All published articles of this journal are available on ScienceDirect.
Exploring the Understanding and Triage Practices of Midwives Working in District Hospitals of Mpumalanga Province, South Africa
Abstract
Background
Triage in healthcare involves the process of prioritizing patients in their level of urgency and also the allocation of resources. However, triage has been used mainly in emergency departments around the world. Only in recent years have triage systems been gradually implemented in maternity units. It is a relatively new concept in maternity units and its landscape is not properly understood.
Objective
The study aimed to explore the understanding and practices of triage by midwives working in the labour wards of selected district hospitals in Mpumalanga province, South Africa.
Methods and Materials
A qualitative, exploratory, and descriptive research design was used to explore the practices and understanding of midwives regarding labour ward triage. A purposive sampling method was used to select experienced midwives who work in labour wards. The sample size was directed by data saturation, reached at the 20th participant. The data were then analysed using thematic analysis. Trustworthiness was ensured through the Lincoln and Guba criteria (1985).
Results
Two themes emerged regarding midwives' understanding and practices of triage namely, a nuanced understanding of triage in the labour wards and a description of existing triage practices of midwives. The themes were interpreted into five sub-themes.
Conclusion
The study revealed that the absence of triage systems in maternity units delays obstetric care, contributing to poor maternal and perinatal outcomes and rising litigation in South Africa. The findings call for the National Department of Health to strengthen triage policies and guidelines and suggest co-designing a triage system with midwives to enhance implementation and feasibility.
1. INTRODUCTION
The World Health Organization (WHO) and the Campaign for Accelerated Reduction of Maternal Mortality in Africa (CARMMA) envisioned a world where every woman and newborn receives quality care and treatment throughout pregnancy, intrapartum, and puerperium period; a world where no woman dies giving birth [1]. However, maternal and perinatal deaths remain a global concern. Approximately 287,000 maternal deaths and 1.9 million stillbirths were reported in 2020 and 2019, respectively [2, 3]. Some scholars and the WHO highlighted that the main causes of maternal and perinatal mortality and morbidity are delays in receiving adequate and appropriate care upon arrival in the maternity units, along with a lack of knowledge of healthcare providers, especially in low and middle-income countries [4, 5]. The United States Agency for International Development (USAID) [6] says that millions of women die as a result of substandard maternal health care services. The WHO reported that to combat maternal and perinatal morbidities, skilled care should be provided before and during birth to save the lives of women and newborns [3]. Halim et al. [7] state that it is of significance to improve the quality of care provided in health facilities by further focusing on strengthening the skills and practices of healthcare providers in the early detection and treatment of complications.
Existing investigations showed that proper triage systems and timely, appropriate treatment upon arrival at maternity units are pivotal in improving patient care quality and reducing maternal and neonatal mortality. Moudi et al. [4] and Fernandes et al. [8] assert that effective triage enhances clinical decision-making by prioritizing care for mothers and their infants based on the severity of their conditions, thereby ensuring timely allocation of medical resources and necessary interventions. Therefore, proper triage facilitates early identification of high-risk cases, enabling prompt interventions that can prevent complications and adverse outcomes. It also ensures that patients receive the correct level of care based on the severity of their condition. Despite evidence demonstrating the critical role of proper triage systems in improving patient care quality and reducing maternal and neonatal mortality, there remains a significant gap in the lack of standardized triage protocols in many maternity units, particularly in Mpumalanga district hospitals. The lack of a structured triage system may jeopardize prompt interventions, contributing to unfavourable maternal and neonatal outcomes. Obstetric triage has been recognized and implemented in certain healthcare settings as a key intervention to address maternal and neonatal mortality. This approach facilitates the prioritization of care, ensuring that high-risk cases receive timely and appropriate interventions, thereby reducing adverse outcomes. For example, in North America, obstetric triage acuity scales are used for a quicker initial assessment and shorter wait times [9]. Furthermore, data on acuity, volume, and trends enhanced the number of nurses and other staffing in triage units [9]. The findings of a study conducted in the United Kingdom asserted that the triaging of pregnant women in obstetric units is associated with improved safety of women and babies and reduced waiting time for obstetric assessment of pregnant women [10]. In Sub-Saharan Africa, a tertiary hospital in Ghana developed and implemented an obstetric triage system [11]. The implementation of the newly developed obstetric triage system resulted in a 44% reduction in patient waiting times over a 12-month period. However, in South Africa, a study by Tukisi et al. [12] highlighted the use of initial assessment within maternity records of pregnant women. Clearly, this is not practiced nationally. South Africa appears to have relied on emergency department systems, such as the South African Triage Scale (SATS) [13], for obstetric triage rather than developing a standardized system of its own. Although the SATS has been adapted to include the triaging of pregnant women in emergency departments, it lacks comprehensive coverage of obstetric emergencies, particularly within maternity units. It only focuses on abdominal trauma during pregnancy, ectopic pregnancies, and vaginal bleeding [13]. In addition, the first author observed that many labor wards in Mpumalanga province lack a formal triage system, which has led to instances of patients delivering in waiting areas. This contributes to poor maternal and perinatal outcomes and has sparked increased public dissatisfaction with the quality of care provided in maternity units. Sumbane et al. [14] assert that these incidents contribute to the rise in intrapartum malpractices in maternity units. Moodley et al. [15] findings agree that lack of triage is associated with late recognition and management of obstetric emergencies by physicians and midwives, resulting in poor maternal and perinatal outcomes.
The nexus between existing literature on maternal and perinatal deaths attributable to avoidable factors and the author's observations underscores the detrimental impact of the absence of a triage system in maternity units. This lack of a structured triage process not only compromises the quality of care but also results in significant financial losses for government budgets due to malpractices and preventable maternal deaths. It also affects the midwives' understanding and practices of triage. A study conducted in South Africa exploring midwives' experiences with the obstetric triage tool found that they struggled to understand its processes due to insufficient guidance. Additionally, the low staffing levels hinder effective implementation and practices, resulting in an unfavorable midwife-to-patient ratio [12]. While midwives play a crucial role in maternal care, there is limited research on their understanding and triage practices, particularly in district hospitals in Mpumalanga Province, South Africa. This could impede timely obstetric interventions, exacerbating poor maternal and perinatal outcomes. In light of this, the current paper focuses on exploring and describing the understanding and triage practices of midwives working in the labor wards of a selected district hospital in Mpumalanga province of South Africa.
2. MATERIALS AND METHODS
2.1. Study Design
An exploratory, descriptive, and qualitative research design underpinned this study to explore and describe the understanding and triage practices of midwives when triaging pregnant women presenting in the labor wards. The use of qualitative research allowed the authors to gain in-depth insight into the triage practices of midwives and reflect their understanding of triage [16].
2.2. Study Setting
The study was conducted in two conveniently selected district hospitals located in two geographically distant districts within the Mpumalanga province of South Africa. This allowed the authors to gather different but broader perspectives on understanding triage and midwifery triage practices in different hospitals. Mpumalanga is located in the north-east area of SA bordering Swaziland and Mozambique to the east, also bordering Limpopo, Gauteng, the Free State, and Kwa-Zulu Natal within the country. It is the second smallest province in SA after Gauteng; it covers approximately 76,495km squared with a population of 4,335,964. Mpumalanga has 3 districts, namely Ehlanzeni, Nkangala and Gert Sibande District; and a total of 17 local municipalities [17]. The province's health structure is composed of district, tertiary, and regional hospitals, some of which are specialized hospitals with a total of 32 public hospitals, and primary healthcare facilities of a total of 289, including community health centers.
2.3. Sampling and Recruitment
The study used a purposive sampling technique to select midwives working in the labor wards of the district hospitals. The two hospitals are the best representation of the public maternity care facilities in the region, as the primary health care facilities refer maternal and neonatal high-risk and emergency cases for further management to them. Therefore, the participants had relevant experience and could contribute meaningful data to address the research objectives. Following obtaining ethical clearance and permission from the university ethics committee and the Mpumalanga Department of Health, respectively, the authors sought permission from the hospital management to recruit midwives working within the labor wards to take part in the study. The study intentions and procedures were explained to the midwives and those who were working in labor wards for more than a year and willing to take part signed and informed consent form.
2.4. Data Collection
The authors used semi-structured one-on-one interviews and field notes for data collection. Prior to the main data collection, a pilot study was conducted to evaluate the interview guide with three midwives. These interviews were transcribed verbatim and sent to qualitative research experts (LM and TM) along with the recordings. Thereafter, arrangements were made between the authors to refine and modify the interview questions. This assisted the authors in refining the interview guide, ensuring that questions were clear, relevant, and aligned with the study objectives. The midwives who participated in the pilot study were not included in the main study.
The participating midwives were interviewed in their free time to avoid interfering with obstetric care. The sample size was determined by data saturation reached the 15th participant when rich and concise information was obtained and no new information was arising on the practices and understanding of triage by midwives. However, an extra 5 participants were interviewed to confirm that there is no new information emerging. The interviews were conducted following an interview guide and probing questions were asked depending on the participant's response to get clarity. After obtaining consent from the participants, the interviews were recorded using an audio recording device. Data collection was carried out from May to July 2024, each interview lasting an average of 30-50 minutes. The interviews were conducted in IsiZulu, English, and Sepedi. Each participant was given equal opportunities to choose the language of preference to express themselves relatively in-depth. During the interview process, the author established a trusting relationship with the key participants and bracketing was done to set aside personal biases, beliefs, and assumptions. This assisted the first author in approaching the data collection process with a more open and objective perspective. Thus, the author remained neutral and asked the key participants the same questions throughout the study, differing from the probing as it depended on the information each participant was providing.
2.5. Data Analysis
The first author tried the best of his ability to transcribe the interviews at the earliest convenience while still being able to recall the events of the interviews. The interviews were transcribed verbatim. The transcribed data were analyzed using thematic analysis. The authors followed the iterative steps of thematic analysis as suggested by Kiger and Varpio [18]. The first author independently read the transcript multiple times to become familiar with the data. Thereafter, the codes and search for potential themes were generated [18, 19]. Furthermore, the author deductively coded the data for codes and theme development. During the analysis, the authors brought in theoretical concepts from the study research questions to make meaning, sense, and interpretation of the data. Through semantic coding of the data, the author was committed to identifying and summarizing the content of the data and, building the codes and themes around what the participants said and reflecting their meanings [19]. Subsequently, the transcripts and audio recordings were sent to other authors (LM, MMR, and TMM) to independently analyze the data, noting that they are qualitative research experts with extensive experience in qualitative research. The themes were then reviewed and named. The analysis process is summarized in the figure below, as suggested by Terry et al. [19] (Table 1).
2.6. Ethical Considerations
The study was granted ethical clearance by the University of Limpopo, Turfloop Research Ethics Committee (TREC/65/2024:PG). Following ethical clear-ance, the permission to conduct the study was granted by the Mpumalanga Department of Health after obtaining a letter of endorsement and support from the clinical facilities' Chief Executive Officers. The authors ensured that all ethical standards were adhered to throughout the study. The participants were provided with detailed consent entailing the purpose of the study and that they are not forced to partake in the research and the study's findings may be published. However, their names won’t be displayed and pseudonyms were used to further ensure anonymity and confidentiality. The author liaised with senior management to assist with providing a private room where interviews were conducted, and other ethical principles such as social justice and non-maleficence were followed.
| Thematic Analysis Steps | Application to the Study |
|---|---|
| Familiarizing with the data | The author listened to the audio recordings and further transcribed the data. Thereafter, the author listened to all the audio recordings once more and reread all the transcripts analytically and critically to get the whole meaning of the textual data. |
| Generating Initial Codes | The author then systematically analyzed the data and further noted any potential codes that were relevant to answering the research questions. Furthermore, the author coded each data item in its entirety before coding another. |
| Searching for themes | The author reviewed the coded data and identified any similarities and overlaps between the codes; then, clustered the codes that seemed to share unifying features and then generated themes. Finally, we collated all the data extracts to each for theme reviewing purposes. |
| Reviewing potential themes | The author reviewed the themes in relation to the coded data and the entire data set; and further checked the potential themes against the collated data extracts. Thereafter, the author reread all the data to ensure that the themes meaningfully capture the entire data set and answer the research questions. |
| Defining and Naming Themes | The author selected, presented, and analyzed the extracts and then presented the story of each theme with the extracts. The data were then connected to the broader research question. Lastly, the researcher named the themes in coherence with the defined themes identified from the entire data set. |
| Producing the report | The author then finalized the themes by ensuring that the were coherent and that they are relevant and meaningful. For trustworthiness purposes, the audio recordings and transcripts were sent to a qualitative research expert for verbatim and analysis. |
| Items | Responses | N |
|---|---|---|
| Gender | 1. Female | 19 |
| 2. Male | 1 | |
| Total | 20 | |
| Age | 1. 20-29 | 2 |
| 2. 30-39 | 2 | |
| 3. 40-49 | 11 | |
| 4. 50-59 | 5 | |
| Total | 20 | |
| I am a (occupation) | 1. Advanced Midwife | 7 |
| 2. Registered midwife/Accoucheur | 13 | |
| Total | 20 | |
| Highest level of qualification | 1. Bachelor's degree | 4 |
| 2. Diploma (R425) | 7 | |
| 3. Advanced diploma in midwifery | 2 | |
| 4. Postgraduate diploma/ honours in advanced midwifery | 7 | |
| 5. Masters in advanced midwifery | 0 | |
| Total | 20 | |
| Years of experience in maternity unit | 1. 1-5 | 6 |
| 2. 6-10 | 3 | |
| 3. 11-15 | 5 | |
| 4. More than 15 | 6 | |
| Total | 20 | |
2.7. Ensuring Trustworthiness
The elements to ensure the trustworthiness of Lincoln and Guba as entailed by Polit and Deck were used [16]. To ensure truth value and credibility, the author engaged in a prolonged engagement with the participants and maintained his personal biases to maintain a more objective stance during data collection. Furthermore, by using multiple data collection methods, the authors were able to gather rich information from the data and also ensure dependability and confirmability. Lastly, to ensure authenticity in this contemporary study, the author faithfully reflected the feelings and tones of the participants through the interpretation of the field notes, and a detailed description of the research methodology is provided to ensure transferability [16, 20, 21].
After ethical clearance, the permission to conduct the study was granted by the Mpumalanga Department of Health after obtaining a letter of endorsement and support from the clinical facilities' Chief Executive Officers. Participants were provided with detailed consent entailing the purpose of the study, that they are not forced to participate in the research and that the study findings may be published. However, their names will not be displayed and pseudonyms were used to further ensure anonymity and confidentiality.
3. RESULTS
Table 2 shows the demographic characteristics of the participants. The interviews were conducted among midwives working in selected district hospitals. Most of the participants were women (19) between the ages of 40-59. The MPs hold various highest qualifications, with 7 holding postgraduate diplomas/honours in advanced midwifery, 4 having an R425 bachelor’s degree in nursing, 7 have an R425 diploma in nursing and lastly, 2 have an advanced diploma in midwifery. Most of the participants have more than 5 years of experience, and advanced midwives are the most experienced of all participants.
After performing a thematic analysis of the data, it was found that the study yielded two main themes and five subthemes. The themes that emerged reflect the understanding and existing triage practices of midwives in triaging women presenting in the labor ward. Fig. (1) shows the themes and subthemes that emerged below.
3.1. Theme 1: Nuanced Understanding of Triaging in Labor Wards
Triaging was described as the process of evaluating and categorizing patients according to their specific needs to determine whether they are emergencies. In addition, triage was identified as a means to prevent unexpected problems in pregnant patients who arrive at the labor and delivery units. Midwives firmly believed that by using triage, they could identify issues early and take prompt action to prevent complications. As a result, they saw triage as a positive step towards strengthening the quality of care. This was supported by the two emerging sub-themes.
3.1.1. Sub-theme 1.1: Basic Understanding of Triage and Maternal Care Guidelines
Most midwives had a diverse understanding of what triage is. They shared detailed insights into their understanding of triaging. Triage was understood as a technique to keep midwives informed of what was happening with the patients. The fundamental component that helps midwives articulate the understanding of triaging in labor is signalling out the pregnant women's needs and, thereafter, sorting them out in the level of urgency. These were supported by the following assertions;
“I think triage in the labour ward is when we place the patients according to their need of attention” P10
“Triaging is right because you will be able to know what kind of patients are waiting for you even if you are busy inside the ward. So, you will have to know which ones are urgent and which ones are not” P8
“It is the look of patients according to their needs and priorities. Looking at which patient needs to be attended like which one is emergency and which one is not.” P19
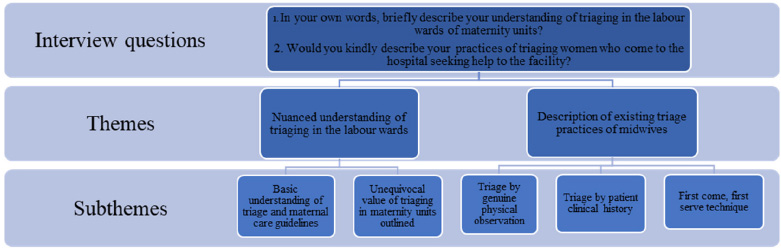
Themes and subthemes.
3.1.1.1. Another Participant Said,
“Triaging is about prioritizing patients, including risks and categorizing patients in terms of their emergencies and risks. So, you manage accordingly…” P16
On the other hand, midwives voiced that their understanding of triage was informed by their understanding of maternity care guidelines. Because while they triaged the patients, they sought guidance from maternal guidelines to provide them with information on how to manage clinical obstetric conditions. This was supported by the following narrative;
“…Also, the maternity guidelines provide us with the information on how the blood pressure is managed.” P16
Drawing from the extracts, there was an absolute shared understanding among midwives about what triaging is and why it should be implemented. One midwife continued to say she is concerned about the lack of understanding of triaging among community health centres, and it is not properly done. This is evidently drawn to the conclusion of overcapacity by low-risk patients in district hospitals.
3.1.2. Sub-theme 1.2: Unequivocal Value of Triaging in Maternity Units Outlined
The midwives understood that no matter what challenges occur within the unit, they should always be familiar with the patients’ conditions in the waiting area to prevent the occurrence of complications. The way their emotions were in sync with their understanding of triage, they viewed triage as the epitome of maternity care. Triage was regarded to be indispensable in maternity care as it can prevent unexpected complications and save both the mother and the baby. With enthusiasm, the midwives said,
“The importance of triage is that we get to save lives, yeah, sooner. You know, because if you attend, if you prioritize on admission, yeah, it's easy to first manage the high-risk patients…” P3
3.1.2.1. Other Participants Said,
“If we triage, like, checking the condition of the patient, because it will help us reduce the perinatal mortality rate to below the target because we get to start with the patients who are high risk first and see a low risk last if we do that…” P9
“The importance of triage is that we should be able to identify the high-risk patients quickly and also manage them fast enough before they complicate more than the way they came in, so it is important.” P16
“So, it is important to first sort them according to their problems so that we’re able to attend those who need help like urgent firstly and be able to avoid or prevent cases of Maternal death and also the death of babies as well” P17
Above all, triage was not only seen as a means of prioritizing patients based on the urgency of their needs but also as a practical approach to improve the overall quality of patient care and ensure timely interventions when providing maternal care. Through triage, midwives felt that they could also diagnose and detect problems early and avoid potential complications. This was supported by these quotes;
“When we triage… we improve nursing care and mortalities decrease below the target of she is in labor, so we must have triage. Meaning, even the intervention, it cannot be delayed. You can provide care fast, in time, even the intrapartum management is going to be better, it will improve.” P9
“…When we triage its better because we’re able to diagnose, see the problem and have it solved early.” P5
According to what the midwives said, triaging in the labour wards is simply beyond sorting priority cases; it is pivotal in providing optimal quality maternal care services. In essence, it ensures that these pregnant women receive the right level of attention and the appropriate amount of care at the appropriate time. In closing, it goes without saying that triage is a multidimensional approach that also ensures the well-being of both the mother and the baby; It prevents poor maternal and perinatal outcomes.
3.2. Theme 2: Descriptions of Existing Triage Practices of Midwives
Despite the detailed and comprehensive understanding of what triaging is among midwives, it was quite saddening to learn that hospitals have no standardized triage system. The participants expressed despair that they do not have set criteria or a triage tool on how to triage pregnant women. They expressed disappointment that they have mainly relied on their experience on how to triage. The absence of the triage system is supported by the following assertions;
“We don’t have triaging system currently; it is just as I said that when a patient comes in, we check them and carry on from there”. P18
3.2.1. The other Participant Commented;
“We do not have a triage criterion like at the casualty. But when you’re at the labor ward like this one…when a patient comes in, you can see that this one is ready to deliver” P13
For this effect, the participants expressed that as a result of not having a standardized triage system in their labor wards. They frequently have to rely on their own professional instincts and sometimes on the available guidelines to triage patients. This was reinforced by the following quote;
“…we are the ones that decide on how to classify a patient as a high risk based on our own assessment as we follow the available guideline.” P15
The results suggest that there is inconsistency in triage practices, which then suggests the importance of having guidelines for triage. It is also noted that the immense knowledge that participants have in providing maternal care plays a particular role in their triage. On the other hand, the midwives revealed other mechanisms to which they relied when providing patient care, predominantly when triaging.
3.2.2. Sub-theme 2.1: First-come, First-serve Techni-que
As previously stated by midwives, they highlighted the issue of not having a triage system in their labor wards. Now, that led them to rely on alternative approaches for triaging. Among the participants, there were those who voiced that they do not triage at all; they resorted to using the first come, first served method. This was supported by the following quotes;
“Normally us here, we look at who came first in line and take them…” P17
Another participant went on to say that they don’t normally prioritize. They usually take whoever comes first and provide healthcare services from there. It seems that the fact that clinical facilities do not have triage systems impacts the triage practices of midwives.
So, if we have more than three patients, they'll start with the one who came first. We don't prioritize, we check, that’s what we do normally.” P9
On the other hand, some of the midwives strongly emphasized that despite using the first-come, first-served approach services, there were circumstances where this approach was overthrown. Most of the time, it was when patients were brought by paramedics on the stretcher and classified as sick or in circumstances where the patient reports to them that she wants to bear down. In some other instances, such as when a patient was referred via the outpatient department, they also had to be prioritized.
“Maybe in case of maternity, we have those high-risk patients, like the eclamptic patient, the antepartum hemorrhage, and then also, they were cord prolapse… they don't come as a self-referral. Most of the time, they come with an ambulance, meaning they'll be accompanied by EMS personnel. Obviously, we'll start with them.” P9
“Usually, the patient is from high-risk clinic and they are being seen by doctors. And then the staff from OPD, they phone us and they tell us that there is a high risk. Let’s say P.E.T or one with a high BP. So, when they come here, they don’t get to sit at the bench but instead, they go straight to P.E.T room” P4
“Those that were, who are, who come bearing down, of course, we prioritise them as they come. As soon as they present themselves for maternity entry, we take them straight to the labour room, we assess them” P3
It would seem that although midwives have a significant understanding of triage and its unequivocal value in the provision of care. But, there remains a concerning issue of not having a triage system. This is evident by extracts showing the struggle of not having a triage system had led the midwives to use approaches that do not really have fruitful outcomes for both baby and mother. Ergo, pain and disappointment were written all over their faces as they expressed themselves. Another participant went on to say that if they had a triage tool, it would be much better because they would be able to avoid problems such as fresh stillbirths. This was an illustration of how disappointed the participants were. With a smothering face of disappointment followed by the 'Mxm' sound, one participant said;
“What can we do? you go patient by patient. Tackle the first problem, then go to the next…” P2
3.2.3. Sub-theme 2.2: Triage by Patient's Clinical History
As mentioned above, midwives relied on different approaches to triage in the labor wards. Among those approaches, triaging by history was one of them. This includes the current patient history, such as what the patient presents with at the clinical facility. Participants viewed the patient's history as an integral part of the triage because, in that way, one understands what is wrong with the patient. This was demonstrated by the following extract;
“…to me triage is that every patient that arrives in maternity must be interviewed to find out if it is a high risk or low risk patient. So, you take history. If there are patients sitting there (pointing waiting area) more than 5 or more, you first get history, subjective history to what is their problem?” P2
3.2.3.1. Another Participant Said;
“We ask them one by one, individually what are you here for? Then we get to differentiate them from the history that I’ve told you we get to know who’s an emergency case.” P7
“…we check whether the patient is complaining, the presenting problem, yeah, we check the presenting problem, whether it's either labour pains…” P11
Some of the midwives further explained that history alone does not mean that a patient is comprehensively triaged. In addition to the brief history, midwives tend to check the antenatal book and clinically assess the patients to corroborate the patient’s history. A participant mentioned that in some instances, when a patient reports vaginal bleeding, she quickly attends to that patient to confirm the bleeding, as patients often confuse blood-stained show with bleeding. This was reinforced by the following assertions;
“So, immediately, I like to check the history. And then, during the history check, you can know whether this patient needs urgent attention or not. So, if they need urgent attention, obviously, you have to make sure you start that with that patient, like your PV bleeding. Even though we're not sure about the PV bleeding because they say blood-stained show is a PV bleeding, so you have to check yourself for it.” P8
“You assess all the patients, and check their history firstly. And you check your antenatal book and check the risks of patients” P16
“I check the patient's files and ask them what they’re here for. You’ll find that the C/section x2 and yet she’s quiet so I’ll start with her. So I triage them according to their files and their needs at that moment if it is urgent or not.” P5
In the closing discussion, the extracts confirm the implication of history in the provision of holistic obstetric care. The triaging process is tangled up in history taking. The taking of patient’s history informs the planning and execution of patient-centred care. The patient's history assists in identifying the specific healthcare needs of pregnant women. Most midwives mentioned that through the patient history, that is how a midwife can determine if the patient is high-risk requiring urgent care.
3.2.4. Sub-theme 2.3: Triage by Genuine Physical Observation
A dominant concern among midwives was the lack of a standardized triage system in the labor wards and that did not make it easier for midwives to triage pregnant women. Some of the midwives expressed that they had to turn to approaches such as physical inspection of the patients. The midwives' inspections focused on identifying the signs and symptoms of hypertensive disorders in pregnancy and the advanced stage of labor. Among the signs and symptoms; pallor, swollen lower extremities, and puffy face were mentioned. This was supported by the following illustrations;
“Yeah, you assess physically. if they are still sitting there, yeah, you assess physically. If you see the pallor, oedema or swollen or puffy face, you see clinical that the patient is not well…” P3
“…we can see some of the patients by just inspection, sometimes there are signs that you can see that this patient might be a pre-eclampsia or eclampsia, you can see signs like swollen lower extremities you see” P19
The midwives continued to say that looking at the patient and seeing that the patient is restless can tell that she is in labor or about to deliver. However, it did not stop there. The inspection was followed by a clinical evaluation to confirm whether she is actually about to deliver. This was supported by the following assertions;
“…when a patient comes in, you can see that this one is ready to deliver. Others do come in and say they are ready to deliver, but when you take a look at them, you see that their faces are clean, you get what I’m saying...Then there are those who come in and say they are ready to deliver and when you take a look at them, you can see that this one needs immediate attention.” P13
“I look at those with severe pains and attend them first. I also do check if she’s not delivering.” P20
“Sometimes the person’s appearance when she is sitting there tells you, sometimes you can see that she has that urge to be down; otherwise someone might become restless and does not seem okay, then others you can see that they are calm. You can call that person and ask her to come so you can check her and see what is going on.” P12
4. DISCUSSION
Triage plays a critical role in improving maternal and neonatal outcomes, particularly in labor wards where timely interventions can prevent life-threatening complications. Maternal and child health has consistently been a significant concern, leading to high mortality rates globally. Drawing back to Sustainable Development Goals SDG 3.1, which aims to Reduce the global maternal mortality ratio to less than 70 per 100,000 live births by 2030 and goal 3.2 aims to end preventable deaths of newborns and children under 5 years of age by 2030. Hence, literature emphasizes the importance of triaging in obstetric units, which enables a more rapid response to emergencies, resulting in improved maternal and fetal surveillance [22, 23]. According to Moudi et al. [4], effective triage allows for the early identification of high-risk cases, ensuring that resources and care are allocated efficiently. Despite its importance, midwives’ understanding of triage and its application in maternity units often varies significantly, influenced by both individual knowledge and the availability of clear guidelines [12]. However, as Tukisi et al. [12] point out, midwives often lack a comprehensive understanding of triage processes, particularly when guidelines are unclear or inadequately implemented. The SATS, for example, while adapted for pregnant women, does not thoroughly address obstetric emergencies, leading to inconsistencies in how midwives apply triage in practice. In settings where staffing levels are low, this limited understanding further complicates the ability to deliver timely care, as midwives are often overwhelmed by patient loads and lack sufficient support [8]. This gap between guidelines and practice highlights the need for better training and clearer protocols to ensure that midwives have a solid foundation in triage processes tailored to the specific needs of labor wards. Just like in Tukisi et al. [12], the midwives in the current study appeared to demonstrate a diverse practice understanding of triage in maternity units.
Most midwives firmly believe that triage is a process of prioritizing patients in terms of their urgency and need. The unequivocal value of triage in maternity units is supported by numerous studies, which demonstrate that triage improves patient outcomes by enabling midwives to prioritize care based on urgency. For example, Fernandes et al. [8] assert that well-structured triage systems enhance clinical decision-making and streamline resource allocation, reducing both waiting times and the risk of adverse outcomes. Furthermore, Moudi et al. [4] highlight that triaging ensures mothers and newborns receive appropriate care at critical moments, particularly in overcrowded or under-resourced settings. Similarly, the understanding of triage by midwives is strongly related to the study of Christian [22] and Moudi et al. [4], who expanded that triage involves prioritization of patients for patient care and allocation of scarce resources to optimize maternal and neonatal outcomes. Despite these benefits, midwives often face significant challenges in implementing triage effectively. A study by Tukisi et al. [12] revealed that inadequate staff numbers and a lack of clear triage guidelines prevent midwives from fully utilizing triage tools, leading to imbalances in the midwife-patient ratio and compromising the quality of care. This underscores the urgent need for healthcare systems to invest in both human resources and the development of triage protocols that are not only easy to understand but also practical for use in the fast-paced environment of maternity units. A nuanced understanding of triage in labor wards is therefore crucial for improving decision-making and ensuring appropriate care is provided to mothers and newborns based on clinical need. While triage is a valuable tool in maternity care, its successful implementation requires a nuanced understanding of both the guidelines and the contextual factors influencing midwives’ ability to apply it effectively.
Although triage in South African obstetric departments is still a relatively new concept, midwives in this study associated their meanings of triage with their triage experiences in emergency and maternity departments. This was because most of the midwives have more than five years’ experience and hold a speciality in midwifery. Moreover, with their level of experience within the maternity units, their triage skills in the labor wards were seemingly enhanced by frequent consultation with South African Maternal Guidelines. As such, midwives viewed triage to be of significant value in patient care, and its implementation within the maternity units helps prevent unforeseen complications for pregnant women and reduces maternal and perinatal mortality. The study by Floyd et al. [23] conceded with the study findings that triaging in maternity units improves maternity quality of care and reduces care delays. Thus improving patient satisfaction. It seems that the unequivocal value of triage by midwives and other studies is related to the South African National core standards and the World Health Organisation in reducing delays in patient care and waiting times through the provision of timely care [24, 25].
Despite the understanding of triaging in maternity units by midwives, midwives were quite saddened by the lack of standardized triage systems within the labor wards. As they expressed that they lacked a triage system, instead they had to rely on an alternative practical approach. Others stated that they relied on their experiences and consultation with the South African maternal guidelines, which only inform midwives about how to manage emergency obstetric conditions, not about how to prioritize. The practices described by the participants in the current study highlight key approaches midwives use in the absence of standardized or formalized triage systems. These approaches, while pragmatic, may be insufficient to ensure the most efficient care prioritization, especially in resource-limited settings. Seemingly, before the 2020s, the lack of triage systems in maternity units was a global issue. This was supported by several studies conducted in Ghana, Iran, Uganda, and Sierra Leone that indicated that before the authors developed effective triage systems, maternity units lacked a formal triage system; instead, they used informal triage systems [4, 23, 26, 27]. In contrast to this study, Tukisi et al.’s study [12] disparage the lack of a standardized triage system in maternity units in South Africa, as it highlighted the use of a nationalized initial assessment of a patient in labor as an obstetric triage tool, seemingly this is not nationally practiced as evidenced by the voices of the midwives in lack of a standardized triage system.
However, due to the lack of a triage system, the midwives said that they normally do not prioritize; instead, they use the first-come, first-serve technique services. Naz et al. [28] conceded that adopting the first-come-first-serve technique services is commonly inappropriate in obstetric care. According to Tukisi et al. [12], midwives in Bojanala district settings resort to this approach due to high patient loads and a lack of clear triage guidelines. While first-come, first-serve technique services may seem equitable, they overlook the clinical urgency of cases, often delaying care for women with critical conditions. Moudi et al. [4] criticize the first-come, first-serve method for its potential to exacerbate adverse outcomes, as it prioritizes arrival time over medical needs. In labor wards, where conditions can rapidly deteriorate, this approach poses significant risks, particularly in cases where early intervention is necessary to prevent maternal and neonatal complications. Thus, while the first-come, first-serve technique may offer simplicity in an overburdened system, it is a suboptimal triage practice that requires re-evaluation in favor of more structured, need-based methods.
Poor triage practices seem to be problematic for all departments, including emergency departments. The recent quantitative analysis of Phukubye et al. [29] indicated a high percentage of poor triage practices among nurses in emergency departments, and ineffective triage is likely to lead to poor patient outcomes. The use of this practice could be linked to a lack of triage training and triage experience among healthcare providers [29], including midwives. This appears to contribute to maternal and perinatal mortality, as indicated by several studies that delay in care in admission at birth contributed to avoidable maternal and perinatal mortality [30]. In fact, this negatively affects public perceptions of maternity care services, evidenced by the number of litigation cases reported to the South African Nursing Council. Although some of the sources are not peer-reviewed, stories of negative public dissatisfaction about maternity care in South Africa are covered by newspapers and social networks. The number of cases related to such avoidable causes shows that there is a need to improve government policies and guidelines about triaging in maternity units in South Africa. This underscores an urgent need to involve key stakeholders, policymakers, and midwives to collaborate towards improvement quality plans to optimize the triage practices of the midwives. Therefore, this will further assist in investigating the justification of not having triage systems in South African maternity care and will be able to identify the key challenges to implementing a triage system.
Midwives further highlighted that there were some circumstances in which they overthrew the above-mentioned practice, particularly when a patient was reporting bearing down or came in accompanied by emergency medical personnel or admission through high-risk. Although this is an effective practice in prioritizing other patients, midwives seem to have little background and strategies to prioritize in labor wards. This indicates the need for standardized triage tools for midwives working in the labor wards. On a positive note, other midwives resorted to more practical triage approaches. Among these are the triaging by clinical history and physical inspection. Triage by patient’s clinical history is another method frequently employed by midwives who participated in the current study. In the realm of triaging, midwives simply check the clinical history, like asking the patient what brings them to the labor ward. Midwives said that such triage practices are sometimes accompanied by checking the maternity case records to corroborate the subjective history of the pregnant woman. Drawing from the midwives' narratives of this study, history taking is quite important as it orients the midwives toward what is wrong with the patient and makes a diagnostic assessment. The study by Peart [31] indicated that the subjective history of patients is a common part of patient care and, more importantly, is also important for triaging. This was also noted in the South African triage manual. Fernandes et al. [8] emphasize that midwives often rely on a patient's medical history as a key factor in assessing risk. This approach allows midwives to quickly identify patients who may have pre-existing conditions, complications in previous pregnancies, or other risk factors that require immediate attention. However, Tukisi et al. [12] argue that this method has limitations, particularly in settings where patient records are incomplete or unavailable, which can hinder accurate risk assessment. Additionally, relying solely on clinical history may result in the under-prioritization of women whose current conditions, despite unremarkable histories, require urgent care. Therefore, while triage by clinical history provides a more informed basis for decision-making, it is insufficient as a standalone approach and, needs to be supplemented with real-time clinical assessments and leads to inaccurate diagnoses.
Triage based on genuine physical observation is another key practice the midwives currently use to assess the condition of labouring women. This method involves the midwife making a real-time evaluation of the patient’s physical state, looking for visible signs of distress, pain levels, or abnormal vital signs. Physical observation can be a critical factor in determining the urgency of care when formal tools are absent, as noted by Fernandes et al. [8]. However, this approach relies heavily on the clinical judgment and experience of the midwife, which can vary significantly due to the number of years in the maternity units. Moudi et al. [4] argue that while physical observation is an important part of triage, it can be subjective and may not always capture the severity of an underlying condition, especially in less experienced midwives. The study of Rochana et al. [32] and Wolf et al. [33] highlighted that quick inspection was common practice even in emergency departments, as it gives clarity as to whether the patient is sick or not. However, Wolf et al. [32] argued that relying on just a quick inspection predisposes patients to risk, as that patient might lack a comprehensive assessment that might detect problems quite early. Furthermore, as Tukisi et al. [12] highlight, this method can be inadequate in busy maternity units where midwives may not have the time to thoroughly assess every patient, leading to potential misjudgements. Thus, while physical observation is a valuable tool in the triage process, its effectiveness is limited by time constraints, workload, and the individual midwife’s expertise. Drawing from the first author's experience in maternity units, this proves to be true, as not all patients will present with all symptoms or any symptoms. For example, in the case of obstetric conditions such as hypertensive disorders in pregnancy, not all patients will present puffy faces and edema, as indicated by the midwives in this study. Similarly, the study of Wolf et al. [32], recommends that midwives not only rely on quick inspection of patients but also conduct a comprehensive triage assessment, as sometimes, with simple quick inspection, a lot can be missed. This concedes with the midwives that revealed that sometimes patients scream in the waiting room, reporting an urge to bear down only to be one centimeter dilated or reporting vaginal bleeding during pregnancy, only to be blood-stained show. It seems that their skills in triaging pregnant women need sharpening for them to triage effectively as they relied on some practices that might prove to impact patients negatively. These findings suggest that there’s a need for a standardised triage system in maternity units. More efforts should be made towards improving the midwife's ineffective triage practices by developing a standardised triage system for maternity units to improve patient outcomes. This also calls for action to change of the midwifery education curriculum and maternal guidelines to include basic triage courses to optimize the midwives’ skills in triaging. Moreover, clinical institutions should also host triage training courses for midwives to enhance their triage practices.
On the other hand, it is worth considering that with current midwives' triage practices, the Sustainable Development Goal targets 3.1 and 3.2 the United Nations of reducing maternal and child mortality by 2030, and the WHO standards of quality maternal and newborn care of the provision of evidence-based practice for routine and emergency care may seem to be a little bit difficult to attain without a proper triage system in place [25]. As suggested by the WHO quality care framework for maternal and newborn healthcare, an evidence-based triage system needs to be developed in collaboration with end users and, thereafter, midwives should be trained to be competent in triaging and given support to implement the triage system [25]. However, looking at the demographic data of the study, one could conclude that the practices and understanding of triage by the midwives were influenced by the level of experience and the qualifications they hold. Hence, the experienced midwives ensured that they applied the scientific skills to inform their practices in triaging pregnant women.
5. LIMITATIONS OF THE STUDY
The lack of funding limited the study to only two district hospitals; the findings may not be representative of midwives' triage practices across a wider range of healthcare settings in South Africa or other regions, limiting the generalizability of the results. A larger number of district hospitals from different regions could help improve the generalizability of the findings. This would capture a wider variety of triage practices and experiences across diverse healthcare settings, leading to more robust conclusions. Despite some similarities between this current study and other studies conducted in emergency departments, this study's findings only reflect midwives' triage practices and understanding in the labour wards and do not reflect any other clinical department triage practices. Therefore, the study results should not be generalized to any other clinical department except the study setting. Considering that the study is qualitative in nature, it could not quantitatively measure the influence of demographic factors on the practices and understanding of midwives. This study recommends more studies to investigate sociodemographic factors influencing midwives’ prac-tices and understanding.
CONCLUSION
The current study explored the understanding and triage practices of midwives working in district hospitals of Mpumalanga Province, South Africa. The findings underscore the critical need for an effective and standardized triage system in maternity units, particularly in resource-limited settings. The absence of such systems has been shown to contribute to delays in care, poor maternal and neonatal outcomes, and increased healthcare litigation. Midwives' current triage practices, which include first-come, first-serve methods, reliance on clinical history, and physical observation, though pragmatic, are inconsistent and inadequate for addressing the complexities of obstetric emergencies. The findings highlight the importance of formal triage protocols that prioritize care based on medical urgency rather than convenience or subjective judgment. To enhance clinical decision-making and improve outcomes, the implementation of structured triage tools—tailored to obstetric care and supported by adequate staffing and resources—is essential. Furthermore, ongoing training for midwives in triage procedures and the integration of evidence-based guidelines into practice are imperative. Addressing these gaps will not only optimize maternal and perinatal outcomes but also reduce preventable maternal deaths and associated healthcare costs. Future research should focus on co-developing triage systems with midwives as key stakeholders to ensure their practical applicability and widespread adoption in maternity care settings.
AUTHOR’S CONTRIBUTIONS
M.W.N.: Conceptualized the study and collected data; M.W.N., L.M., M.M.R., and T.M.M.: Analysed and interpreted the data; L.M., M.M.R., and T.M.M.: Supervised the study; L.M. and M.M.R.: Reviewed and edited the manuscript.
LIST OF ABBREVIATIONS
| CARMMA | = Campaign for Accelerated Reduction of Maternal Mortality in Africa |
| SATS | = South African Triage Scale |
| USAID | = United States Agency for International Development |
| WHO | = World Health Organization |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study forms part of a PhD project and it was granted ethical clearance by the University of Limpopo, Turfloop Research Ethics Committee, South Africa (TREC/65/2024:PG).
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICATION
The consent to publish from the participants was obtained through detailed written consent.
AVAILABILITY OF DATA AND MATERIALS
The dataset used in this study is available upon reasonable request from the corresponding author [M.N].
ACKNOWLEDGEMENTS
The study acknowledges all the midwives who took the time to participate in this study.


