a pilot phase [43] and now includes about 60 health centres and hospitals, which routinely record health data using ICD-10. The Health Information System is starting to provide high-quality data, which are needed for national and sub-national planning, policy implementation and monitoring of health outcomes and services. The inclusion of data on registration of deaths e-health information system is set up is a priority of the programme, to be implemented in the nearest future. Health data monitoring for the population and better knowledge about changes in disease burden will be paramount in allocating human and financial resources [44].
CONCLUSION
Knowledge and interpretation of vital statistics, including information on natural causes of death, is essential health intelligence in determining the most frequent, serious, treatable or preventable conditions threatening the health of a population. Investing in the implementation of an epidemiological surveillance system as a routine public health practice, coupled with the development of a culture of using data for decision-making, will be paramount in obtaining reliable information on causes of death and thus overcoming the limitations for analysis associated with an absence of reliable data.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The study has been granted ethics approval from the Scientific Committee of the Statistics and Informatics Department at the University of Sulaymaniyah, Iraq (reference number 13, on the date 14/6/2020).
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Not applicable.
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article will be made available by the authors, without undue reservation, to any qualified researcher.
FUNDING
This research was not granted any specific fund.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
SSO, AHH, QSA collected data; EGL and BFB designed the study; DGD and MS performed analysis; SSO, BFB, EGL commented on the results; SSO, AHH, QSA, and BFB made and maintained contact with local health authorities; EGL, MS and DGD conceptualized and wrote the paper’s drafts; all the authors significantly contributed to reviewing and revising the paper.
Our thanks are due to the personnel of the Registration Bureau and Forensic Medicine Department, who were actively and devotedly committed to sharing data. Special thanks also go to the General Director of Sulaymaniyah Health Directorate.


