All published articles of this journal are available on ScienceDirect.
Epidemiology Study of the Outbreak of Diseases Transmitted through Water and Food in Ardabil Province during the Years 2013-2022
Abstract
Background
Outbreak reporting is essential for a proper understanding of foodborne disease epidemiology. Accurate reporting makes it possible to identify the type of contaminated food, the location of the outbreak, and the factors affecting the consumption of contaminated food and to use this information in control and prevention strategies.
Objective
Therefore, this study was conducted to investigate the epidemiology of disease outbreaks transmitted through water and food in Ardabil province from 2013 to 2022.
Methods
In the current study, the statistical population included all cases of food-borne diseases recorded in all cities of Ardabil province from 2013 to 2022. The desired data were obtained from the Health Department of Ardabil University of Medical Sciences.
Results
The basis of diagnosis was all suspected patients who shared food or drinking water and shared digestive symptoms. After receiving the results of the tests of water, food, and human samples taken during the flood, the cause of the flood was determined, and the results were recorded as the final report of the flood in the portal of the Labor and Environment Health Center. After collecting the information in the researcher's checklist, it was entered into statistical software to analyze the data using statistical software. A total of 223 cases of flooding have been reported in Ardabil province. In terms of examining the months when the spread of the disease reached the maximum level, different data have been recorded. Khalkhal City, Ardabil City, and Beileh Savar City reported the highest number of floods. This prevalence was higher in urban areas and in the age group of 16 to 30 years. The dominant gender group was mostly women.
Conclusion
In most cases, the primary location was the home, and the main food consumed was kebab or broth. The causative agent remained unidentified in most patients.
1. INTRODUCTION
Nowadays, due to many reasons, diseases transmitted by water and food and the outbreaks caused by them are spreading around the world, and every year, they cause illness and death of a significant number of people [1]. According to estimates, 88% of diarrheal diseases in the world are due to the consumption of unhealthy water and the unfavorable condition of sewers, and this percentage is even higher in third-world countries [2]. Food and waterborne diseases are caused by bacteria, parasites, viruses, and prions [3]. An outbreak of a disease transmitted through food and water occurs when a group consumes contaminated food and water, leading to illness in at least two people. Thirty-one pathogens transmitted through food have been identified, and it was found that viruses are the main cause of disease and bacteria are the main cause of hospitalization and death [4, 5]. The most common causes of foodborne diseases include Listeria monocytogenes, Clostridium perfringens, Escherichia coli, Staphylococcus aureus, Salmonella enterica, Bacillus cereus, Vibrio species, and Campylobacter [6]. Foodborne diseases can cause a broad spectrum of health issues, from minor discomfort to severe conditions that may end in death [7]. The highly contagious nature of certain agents causing Shigella outbreaks, transmitted through food and water, classifies them among the second tier of bioterrorist agents [8]. Changes in food technology, lifestyle, purchasing food in large quantities, prolonged storage in refrigerators, and insufficient knowledge about food hygiene, including proper storage and cooking methods, have contributed to the increasing incidence of foodborne outbreaks [9, 10]. Another important fact is that diarrheal diseases caused by food contamination usually heal in 24 to 48 hours without any medical intervention and are usually undiagnosed and unreported. This poses a significant challenge, particularly when an active disease surveillance system is lacking, making timely response and control difficult. As a result, outbreaks can lead to human casualties and extensive material damage [11, 12]. In industrialized countries, every year, more than 30% of people are infected with food-borne diseases, and 20 people die from these diseases every year for every one million people [13]. In England, spongiform encephalopathy (mad cow disease) cost the country approximately 9 billion dollars between 1988 and 1990. In such cases, epidemiologists, unlike clinical doctors who focus on maintaining individual health, concentrate their efforts on the health of communities. In general, food-borne diseases cause illness in two ways: by invading and multiplying in the mucosal layers of the intestine and other tissues, as seen with Shigella, or by multiplying within the intestinal lumen and releasing toxins, as observed with Vibrio cholerae and E. coli. The sources of these risks include all foods and beverages consumed at home or in restaurants. Notably, other cases can cause illness differently, such as botulism in infants and children resulting from consuming honey contaminated with Clostridium botulinum [14-17]. Interesting results have been obtained in similar studies, which are discussed below. WU et al., for instance, conducted research to examine the epidemiology of foodborne disease outbreaks in Shandong Province, China, from 2011 to 2016. The findings showed that the causes of foodborne disease outbreaks in Shandong Province were as follows: 747 cases (74%) were linked to an unknown agent, 115 cases (11.4%) to poisonous plants and animals and their toxins, 36 cases (3.6%) to nitrites and nitrates, and 27 cases (2.7%) to Vibrio parahaemolyticus. Additionally, in terms of the type of food consumed, meat and its derivatives accounted for 138 cases (13.2%), aquatic products for 81 cases (7.8%), and unknown foods for 299 cases (28.7%) of foodborne diseases [18]. Mattia et al. conducted a study examining the prevalence of foodborne diseases in the United States between 2009 and 2015. The study estimates that foodborne disease agents cause around 9.4 million illnesses each year. However, only a small fraction of these diseases are well-documented. The Foodborne Disease Outbreak Surveillance System (FDOSS) collects data on foodborne disease outbreaks, defined as two or more cases of the same disease resulting from the consumption of a common food [19]. Considering the importance of the issue at the international level, it seems that the investigation of this issue in Iran can also provide appropriate information to health managers to make health decisions at the macro level.
2. METHODOLOGY
This cross-sectional epidemiological study was conducted at Ardabil University of Medical Sciences in the Department of Combating Environmental Health Diseases in 2022.
2.1. Statistical Population and Sampling Method
In the current study, the statistical population included all cases of food-borne diseases (bacterial, fungal, and viral) in all cities of Ardabil province from 2013 to 2022. Based on the population of Ardabil province from the most recent census (approximately 1.251 million people) and data from its constituent cities, efforts were made to include all foodborne diseases in the list. Data representing over 70% of the provincial population were incorporated into the study. Therefore, this study is classified as a full census study.
In the current study, the statistical population included all cases of food-borne diseases registered in all cities of Ardabil province during the years 2013-2022. The desired data were obtained from the Health Department at Ardabil University of Medical Sciences. The basis for diagnosis was that all suspected patients shared common food or drinking water and shared gastrointestinal symptoms At the end of the outbreak, the incident is analyzed, and a report is compiled by the city health center. This report includes the date and location of the outbreak, disease symptoms, the type and number of drinking water sources, the level of free chlorine in the drinking water consumed during the previous month, the time of the outbreak, the responsible entity for the water supply (e.g., city water and sewage company, rural water and sewage company, council, board of trustees, etc.), and the results of water microbial sampling conducted over the last three months. The report is submitted to the provincial health center within 24 h.
The provincial health center’s outbreak program expert uploads the collected data to the Ministry of Health’s Labor and Environmental Health Center portal. Upon receiving the results of water, food, and human sample tests taken during the outbreak, the cause is identified, and the findings are recorded as the final outbreak report in the portal of the Labor and Environmental Health Center. In the present study, the relationship between the reported outbreaks and various variables, including age, sex, disease agent, region, location of the outbreak, and time of the outbreak, was investigated. After the information was collected using the researcher’s checklist, it was entered into statistical software for analysis.
After data collection, patient information was entered into SPSS software (version 26), and variables were coded. Descriptive statistics were employed to summarize the data, presenting the mean, standard deviation, minimum, and maximum for parametric variables and frequency and percentage for categorical variables. Descriptive statistics were also used to examine the distribution of flood frequency across different variables.
| - | Frequency | % Frequency | |
|---|---|---|---|
| Year of outbreak | 2012 | 31 | 37.8 |
| 2013 | 51 | 62.2 | |
| Area | urban | 29 | 35.4 |
| rural | 53 | 64.6 | |
3. RESULTS
Table 1 shows that, in Ardabil province, 82 foodborne outbreaks were reported across 2013 and 2014, including 31 outbreaks in 2013 and 51 outbreaks in 2014.
The majority of outbreaks occurred in September and August, with 19 cases (23.2%) and 18 cases (22%), respectively (Fig. 1). The summer season had the highest total of outbreaks, with 42 cases (51.2%) (Fig. 2). Khalkhal had the highest number of outbreaks (18 cases, 22%), followed by Ardabil (15 cases, 18.3%) and Bileh Savar (13 cases, 15.9%) (Fig. 3). Outbreaks were more frequent in rural areas, with 53 cases (64.6%) compared to 29 cases (35.4%) in urban areas (Tables 1 and 2). According to Table 3, in 26 cases (31.7%), the predominant age group for outbreaks was 16 to 30 years, while in 24 cases (29.3%), the age group was not specified. The majority of outbreaks occurred in males, with 24 cases (29.3%), and females represented 41 cases (50%). The most common location of outbreaks was at home, with 57 cases (69.5%) reported in households (Fig. 4). Regarding the mode of transmission, 40 cases (48.8%) were attributed to food, 30 cases (36.6%) were of unknown transmission, and 8 cases (9.8%) were attributed to water. Additionally, 4 cases (4.9%) were associated with both food and water as the transmission sources (Fig. 5). The main contaminated food source was unidentified in 23 cases (28%), while kebab, broth, and other meat products were reported in 14 cases (17.1%). Other contaminated food sources included drinking water, fruit/juice, and chicken/poultry. The pathogen responsible for the outbreaks was unidentified in 72 cases (87.5%), while the responsible pathogen was identified in only 10 cases (12.5%) (Table 2). According to Table 4, Entamoeba histolytica was reported in 6 cases (7.3%), while pathogens such as E. coli, rotavirus, Salmonella, and Staphylococcus were each reported in one case (2.1%). According to Table 5, the average number of people infected per outbreak was 6.98, and the average number of hospitalizations was 1.30. No deaths were reported in the studied outbreaks.
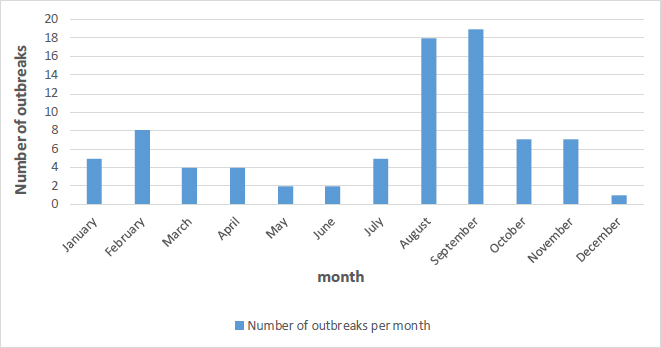
Number of outbreaks per month.
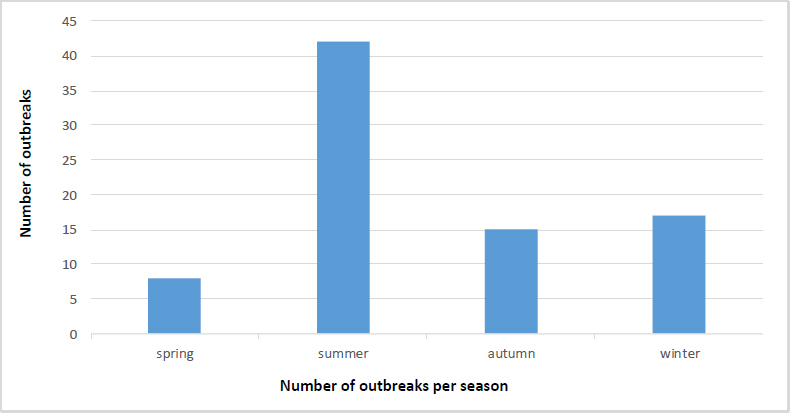
Number of outbreaks per season.
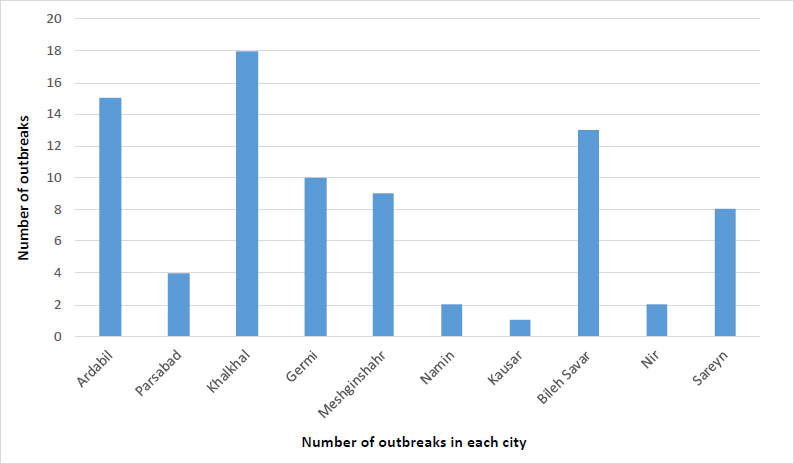
The number of outbreaks in each city.
| - | - | Frequency | %Frequency |
|---|---|---|---|
| Type of contaminated water/main food | Chicken | 5 | 6.1 |
| Kebab/broth/other meat dishes | 14 | 17.1 | |
| Eggs and other poultry | 3 | 3.7 | |
| Salad/vegetables/poisonous mushroom | 4 | 4.9 | |
| Drinking water | 8 | 9.8 | |
| Fruit/juice | 7 | 8.5 | |
| other | 11 | 13.4 | |
| Unknown | 23 | 28 | |
| Cake/dessert | 1 | 1.2 | |
| Soup | 3 | 3.7 | |
| Fish/seafood | 2 | 2.4 | |
| Sausage /other fast foods | 1 | 1.2 |
| Age Category | No Dominant Age Group | 24 | 29.3 |
|---|---|---|---|
| - | 0 to 5 years | 8 | 9.8 |
| 5 to 16 years | 4 | 4.9 | |
| 16 to 30 years | 26 | 31.7 | |
| More than 46 years | 20 | 24.4 | |
| Sex group | - | ||
| Male | 24 | 29.3 | |
| Female | 41 | 50 | |
| No dominant sex group | 17 | 20.7 | |
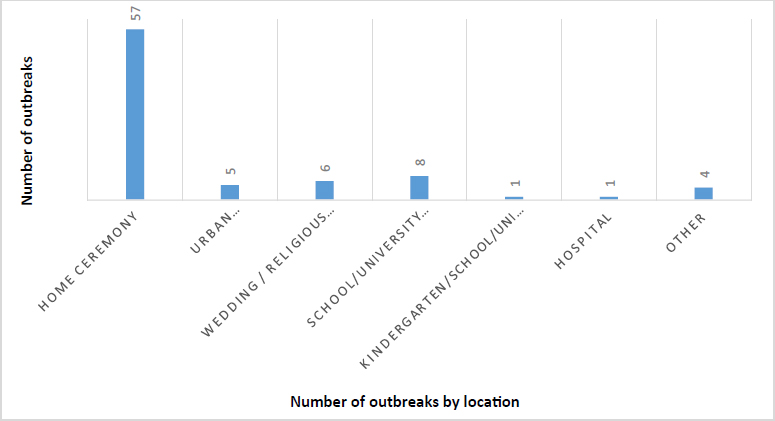
Number of outbreaks by location.
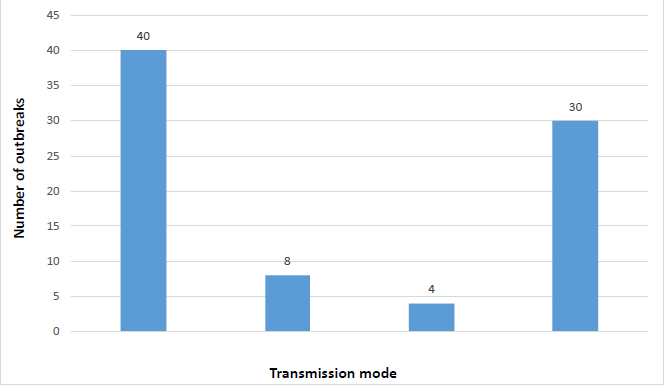
Number of outbreaks in terms of X-axis.
| Outbreak pathogen | Entamoeba histolytica | 6 | 60 |
|---|---|---|---|
| pathogenic E. coli | 1 | 10 | |
| - | 1 | 10 | |
| Rotavirus | |||
| salmonella | 1 | 10 | |
| Staphylococcal toxin | 1 | 10 |
| - | Mean | Standard Deviation | Minimum | Maximum |
|---|---|---|---|---|
| The number of patients | 6.98 | 25.81 | 0 | 234 |
| Number of hospitalizations | 1.3 | 5.71 | 0 | 51 |
| Number of deaths | 0 | 0 | 0 | 0 |
According to the data of the Health Department of Ardabil University of Medical Sciences, there were no reports of outbreaks between 2014 and 2018, which shows that the activities of the health department have been successful in preventing these outbreaks. However, 13, 34, and 94 outbreaks have been reported in 2020, 2021, and 2022, respectively.
In terms of timing, the frequency of outbreaks reached its highest number during specific seasons. For instance, in 2020, the autumn and winter seasons each accounted for the highest number of outbreaks, with 5 cases (38.4%) reported in each season. In 2021, the summer season saw the highest number of outbreaks, with 14 cases (41.17%), and similarly, in 2022, the summer season reported 41 cases (43.61%) (Fig. 6). On average, the summer season can be considered a high-risk period for an increase in the number of affected individuals (Table 6).
The table above outlines the monthly distribution of disease outbreaks, making it possible to compare the data across three-year periods.
According to Tables 7 and 8, in 2020, Bileh Savar had the highest number of outbreaks, with 4 recorded cases, and 9 out of 13 outbreaks were reported in rural areas. In 2021, Meshgin Shahr reported the most outbreaks, with 11 cases, while rural areas experienced the highest number of outbreaks, with 23 cases. In 2022, Ardabil registered the highest number of outbreaks, with 37 cases, and the urban area had the highest number of outbreaks in that year.
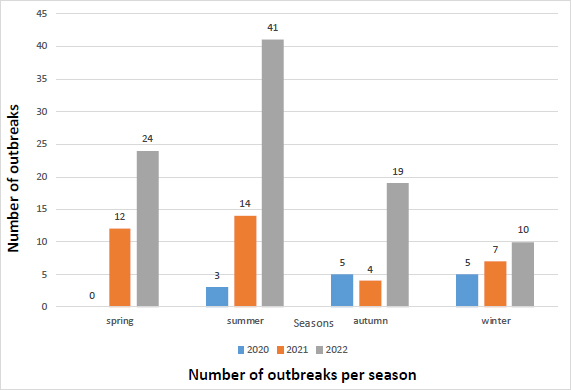
Number of outbreaks per season.
| Year/month | 2020 | 2021 | 2022 |
|---|---|---|---|
| January | 0 | 3 | 5 |
| February | 2 | 3 | 1 |
| March | 3 | 1 | 4 |
| April | 0 | 2 | 4 |
| May | 0 | 4 | 7 |
| June | 0 | 6 | 13 |
| July | 1 | 10 | 16 |
| August | 2 | 3 | 11 |
| September | 0 | 1 | 14 |
| October | 1 | 1 | 16 |
| November | 2 | 0 | 2 |
| December | 2 | 0 | 1 |
| - | 2020 | 2021 | 2022 |
|---|---|---|---|
| Ardabil | 0 | 3 | 37 |
| Parsabad | 1 | 2 | 9 |
| Khalkhal | 0 | 0 | 0 |
| Germi | 0 | 7 | 7 |
| Meshginshahr | 3 | 11 | 20 |
| Namin | 0 | 3 | 5 |
| Kausar | 0 | 2 | 3 |
| Bileh Savar | 4 | 4 | 7 |
| Nir | 2 | 2 | 1 |
| Sareyn | 3 | 2 | 5 |
| - | 2020 | 2021 | 2022 |
|---|---|---|---|
| Urban area | 3 | 9 | 48 |
| Rural area | 9 | 23 | 45 |
| The outskirts of the city | 0 | 1 | 1 |
| Nomadic area | 1 | 1 | 0 |
| Year/Source of Creation | 2020 | 2021 | 2022 |
|---|---|---|---|
| Food | 12 | 13 | 73 |
| Water | 0 | 9 | 6 |
| Watr and food | 0 | 3 | 3 |
| Uncertain | 1 | 10 | 12 |
| Symptom of Disease | 2020 | 2021 | 2022 |
|---|---|---|---|
| Acute bloody diarrhea syndrome | 0 | 0 | 1 |
| Watery diarrhea syndrome | 4 | 15 | 32 |
| Food poisoning syndrome | 9 | 19 | 61 |
According to Table 9, it is evident that the food with the highest reported cases should be considered a significant source of concern. If possible, training should be provided to the public to help prevent such occurrences in the future.
Table 10 shows that food poisoning syndrome accounted for the highest number of cases.
Additional data from the Deputy Health Ministry indicates that, in 2020, one outbreak was recorded at food preparation and distribution centers. Additionally, 8 outbreaks were linked to home ceremonies.
In 2021, two outbreaks were associated with wedding ceremonies, while the remaining cases were linked to home ceremonies. In 2022, one outbreak occurred in barracks; five were related to food preparation and distribution centers, and 86 were associated with home ceremonies. This distribution highlights the importance of maintaining proper hygiene across all settings.
4. DISCUSSION
The interconnection between climate change, environmental factors, and public health challenges related to food-borne and water-borne diseases is of paramount importance, particularly given that the highest burden of these diseases falls on children. In recent years, Africa and Southeast Asia have been identified as regions with the greatest disease burden. The quality and quantity of water significantly impact the overall burden of infectious diseases, especially in low- and middle-income countries (LMICs). Addressing these issues requires comprehensive strategies that not only target immediate health concerns but also consider the broader environmental context. The implications of climate change on disease transmission pathways necessitate a proactive approach to public health planning and intervention. Prioritizing improvements in water quality and sanitation can mitigate the adverse effects of these diseases while enhancing the resilience of vulnerable populations. In conclusion, a multi-faceted approach that integrates environmental health, public health policy, and community engagement is essential for effectively combating the challenges posed by food-borne and water-borne diseases in a changing climate [20, 21].Disease burden assessment is important for informing national, regional, and global strategies and guiding investment. The outcomes associated with unsafe water, sanitation, and hygiene (WASH) practices contribute significantly to global health challenges, accounting for approximately 2.5% of total deaths and 2.9% of global disability-adjusted life years (DALYs) across all causes [22, 23].
The results of the present study showed that the causes of outbreaks of waterborne and foodborne diseases were determined by laboratory results in only 12.5% of cases. The most common cause of these outbreaks was identified as Entamoeba histolytica. Understanding the epidemiology of foodborne diseases is essential for identifying effective methods of investigation, control, and prevention. The completeness and detail of outbreak data have significantly improved due to advancements in laboratory methods over recent years. The continued occurrence of foodborne infections calls for better foodborne disease risk reduction and control interventions. Moreover, since food can become contaminated at any point along the food processing and preparation chain, including in consumers' kitchens, interventions must be made at every stage, from farm to table [24, 25]., Furthermore, to meet the increasing demand for food driven by the growing global population, industrial-scale and centralized production systems, such as large-scale agriculture, livestock production, and food processing and distribution, have been expanded. While these systems are essential to meet food demand, they have also been associated with an increased risk of foodborne illnesses. Strategies to control microbial food safety hazards include the adoption of good agricultural practices. In addition to closely monitored production methods, it is important to implement standard operating procedures for sanitation, train employees to prevent food contamination through proper cleaning and disinfection of food-contact surfaces and equipment and ensure the prevention of cross-contamination and good personal hygiene. At the consumer level, food safety can be enhanced by following food preparation guidelines, avoiding foods commonly linked to foodborne illnesses (such as raw or undercooked meat, poultry, seafood, eggs, and raw sprouts, as well as non-disinfected fruit) to reduce the risk of foodborne diseases [26, 27]. Closer collaboration between food safety educators and the media is essential to enhance public education on food safety. This study is one of the most comprehensive investigations into the outbreak of waterborne and foodborne diseases in Ardabil province. The findings revealed that only 12.5% of flooding cases were identified with an etiologic agent, a figure that varies across countries and is generally higher in other studies. Although the identification of etiological agents has improved in recent years, a significant percentage of outbreaks still occur without the identification of the causative agent. According to a previous report from the Ministry of Health's Office of Communicable Diseases, the total number of reported outbreaks increased nationwide between 2016 and 2018 [28, 29]. Undoubtedly, increasing public education can play a significant role in reducing the incidence of water- and foodborne diseases, as well as other environmental factors. For instance, a study conducted during the COVID-19 pandemic in South Korea illustrates the impact of education on adherence to health protocols. However, the observed lack of consistent compliance with these hygiene routines over time underscores the necessity for ongoing education tailored to various demographic groups. Furthermore, a comprehensive understanding of the target community can enhance the effectiveness of educational initiatives and lead to the design of targeted interventions. This approach addresses not only immediate health concerns but also fosters long-term behavioral changes essential for disease prevention [30].
The increase in the number of foodborne disease outbreaks over recent years may reflect improvements in care, investigation, and reporting. In the current study, with the exception of botulism, which does not follow a specific temporal trend, the majority of outbreaks occurred during the summer season. These findings are consistent with those reported in similar studies [31, 32].
In analyzing the reasons behind the occurrence of such conditions within society, it is crucial to consider and focus on cultural, economic, and social factors. For example, the World Health Organization (WHO) illustrates how non-medical factors, including income, education, and working conditions, significantly influence health outcomes. It emphasizes that addressing these social determinants is vital for reducing health inequalities and improving the overall health of the population. As known, communities with limited economic resources may lack adequate healthcare facilities, increasing their vulnerability to diseases transmitted through contaminated water and food sources. Furthermore, the level of education in these communities profoundly impacts health literacy, which in turn affects individuals' ability to engage in preventive health behaviors [33].
Moreover, due to the increasing consumption of food outside the home, particularly during the summer season, and the favorable temperature and humidity conditions for the growth and reproduction of pathogenic agents, outbreaks of foodborne diseases are more common in hot seasons than in others. In the present study, the majority of outbreaks were associated with homes. However, a study conducted in South Africa found that most outbreaks were related to institutions, followed by homes. This difference may be attributed to cultural factors. While the consumption of meat-based foods was the most common cause of outbreaks, milk and dairy products, as well as the consumption of poisonous mushrooms and vegetables, contributed to only a small proportion of cases [34]. In a study conducted in China, the highest number of outbreaks was related to eating meat, and then vegetables, and the highest number of deaths was related to eating poisonous mushrooms [35]. In a study conducted by the French military, the highest number of outbreaks was related to the consumption of meat, salads mixed with sauce, and seafood [17]. In addition to the positive outcomes of such studies on public education, another important result concerns management within healthcare systems. As observed, the economic burden caused by a pandemic can severely impact healthcare systems. Senior managers can alleviate the adverse effects of such pandemics by investing in educational initiatives. Effective management of disease outbreaks, particularly in countries with healthcare personnel shortages, can not only reduce economic strain but also enhance hospitals' ability to accommodate patients. Implementing preventive measures and strengthening healthcare system capacity are essential steps in combating water- and foodborne diseases. Ongoing evaluation and adaptation of strategies will be crucial for achieving long-term public health goals [36].
Finally, further research is essential to better understand the biology, ecology, and transmission of foodborne pathogens, which will help in developing more effective pathogen control strategies. In addition, to improve the control of foodborne pathogens, additional studies are required to explore the mechanisms behind the evolution and emergence of new bacterial pathogens [37].
CONCLUSION
Foodborne outbreaks in Ardabil province during the 1990s predominantly occurred in the months of August and September, with a peak in the summer season. The cities of Khalkhal and Ardabil recorded the highest number of outbreaks. These incidents were primarily reported in urban areas and affected individuals in the 16 to 30-year age group. The female population was more commonly affected. The majority of outbreaks took place in households, and kebab/broth was the most frequently implicated food. The etiological agent remained unidentified in the majority of cases.
The rate of identifying the cause of an outbreak is a crucial indicator of the epidemiological quality of the investigation. This index is influenced by factors such as the number of samples collected and the success of testing these samples. A major challenge in the current surveillance system for waterborne and foodborne diseases lies in accurately identifying the cause of outbreaks. To address this, it is essential to conduct epidemiological studies over shorter timeframes to monitor changes in disease patterns. Given the establishment of electronic health records for Iranians in recent years, it is recommended to conduct a comprehensive study utilizing individual data from those affected by the factors contributing to outbreaks of waterborne and foodborne diseases.
AUTHORS’ CONTRIBUTION
A.D., H.Z., A.G., and M.J.: Study conception and design; A.G., H.G., and A.D.: Data collection; A.D., S.A., and H.Z.: Analysis and interpretation of results; A.D., H.Z., M.J., S.A., H.G., and A.G.: Draft manuscript. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| LMICs | = Middle-income Countries |
| WHO | = World Health Organization |
| FDOSS | = Foodborne Disease Outbreak Surveillance System |
| WASH | = Water, Sanitation, and Hygiene |
| DALYs | = Disability-adjusted Life Years |
| COVID-19 | = Coronavirus Disease of 2019 |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The study was approved by the Ethical Committee of Ardabil University of Medical Sciences, Iran (Code of ethics: with IR.ARUMS.REC.1400.123).
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
AVAILABILITY OF DATA AND MATERIALS
All the data and supporting information are provided within the article.
FUNDING
This study was funded by Ardabil University of Medical Sciences (Awards/Grant number: IR.ARUMS.REC.1400. 123).
CONFLICT OF INTEREST
Dr. Saeed Amini is the Editorial Associate Board Members of The Open Public Health Journal.
ACKNOWLEDGEMENTS
This study was extracted from the research project with IR.ARUMS.REC.1400.123 at the Ardabil University of Medical Sciences. Thus, we acknowledge the research and technology deputy of the University for the financial support.


