All published articles of this journal are available on ScienceDirect.
Investigating the Serum Level of Vitamin D and its Relationship with the Outcome of the Disease in Patients with COVID-19 Infection
Abstract
Background
Various studies have reported that the normal level of vitamin D is related to the improvement of the prognosis of patients. Therefore, the level of vitamin D should be checked in hospitalized patients and in cases of vitamin D deficiency.
Aim
This study was conducted to investigate the serum level of vitamin D and its relationship with the outcome of the disease in hospitalized patients with COVID-19.
Methods
This is a cross-sectional study (descriptive-analytical) that examined 100 patients with COVID-19. After obtaining permission from Jiroft University of Medical Sciences, the desired data was collected using a researcher-made checklist. The data of the study was collected by the researcher visiting the inpatient wards of the COVID-19 patients. Data were analyzed using SPSS-v-22 software.
Results
The average age of the patients was 54.3 ± 24.7 years (age range 3 to 96 years), of which 53 were women and 47 were men. Only 53% of the examined patients were hospitalized, and the rest were included in the study as outpatients. The level of vitamin D in hospitalized people was significantly lower than in outpatients, the serum level of vitamin D in deceased people was lower than in other groups, and a significant relationship was found between age and vitamin D levels in people with COVID-19.
Conclusion
The results demonstrated that the frequency of vitamin D deficiency was higher in patients with COVID-19. There was a significant relationship between the average serum level of vitamin D and the severity of COVID-19 disease.
1. INTRODUCTION
In the last two decades, it has become clear that vitamin D is important not only for regulating calcium and phosphate and maintaining bone and tooth health but also for many important intracellular functions in children and adults. Many studies have also reported that vitamin D is particularly important in regulating the immune system [1, 2]. In recent years, the role of vitamin D deficiency in various diseases, such as cancer, diabetes, multiple sclerosis, and neuropathic pain, has been reported [3-5]. Moreover, by controlling the production of inflammatory cytokines, vitamin D can be used as a useful anti-inflammatory agent to control the process of damage to nerve cells in old age and Alzheimer's disease [6]. During the global epidemic of COVID-19, various reports have been reported regarding the beneficial effects of vitamin D in preventing the disease and reducing the severity of the disease in infected people [7, 8]. Vitamin D can affect the activity of the innate and specific immune system by regulating the activity of immune cells, increasing the production of antimicrobial agents, and modulating the production of inflammatory cytokines and secreted antibodies [9-11]. Today, a large part of the world's population is facing the risk of vitamin D deficiency [12, 13], and according to the reports about the relationship between vitamin D and COVID-19, further study on the physiological and pathological effects of vitamin D is more necessary [7, 8].
In Iran, due to religious issues, such as the Islamic veil, especially for women, and less exposure to the sun in the northern half of the country, vitamin D deficiency is common among the people [14], and this can be one of the reasons for the spread of the COVID-19 in the country. This disease especially has more severe effects among the social strata with severe vitamin D deficiency, which can be prevented by compensating for this deficiency in the first degree. In the second degree, the severe complications and deaths caused by it can be prevented [7, 8]. Acute and chronic inflammation is the cause of many infections, especially respiratory infections, such as COVID-19, which causes progressive tissue destruction through the release of reactive oxygen species (ROS) and the production of cytokines at the site of inflammation [8]. Vitamin D exerts its anti-inflammatory effects through several mechanisms. First, vitamin D inhibits prost- aglandin production by inhibiting cyclooxygenase-2 (Cyclooxygenase; COX2) enzyme [12, 13]. By increasing the permeability of blood vessels, prostaglandin facilitates the passage of immune cells into the tissue and causes inflammation symptoms. Second, by activating the phosphatase enzyme and preventing the phosphorylation and activation of p38 MAPK, vitamin D inhibits the p38MAPK signaling pathway, which is a specific pathway for the production of inflammatory cytokines. Thirdly, vitamin D reduces the transcription rate of inflammatory genes by inhibiting factor transcription. In addition, it has been shown that vitamin D regulates the interaction between immune cells and cancer cells, thereby preventing the overactivation of immune cells and excessive production of pro-inflammatory cytokines [3, 14-16]. According to these results, it can be suggested that vitamin D can regulate the activation of immune cells and the production of inflammatory cytokines by regulating the interaction between immune cells and virus-infected cells in viral diseases, such as COVID-19. Therefore, consuming vitamin D in the form of medicinal supplements is very necessary and important, especially in the conditions of the COVID-19 epidemic. Of course, depending on the age, nutritional, occupational, and geographic conditions in different people, the amount of deficiency and the need to compensate for it is different, and it is necessary to consult a doctor and check the serum level of vitamin D. Therefore, the present study aims to check the serum level of vitamin D and its relationship with the outcome of the disease in patients with COVID-19.
2. METHODS AND MATERIALS
This study is a cross-sectional (descriptive-analytical) study. In this study, the research population included all patients with COVID-19 who were referred to Imam Khomeini Hospital in Jiroft in 2022. The inclusion criteria included patients with COVID-19 whose disease was diagnosed by an expert using the RT-test. PCR was confirmed with a positive result. Patients who did not agree to participate in the study, the pregnant woman, and the discharged person were excluded with personal consent. After obtaining permission from Jiroft University of Medical Sciences, the desired data was collected using a researcher-made checklist. The serum level of vitamin D was measured in these patients, and if the level of vitamin D is less than 20, it is deficient, 20-29 is insufficient, 30-100 is sufficient, and more than 100 ng/ml is classified as toxic. The data of the study was collected by the researcher visiting the inpatient wards of the COVID-19 patients and using a pre-prepared checklist, including demographic information of underlying diseases, discharge, transfer to the intensive care unit, death, days of hospitalization, and vitamin D level using the monobind vitamin kit D prepared by the ELISA method.
One of the limitations of this research was the lack of sufficient information in some required fields, as well as the possibility of non-cooperation of some participants in the research.
After entering the questionnaire data into SPSS software version 22, the number of selected samples was calculated. First, the statistical indicators related to descriptive statistics, such as mean, standard deviation, frequency, and frequency percentage, were calculated, then the Kolmogorov-Smirnov test was conducted to check the normality status. Afterward, parametric tests, such as the t-test of two independent samples, analysis of variance, or their non-parametric counterparts, such as the Mann-Whitney test, Kruskal-Wallis test, and chi-square test, were conducted to test the hypotheses. The significance level in this research was considered less than 0.05.
3. RESULTS
The present study is cross-sectional (descriptive-analytical) that examined 100 patients with COVID-19, who were referred to Imam Khomeini Hospital. Table 1 presents the information related to the demographic variables of the examined people. The average age of the patients was 54.3 ± 24.7 years (age range 3 to 96 years), with the highest frequency in the age group of 61 to 80 years (31%), and the lowest frequency was observed in the age range of 1 to 20 years (13%). Out of 100 people surveyed, 53 were women and 47 were men. Only 53% of the examined patients were hospitalized, and the rest were included in the study as outpatients.
| Variables | Frequency | |
|---|---|---|
| Age | 1-20 | 13 |
| 21-40 | 17 | |
| 41-60 | 21 | |
| 61-80 | 31 | |
| >80 | 18 | |
| Sex | Female | 53 |
| Male | 47 | |
As mentioned in Table 2, the average White Blood Cell (WBC) in hospitalized and outpatient patients with COVID-19 was 20.36 and 9.98, respectively, which was higher in hospitalized patients than outpatients. They were not within the normal WBC range of 4,500 to 11,000 per microliter (4.5 to 11.0 × 109/L).
The average Erythrocyte Sedimentation Rate (ESR) in hospitalized and outpatient patients with COVID-19 was 29.07 and 32.88, respectively, which was higher in outpatients than in hospitalized patients, and in hospitalized patients, ESR was not within the normal range (less than 20).
| Variables | Group | |||
|---|---|---|---|---|
| Hospitalized | Outpatient | |||
| Mean | Standard Deviation | Mean | Standard Deviation | |
| White Blood Cell (WBC) | 20.36 | 18.88 | 9.98 | 6.9 |
| Erythrocyte Sedimentation Rate (ESR) |
29.07 | 27.6 | 32.88 | 28.4 |
| C Reactive Protein (CRP) | 34.62 | 26.5 | 7.57 | 1.9 |
The average C Reactive Protein (CRP) in hospitalized and outpatient patients with COVID-19 was 34.62 and 7.57, respectively, which was higher in hospitalized patients than outpatients and was not in the normal range of CRP (less than 10 mg/l).
As mentioned in Table 3, the average serum level of vitamin D in people with COVID-19 in both outpatient and inpatient groups was 22.35 and 22.18 ng/ml, respectively, and the level of vitamin D in hospitalized people was less than in outpatients. Moreover, a statistically significant difference was found in terms of the obtained averages (p<0.05).
| Variables | Group | P-value | |||
|---|---|---|---|---|---|
| Hospitalized | Outpatient | ||||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| Vitamin serum level D | 35.27 | 22.05 | 22.18 | 9.2 | 0.000 |
| Variables | Group | |
|---|---|---|
| Vitamin D levels | Hospitalized | Outpatient |
| Frequency (percent) | Frequency (percent) | |
| < 20 | 32 (60.3%) | 29 (61.7%) |
| 20-29 | 11 (20.7%) | 14 (29.7%) |
| 30-100 | 10 (19%) | 4 (8.6%) |
| Total | 53 (100%) | 47 (100%) |
Table 4 presents the information related to different levels of vitamin D in patients with COVID-19 who were undergoing outpatient treatment and hospitalization. Out of 53 hospitalized people, 32 people (60.3%) had vitamin D levels less than 20, 11 people (20.7%) had levels from 20 to 29, and 10 people (19%) had vitamin D levels in the range of 30 to 100. Out of 43 people who were in outpatient treatment, 29 people (61.7%) had vitamin D levels of less than 20, 14 people (29.7%) had vitamin D levels in the range of 20 to 29, and 4 people (8.6%) had in the range of 30 to 100.
Table 5 presents the information related to the relationship between the average serum level of vitamin D and age. The results indicated that in outpatients, the highest average level of vitamin D in the 21 to 40-year age group was 46.8 ng/ml, and the lowest average level of vitamin D in the age group over 80 years old was 25.94 ng/ml. Moreover, in hospitalized people, the highest average level of vitamin D in the group 21 to 40 years old was 26.11 ng/ml, and the lowest average level of vitamin D in the age group over 80 years was 19.5 ng/ml. A statistically significant relationship was observed between the serum levels of vitamin D and the age of people with COVID-19 (P-value <0.05).
Table 6 presents information related to the relationship between the average serum level of vitamin D and gender. The results indicated that in both outpatient and inpatient groups, the serum level of vitamin D was lower in men than in women, and there was a statistically significant relationship between the mean serum level of vitamin D and gender (P-value <0.05).
Table 7 presents the information related to the relationship between the average serum level of vitamin D and underlying disease. In both outpatient and inpatient groups, the average serum level of vitamin D in people with underlying disease was lower than in people with no underlying disease. Moreover, there was no significant relationship between the mean serum level of vitamin D and underlying disease (P-value >0.05).
Table 8 presents the information related to the relationship between the average serum level of vitamin D and the prognosis of the disease. In hospitalized people, the average serum level of vitamin D in people who died was lower than in other groups, and statistically, there was a significant relationship between the average level of serum vitamin D and the prognosis of the disease (P-value <0.05).
Table 9 presents information related to the relationship between the average serum level of vitamin D and days of hospitalization. No relationship was found between the average level of serum vitamin D and days of hospitalization in patients with COVID-19 (P-value >0.05) (Fig. 1).
| Variables | Group | P-value | |||
|---|---|---|---|---|---|
| Outpatient | Hospitalized | ||||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| 1-20 | 38.78 | 9.9 | - | - | 0.001 |
| 21-40 | 46.8 | 16.2 | 26.11 | 10.08 | |
| 41-60 | 34.95 | 11.6 | 22.13 | 8.1 | |
| 61-80 | 28.79 | 20.8 | 21.20 | 8.8 | |
| >80 | 25.94 | 26.5 | 19.5 | 2.2 | |
| Variables | Group | P-value | |||
|---|---|---|---|---|---|
| Outpatient | Hospitalized | ||||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| Mean | 32.6 | 13.1 | 21.92 | 9.6 | 0.04 |
| Women | 36.8 | 26.02 | 22.79 | 8.2 | |
| Variables | Group | P-value | |||
|---|---|---|---|---|---|
| Outpatient | Hospitalized | ||||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| Yes | 34.2 | 22.5 | 21.74 | 10.7 | 0.239 |
| No | 36.8 | 21.6 | 22.27 | 9.01 | |
| Variables | Group | P-value | |||
|---|---|---|---|---|---|
| Hospitalized | Outpatient | ||||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| Discharge | 24.1 | 23.2 | 35.27 | 22.05 | 0.03 |
| Death | 20.1 | 2.4 | - | - | |
| Transfer to ICU | 22.1 | 11.9 | - | - | |
| Variables | Group | P-value | |
|---|---|---|---|
| Hospitalized | - | ||
| Mean | Standard Deviation | ||
| 3-4 | 23.7 | 9.1 | 0.782 |
| 5-6 | 21.5 | 2.34 | |
| 6-8 | 21.6 | 18.3 | |
| > 8 | 21.6 | 18.3 | |
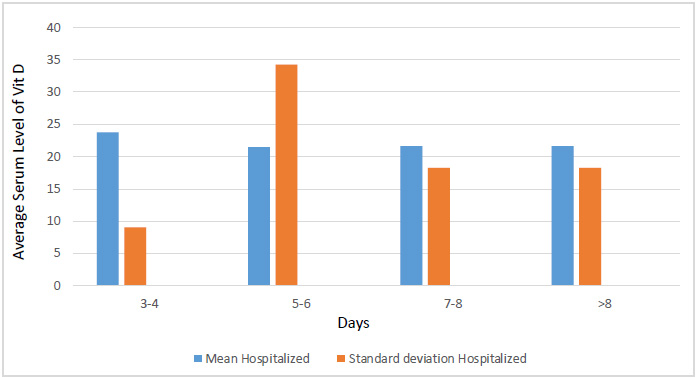
Correlation between the average serum level of vitamin D and days of hospitalization in patients with COVID-19.
4. DISCUSSION
One of the topics that has received a lot of attention from researchers over the years is the relationship between serum levels of vitamin D and respiratory diseases. In various studies, the effect of vitamin D on chronic obstructive pulmonary diseases, asthma, allergies, influenza, and upper respiratory infections has been explored [17-19]. With the start of the COVID-19 pandemic, many reports have been published about the effects of this vitamin in preventing the disease and reducing the severity of the disease in infected people [20]. Therefore, the present study aimed to determine the serum level of vitamin D and its relationship with the outcome of the disease in patients with COVID-19.
The results of the present study showed that the level of vitamin D in hospitalized people was significantly lower than that of outpatients. In other words, a significant relationship was found between the level of vitamin D and the severity of the disease of COVID-19. Evidence of an association between 25-hydroxyvitamin D deficiency and poor disease outcomes has been reported in several studies [21-23]. In the study by Im et al., which investigated the status of vitamins and minerals in patients with the 2019 coronavirus, it was found that the serum level of vitamin D in patients with the acute form of COVID-19 was significantly lower compared to the mild group. On the other hand, in this study, the frequency of vitamin D deficiency was significantly higher in the group of patients with COVID-19 [24].
The meta-analysis study by Ghasemian et al. also reported that a significant fraction of patients with COVID-19 suffered from vitamin D deficiency and insufficiency, which is also related to the increased risk of COVID-19 [25]. In the study by Faul et al., it was found that the serum level of vitamin D in patients with coronavirus who ultimately required hospitalization in the ICU was lower than in patients with milder manifestations who were hospitalized in the general ward [26]. Notz et al. reported that 25-hydroxyvitamin D status was not associated with changes in the clinical course of the disease, but low 25-hydroxyvitamin D levels were associated with prolonged mechanical ventilation and worse APACHE2 score [27]. Hosack and colleagues also stated that the lack of vitamin D serum level increases the possibility of the occurrence of cytokine storms and severe disease of COVID-19. It was found that the deficiency of vitamin D plays a vital role in the prevalence and severity of disease. However, they could not find a statistically significant difference between this deficiency and the death rate caused by the coronavirus [28]. Aygun stated in his study that vitamin D prevents the occurrence of cytokine storms by several mechanisms and significantly reduces the exacerbation of COVID-19 and multi-organ failure syndrome [29]. Understanding the role of vitamin D in the function of innate and adaptive immunity, Chandran and colleagues stated that the administration of this vitamin is like water to fire in preventing cytokine storms [30]. In their study, Katz et al. also examined vitamin D deficiency in terms of its effect on the prevalence and severity of COVID-19 disease, along with risk factors, such as respiratory and heart failure, diabetes, obesity, and black race, and on the role of correcting this deficiency in reducing the incidence and emphasized the complications of COVID-19 [31]. Pizzin et al. stated that vitamin D deficiency is common in patients with COVID-19, but it is not related to the consequences of the disease [32]. Maqboli et al. stated that improving vitamin D status in the general population and hospitalized patients with COVID-19 has a potential effect in reducing the severity of the disease [33]. Ye et al. pointed out the positive relationship between vitamin D deficiency and the severity of the disease of COVID-19 and also stated that elderly people with underlying diseases are exposed to more severe forms of the disease [34]. However, in a study by Lohia et al., no statistically significant correlation was found between vitamin D levels and disease severity [35], and Hernández et al. reported no correlation between vitamin D levels and disease severity [36]. Vitamin D plays a key role as a negative endocrine regulator in the RAS and prevents the expression of renin. This micronutrient induces the Mas/Ang/ACE2 axis, inhibits the activity of the AT1/Ang/ACE2 axis, and finally has a protective effect against acute lung injuries and Acute Respiratory Distress Syndrome (ARDS).
Vitamin D also plays a role in trapping and preventing SARS-CoV-2 replication by reducing pro-inflammatory cytokines, increasing anti-inflammatory cytokines, increasing antimicrobial peptides, and activating defense cells such as macrophages. Therefore, targeting the imbalanced RAS and regulating the downregulation of ACE2 by vitamin D is a promising therapeutic approach to combat COVID-19 and ARDS [37].
In the current study, the serum level of vitamin D was lower in deceased people than in other groups. In this regard, Baktash et al. investigated the status of serum vitamin D and the outcome of the disease in elderly patients with COVID-19. Patients with COVID-19 who had a lower vitamin D level compared to patients of the same age who received vitamin D supplements demonstrated a more unfavorable outcome [23]. Sulli et al. reported in their study that serum vitamin D deficiency is associated with more severe pulmonary involvement, longer disease duration, and risk of death in elderly patients with COVID-19 [38]. Raharusun et al. reported that serum vitamin D status has a significant positive relationship with the outcome of mortality in infected people [39]. Ling et al. stated that treatment with a high dose of cholecalciferol is related to the reduction of mortality in COVID-19 patients [40]. Adami. et al. reported that vitamin D deficiency is associated with more severe respiratory failure [41]. Karahan et al. reported that the serum level of vitamin D is a predictive factor for mortality in affected individuals [42]. De Smet et al. demonstrated that the low level of serum vitamin D is related to the mortality rate caused by COVID-19 [43]. Infante et al. suggested an inverse relationship between the serum vitamin D level and the mortality rate [44]. Carpagnano et al. showed that the risk of mortality is higher in patients with severe vitamin D deficiency [45]. However, in a study by Azadeh et al., serum levels of vitamin D in deceased patients and recovered patients were investigated and compared in two groups of hospitalized and non-hospitalized patients in the ICU. Finally, a significant difference in serum levels of vitamin D was observed between these groups [46].
The findings of the research showed a significant relationship between age and vitamin D levels in people with COVID-19. With increasing age, the level of vitamin D decreases. Since the beginning of the COVID-19 pandemic, age has been identified as a risk factor for morbidity and mortality. Although there have been changes in the researchers' observations over time, the rate of this disease is still higher in the elderly. According to the United States Centers for Disease Control (CDC) and Prevention, a high percentage of deaths caused by the coronavirus was reported in people over 65 years old. Moreover, the risk of infection was found to be higher in the elderly. On the other hand, with age, the production of vitamin D by the skin decreases, and disorders in the body's hormonal system can occur, including disorders in the metabolism of vitamin D [47]. Estimates of risk factors for mortality due to COVID-19 were investigated by Caramelo et al. in China. The results of this study demonstrated that age is a variable associated with a higher risk of mortality due to COVID-19 [48]. In the study conducted by Grasselli et al. on the risk factors related to mortality in patients with COVID-19 in Italy in intensive care units, age was also introduced as a risk factor for the disease [49]. The serum concentration of vitamin D decreases with age, and this vitamin may be important in the context of COVID-19 because the mortality rate in these patients increases with age [50].
In the study by Mohammadi et al., vitamin D deficiency was evaluated in both sexes, and this deficiency was more common in men than in women [51]. However, contrary to the present study's findings, the results of the study by Hossein Nezhad and Holick demonstrated that the serum level of vitamin D in women was lower than in men. This difference in the findings can be related to the different geographical situations, socio-cultural situations, and nutritional status of the people investigated in the two studies mentioned [14]. On the other hand, gender is also known as one of the risk factors for COVID-19, which is mentioned in most studies. In the report of the World Health Organization on February 28th, 2020, it was determined that 51.1% of the deceased were men [52]. In the meta-analysis published in April, 2020, which examined the results of 656 patients, the rate of infection was also higher in men, and these results were consistent with our studies [53]. So far, about 60% of deaths due to COVID-19 have been reported in men, which is consistent with the studies reporting the increase in the death rate of men due to COVID-19 compared to women [49]. According to Caramelo et al., a higher death rate in men was also reported in China [48].
Among other findings of the research, the average ESR, WBC, and CRP in patients with COVID-19 were not within the range. In their study, Zhu et al. concluded that the WBC count was within the normal range at admission, but those with higher WBC had a much higher chance of death. Moreover, a significant relationship between WBC count and death rate was also reported [54]. The average CRP in the study was 75.81 ± 54, which indicated that the degree of increase in CRP indicates the systemic release of cytokines, and the increase in CRP>41 indicates the worsening of the disease [55]. Liu et al. conducted research to describe the clinical manifestations and features of CT scans and laboratory results of COVID-19 disease in 15 pregnant women. Their results showed that the most common abnormal laboratory findings were a decrease in blood lymphocytes (12.15 patients) and an increase in CRP (10.15 patients) [56]. In a retrospective study on 1099 patients, increased CRP was found in 60.7% of patients with COVID-19, and on the other hand, the increase in inflammatory markers CRP and LDH was significant in patients with severe disease [57]. A higher level of CRP was associated with worse clinical outcomes of the COVID-19 disease, including the development of ARDS, increased troponin levels, and myocarditis, as well as higher mortality [58]. Studies reported that patients who were over 60 years old demonstrated more symptoms, such as lymphopenia, thrombocytopenia, and increased levels of CRP and lactate dehydrogenase [59]. Further investigations showed an increase in CRP and ESR, and also, by examining the CT image symptoms, such as ground-glass opacification/opacity or GGO, fibrotic streaks, subpleural transparent lines, and thick lungs were observed [60]. A significant increase in infection-related biomarkers of patients, such as interleukin-6, serum ferritin, CRP, and ESR, was also reported [61]. Another study, on the blood samples of 1099 patients infected with COVID-19 from different provinces of China, reported that in 83.2% of patients, the level of lymphocytes was lower than normal, and in 36.2% of patients, platelets were lower than normal. The normal limit and the number of leukocytes in 33.7% of infected patients were found to be lower than normal [62].
CONCLUSION AND RECOMMENDATIONS
Based on the findings presented, it is evident that vitamin D levels play a crucial role in the outcomes of COVID-19 patients. The significantly lower levels of vitamin D in COVID-19 patients admitted to the corona ward compared to those treated on an outpatient basis suggest a potential link between vitamin D status and disease severity. This highlights the importance of monitoring and potentially supplementing vitamin D levels in COVID-19 patients to improve outcomes and potentially reduce the need for hospitalization.
Furthermore, the association between lower serum vitamin D levels in individuals who succumbed to COVID-19 compared to survivors underscores the potential impact of vitamin D on mortality rates in COVID-19 patients. This finding emphasizes the need for further research into the mechanisms by which vitamin D may influence disease progression and outcomes in COVID-19. It also suggests that optimizing vitamin D levels could be a critical factor in reducing mortality rates among COVID-19 patients.
The observed relationship between age and vitamin D levels in individuals with COVID-19, as well as the gender disparity in vitamin D levels among male and female patients, points towards potential demographic factors that may influence vitamin D status and its implications for COVID-19 outcomes. Understanding these demo- graphic variations can help improve interventions and treatment strategies to address specific risk factors associated with vitamin D deficiency in different patient populations.
Moreover, the significant association between the average serum level of vitamin D and the severity of COVID-19 highlights the potential role of vitamin D in modulating the immune response and inflammatory processes involved in COVID-19 pathogenesis. This suggests that maintaining optimal vitamin D levels could be a key factor in mitigating the severity of COVID-19 and improving overall prognosis. Further research and clinical trials are warranted to explore the therapeutic potential of vitamin D supplementation in COVID-19 management and to elucidate the underlying mechanisms of its effects on disease outcomes.
RECOMMENDATIONS FOR HEALTH POLICY MAKERS
Promote Vitamin D Screening
Encourage routine screening for vitamin D levels in individuals at risk of COVID-19, such as older adults, individuals with pre-existing conditions, and those from marginalized communities. Implementing targeted screening programs can help identify individuals with vitamin D deficiency early on and facilitate timely interventions to optimize their vitamin D status.
Develop Guidelines for Vitamin D Supplementation
Establish evidence-based guidelines for vitamin D supplementation in COVID-19 patients, especially those with low serum levels. Health policymakers should work closely with healthcare professionals to determine appropriate dosages and duration of supplementation based on individual needs and disease severity.
Educate Healthcare Providers
Training and educational resources should be provided to healthcare providers on the importance of monitoring and addressing vitamin D deficiency in COVID-19 patients. Enhancing provider knowledge of the role of vitamin D in immune function and its potential impact on disease outcomes can improve patient care and treatment strategies.
Incorporate Vitamin D into Public Health Strategies
Integrate recommendations for maintaining adequate vitamin D levels into public health campaigns and initiatives. Encourage sunlight exposure, dietary sources of vitamin D, and supplementation where necessary to support overall immune health and potentially reduce the severity of COVID-19 infections.
Support Research on Vitamin D and COVID-19
Allocate resources for further research into the mechanisms underlying the relationship between vitamin D status and COVID-19 outcomes. Funding studies to investigate the effects of vitamin D supplementation on disease progression, mortality rates, and immune responses can provide valuable insights for future treatment guidelines and public health policies.
By implementing these recommendations, health policymakers can contribute to a more comprehensive approach to managing COVID-19, considering the potential impact of vitamin D status on disease outcomes. Prioritizing strategies to optimize vitamin D levels in at-risk populations can potentially improve patient outcomes, reduce healthcare burden, and enhance overall public health resilience in the face of the ongoing pandemic.
AUTHORS’ CONTRIBUTION
It is hereby acknowledged that all authors have accepted responsibility for the manuscript's content and consented to its submission. They have meticulously reviewed all results and unanimously approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| WBC | = White Blood Cell |
| ESR | = Erythrocyte Sedimentation Rate |
| CRP | = C Reactive Protein |
| CDC | = Centers for Disease Control |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This project was approved by the ethics committee of Jiroft University of Medical Sciences, Iran under the ethics code IR.JMU.REC.1401.009.
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
AVAILABILITY OF DATA AND MATERIALS
The data that support the findings of this study are available from the corresponding author [S.D.] upon reasonable request.
FUNDING
This research was carried out with the financial support of Jiroft University of Medical Sciences, Iran.
ACKNOWLEDGEMENTS
The authors appreciate the collaboration of the manager and staff of Imam Khomeini Hospital in Jiroft for this research.


