All published articles of this journal are available on ScienceDirect.
Variation in Rates of Neonatal Opioid Withdrawal Syndrome and Opioid-related Hospitalizations in New York State, 2018
Abstract
Background and Objective
Rates of neonatal opioid withdrawal syndrome (NOWS) among infants and opioid-related hospitalizations among adults have increased in recent decades. We examined rates of NOWS births and opioid-related hospitalizations among adult females of childbearing age overall and by sociodemographic and geographic factors using hospitalization data.
Methods
We used data from the New York State Inpatient Database for 2018 from the Healthcare Cost and Utilization Project. We identified infants with NOWS and opioid-related hospitalizations using diagnosis codes and calculated rates of NOWS per 1,000 live births and opioid-related hospitalizations per 1,000 hospitalizations among females of childbearing age. We compared rates by geographic and sociodemographic factors and examined the correlation between county-level rates.
Results
The NOWS rate was 4.66 per 1,000 live births, while the rate of opioid-related hospitalizations was 36.6 per 1,000 hospitalizations. There was variation by county and sociodemographic factors including urban-rural classification, race and ethnicity, insurance payer, and median income. We found the highest rates for both NOWS and opioid-related hospitalizations in non-metropolitan areas, among patients with public insurance, and among non-Hispanic White or Native American populations. There was a significant linear correlation (r=0.28; p=0.03) between county-level rates; however, only 32% of counties were concordant in quartiles for both measures.
Conclusion
Our findings indicate variation in rates of NOWS and opioid-related hospitalizations by geographic and sociodemographic factors, with only moderate concordance in county-level rates. These findings may provide a nuanced interpretation by examining measures impacting both women and infants and have important implications in prioritizing treatment access.
1. INTRODUCTION
Rates of neonatal opioid withdrawal syndrome (NOWS) have increased substantially over the last two decades, with recent national estimates of 7.3 per 1,000 births [1, 2]. Newborns with NOWS account for a growing percentage of admissions to the neonatal intensive care unit (NICU), with hospitals reporting as many as 20% of NICU admissions due to newborns with NOWS [1, 3]. However, recent NOWS management guidelines published in 2020 recommend care outside of the NICU setting to facilitate rooming-in, and other non-pharmacologic treatment approaches [4]. Prior studies have reported wide geographic variation in rates of NOWS, with higher rates in rural and lower-income areas [1, 2, 5]. Race and ethnicity are also associated with NOWS, with the highest rates among non-Hispanic White infants and the lowest among Asian and Pacific Islander infants [1, 5].
Population-level rates of opioid-related hospitalizations among adults have also increased since at least the early 2000s [6, 7]. Recent studies have reported estimates of 300 opioid-related hospitalizations per 100,000 population, with wide variation by state and region [8]. Nationally, large metropolitan areas experienced the highest rates of opioid-related hospitalizations, but rates in these areas have remained relatively stable from 2005-2016 [8]. Conversely, smaller metropolitan and rural areas experienced substantial increases during the same period [8]. There was a decreasing trend in rates from 387 per 100,000 population in the lowest income quartile to 205 per 100,000 in the highest income quartile [8].
Despite a likely association between rates of opioid-related hospitalizations and incidence of NOWS, few studies have explicitly examined ecologic relationships between these two outcomes of the opioid epidemic. Using data on hospitalizations from New York State in 2018, we examine rates of NOWS among newborns and rates of opioid-related hospitalizations among adult females of childbearing age, further stratifying these rates by sociodemographic and geographic factors. Finally, we investigate the county-level associations between rates of NOWS and opioid-related hospitalizations, hypothesizing rates of NOWS would be higher in counties with higher rates of opioid-related hospitalizations.
2. MATERIALS AND METHODS
2.1. Data Source
This study used data on inpatient discharges from January – December 2018 from the New York State Inpatient Database (SID), which is collected as part of the Healthcare Cost and Utilization Project (HCUP) and administered by the Agency for Healthcare Research and Quality (AHRQ) [9, 10]. The SID includes discharges from nearly every non-federal acute care hospital in the state and contains administrative data, including sociodemographic characteristics, geographic factors, diagnoses, procedures, and hospital utilization [9, 10]. The administrative data used in this study conforms to the definition of a limited data set under HIPAA and does not require review or approval by an institutional review board per the data use agreement.
2.2. Patient Selection Criteria
To examine the rates of NOWS births, we identified birth discharges based on newborn admission type, which includes babies born both within a hospital and those born outside of a hospital who were admitted for newborn screening or other related care. Infants with NOWS were identified by the International Classification of Diseases, Tenth Revision (ICD-10) diagnosis code P96.1 – Neonatal withdrawal symptoms from maternal use of drugs of addiction.
To examine rates of opioid-related hospitalizations, we restricted the hospitalizations to females of childbearing age, defined by the Centers for Disease Control and Prevention (CDC) age range of 18 – 44 years [11]. ICD-10 diagnosis codes identified opioid-related hospitalizations in any position (primary or secondary) for opioid use and dependence (codes beginning with F11) and poisoning and adverse effects of opioids (T40.0 – T40.4, T40.6). The entire list of included codes has been published previously using HCUP SID data from multiple states [8, 12].
2.3. Measures
We calculated rates of NOWS per 1,000 live births and rates of opioid-related hospitalizations per 1,000 hospitalizations among females of childbearing age. Rates were calculated overall and by geographic and sociodemographic factors. Geographic factors were based on patient residence and included county and an urban-rural category defined using 2013 Urban Influence Codes (UIC) consisting of four categories: large metropolitan areas with at least 1 million residents, small metropolitan areas with less than 1 million residents, micropolitan areas, and not metropolitan or micropolitan [13, 14]. Sociodemographic factors included race and ethnicity, primary insurance payer, and median household income quartile by ZIP code relative to the state income distribution. Observations with unknown or unavailable information for sociodemographic factors were retained in the sample. Geographic information was available for all counties regardless of county size, though the data use agreement prohibits reporting frequencies of 10 or fewer.
2.4. Statistical Analysis
We report unadjusted and adjusted rates and 95% Poisson confidence intervals overall and by geographic and sociodemographic factors. Poisson regression was used to estimate adjusted rates by sociodemographic factors. Adjusted models included patient race and ethnicity, insurance payor, rural/urban category, and median household income state quartile. We report incidence rate ratios (IRR) and 95% confidence intervals (CI) from adjusted models. We used the Spearman correlation to examine the unadjusted association between rates of NOWS and opioid-related hospitalizations by county. County-level rates were ranked in ascending order and divided into quartiles to describe the concordance between NOWS and opioid-related hospitalizations. All analyses were performed in SAS (version 9.4; Cary, NC). We constructed county-level maps for rates using Datawrapper [15].
3. RESULTS
3.1. Neonatal Opioid Withdrawal Syndrome
There were n=935 infants with NOWS born in New York state in 2018 and the overall rate of NOWS was 4.66 per 1,000 live births. Fig. (1A) presents the rate of NOWS per 1,000 births by county of residence (an interactive version of the same map can be found at https://datawrapper.dwcdn.net/7CZyF/1/). The median per county was 7.97 NOWS per 1,000 births (interquartile range, IQR=3.19-12.54; range 0-28.95). Four counties (Sullivan, Niagara, Washington, and Cortland) had rates over 20 per 1,000, with the highest rate in Sullivan County, which was 28.95 per 1,000. Counties in New York City had rates of NOWS births less than 5 per 1,000, except for Richmond County (Staten Island), which had a rate of 8.49 per 1,000.
Fig. (2) presents unadjusted and adjusted rates of NOWS births by sociodemographic and geographic factors. Unadjusted and adjusted NOWS rates and adjusted incidence rate ratios by sociodemographic and geographic factors are reported in full in Table 1. There was substantial variation in rates by race and ethnicity, insurance payer, urban-rural classification, and median household income quartile. Unadjusted and adjusted rates were highest among non-Hispanic White and Native American infants and lowest among Asian Pacific Islander and Hispanic infants. Infants with public insurance had unadjusted rates over five times higher and adjusted rates nearly nine times higher than those with private insurance (adjusted incidence rate ratio, aIRR=8.88; 95% CI: 7.29, 10.8). Smaller micropolitan or more rural counties had much higher rates than metropolitan areas. Compared to large metropolitan areas, counties classified as neither metropolitan nor micropolitan had unadjusted rates over three times higher, which was slightly attenuated after adjustment (aIRR=2.16; 95% CI: 1.57, 2.96). ZIP codes in lower-income quartiles also had higher unadjusted rates of NOWS than those in higher-income quartiles, though this difference was attenuated in the adjusted model.
3.2. Opioid-related Hospitalizations among Females of Childbearing Age
In 2018, there were n=14,599 opioid-related hospitalizations, with an overall rate of 36.6 per 1,000 hospitalizations among females of childbearing age. Fig. (1B) illustrates the geographic variation in opioid-related hospitalizations by county (interactive version can be found at https://datawrapper.dwcdn.net/c8xaR/1/). Per county, the median rate was 48.6 per 1,000 hospitalizations (IQR=35.43-66.67; range 12.73-219.51). Six counties had rates greater than 90 per 1,000 (Hamilton, Chautauqua, Greene, Sullivan, Ulster, and Essex), with Hamilton County being the highest in the state at 219.51 per 1,000. Counties in New York City were in the lower range with rates below 30 per 1,000, except for Richmond County (Staten Island), which had a rate of 48.8 per 1,000.
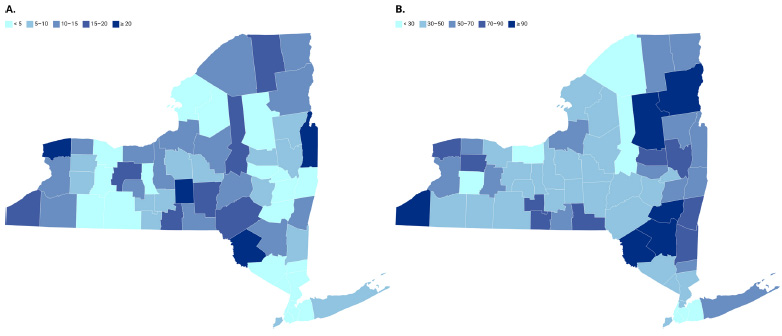
Rates of (A) NOWS per 1,000 live births and (B) opioid-related hospitalizations per 1,000 hospitalizations among females of childbearing age (18-44 years), by county in New York state, 2018.
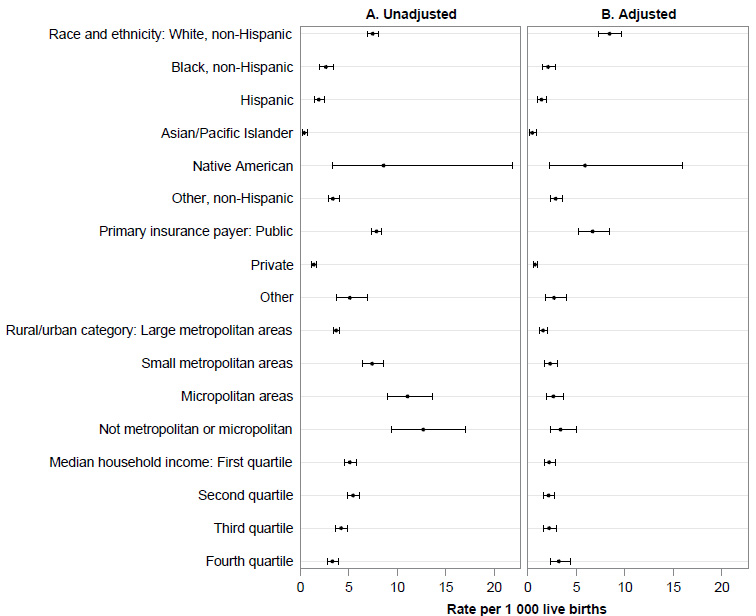
(A) Unadjusted and (B) adjusted rates and 95% confidence intervals of NOWS per 1,000 live births by sociodemographic and geographic factors in New York state, 2018.
Fig. (3) presents unadjusted and adjusted rates of opioid-related hospitalizations among females of childbearing age by sociodemographic and geographic factors. Rates and incidence rate ratios by sociodemographic and geographic factors are reported in full in Table 1. Unadjusted and adjusted rates were highest among non-Hispanic White and Native American females and lowest among Asian or Pacific Islanders. Public insurance was associated with unadjusted rates four times higher than private insurance and adjusted rates that were nearly six times higher (aIRR=5.78; 95% CI: 6.02, 5.49). Micropolitan or rural counties had higher unadjusted rates compared to metropolitan areas. Unadjusted rates in the smallest counties classified as neither metropolitan or micropolitan were twice that of large metropolitan counties with some attenuation after adjustment (aIRR=1.25; 95% CI: 1.13, 1.38). ZIP codes in the lowest income quartile also had higher unadjusted rates, though this difference was attenuated after adjustment.
3.3. Association between NOWS and Opioid-related Hospitalizations
Fig. (4) presents a scatterplot of the county-level rankings for rates of NOWS births and opioid-related hospitalizations among females of childbearing age. There was a statistically significant correlation (r=0.28; p=0.03) between county-level rates. One-third of counties (20/62; 32%) were concordant in their quartiles for opioid-related hospitalizations and NOWS. The remaining counties were discordant, though the majority (25/62; 40%) had a discrepancy of only one quartile. Two counties (3%) were in the highest (worst) quartile for opioid-related hospitalizations but lowest (best) quartile for NOWS, while 3 (5%) were in the lowest quartile for hospitalizations but highest for NOWS.
| NOWS | Opioid-related Hospitalizations | ||||||
|---|---|---|---|---|---|---|---|
| Unadjusted Rate (95% CI) |
Adjusted Rate (95% CI) |
Adjusted IRR (95% CI) |
Unadjusted Rate (95% CI) |
Adjusted Rate (95% CI) |
Adjusted IRR (95% CI) |
||
| Race and ethnicity | |||||||
| White, non-Hispanic | 7.44 (6.90, 8.02) | 8.41 (7.29, 9.70) | 1.00 (Reference) | 58.08 (56.99, 59.19) | 54.64 (52.21, 57.19) | 1.00 (Reference) | |
| Black, non-Hispanic | 2.61 (2.02, 3.37) | 2.10 (1.55, 2.85) | 0.25 (0.19, 0.33) | 21.83 (20.78, 22.92) | 14.51 (13.50, 15.58) | 0.27 (0.25, 0.28) | |
| Hispanic | 1.90 (1.45, 2.47) | 1.38 (1.01, 1.89) | 0.16 (0.12, 0.22) | 23.12 (22.06, 24.22) | 14.31 (13.34, 15.36) | 0.26 (0.25, 0.28) | |
| Asian/Pacific Islander | 0.39 (0.20, 0.77) | 0.44 (0.22, 0.90) | 0.05 (0.03, 0.11) | 4.59 (3.89, 5.42) | 4.13 (3.46, 4.92) | 0.08 (0.06, 0.09) | |
| Native American | 8.60 (3.35, 21.91) | 5.91 (2.20, 15.9) | 0.70 (0.26, 1.88) | 46.90 (35.76, 61.31) | 32.22 (24.20, 42.89) | 0.59 (0.44, 0.78) | |
| Other, non-Hispanic | 3.39 (2.88, 3.99) | 2.88 (2.31, 3.60) | 0.34 (0.28, 0.41) | 21.64 (20.37, 22.99) | 16.45 (15.21, 17.79) | 0.30 (0.28, 0.32) | |
| Primary insurance payer | |||||||
| Public | 7.84 (7.30, 8.42) | 6.67 (5.26, 8.46) | 1.00 (Reference) | 56.82 (55.83, 57.83) | 39.49 (36.96, 42.20) | 1.00 (Reference) | |
| Private | 1.38 (1.16, 1.63) | 0.75 (0.56, 1.01) | 0.11 (0.09, 0.14) | 13.91 (13.38, 14.46) | 6.85 (6.35, 7.39) | 0.17 (0.17, 0.18) | |
| Other | 5.09 (3.75, 6.89) | 2.71 (1.85, 3.96) | 0.41 (0.30, 0.56) | 32.10 (29.06, 35.45) | 18.41 (16.33, 20.77) | 0.47 (0.42, 0.52) | |
| Rural/Urban category | |||||||
| Large metropolitan areas | 3.71 (3.43, 4.01) | 1.57 (1.23, 2.00) | 1.00 (Reference) | 32.23 (31.62, 32.84) | 15.40 (14.40, 16.47) | 1.00 (Reference) | |
| Small metropolitan areas | 7.42 (6.43, 8.57) | 2.30 (1.75, 3.03) | 1.46 (1.23, 1.73) | 53.21 (51.28, 55.21) | 17.07 (15.80, 18.44) | 1.11 (1.06, 1.16) | |
| Micropolitan areas | 11.07 (8.97, 13.65) | 2.64 (1.92, 3.63) | 1.68 (1.32, 2.13) | 66.27 (62.65, 70.09) | 16.83 (15.37, 18.43) | 1.09 (1.02, 1.17) | |
| Not metropolitan or micropolitan | 12.71 (9.45, 17.07) | 3.39 (2.30, 5.00) | 2.16 (1.57, 2.96) | 65.18 (59.32, 71.58) | 19.22 (17.04, 21.69) | 1.25 (1.13, 1.38) | |
| Median household income | |||||||
| First quartile | 5.13 (4.58, 5.75) | 2.17 (1.67, 2.83) | 1.00 (Reference) | 40.71 (39.64, 41.81) | 18.15 (16.84, 19.56) | 1.00 (Reference) | |
| Second quartile | 5.43 (4.84, 6.10) | 2.11 (1.61, 2.78) | 0.97 (0.82, 1.15) | 34.64 (33.52, 35.80) | 13.59 (12.57, 14.70) | 0.75 (0.72, 0.78) | |
| Third quartile | 4.20 (3.65, 4.82) | 2.18 (1.63, 2.91) | 1.00 (0.83, 1.21) | 35.04 (33.85, 36.27) | 16.21 (14.95, 17.58) | 0.89 (0.85, 0.94) | |
| Fourth quartile | 3.34 (2.84, 3.92) | 3.23 (2.38, 4.37) | 1.48 (1.19, 1.85) | 34.85 (33.59, 36.17) | 21.27 (19.55, 23.14) | 1.17 (1.11, 1.23) | |
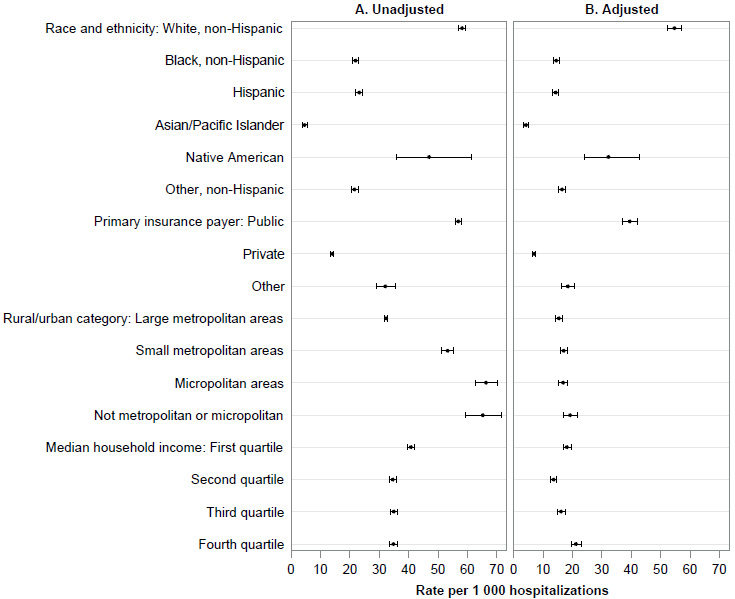
(A) Unadjusted and (B) adjusted rates and 95% confidence intervals of opioid-related hospitalizations per 1,000 hospitalizations among females of childbearing age (18-44 years) by sociodemographic and geographic factors in New York state, 2018.
4. DISCUSSION
Using data on hospitalizations in New York State in 2018, we found substantial variation in rates of NOWS and opioid-related hospitalizations among females of childbearing age by both geographic and sociodemographic factors. Consistent with our hypothesis, county-level rates of NOWS were correlated with rates of opioid-related hospitalizations, but only a third of counties were concordant with respect to the rates of NOWS and opioid-related hospitalizations. Few studies have examined these measures simultaneously to understand the broader impact of the opioid epidemic on both women and infants. Our findings may offer a nuanced interpretation to identify populations at the highest risk for adverse outcomes of opioid exposure who may have been overlooked by prior studies examining only a single measure.
We found an overall rate of NOWS just under 5.0 per 1,000 births and a median per county rate of nearly 8.0 per 1,000. These findings are similar to rates of NOWS reported by the New York State Department of Health for 2018, which indicated a rate of 9.0 per 1,000, as well as a prior study using 2017 national data, which reported a rate of 7.3 per 1,000 [1, 16]. Our findings were also similar with respect to sociodemographic differences, including higher rates among non-Hispanic White infants, residents of rural areas, lower-income ZIP codes, and those with public insurance, while rates were lowest among Asian or Pacific Islander infants, residents of large metropolitan areas, higher-income ZIP codes, and those with private insurance [1, 5].
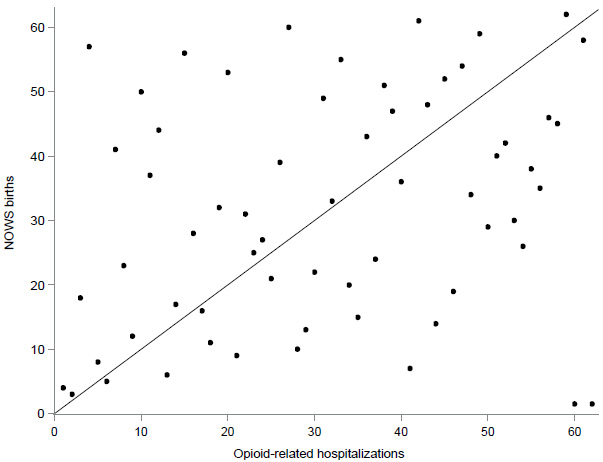
County-level rankings for rates of NOWS per 1,000 live births and opioid-related hospitalizations per 1,000 hospitalizations among females of childbearing age (18-44 years) in New York state, 2018.
We found an overall rate of opioid-related hospitalizations of 36.6 per 1,000 hospitalizations among females of childbearing age. Similar to rates of NOWS, opioid-related hospitalizations were higher in smaller cities and towns (micropolitan) or rural areas, lower income areas, non-Hispanic White and Native American females, and among those with public insurance. A prior population-based study found a rate of 4.1 per 1,000 people in New York in 2016, with higher rates in large metropolitan areas, lower income populations, and among males [8]. A 2018 report from the New York State Department of Health reported a crude rate of 1.2 per 1,000 population overall and 0.69 per 1,000 for females, with higher rates in New York City compared to the rest of the state [16]. A national study using data from the HCUP National Inpatient Sample reported estimates of nearly 2 per 1,000 hospitalizations in 2016 [6]. While we found similar sociodemographic differences to prior studies, our overall rates were higher than previously reported population- or hospital-based estimates. In addition, we found rates of opioid-related hospitalizations were highest among patients from non-metropolitan areas, which is contrary to prior studies indicating higher rates for metropolitan areas [7, 8, 12]. These differences may be explained by our geographic measures, which were based on patient residence, while prior studies have used hospital location, which may result in higher rates for larger metropolitan hospitals with larger catchment areas. In addition, our rates may not be directly comparable to prior estimates due to our age and sex-specific inclusion criteria focusing on females of childbearing age and including both primary and secondary opioid-related diagnoses, resulting in higher sensitivity.
Our findings indicate that non-metropolitan areas, including smaller cities and rural areas, had the highest rates for both NOWS and opioid-related hospitalizations, while large metropolitan areas were among the lowest. Sullivan County, a rural county within the Catskill Mountains about 100 miles from New York City, was among the worst in the state for opioid-related hospitalizations and NOWS. This finding is consistent with the New York State Annual Opioid Report for 2018, which identified this county as among the highest opioid morbidity and mortality and consistently in the highest quartile for age-adjusted mortality rate, opioid hospitalizations, emergency department visits, and NOWS, as well as a prior study using 2014 data which found this county had the highest opioid-related mortality in the state [16, 17]. Interestingly, large metropolitan counties within and adjacent to New York City had rates among the lowest in the state for opioid-related hospitalizations and NOWS, similar to county-level estimates reported in the state’s Annual Opioid Report [16]. Differences between metropolitan and non-metropolitan areas may be explained by a lack of access to treatment, particularly in rural areas, as well as, higher rates of poverty and/or other social determinants of health concentrated in rural areas [18, 19].
Overall, we found only a weak-to-moderate correlation between opioid-related hospitalizations and NOWS rates. Several possible contributing factors could explain this discordance. This may indicate under-coding or under-diagnosis of NOWS, resulting in lower rates of NOWS in counties with high rates of opioid-related hospitalizations. In addition, geographical variation in rates of pregnancy, access to contraceptive and/or abortion services, and rates of pregnancy continuation may contribute to the discordance we observed. This finding could also be explained in part by lower access to treatment for opioid use disorder (OUD) and the potential for higher utilization of illicit opioids in counties with higher rates of opioid-related hospitalizations but lower rates of NOWS births [17, 18]. Due to its shorter half-life compared to prescribed OUD treatment with methadone, prenatal exposure to heroin has been associated with less severe and shorter duration NOWS symptoms, which may not result in an ICD-coded NOWS diagnosis [20]. However, there was no information available in the HCUP data on the type of pre-natal opioid exposure or maternal access to OUD treatment such as methadone, buprenorphine, or other medication-assisted treatment.
Lack of access to OUD treatment is a growing issue and has been exacerbated by the COVID-19 pandemic, particularly in rural areas [17-19, 21-24]. While national, state, and local efforts have attempted to improve treatment access through a variety of mechanisms [18, 24, 25], a report using 2018 national data from the Substance Abuse and Mental Health Services Administration (SAMHSA) found low access to treatment based on the number of buprenorphine-waivered physicians [21]. Over 50% of counties in the U.S. had a high need for treatment services but few or no buprenorphine-waivered providers, particularly in more rural areas [21]. In New York, only Chemung County along the southern border with Pennsylvania was classified as a high-need, low-access county [21]. Interestingly, our analysis found this county had higher than average rates of opioid-related hospitalizations but only slightly elevated rates of NOWS, while several other counties with even higher rates of opioid-related hospitalizations in our analysis were not considered high need. While federal regulations requiring buprenorphine waivers were removed entirely through the Mainstreaming Addiction (MAT) Act in 2022, a major milestone in reducing regulatory barriers to OUD treatment, additional efforts are needed to improve access, availability, and equity across the continuum of care and throughout the life course [25].
This study has a number of limitations. First, the data included in this study was limited to New York State, which may not be generalizable to other states or regions. However, we chose to focus our analysis on New York as one of the most populous states, with a diverse population and large variation in county size and urbanicity from large metropolitan to rural areas. Second, this study relied on the use of administrative data, which may be incomplete regarding clinical factors such as comorbidities and/or sociodemographic factors. We identified NOWS and opioid-related hospitalizations using ICD-10 diagnosis codes, which may underestimate or overestimate the true rates due to errors in diagnostic coding and billing [26-28]. Under or overestimates in rates could result in misclassification of counties at higher risk for NOWS births and/or opioid-related hospitalizations, which may impact policy recommendations based on these findings. Third, we performed an ecological analysis examining overall rates by county and sociodemographic factors aggregated from hospitalization data and did not account for other county-level factors from the Census or other sources (e.g., unemployment rates, educational attainment, poverty rates, etc.) or individual-level characteristics (e.g., employment, educational attainment, household income, health insurance, etc.). Future studies are needed to explore associations with additional sociodemographic factors that were not available in the administrative data used in this study. Fourth, we used a sensitive measure for opioid-related hospitalizations among all females of childbearing age, rather than restricting to only delivery hospitalizations, which would likely have a higher concordance with NOWS births. We chose this measure to have a broader catchment of the population hypothetically at risk for NOWS births rather than just those currently pregnant and hospitalized at delivery. When applied to longitudinal, timely data sources, the measure definition we used could serve as a leading indicator of opioid dependence and overdoses in the population and could be helpful in forecasting trends in the incidence of NOWS births. Finally, this was a cross-sectional study using data from 2018, and therefore, our findings do not reflect any recent shifts due to the COVID-19 pandemic or other factors [22, 23]. Similar to other large publicly available datasets, data in the HCUP SID are lagged by 3 or more years [9]. Therefore, even the most recent data currently available from HCUP would not reflect recent changes later into the pandemic or post-pandemic. Longitudinal studies are needed to explore associations between rates of NOWS births and opioid-related hospitalizations over time and consider changes related to the pandemic. Despite these limitations, these findings add to the literature examining the epidemiology of perinatal opioid exposure for mothers and infants, particularly by examining measures related to both populations impacted by the opioid epidemic.
CONCLUSION
We found that non-metropolitan areas, patients with public insurance, and non-Hispanic White or Native American populations have the highest rates of NOWS and opioid-related hospitalizations in New York state, with only a weak-to-moderate correlation between county-level rates. Our findings may have important implications in prioritizing access to OUD treatment, particularly for vulnerable populations at the highest risk for adverse opioid-related outcomes. Treatment access is crucial for women of childbearing age to improve outcomes and reduce the incidence and severity of NOWS by facilitating earlier treatment initiation, ideally prior to pregnancy. By examining opioid-related outcomes in both women and infants simultaneously, our findings may inform public health policy, allowing for targeted interventions and expanded treatment access in counties and sub-populations with higher rates of NOWS and/or opioid-related hospitalizations.
AUTHORS’ CONTRIBUTION
It is hereby acknowledged that all authors have accepted responsibility for the manuscript's content and consented to its submission. They have meticulously reviewed all results and unanimously approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| NOWS | = Neonatal Opioid Withdrawal Syndrome |
| HCUP | = Healthcare Cost and Utilization Project |
| SID | = State Inpatient Database |
ETHICAL STATEMENT
The administrative data used in this study conforms to the definition of a limited data set under HIPAA and does not require ethical review or approval by an institutional review board per the data use agreement.
AVAILABILITY OF DATA AND MATERIALS
The data used in this study was acquired from the New York State Inpatient Database and is available from the Healthcare Cost and Utilization Project (HCUP), administered by the Agency for Healthcare Research and Quality. The HCUP data use agreement (available here: https://hcup-us.ahrq.gov/team/StateDUA.jsp) prohibits sharing or redistribution of the data. More information on accessing HCUP data can be found at: https://hcup-us.ahrq.gov/.
ACKNOWLEDGEMENTS
Declared none.


