All published articles of this journal are available on ScienceDirect.
Samoby (Safe Mom And Baby): An Android-based Application Increasing The Success Of Childbirth Planning And Complication Prevention Program
Abstract
Introduction
The childbirth planning and complication prevention programme in the Sukorame Health Center area has faced challenges in implementation. Many pregnant women have not displayed the childbirth planning and complication prevention program stickers on their doors or windows, preventing the local community recognizing that a pregnant women lives in the area. The stickers are often incomplete. To maximize the success of the program an Android-based application called Samoby (Save Mom and Baby) was introduced. This study aimed to determine the effect of the Samoby (mom and baby safe) application on improving the childbirth planning and complication prevention program in the Sukorame Health Center area, Kediri City.
Method
This study used a pre-experimental design using a one-group pre-test and post-test approach, without a comparison group. Data were collected through questionnaires and observation sheets . The population was 50 pregnant women from the Sukorame Health Center area, Kediri, determined by a simple random sampling technique. Data were analyzed using the Wilcoxon Match Pairs Test, obtaining a p-value of 0.001.
Result
The study demonstrated that the android-based application had proven to be more effective in increasing the success of the childbirth planning and complication prevention program. The Samoby application allowed midwives could monitor the the completion and display of program stickers, leading to better compliance..
Conclusion
Samoby, an Android-based application, could increase the success of the childbirth planning and complication prevention program by 38% in the Sukorame Health Center Area, Kediri. However, t its use is limited to pregnant women with Android smartphones. The app could be further enhanced by adding new, more comprehensive features. Therefore, further research should explore the impact of Samoby with larger sample sizes and a control group.
1. INTRODUCTION
Preliminary interviews with a midwive from the Sukorame Health Center area revealed that the childbirth planning and complication prevention program has not been functioning effectively . Not all pregnant women display The program stickers on their doors and windows, which prevents neighbors from recognizing that a pregnant woman lives in the area. Additionally, many of the stickers have not been filled out completely. A study found that only 27.5% of pregnant women had adequately prepared for childbirth and potential complications [1]. Similarly, another study in the Farta District of Ethiopia reported that only 34% of women had implemented labor and complication preparation measures [2].
Proper preparation for labor and complications is crucial in preventing delays in emergency care for pregnant and birthing women. A study highlighted the SMGL (Saving Mothers Giving Life) program, which was designed to reduce maternal mortality by addressing three critical delays. The first delay involves factors that affect the decision to seek delivery care at a health facility. These factors include lack of birth planning, unawareness of pregnancy danger signs, negative perceptions of healthcare facilities, and financial or geographical barriers [3].
Several factors can influence how well pregnant women prepare for labor and potential complications. One study identified monthly income as a significant factor associated with labor preparation and complication prevention [4]. Other study have highlighted that a history of obstetric complications, knowledge of danger signs, positive attitudes, early antenatal care visits living in urban areas, employment in government roles, and good economic standing, all contribute to better labor preparations [5]. These findings align with another study that found family-oriented education programs for pregnant women improved birth readiness [6]. Additional factors such as education, age, and religion have also been linked to labor and complication preparation [7]. Women who have given birth before (multiparous) are more likely than the first-time mothers (primiparous) to properly prepare for labor and potential complications [8].
Marco and IK developed an Android application aimed at cost-effective prenatal care. This app offered tailored prenatal education based on patient's risk factors and allowed for monitoring of vital signs and weight between visits. However, the study concluded that the use of mobile prenatal care applications did not reduce the frequency of prenatal visits or affect patient satisfaction [9]. Dalton, JA created Health-e Babies, an Android app for pregnant women attending tertiary hospitals in low socioeconomic communities. The app provided pregnancy-related information aimed to increase confidence, and reduce anxiety. Despite its goals, 76% of the participants did not complete the trial highlighting the challenges of implementing pregnancy apps in socially disadvantaged communities. The study found that social and mental health factors, financial constraints, and technological capabilities influenced women's engagement with mobile apps [10].
Gupta developed an Android application called SEWA, which aimed to identify high-risk pregnancies and record antenatal care (ANC) visits, referrals, and birth outcomes for a year. The app led to a notable increase in the identification of high-risk pregnancies from 3.5% to 27.9%. Additionally, 53% of high-risk pregnancies were recorded through the app via text message. The study concluded that the SEWA app is a viable and sustainable solution for identifying high-risk pregnancies and reducing maternal mortality [11]. Sanghvi designed an Android-based electronic health worker decision support tool called epartogram. After midwives were trained to use the application, the epartogram was shown to assist in labor decisions, such as encouraging ambulation, fluid intake and addresing abnormal fetal welfare measurements. Its use was linked to improved adherence to labor care recommendations and reduction in adverse fetal outcomes. Continued development of the epartogram to incorporate new clinical rules from 2018 WHO recommendations on intrapartum care is expected to further enhance labor monitoring and quality care in healthcare system [12].
While these previous studies on Android-based applications for pregnant women have focused on prenatal education, pregnancy monitoring, identifying high-risk pregnancies, tracking vital signs and weight, recording antenatal care visits, increasing pregnant women’s confidence and reducing anxiety none have addressed monitoring childbirth preparation or complication readiness program. Childbirth preparation and complication readiness are crucial for reducing maternal and infant mortality. Despite the importance of these programs, no research has yet explored the development of an Android-based application specifically designed to monitor labor preparation and readiness for complications in pregnant women.
Proper preparation for labor and complications can ensure a safe delivery, leading to healthy mothers, and babies. regular antenatal care visits with midwives play a key role in this process. One study emphasized that early preparation for birth and complication is an essential strategy for ensuring safe deliveries [13].
Given this background, the researcher is interested in conducting a study titled “The Effect of Using the Samoby (Safe Mom And Baby) Android-Based Application on the Childbirth Planning and Complication Prevention Program in the Sukorame Health Center Work Area, Kediri.”
This study aimed to analyze the impact of using the SAMOBY application on the success of the childbirth planning and complication prevention program. By using Samoby, midwives can monitor the program more efficiently They no longer need to visit each pregnant woman’s home to check whether the program stickers have been displayed properly. If a pregnant woman has not uploaded a photo of the completed sticker, which should be affixed to her front door or window, the midwives can send a reminder through the app’s chat feature.
The key differences between this study and previous ones are:
(1) The Samoby application is designed to be simpler and easier for pregnant women to use
(2) The app includes a chat feature, allowing pregnant women to consult with midwives about their pregnancy.
(3) The app has a feature for uploading photos of the completed childbirth planning and complication prevention stickers which are to be displayed on the window or front door of the house
2. METHOD
This study is a quantitative study that uses a pre-experimental design with a one group pre-test and post-test approach, without a comparison group.
2.1. Respondent
The population for this study included all pregnant women within the Sukorame Health Center work area. A sample of 50 participants was selected using a simple random sampling. Inclusion criteria required that respondents be pregnant women at any stage of pregnancy, and they possess an Android smartphone with at least 500 MB of RAM. Exclusion criteria included pregnant women who were unable to operate android applications or were unwilling to participate in the study. All pregnant women who met the inclusion criteria were willing to be respondents. There are no other significant characteristics of the respondents.
2.2. Confounding Variables
One of the confounding variables in this research is the economic status of the participants. Pregnant women who cannot afford an Android smartphone, are unable to access the Samoby application, which requires a device with a minimum of 500 MB of RAM. To overcome this, pregnant women who do not own an Android smartphone, can borrow one from a family member or neighbor.
2.3. Data Collection
Samoby is a product of advancements in information technology. The application, which is 10.12 MB in size, can be downloaded from a designated website. Samoby contains several features, including: educational material, health data, consultation and a feature for uploading photos of the birth planning and complication prevention stickers. The pregnant woman’s profile in the app includes personal data. The material feature provides educational content on The childbirth planning and complication prevention program. The health feature records the mother's pregnancy condition, which is updated after each pregnancy check-up. The consultation feature allows users to communicate with a midwife. A key feature that contributes to the success of the childbirth planning program is the ability to upload photos of the stickers.
The sticker used in the birth planning and complications prevention program contain essential information, such as: the mother's name, estimated delivery date, birth attendant, place of birth, birth companion, transportation and a prospective blood donor. When the sticker is fully completed, the pregnant woman is considered prepared for childbirth and possible complications. Respondents were gathered at the Bandar Lor village hall, with only the participants and the researchers present. On the first day, respondents completed a pre-test questionnaire an observation sheet to assess their adherence to the birth planning and complication prevention program. No prior trials were conducted. The respondents were then given an explanation about the Samoby application and The childbirth planning and complication prevention program For the next two weeks, their progress in completing the birth planning and complication prevention stickers was monitored through the Samoby application. After 2 weeks, participants filled out a post-test questionnaire to evaluate the outcomes.
3. RESULT
The Wilcoxon matched-pairs test was used to analyze the effect of the Samoby Android-based application on the success of the childbirth planning and complication prevention program. The SPSS analysis revealed a p-value of 0.001, indicating that the use of Samoby had a statistically significant effect on the success of the program Figs. (1-3).
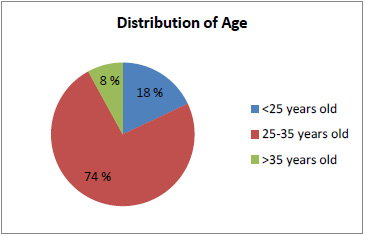
Age distribution diagram of respondents.
Of the 50 respondents, 9 people (18 %) were <25 years old, 37 people (74 %) were 25-35 years old, and 4 people (8 %) were over 35 years old.
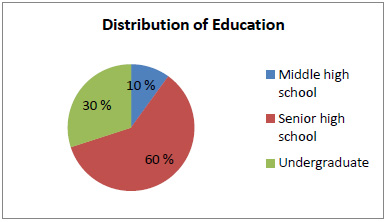
Distribution diagram of respondents' education.
Regarding educational background, 5 people (10 %) had a junior high school education, 30 people (60 %) had a senior high school education, and 15 people (30 %) held undergraduate degrees.
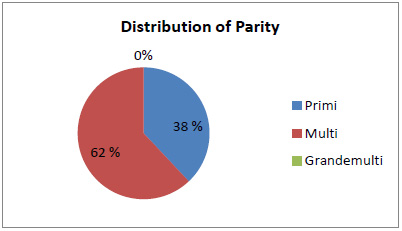
Distribution diagram of respondents' parity.
In term of parity, 19 people (38 %) with primigravida, while 31 people (62 %) were multigravida.
Table 1 shows that, before receiving education through Samoby 31 respondents (62%) demonstrated good implementation of the childbirth planning and complication prevention program while the remaining 19 respondents (38%) showed poor implementation.
| Category | Frequency | Percentage |
|---|---|---|
| Good | 31 | 62 |
| Less | 19 | 38 |
| Total | 50 | 100 |
From the result of Table 2, it was found that the success of the childbirth planning and complication prevention program after being given education using the Samoby application increased.
From the results of Table 3, after being given education using the Samoby android-based application, eight items from the the childbirth planning and complication prevention program had reached 100%, while two points reached 92%.
| Category | Frequency | Percentage |
|---|---|---|
| Good | 50 | 100 |
| Less | 0 | 0 |
| Total | 50 | 100 |
4. DISCUSSION
The childbirth planning and complication prevention program before education with heSamoby App Before receiving education through the Samoby application, 31 respondents (62%) had successfully implemented the childbirth planning and complication prevention program . While 62% were classified as ‘good’, none of them had fully completed all points in the program These points include having the childbirth planning and complication prevention sticker, affixing the sticker, and completely filling in sticker. Missing items included the estimated date of labor, plans for birth helper, birth attendant, transportation, potential blood donors, delivery funds, and post-childbirth contraceptive plans . This is because pregnant women do not fully understand the benefits of The childbirth planning and complication prevention program. A study explained that 41.9% of pregnant women in Nigeria have labor and complication readiness [14]. Another study also explained that only 11.4% and 7.6% of pregnant women had prepared for labor and complications in Kenya and Tanzania [15].
| S.No. | Items in the Childbirth Planning and Complication Prevention Program | Before Samoby | After Samoby |
|---|---|---|---|
| 1 | Having the childbirth planning and complication prevention program sticker | 74% | 100% |
| 2 | Sticking tthe childbirth planning and complication prevention program sticker | 62% | 100% |
| 3 | Estimated of labor | 64% | 100% |
| 4 | Plan for birth helper | 64% | 100% |
| 5 | Plan for birth place | 64% | 100% |
| 6 | Plan for birth attendant | 62% | 100% |
| 7 | Plan for transportation | 58% | 100% |
| 8 | Plan for potential blood donor | 0% | 92% |
| 9 | Labor cost | 72% | 100% |
| 10 | Plan for contraceptive after delivery | 22% | 92% |
Only 74% of pregnant women had received the childbirth planning and complication prevention program stickers, while the rest did not. According to the district midwife, all pregnant women have received stickers, along with MCH (Maternal and Child Health) books. So if there are pregnant women claimed they did not have the stickers, it is likely that the sticker fell off or was lost, possibly due to lack of understanding of their significance. Midwives should explain the benefits of the childbirth planning and complication prevention program stickers and how to fill them out to pregnant women earlier during the first antenatal care visit. Filling in all the items indicates that the mother is ready to face labor and complications. A study explained that monitoring labor preparation should be done routinely in the clinic to help maintain and improve labor preparation and complications [16].
There were 62% of pregnant women had attached the childbirth planning and complication prevention programme stickers, while 38% had not . Those who di not attach the stickers cited reasons such as not knowing that the stickers had to be attached or feeling embarrassed to stick the stickers outside the house. The stickers should be placed outside the house, either on the door the window, so that neighbours are aware there is a pregnant woman in the house. Some of the obstacles in the implementation of the program are a lack of understanding among community, families, and mothers about its purpose and benefits, insufficient information from health workers, irregular pregnancy check-ups and non-optimal implementation of pregnancy classes. Information about childbirth planning and complication prevention program can be provided by midwives during Antenatal care visits or pregnancy classes. A study explained that pregnant women who attended pregnancy classes had better preparation for childbirth and its complications [17].
One of the key points in the program points is about “the Estimated Day of Birth” which 64% of pregnant women have filled in, and 36% of them have not filled in This gap was due to pregnant women being unaware that stickers must be filled in and not knowing how to fill in. When giving the stickers, midwives should explain how to fill them in. It is good to involve husbands in the process. A study explained that the participation of husbands in pregnancy checks increases the awareness of pregnant women in preparation for childbirth and complications [18].
Another point is “the plan for birth helper”. Sixty four percent of pregnant women had filled in this section, while the remaining had not. This was because pregnant women had not yet decided who would assist them during their birth . Pregnant women can choose a skilled birth helper according to their preferences. A study explained that birth preparation and complication preparedness can improve access to profesional obstetric care [19]. Another study explained that women who have enough money to give birth are 10.87 times more likely to seek skilled birth helper. Women should be allowed to choose the gender of their preferred professional birth helper when giving birth [20].
The point “planned place of delivery”, there are 64% of pregnant women had filled it and the rest were not, this is because pregnant women have not consulted with their husbands and families to determine where the place of delivery will be. Most of them cannot determine the place of delivery by themselves. A study explained that decision-making about where to give birth is mostly taken by the husband/family [21].
In the point “Plan for a birth companion”, 62% of respondents had filled in and the rest had not. It was because they did not know who will be their birth companion in the future. Birth companions are the closest people to the mother who will accompany her during childbirth. Birth companions play a big role in providing support and comfort during childbirth. A study explained that allowing pregnant women to have a companion at the time of delivery can be a cost-effective intervention to improve the quality of care, especially in primiparous mothers [22].
The point “Plan for the transportation used if at any time referral is needed” only 58% had been filled in, while the rest had not . This was because pregnant women did not know what vehicle to use, with many only having access to a motorcycle. A study explained that 80.8% of pregnant women has not prepared a transportation used in an emergency [23]. Husbands/families should provide transportation for their wives if referral is necessary. A study explained that the husband's participation in birth and complication preparedness about transportation planning for referral of pregnant women to the hospital needs to be considered to achieve better partner participation [24].
At the point of “Plan for potential blood donors,” all respondents (100%) had not filled in, all pregnant women did not have a plan for potential blood donors because they were unaware family members who have the same blood type. The availability of potential blood donors for pregnant women is very important, in preparation if the mother has bleeding during and after labor. A study explained that <50% of pregnant women who have prepared a potential blood donor have a more mature preparation [25]. Another study explained that 8.18% pregnant women already have prospective blood donors in preparation for emergencies in labor [26]. This is also in accordance with a study which explained that 26.5% of the causes of maternal deaths are postpartum hemorrhage [27].
On the point “Preparation of funds for delivery”, 72% of pregnant women already had funds for delivery, and 44% had not prepared funds for delivery (still in the process of collecting funds). A study explains that early antenatal care is a mediating factor for delivery at a health facility. Women with higher education and no financial concerns are more likely to have early antenatal care and ensure smooth delivery. Therefore, it is important to design and implement policies for socially and economically disadvantaged women [28].
In the “contraceptive plan” section, only 22% of pregnant women had filled it in, and the rest did not have a contraceptive plan after delivery. Contraceptive plans are very important to plan during pregnancy. Midwives should provide counseling about various contraceptives when pregnant women do pregnancy checks. Pregnant women should have determined the contraceptive method that will be used after giving birth. A study explained that pregnant women who were given counseling about contraception at least once, 38.5% used modern contraception after childbirth, besides that there were 5 factors that influenced mothers to use modern contraception after childbirth, namely: receiving counseling on contraception during pregnancy check-ups, satisfaction with antenatal care services, counseling on labor and complications, breastfeeding guidance, and postpartum care education [29].
4.1. The Childbirth Planning and C prevention Program after Education with the Samoby App
The success of the childbirth planning and complication prevention programme after being given education on the use of the samoby app was in the good category (100%). However, four respondents had not filled in the program sticker completely. Items that had not been filled in were plans for potential blood donors, funding plans, and contraceptive plans after childbirth. It was due to the respondents’ lack of cooperation, as they were busy taking care of children so they did not have time to open the application. Application monitoring was carried out after pregnant women received education about the childbirth planning and complication prevention programme using the samoby application. Despite continuous monitoring by the researchers, including reminders via the app's chat feature, three respondents failed to respond before the study's deadline..
After the education through Samoby app, all pregnant women already have a plan regarding the vehicle which will be used during the delivery process. All pregnant women answered that they would use a private vehicle. Almost all pregnant women mentioned that their personal vehicle was a motorcycle, but they were willing to borrow a car from their relatives if there was an emergency and a referral to the hospital was needed. If a pregnant woman needs to be referred to the hospital, the transportation is ready. This can prevent delays in getting adequate treatment at the referral hospital. A study explained that 61.8% of women in the High Priority Districts of Uttar Pradesh India have readiness for labor and complications both in terms of facilities and transportation. Optimizing effective counseling during antenatal check-ups can improve childbirth preparedness [30].
All pregnant women already had already planned for the cost delivery. Almost all pregnant women answered using health insurance. A study explained that Health Insurance is important in preparing for childbirth and complications [31]. There were also some pregnant women who prepared money independently for labor costs, but there were still pregnant women who were still collecting labor costs. It is important to prepare funds for childbirth from earlier pregnancy, with the availability of funds, pregnant women can choose skilled birth attendants according to their want. A study explained that preparation for birth and complications increases timely access to professional maternal and infant services [32].
All pregnant women already have a plan for who will be their companion during labor. Almost all respondents want to be accompanied by a husband in their side. The presence of a labor companion plays a big role in providing peace and comfort to the laboring mother. Labor companions can also assist mothers in caring for themselves and their babies. A study explains that the presence of a birth companion is associated with several beneficial practices and reduced interventions in labor care [33]. Some respondents chose to be accompanied by their mothers, or other family members such as younger siblings because their husbands worked out of town. A study explains that 47% of birth attendants are family members of pregnant women. Pregnant women without a birth attendant are more likely to experience physical violence, non-consensual medical procedures, and poor communication [34].
Most respondents already had also planned for potential blood donor. Only 4 out of 50 respondents did not have a plan for potential blood donors. The busyness of family members caused them not to have time to check their blood type. Prospective blood donors for labor are crucial to prepare. If the mother have bleeding during labor and needs a blood donor, then the donors should be ready to donate blood, so there is no delay which can result in maternal death. A study explained that 48.5% of pregnant women were prepared for childbirth and complications, factors associated with preparation for childbirth and complications are: preparation of blood donors, identification of skilled birth helper and counseling to husbands and families [35].
After the childbirth planning and complication prevention program counseling using the samoby application, most respondents already had a contraceptive plan that will be used after delivery. Almost all pregnant women mentioned the contraceptives they will us are IUDs, implants, and injections. However, four respondents had not arranged the donors was because the respondents were busy taking care of children so they did not have time to fill in the sticker and open the samoby application to fill in the contraceptive plan data. A contraceptive plan after childbirth is very important to be prepared during pregnancy so that the mother can determine the right contraceptive for her. A study explained that midwives should provide counseling about contraception and contraindications before delivery to facilitate the mother's decision about the most appropriate contraception [36]. Planning for contraception before delivery is appropriate to prevent early pregnancy after delivery, and contraception can be provided while the woman is in labor and still being treated at the birthing clinic or hospital. Another study explains that women who want effective contraception should already have a contraceptive method before discharge from the hospital, this is to minimize barriers to contraceptive method provision [37].
4.2. Effect of Samoby Application on Improving the Childbirth Planning and Complication Prevention Program
Based on the results of the Wilcoxon test, a p-value of 0.001 was obtained, indicating significanteffect of using the Samoby application on increasing the childbirth planning and complication prevention program. Samoby is an Android-based mobile application designed to monitor childbirth planning and complication prevention program monitoring tool. This application can be found on the website with size of 10.12 MB. Nowdays, the use of communication tools such as smartphones and computers has become an inseparable part of life. Services provided by smartphones can be used to make it easier for clients to obtain information about health. Health education information provided using smartphone services can improve preventive health services. This will greatly benefit health workers, as the wide reach of the internet will allow more individuals to obtain health information. A study stated that portable devices such as smartphones have become ubiquitous. The concept of e-health utilizes telephones, computers, internet and related applications to improve the healthcare industry [38]. Another study explained that with the development of smartphone technology accompanied by the expansion of fifth-generation mobile networks will play a key role in the healthcare system [39].
The samoby application offers several useful features, one of which allow pregnant women can take a photo of the childbirth planning and complication prevention program sticker that has been completed and affixed in front of the house and then upload the sticker photo on the application. Midwives in monitoring the program do not need to come to the homes of pregnant women one by one, simply by looking through the application. A study explained that the development of information and communication technology has changed the way health care is delivered. Many services are available via computer and mobile [40].
In addition, the samoby application also include a chat feature that can be used if pregnant women want to consult a midwife regarding their pregnancy. Midwives can provide explanations related to complaints experienced by pregnant women through the chat feature. The chat feature can also be used to remind pregnant women who have not completed the e childbirth planning and complication prevention program sticker. This samoby application can facilitate the task of midwives. A study explains that with web-based applications and the internet, health promotion officers can provide feedback using customized messages [41].
There is also a feature that contains material about the childbirth planning and complication prevention program. The material can be learned by pregnant women, husbands, and families at any time. The material was written using simple language so it can be easily understood. The design is engaging to prevent boredom. A study explains that social media is a good instrument as a teaching and learning tool [42]. Another study explained that mobile information should be easily accessible and use simple language [43].
The childbirth planning and complication prevention program is facilitated by midwives in rural in order to increase the active role of husbands, families, and communities in planning safe delivery and preparation for complications also planning the use of postpartum family planning using stickers as a target notification media in order to increase the coverage and quality of health services for mothers and newborns. This program is expected to reduce maternal and infant mortality rates. A study explains that preparation for labor and complications is important for perinatal survival [19].
The success of this program is also supported by the provision of health education about the childbirth planning and complication prevention program. Before giving an explanation of the samoby application, pregnant women were explained of the childbirth planning and complication prevention program, the benefits of it and how to fill in the sticker. Pregnant women were also given health education about pregnancy danger signs and what to do if they encounter these warning signs. Health education can provide an opportunity for pregnant women to discuss their concerns with health workers, both about things that must be done to prevent complications that occur in pregnancy and complaints experienced by mothers during pregnancy. Another study explains that educating mothers and increasing their awareness of danger signs of pregnancy and childbirth can improve labor preparation and complication preparedness. Another study explained that health facilities, program managers, and policy makers should be responsible and work together to improve health education services, knowledge about birth preparation, and complication readiness through accessible health education strategies [44]. Another study explained that pregnant women's knowledge about labor preparation and complication readiness is a factor associated with the successful implementation of these plans [45]. This is also in line with the previous study which explained that the level of knowledge of pregnant women about danger signs affects preparation for childbirth and complications. It is necessary to emphasize the quality of information provided to pregnant women during pregnancy check-upsand pregnant women with low economic conditions [46].
Providing health education about the childbirth planning and complication prevention program should not only be given to pregnant woman but also to the family or husband. Husbands must understand program so that they can participate directly. Husbands must also understand the danger signs of pregnancy. In a family, the husband is the head of the family and the decision-maker. A study explained that a husband's knowledge of pregnancy danger signs, labor preparation, and complication readiness is associated with overalllabor and complication readiness [47].
There are, however, several limitations to this study.These include a small sample size of only 50 respondents, aa lack of material features in the app, the absence of information about pregnancy danger signs, and the fact that the data analysis did not include a control group. Despite these limitations, the Samoby app has demonstrated its ability to improve the success of the childbirth planning and complication prevention program, which in turn has potential to reduce maternal and infant mortality rates.
CONCLUSION
Samoby app hhas increased the success of the childbirth planning and complication prevention Program by 38% in the the Sukorame Health Center working area,, Kediri. By using Samoby app, midwives can monitor the program through the application midwife doesn't have to come to the pregnant woman's house to check the childbirth planning and complication prevention program sticker attachment. In the Samoby app, there is also a chat feature which can be used by pregnant women to consult with midwives related to their pregnancy problem. The long-term impact of using the Samoby application is expected to reduce maternal and infant mortality rates through better birth planning and prevention of complications.
AUTHORS' CONTRIBUTION
It is hereby acknowledged that all authors have accepted responsibility for the manuscript's content and consented to its submission. They have meticulously reviewed all results and unanimously approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| ANC | = Antenatal Care |
| MCH | = Maternal and Child Health |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The study was approved by the ethical and research commitee at the Politeknik Kesehatan Kemenkes Malang, Indonesia under the number 382/KEPK-POLKESMA/2019.
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICATION
Informed consent was obtained from all the participants prior to study inclusion. Participants agreed before gaining access to the survey
AVAILABILITY OF DATA AND MATERIALS
The data and supportive information are available within the article.
ACKNOWLEDGEMENTS
Declared none.


