All published articles of this journal are available on ScienceDirect.
Patients' Barriers to Effective Pain Management: A Correlational Study
Abstract
Background
Dealing with pain management is an issue that greatly impacts the well-being and health outcomes of individuals living with chronic pain. This research aimed to explore how patient-related obstacles affect the pain management practices of nurses, in public Jordanian hospitals.
Methods
The study involved a selection of 98 registered nurses who completed a self-administered questionnaire to assess patient-related barriers and pain management practices. The collected data was analyzed using SPSS and PLS SEM to test hypotheses.
Results
It was discovered that patient-related obstacles had an impact on pain assessment as well as both pharmacological and non-pharmacological interventions. Additionally, the study revealed that nurses displayed moderate level of pain management practices. The R2 values showed that patient related barriers explained a substantial amount of variance in pain management practices.
Discussion
This investigation underscored the importance of addressing patient related barriers when it comes to managing patients’ pain. It was recommended that nurses take on a role in empowering patients to overcome their obstacles and enhance their own pain management techniques. Furthermore, there is a need for research into other factors influencing pain management practices. The study acknowledged limitations within its methodology.
Conclusion
By demonstrating how patient-related barriers impact the way nurses handle patient pain, this study contributes insights to the existing literature on effective pain management. The study offered recommendations and suggestions for improving nursing practice and conducting future research on pain management.
1. INTRODUCTION
Just imagine what it would be like to live with pain that your healthcare providers are not able to properly understand or address. How would you feel in such a situation? What actions would you take? Sadly, this is the reality for patients who encounter different obstacles when it comes to managing their pain. These barriers, including a lack of awareness of concerns about addiction and cultural beliefs hinder their ability to effectively communicate and cope with their pain. As a result, their quality of life and overall outcomes suffer well. Undertreated pain can be life-threatening [1, 2]. It influences the patients’ safety [3] by affecting many human systems, such as the cardiovascular system [4], the respiratory system [5, 6], the gastrointestinal system [7], the endocrine system [8], the immune system [8, 9], and the musculoskeletal system [10]. Also, this problem occurs in many countries around the world caused by financial crises [11]. The pain management deficiency costs countries millions of dollars per annum, as a consequence of patient’s readmission, visiting outpatient, visiting emergency departments, and increased hospitalization period [12]. So, there is an urgent need to assess the pain management practices and evaluate its determinants.
Pain management is a process that consists of providing interventions to relieve the patients’ pain [13, 14] and assessing the patients’ pain by using the appropriate pain assessment tool before and after the intervention [14, 15].
Pain management interventions are classified into pharmacological and non-pharmacological interventions. The pharmacological intervention is defined as administering the appropriate and effective analgesic drug to relieve the patient’s pain; it includes administering opioid analgesic, non-opioid analgesic, and adjuvant [16]. Conversely, the non-pharmacological intervention is defined as using any method designed to relieve the patients’ pain without using the medication administration, such as stimulating sight and hearing senses to decrease unpleasant feelings through music or video [17, 18]. Moreover, patients’ education and guidance can contribute to relieving the patients’ pain by decreasing anxiety, such as teaching them breathing techniques, muscle relaxation, and correct posture [19, 20]. Furthermore, using exercises, art therapy, cold compresses, heat pads, contemplation, imagination, relaxation, and distraction may also work [21-23].
A number of researches have been conducted in the past to reveal deficiency in pharmacological pain management with emphasis on the adherence to analgesic prescription. For instance, some nurses were found to give analgesics only when the patient demanded it rather than as scheduled [24, 25]. This raises ethical concerns because this practice is not in conformity with the universally accepted patient rights which include the right to relieve pain as a fundamental human right [26–28]. Furthermore, although 91% of the patients complained of pain on the first postoperative day, analgesia was given less frequently than is recommended [21, 29]. Another research showed that less than a quarter of the post-hip-fracture patients took scheduled analgesics at regular intervals, even though the prescription was made by their physicians [30].
This under-treatment also points to shortcomings in the implementation of the planned treatments and at the same time raises concern about the ethical conduct of healthcare practitioners in managing patients’ pain. This may indicate a lack of professionalism thus putting patients through avoidable discomfort and may also discourage patients from seeking the services of healthcare practitioners. These ethical problems need to be solved to enhance the effectiveness of pain control and to develop the concept of centrality of the patient in the healthcare setting.
On the other hand, other studies revealed that pain management deficiency appears mainly in non-pharmacological intervention, that not more than six percent of nurses used a non-pharmacological method [31]. Other study results revealed a severe deficiency in the non-pharmacological pain management by observing the pain management practices of 52 Australian nurses [25]. In addition, a study conducted in America by auditing the patients’ files found an unexpected finding; it showed that 90 percent of the non-pharmacological intervention to relieve the patients’ pain was not documented. In a similar vein [24, 32, 33], stated that health care providers rarely use non-pharmacological intervention. In brief, many studies have shown that many patients suffer from an unrelieved pain as a result of the nurses’ interventional deficiency in pain management [34-38] because they wrongly believe that the patient should experience slight discomfort [39, 40] or tolerate the pain until it becomes unbearable before taking pain relief [41].
There are many advantages to using the non-pharmacological intervention. It can improve the patients’ feelings about their health status, reducing their pain to a tolerable level [42, 43], and decreasing the risk of drug interaction or adverse effect [42, 44]. But using the two methods of interventions at the same time is more effective than controlling the pain by using one method [31, 45] and it leads to reduced mortality and morbidity among patients [46].
Pain management deficiency is not limited to the intervention to relieve the patients’ pain but also the assessment, as indicated by the literature. According to [47-49], deficiency in pain reassessment occurs after the analgesic drugs are administered to the patient suffering from pain. The deficiency within the assessment and reassessment phases clearly appeared in a study by [50], who reviewed the medical records of 117 patients to assess compliance with the Joint Commission's pain management standards. Unfortunately, they found that the assessment of the patients’ pain and the reassessment after the procedures or treatments were not documented for most patients.
Over the past two decades, the researchers only focused on assessing the impact of nurses’ barriers (i.e. knowledge, attitudes, self-efficacy) on their practices regarding pain management (i.e. Assessment, pharmaco- logical and non-pharmacological intervention) and they found significant results [38, 51-57]. Unfortunately, they fail to consider the impact of the patient's refusal to report their pain, especially if there are misconceptions about how to manage pain. (i.e. patients barrier). Also, previous studies failed to make a comparison between the levels of pain management stages (i.e. Assessment, pharmaco- logical and non-pharmacological intervention). Thus, the current study aimed to fill the literature gaps assessing the relationship between patients’ barriers regarding pain management and their pain management practices. Moreover, it will make a comparison between the levels of pain management stages. The findings of this study will help improve the nurses' practices (assessing and controlling patients' pain) in healthcare settings, consequently enhancing the quality of patients' lives.
2. METHODOLOGY
2.1. The Participants
To achieve our study objectives, we needed a representative sample size that would ensure adequate statistical power and minimize sampling error. To determine the required sample size, we utilized G*Power 3.1 software, which calculates the sample size based on the desired effect size, alpha level, and power level [58]. According to the software recommendation, a minimum of 166 registered nurses were necessary for our study.
To select participants from the population of registered nurses working in large and medium-sized general government hospitals in Jordan, we employed a random sampling technique. Due to the limited availability of email addresses among registered nurses in Jordan and restrictions imposed by the Ministry of Health on sharing such information, we opted for a paper-based questionnaire distribution method. Additionally, the relatively small geographical area of Jordan and the limited number of target hospitals further supported this approach.
The selected participants received a paper questionnaire along with a cover letter that explained the purpose and significance of the study, ensured confi- dentiality and anonymity of responses, and emphasized participation. Additionally, we maintained communication with the participants through phone calls to their workplaces to remind them to complete and return the questionnaire.
Out of the 166 questionnaires distributed, we received 98 completed questionnaires, resulting in a response rate of 59%. According to [59], response rates between 50-70% are generally considered satisfactory in social and educational research, as they strike a balance between practical feasibility and the need to limit sampling bias. Therefore, our 59% response rate meets this criterion and can be considered satisfactory for this type of study.
2.2. The Survey
The researchers used a self-administered questionnaire to collect information from participants. Before answering the questions, participants were informed about the purpose of the survey and provided written consent. The questionnaire consisted of five sections: patient-related barriers to pain control, personal details, pain assessment, pharmacological intervention, and non-pharmacological intervention to control pain. The personal details section included questions about gender, age, education level, work history, experience with pain, and training in pain management. In the section on patient-related barriers, participants were asked to indicate their level of agreement or disagreement with 16 items about challenges they face in managing their patient’s pain.
The 19 items in the pain assessment section examined how frequently participants utilized various techniques to gauge the intensity of pain in their patients. Nonpharmacological and pharmacological intervention were the two subsections of the section on pain interventions. There were 13 items in the non- pharmacological intervention component that assessed how frequently participants employed different non-drug pain relief methods on their patients. 9 items in the questionnaire on pharmacological interventions assessed how frequently individuals utilized various classes of medications to ease their patients' pain. Every question in the sections on pain evaluation and pain intervention used a 7-point Likert scale, with 1 being “Never” and 7 being “Constantly.” The items in the section on patient-related barriers likewise employed a 7-point Likert scale, with 1 being the strongest disagreement and 7 being the strongest agreement.
Ethical approval for this study was obtained from the Ministry of Health’s Ethics Committee, allowing data collection across all government hospitals operating under the Jordanian Ministry of Health.
2.3. Data Analysis Software
The researchers prepared the data for analysis by assigning codes to the responses. They utilized a software program named SPSS version 20 to compute statistics of the data, such as frequency of answers, average scores, and variability. These statistics are referred to as descriptive data since they provide an overview of the sample’s characteristics. Moreover, we employed another software called SmartPLS version 3.0 to explore relationships between the study variables [60]. This program allowed researchers to estimate the extent to which each variable influenced or was influenced by another variable and test whether these influences were statistically significant or not. These estimations are termed path coefficients as they illustrate the paths of influence between variables. To determine if a path coefficient was significant or not the researchers established a criterion; the probability of obtaining that coefficient by chance had to be less than 5%. Thirobability is known as a significant level which is represented by p-value. In this study, a significance level of p value < 0.05 was chosen for all tests conducted by the researchers.
2.4. Analysis Process
Data analysis began with descriptive analysis, using means and standard deviations, to examine latent variables measured on a 7-point Likert scale, grouped as low, moderate, or high. To investigate relationships between variables, Partial Least Squares Structural Equation Modeling [PLS-SEM] was applied in two stages: measurement model assessment and structural model assessment. The measurement model evaluated reliability, internal consistency, convergent validity, and discriminant validity. The structural model then analyzed path coefficients, R-squared values, effect sizes, and predictive relevance to confirm the robustness and predictive power of the model, ensuring alignment with the research objectives.
2.4.1. Descriptive Analysis of Latent Variables
We conducted a descriptive analysis of the variables in our model by looking at their means and standard deviations. In this study we measured all the variables using a Likert scale ranging from 1 to 7 where a score of 7 represents agreement and a score of 1 represents disagreement. To make it easier for analysis we categorized the Seven Point Scale into three groups: low, moderate, and high. Generally, scores below 2 are considered low (calculated as 7 divided by 7 plus the value of 1) scores, above 6 are considered high (calculated as the value of 7 minus 7 divided by 7) and moderate scores fall between low and high [14].
2.4.2. PLS-SEM Path Model Analysis
In this study a two-step approach was employed to assess and present the PLS SEM path model depicted in Fig. (1). The initial step focused on evaluating the measurement model, which gauges the extent to which the observed variables accurately capture the variables within the model. The subsequent step involved scrutinizing the structural model, which investigates the connections between these variables [61,62].
2.5. Measurement Model Assessment
When evaluating a measurement model, it is essential to consider four factors. Firstly, we have reliability, which refers to the consistency of the measurement scale. A reliable scale should produce similar results when administered to individuals multiple times, ensuring that it consistently measures the same thing each time it is used. Another aspect is internal consistency reliability which measures how effectively the items, on a scale are correlated with one another. A scale with consistency and reliability ensures that all items effectively measure the concept and do not assess unrelated constructs. Convergent validity examines how well a measurement scale correlates with measures of the concept assessing whether it aligns with measures that should theoretically measure the same underlying construct. Lastly, there's validity, which evaluates the degree of correlation, between a measurement scale and measures of concepts. It ensures that the measurement scale specifically focuses on the intended construct and is not unduly influenced by factors. Together these four characteristics contribute to ensuring an accurate assessment of a measurement model's rigor and precision. [61, 62].
We assessed the reliability of each item based on the loadings of each construct [61]. Items, with loadings below 0.40 or above 0.7 were then removed in accordance with [63] to ensure a level of composite reliability [.70 or higher]. To evaluate the internal consistency reliability, we calculated the composite reliability and removed items with the lowest outer loadings based on this evaluation [64,65]. Following this we conducted a convergence validity test as suggested by [66], which measured the average variation extracted for each latent construct. For every latent construct, it is necessary to have an average variation extracted of 0.50 or more [67]. We also determined the discriminant validity by comparing the square roots of average variance extracted with correlations among latent constructs. As a guideline the square root of the average variance extracted should be greater than the correlation between latent constructs [66].
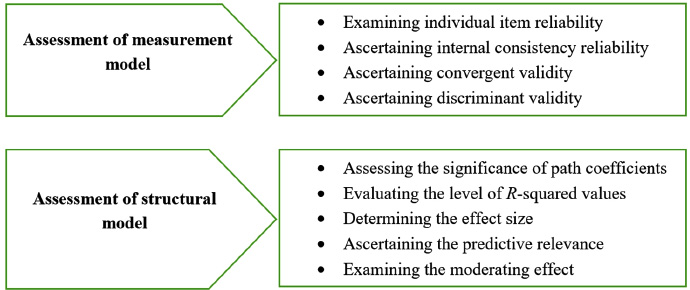
Two-step process for assessing PLS path models.
Source: [62]
2.6. Structural Model Assessment:
To evaluate the structural model, we examined the significance of path coefficients, R-squared values (R2), effect size (f2), and predictive relevance (Q2) [62]. Path coefficients were calculated through a bootstrapping method with 5,000 samples to test the significance of relationships among variables [63]. Path coefficients with p-values below 0.05 were considered statistically significant.
The R-squared [R2] measure, commonly used by statisticians, indicates the extent to which the variation in a dependent variable can be explained by one or more predictor variables [68]. In PLS-SEM, R2 classified as substantial [0.26], moderate [0.13], and weak [0.02] for the model’s variables [60]. Additionally, the effect size [f2] was assessed to examine the impact of each independent latent variable on a dependent latent variable, based on changes in the R2 value [67]. Effect size is considered weak at 0.02, medium at 0.15, and strong at 0.35 [69].
Predictive relevance refers to how a least squares structural equation model (PLS SEM) can accurately predict new data. It serves as a means of assessing the goodness of fit of a PLS SEM model [70]. To evaluate relevance one approach is to employ a technique called blindfolding. In blindfolding a portion of the data is intentionally left out from the model. Then this omitted data is predicted using the model. If the model can successfully predict the omitted data, it demonstrates relevance.
Another method to assess relevance involves calculating validated redundancy values. These values are derived by dividing the data into two sets: one, for training purposes and another for testing purposes. The training set is used to train the model, which is subsequently employed to predict values in the test set. The cross validated redundancy values (cv-red Q2) indicate how well these predicted values correlate with the values in the test set. Research models that yield cross validated redundancy values more than 0 are considered to possess predictive relevance. Conversely models with cross validated redundancy values, below 0 are deemed not to exhibit relevance [71].
3. RESULTS
3.1. Respondent Demographics
A total of 98 nurses participated in the survey. It was found that 58% of them were female. The average age of the nurses based on the information provided was 30 years old. As per the survey results 47% of the nurses (46 respondents) had an experience ranging from one to five years. Among all respondents, 7% (seven individuals) held master’s degrees while 93% (91 individuals) possessed bachelor’s degrees. Interestingly it was observed that a significant majority of nurses (78%)—76 in total—had never undergone any training program for pain management. Moreover, an astonishing 84% reported experiencing pain at some point in their lives. For demographic information about the participants please refer to Table 1 below.
3.2. Descriptive Analysis of Latent Variables
The mean scores for the study variables, which are listed in Table 2, range from 3.5096 to 5.1992. The assessment variable had a mean of 5.1992 and a standard deviation of 1.20693 indicating that respondents are moderately involved in pain assessment. Additionally, the table shows that non-pharmacological interventions have a mean of 5.1177 with a deviation of 1.16425 suggesting a moderate level of implementation. Furthermore, pharmacological interventions were perceived as moderate (mean = 5.1088 standard deviation = 1.08632). Lastly, patient related barriers were reported at a moderate level (mean =3.5096 standard deviation = 0.91783).
| Respondents Characteristic | Categories | Frequency |
|---|---|---|
| Sex | Male | 41 |
| Female | 57 | |
| Education | Baccalaureate degree | 91 |
| Master’s degree | 7 | |
| Total experiences | One to five years | 46 |
| Six to ten years | 32 | |
| Eleven to fifteen years | 14 | |
| Sixteen to twenty years | 6 | |
| Training | Yes | 22 |
| No | 76 | |
| Severe pain experience | Yes | 84 |
| No | 14 | |
| Age | Mean | 29.88 |
| Standard deviation | 4.806 |
| Study Variables | Number of Items | Mean | Standard Deviation |
|---|---|---|---|
| Assessment | 19 | 5.1992 | 1.20693 |
| Non-pharmacological | 13 | 5.1177 | 1.16425 |
| Pharmacological | 9 | 5.1088 | 1.08632 |
| Patients related barriers | 16 | 3.5096 | 0.91783 |
| Construct | Cronbach’s Alpha | Composite Reliability | AVE |
|---|---|---|---|
| Assessment | 0.971 | 0.974 | 0.661 |
| Non-pharmacological | 0.954 | 0.960 | 0.647 |
| Patients related barriers | 0.905 | 0.920 | 0.513 |
| Pharmacological | 0.916 | 0.931 | 0.600 |
3.3. Evaluation of the PLS-SEM Path Model
3.3.1. Measurement Model Assessment
The measurement model exhibited strong reliability and validity. Cronbach's alpha values exceeded 0.90 for all constructs (Assessment, Non-pharmacological, Patient related barriers, and Pharmacological), indicating high internal consistency. Composite reliability values were above 0.70, and AVE values exceeded 0.50, demonstrating adequate reliability and convergent validity. These results provide a solid foundation for further analysis (see Table 3 & Fig. 2).
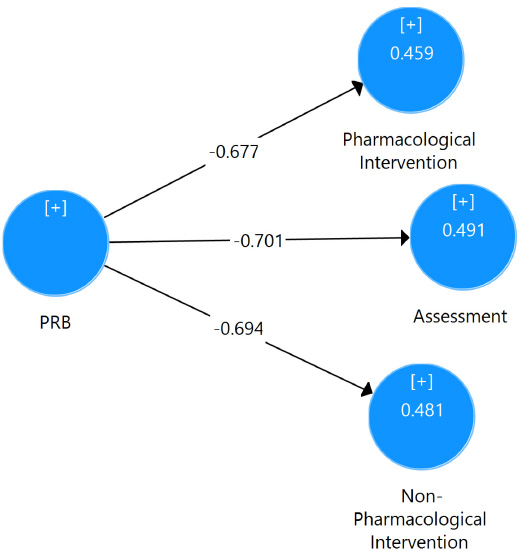
Measurement model.
3.4. Analysing the Structural Model
3.4.1. The Significant of Path Coefficient
Based on Hypothesis 1 we anticipated a negative correlation between patient related barriers and pain assessment. The study’s findings (Table 4 & Fig. 3) confirm that these variables are indeed negatively related (β = -0.701 t = 12.193, p < 0.01) supporting Hypothesis 1. Furthermore, patient-related barriers were found to have a negative correlation with non-pharmacological interventions (β = -0.694, t = 10.590 p < 0.01) thus validating Hypothesis 2. Hypothesis 3 predicted a significant and negative relationship between patient related barriers and pharmacological interventions. The results demonstrate that this relationship is indeed significant and negative (β = -0.677 t = 10.344 p < 0.01) providing support, for the hypothesis. The analysis of path coefficients, for the model is presented in Table 4 and Fig. (3).
3.4.2. Evaluating the Level of R-Squared [R2] Value
In our study, we found significant R2 values for each dependent variable, indicating substantial variance explained by the model. Specifically, the R2 for pharmacological intervention was 0.459, accounting for nearly 46% of its variability. The R2 value for assessing patient pain levels was 0.491, explaining approximately 49% of the variance, while the R2 of 0.481 for non-pharmacological intervention indicated that about 48% of its variability was explained. These findings highlight the model's effectiveness in capturing significant variance across all dependent variables.
| Hypotheses | Relation | Beta | SD | T-Value | p-Value | Findings |
|---|---|---|---|---|---|---|
| H1 | Patient-related barriers & pain assessment | -0.701 | 0.057 | 12.193 | 0.000 | Sig. at the 0.01 level |
| H2 | Patient related barriers & non-pharmacological interventions | -0.694 | 0.066 | 10.590 | 0.000 | Sig. at the 0.01 level |
| H3 | Patient related barriers & pharmacological interventions | -0.677 | 0.065 | 10.344 | 0.000 | Sig. at the 0.01 level |
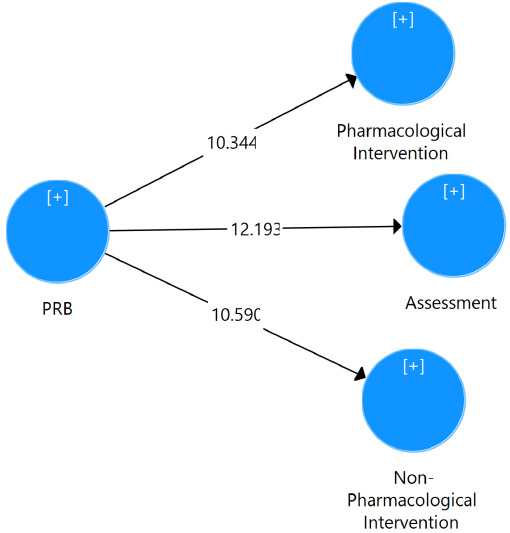
Structural model.
| Dependent Variables | F-squared | Effect |
|---|---|---|
| Assessment | 0.965 | Strong |
| Non-pharmacological | 0.928 | Strong |
| Pharmacological | 0.847 | Strong |
| Dependent Variables | SSO | SSE | 1-SSE/SSO [cv-red Q2] |
|---|---|---|---|
| Assessment | 1862 | 1282.126 | 0.311 |
| Non-pharmacological | 1274 | 895.174 | 0.297 |
| Pharmacological | 882 | 653.787 | 0.259 |
3.4.3. Assessment of Effect Size [f2]
According to the data presented in Table 5, it is evident that the independent variable, which pertains to barriers faced by patients has a high impact on all dependent variables; assessment, non-pharmacological interventions and pharmacological interventions. This suggests that patients’ barriers play a role in predicting these three factors.
3.4.4. Assessment of Predictive Relevance [Q2]
Our study found that the blindfolding procedure yielded results above zero, indicating that our model has predictive relevance. This is further supported by redundancy values from cross-validation, all exceeding zero [62, 67]. As shown in Table 6, the assessment had an SSO of 1862 and an SSE of 1282.126, resulting in a cv-red Q2 value of 0.311. For non-pharmacological interventions, the SSO was 1274 and the SSE was 895.174, yielding a cv-red Q2 of 0.297. For pharmacological interventions, the SSO was 882 and the SSE was 653.787, leading to a cv-red Q2 of 0.259. These results confirm the model's predictive capability in clinical practice.
4. DISCUSSION
This study found that the participants had moderate levels of assessment, non-pharmacological interventions, pharmacological interventions, and patient-related barriers, which is similar to what other studies have found [56, 72].
The Patient related barriers and Pain Assessment were highly significant and negative related (β = -0.701, t = 12.193, p< 0.01). Unfortunately, previous studies ignored to assess the effect of patients’ barriers. The findings of this study are consistent with those of previous Jordanian studies on the effects of nurse-related barriers [38, 56, 73] as well as in other countries [51, 74]. A negative relationship was also found between patient-related barriers and non-pharmacological interventions (β = -0.694, t = 10.590, p < 0.01). This result is also consistent with previous studies that assessed the nurses-related barriers [55, 76]. Finally, the study results showed a significant negative relationship between patient-related barriers and pharmacological interventions (β = -0.677, t = 10.344, p < 0.01), this result in line with earlier Jordanian studies among different population [38, 56, 74].
Some of the obstacles that may be encountered include patients’ lack of knowledge, fear of becoming addicted, and cultural norms and beliefs. To overcome these challenges, nurses must work with physicians, pharmacists, and mental health professionals to develop a multifaceted pain management plan. This involves teaching patients about pain control, listening to their concerns and giving them a chance to make some decisions. By breaking these barriers through a team approach, nurses will be able to enhance pain management practices thus enhancing patient’s pain.
However, one aspect to consider is that this study has limitations primarily because it involved a small sample size since the recruitment was limited to public hospitals, which may restrict the generalizability of the findings. The study utilized self-report measures which may introduce bias or errors in data collection. Furthermore, the study design was cross-sectional limiting causal inferences or longitudinal analysis. Future studies should aim to include more diverse samples while utilizing measures as well, as longitudinal or experimental designs to validate and expand upon these findings.
Ultimately the barriers associated with patients accounted for less than half of the variability in each stage of pain management. Therefore, it is crucial for research in this area to concentrate on evaluating the impact of factors such as organizational policies and guidelines.
CONCLUSION
This research contributes to the current understanding of pain management by investigating how patient related obstacles impact the way nurses handle pain. The findings indicate that patient related barriers have an effect on pain assessment as well as the use of both medication and non-medication approaches. The study also offers suggestions for enhancing nursing practices and guiding research in the field of pain management.
AUTHOR'S CONTRIBUTION
H.S.: Visualization; K.I.: Investigation; B.A.: Draft manuscript. All authors reviewed the results and approved the final version of the manuscript.
ABBREVIATION
| PLS-SEM | = Partial Least Squares Structural Equation Modeling |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The Ethical Committee of Jordanian Ministry of Health, Jordan has approved this particular study approval no. AB-15359.
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
AVAILABILITY OF DATA AND MATERIAL
All the data and supporting information is provided within the article.
ACKNOWLEDGEMENTS
Declared none.


