All published articles of this journal are available on ScienceDirect.
Knowledge, Attitudes, and Perceptions towards COVID-19 Disease and Vaccinations: A Cross-sectional Study from a Developing Country
Abstract
Background
The world has faced challenges in persuading developing nations to adopt COVID-19 vaccines. Despite initial vaccine campaigns, COVID-19 is a global health crisis, and regional and population vaccination efforts vary. Knowledge, attitudes, and views regarding COVID-19 vaccination reveal how well the community understands its value and effectiveness. Public health strategies and efforts to boost vaccination rates depend on this understanding. Thus, this study examined the knowledge, attitudes, and practices of adults from a developing country toward the COVID-19 vaccination and their post-vaccination experience.
Methods
A dual-language (Arabic and English) questionnaire was developed and validated to assess COVID-19 vaccination knowledge, attitudes, and perceptions of the participants. The study questionnaire was developed and validated as an instrument. The questionnaire was distributed via Google Forms for a cross-sectional study, and all analyses were carried out using IBM SPSS.
Results
Six hundred thirty-five participants between 18 and 60 years responded to the questionnaire. The majority of respondents were female (64.3%) and middle-income (500-1000 JOD/month) (43.9%). Chronic illnesses were absent in 87.9% of participants. At least one COVID-19 immunization was given to 90.7% of them. COVID-19-infected people had more knowledge about the disease (B= 0.537; p=0.037). Greater COVID-19 vaccine knowledge was also linked with greater monthly income (B= 0.232; p=0.032) and postgraduate education (B= 0.405; p=0.014). Postgraduate education was also associated with higher positive views of COVID-19 immunization (B= 1.160; p=0.029). COVID-19-infected people were less likely to support vaccination (B= -0.758; p=0.024).
Conclusion
The study found that individuals understand and approve of the COVID-19 vaccine. They were rational and optimistic about the COVID-19 vaccine. Various characteristics that improve vaccination knowledge, attitudes, and perceptions were also explored. To ascertain long-term COVID-19 protection, vaccination attitudes and post-vaccination experiences of the people must be assessed as knowledge and attitudes change. This information may be useful for booster dose and immunization campaign messages. Conducting and reporting studies help policymakers to make informed decisions as knowledge, attitudes, and perceptions change during pandemics.
1. INTRODUCTION
Despite the development of many COVID-19 vaccines, the world has faced a considerable challenge related to the willingness to accept them in different countries, including developing countries, such as Jordan. COVID-19 is a critical health problem worldwide, and vaccine hesitancy is a major threat to the success of COVID-19 attenuation or control programs. All population segments are susceptible to COVID-19, and the elderly with concomitant diseases seem to be most affected [1].
Beyond the disease itself, unprecedented social and economic hardships have been unveiled across the globe due to this infection [2]. Although many therapeutic compounds and drugs have been proposed and reused in the fight against COVID-19, they have remained supportive treatment options [3, 4]. Vaccines have been pivotal in reducing the incidence of infectious diseases and associated mortality [5]. They are considered one of the most cost-effective public health interventions, preventing millions of childhood diseases in the United States alone [6]. Vaccination programs have successfully controlled deadly diseases like smallpox and significantly reduced the incidence of diseases, such as tuberculosis and hepatitis B [7]. However, challenges like vaccine hesitancy and the need for adult and adolescent vaccines in immunization programs persist [8]. The COVID-19 pandemic highlighted the importance of vaccines, with public health agencies facing challenges like misinformation campaigns and supply shortages while implementing vaccination systems [9]. The public recognizes the critical role of vaccination in disease prevention and eradication, as seen in the global efforts against diseases like smallpox and the recent interest in vaccines for emerging health threats. Vaccines have advanced significantly from the innovative techniques of the 1500s to the technology currently employed in COVID-19 vaccines. Vaccines currently protect against over 20 diseases, including Ebola, cervical cancer, and pneumonia, and child mortality has decreased by more than 50 percent in the last three decades, largely due to vaccines. Nonetheless, more must be done. A significant proportion of the world's infants, one in every five, remain unvaccinated. To guarantee immunity from vaccine-preventable diseases for all children and adults, the forthcoming decades will demand international collaboration, financial resources, dedication, and foresight [10]. As of March 30th, 2023, at least 199 vaccines are in preclinical development in animals and 183 in clinical development in humans [11].
Data on knowledge, attitudes, and perception (KAP) toward COVID-19 and vaccines play an important role in determining whether a society is ready to accept measures concerning behavioral changes suggested by health authorities. KAP studies provide basic information on selecting the type of intervention needed to change myths about the disease and treatments. Evaluating the KAP on COVID-19 and vaccines in society will help create better planning and strategies for preventing insufficient and/or misinformation about the disease and its protective measures, such as vaccines, and for developing health promotion programs [12]. By 2024, the field of public health has successfully adjusted to the ongoing presence of COVID-19, which has become endemic. Despite the decline of the pandemic, it is still crucial to examine the knowledge, attitudes, and behaviors of the population toward vaccination (KAP). This study thoroughly examines the knowledge, attitudes, and practices (KAP) of Jordanians at the beginning of the COVID-19 vaccination campaign. It establishes an essential historical reference point for present and future public health strategies. The continual emergence of novel COVID-19 variants necessitates focused attention and flexibility of the public health authorities. This study, conducted throughout a pivotal vaccination effort, highlighted the level of acceptance and opposition among the Jordanian population. These insights are essential for determining public health messages and implementing strategies to address and reduce future variant concerns. In addition, our study also offers the opportunity for comparison and trend analysis. Health authorities can enhance their comprehension of public health engagement and vaccination rates by monitoring the evolution of public attitudes and knowledge. This is crucial for formulating strategies to improve future immunization initiatives for COVID-19 and other contagious diseases that pose a threat to public health. Additionally, our discoveries contribute to global knowledge and capabilities in responding to pandemics. Their distinct viewpoint from Jordan, a nation with its own socio-economic and cultural contexts, enhances the worldwide discourse on handling public health crises. Our insights can inform public health strategy and implementation in places with comparable cultural and structural dynamics. To effectively address vaccination hesitancy and acceptance, it is crucial to comprehend the underlying factors that contribute to it. This study has identified beliefs and cultural barriers that can be used to guide public health education and behavioral interventions.
The current study investigates KAP toward COVID-19 vaccination among Jordanian adults as a representative developing country facing specific vaccine uptake challenges. This research is particularly significant in the context of the need to reduce the pandemic's burden and prevent further health crises. In this way, the aim is to uncover actionable insights by investigating multi-faceted influences on vaccination behavior, given the socioeconomic factors and past health experiences of the people. Insights from this will help improve public health strategies for better vaccine acceptance. This research, therefore, underlines the critical factors that determine vaccine hesitancy and acceptance with an extensive analysis of a large, diversified sample, which is very important in the design of effective public health campaigns tailored to the needs and concerns of populations in similar settings.
Our approach assists policymakers in identifying gaps in both information and attitudes. Knowing the areas where educational and health resources are required is crucial for effectively distributing resources to promote an educated and receptive population. This study analyzes Knowledge, Attitudes, and Practices (KAP) towards COVID-19 vaccination. It aims to enhance understanding of past and current challenges and provide the necessary knowledge to respond effectively to future public health crises. By drawing lessons from the pandemic, a more knowledgeable and adaptable public health system capable of successfully and efficiently managing future epidemic threats can be established.
2. METHODOLOGY
2.1. Study Design
This was a cross-sectional study involving Jordanian adults aged 18 to 60. The exclusion criteria consisted of individuals who refused to consent, non-Jordanians, Jordanians who were not currently residing in Jordan, and participants who filled out the questionnaire more than once. With an acceptable margin of error set at approximately 0.5, the recommended sample size for the study was 585 participants. Assuming a 10% rate of incomplete responses, the final sample size for the study was determined to be 635 participants.
2.2. Ethical Approval
This study received approval for implementation by the Jawatankuasa Etika Penyelidikan Manusia Universiti Sains Malaysia (JEPeM-USM) and has been assigned a study protocol code (USM/JEPeM/21110726). The study protocol also received approval from the Institutional Review Board (IRB) committee at Jordan University of Science and Technology and has been assigned a study protocol code (156/147/2022). This research was conducted on humans by the Helsinki Declaration of 1975, as revised in 2013 (http://ethics.iit.edu/ecodes/node/3931).
2.3. Questionnaire Development
The questionnaire was self-developed except for two questions (21 and 39) that were obtained based on previous studies [13, 14]. Briefly, the questions were formulated in 4 domains.
Domain 1 covered the general demographics and characteristics (age, gender, marital status, employment, occupation, living conditions, location and place of residence, income, education level, medical history, nationality, and three general questions about their previous experience with COVID-19) of the participants.
Domain 2 was about the knowledge of participants of COVID-19 and its vaccinations. This domain was categorized into two subdomains: Subdomain 1: assessing the participants’ general knowledge about the COVID-19 disease, which contained one item that was divided into eight subitems on a five Likert scale from strongly agree to strongly disagree and 14 items with multiple choice answers (various answers may apply). Meanwhile, subdomain 2 assessed the general knowledge of participants about the COVID-19 vaccination. This subdomain was aimed to evaluate the understanding of study participants about many aspects, such as the general knowledge about the COVID-19 vaccinations, symptoms, real complications, and myths, as well as the most trustable source of knowledge about the COVID-19 vaccine. It contained 1 item on a five-point Likert scale from strongly agree to strongly disagree, six items with multiple choice answers (various answers may apply), and three items with Yes/No answers.
Domain 3 was about the perceptions and attitudes of the participants. This domain included eight items about taking the COVID-19 vaccines, covering their attitude and perception toward administering the vaccines to their children or the elderly who depend on them or can be influenced by their opinions.
Domain 4 was formulated in the multi-question form to understand the reasons behind vaccination hesitancy, if it exists, and consequently to highlight probable techniques and recommendations to increase vaccination acceptance.
2.4. Questionnaire Translation
The developed English version of the questionnaire was translated into Arabic using the forward and backward translation process. The purposive sampling method was used to recruit four translators who fulfilled the following inclusion criteria: a) an individual with educational qualification of at least a PhD degree; b) a native Arabic speaker for forwarding translator and a native English speaker for the backward translator; c) bilingual in Arabic and English. All the translators recruited were among the professionals and faculty members at Jordan University of Science and Technology.
While forwarding the translation, two translators independently translated the original English version of the questionnaire to the Arabic version. A discussion involving the translators and researchers was held to achieve a consensus on the differences between the two translation versions and to produce a single harmonized Arabic version of the questionnaires. During backward translation, two other translators independently translated the harmonized Arabic version of the questionnaire from Arabic to English. Both backward versions of the questionnaire were reviewed and compared against the original English version to evaluate the equivalency of concepts. Any contradiction in the meaning between backward and original versions was reviewed. Items in the Arabic version that did not share a similar intention to the original version were re-worded and revised in producing the final version.
2.5. Face Content Questionnaire Validation
Face content validation was carried out for both Arabic and English questionnaires and began immediately after translation by ten professionals consisting of faculty members at Jordan University of Science and Technology with at least five years of working experience in the healthcare sector, who were bilingual speakers and had at least an educational qualification of bachelor’s degree in medical or pharmacy background [15]. Experts who fulfilled the inclusion criteria were recruited using purposive sampling for the content validation of both versions.
All experts on the panel were given a copy of both versions and the content validity feedback form to evaluate the English and Arabic versions of the questionnaires based on four criteria of the Content Validity Index (CVI). Experts were asked to rate each item on the scale according to these four criteria: relevance, simplicity, clarity, and ambiguity, using the 4-point Likert scale, where a score of 1¼ was considered not relevant, 2¼ indicated that the item needs some revision, 3¼ suggested that the item was relevant but needed minor revision, and 4¼ indicated that the item was very appropriate.
After completion of the content validation, the questionnaires were revised and modified based on the constructive feedback provided by the expert panel. Items were aimed to be removed if more than one expert agreed that the item was irrelevant (did not happen). Other than that, any item with an average rate of less than 4¼ was reviewed and modified, when necessary, after discussion with the investigator panel. The final English and Arabic versions of the questionnaires were then produced.
2.6. Pilot Study
A pilot study was conducted on 75 participants who responded to the questionnaire during the pilot study and were aged 18-60. Consequently, regarding the sample size for the pilot/validating study, more than 10% of the total estimated sample size was involved in the pilot study [16]. Therefore, a minimum of 39 participants were recruited by distributing the questionnaire on WhatsApp private groups, including Jordan University of Science and Technology staff and students who filled out the questionnaire on Google Forms, with a copy of the administered questionnaire both in Arabic and English. Cronbach’s alpha was not less than 0.65 for any questionnaire items.
The staff were chosen carefully to represent various backgrounds; some had bachelor's degrees (students), master’s degrees, and Ph.D. degrees, workers, farmers, labor workers, diploma degrees, non-college degree holders, and elderly employees. It should be noted that the retirement age of workers in Jordan is 70 years.
To avoid the questionnaire being answered twice by the same person, the survey was distributed privately to private groups and sent in private messages to ensure that the questionnaire was filled out once. At the end of the questionnaire, the participants were also asked whether they had filled it out. Those questionnaires with a “yes” answer to the previous question, if any, were excluded from the study.
The first page of the online questionnaire described and summarized the purpose of the study. Before the questionnaire was given to the participants, they were asked to sign a consent form of participation. The first questions also asked about the participants' age, nationality, and current residency status to fulfill the inclusion/exclusion criteria.
2.7. Data Collection
A validated questionnaire was distributed on WhatsApp and Facebook via Google Forms, with copies in Arabic and English. This study used the purposive sampling method to recruit participants to understand the knowledge, attitude, and practice of COVID-19 vaccination among Jordanian adults. Purposive sampling was used to gather detailed and relevant information from persons representative of the population most affected or concerned with vaccination policies.
2.8. Statistical Analysis
The data were analyzed using SPSS Statistics for Windows, version 28.0, Armonk, NY, USA. The data on categorical variables are summarized in percentages, and the data on continuous variables are summarized in mean and standard deviation (SD).
The COVID-19 disease knowledge score was calculated by summing the responses to the five respective items (K1, K3, K4, K6 (inverted), and K8). Higher scores indicate higher knowledge (range: 5–25). To calculate the knowledge score of the COVID-19 vaccine (including items 26, 27, 28, and 30), the correct answers were given a score of 1, and the incorrect or do not know answers were given a score of 0 (range of correct answers: 0-4). In the question about the possible side effects of the vaccines, the participants were considered to have given a proper answer if they identified at least two side effects of the vaccines.
The 'attitudes and perceptions of COVID-19 vaccination' score was calculated by summing up the responses on items A2, A3, A12, A13, and A14. Higher scores indicate more positive attitudes and perceptions towards the COVID-19 vaccination (total score range: 5–25).
Generalized linear models were used to analyze the extent to which the sociodemographic and health characteristics of the participants could predict COVID-19 disease knowledge, COVID-19 vaccination knowledge, and the attitudes and perceptions of COVID-19 vaccination. Coefficients, 95% confidence intervals (95% CI), and p-values are presented. p values <0.05 were considered statistically significant.
3. RESULTS
The sociodemographic and health characteristics of the participants are summarized in Table 1. A total of 635 individuals participated in the study, with a mean age of 29.5±7.60. The majority being women (64.3%). Most participants had an undergraduate degree (76.0%). Almost all the participants were Jordanian nationals (95.3%) and lived in urban areas in Jordan (94.9%). A significant number of the participants were unemployed (62.8%) and nonsmokers (74.1%). Regarding monthly family income, 43.9% of participants fell within the middle-income range of 500-1000 JOD/month. Most participants did not report having any chronic diseases (87.9%), and 90.7% had received at least one dose of the COVID-19 vaccine. Only a tiny percentage of the participants reported being currently infected with COVID-19 (1.1%), while a larger percentage reported having been infected at some point (64.2%).
| - | - | n (%) |
|---|---|---|
| Gender | Female | 407 (64.3) |
| Male | 226 (35.7) | |
| Place of residence | Urban | 463 (73.0) |
| Rural area or village | 171 (27.0) | |
| Marital status | Single | 460 (72.7) |
| Married | 161 (25.4) | |
| Divorced/widowed | 12 (1.9) | |
| Monthly family income (JOD) | <500 | 187 (29.8) |
| 500 - 1000 | 275 (43.9) | |
| >1000 | 165 (26.3) | |
| Educational level | Primary School | 3 (0.5) |
| High School | 38 (6.0) | |
| Professional Diploma | 17 (2.7) | |
| Undergraduate Degree | 481 (76.0) | |
| Postgraduate Degree | 94 (14.8) | |
| Employment status | Employed | 212 (34.9) |
| Unemployed | 381 (62.8) | |
| Retired | 14 (2.3) | |
| Smoking status | Yes | 164 (25.9) |
| No | 468 (74.1) | |
| Chronic diseases | None | 546 (87.9) |
| At least one | 75 (12.1) | |
| Influenza vaccination (yearly) | Yes | 557 (88.1) |
| No | 75 (11.9) | |
| COVID-19 vaccination (ever) | Yes | 573 (90.7) |
| No | 59 (9.3) | |
| Currently infected with COVID-19 | Yes | 7 (1.1) |
| No | 606 (95.7) | |
| Don’t know | 20 (3.2) | |
| Ever been infected with COVID-19? | Yes | 405 (64.2) |
| No | 226 (35.8) |
| - | Strongly Agree | Agree | Neutral | Disagree | Strongly Disagree | - |
|---|---|---|---|---|---|---|
| n (%) | Mean (SD)* | |||||
| • I think that COVID-19 actually exists | 253 (40.5) | 237 (38.0) | 108 (17.3) | 18 (2.9) | 8 (1.3) | 4.14 (0.89) |
| • COVID-19 has several negative consequences that extend beyond direct effects on health | 203 (32.6) | 278 (44.6) | 117 (18.8) | 19 (3.0) | 6 (1.0) | 4.05 (0.85) |
| • COVID-19 is life-threatening and can cause death | 239 (38.4) | 261 (41.9) | 93 (14.9) | 23(3.7) | 7 (1.1) | 4.13 (0.88) |
| • COVID-19 is like other viruses; it does not need this media hype | 74 (11.9) | 164 (26.4) | 213 (34.2) | 113 (18.2) | 58 (9.3) | 2.87 (1.13) |
| • There is a remarkably effective COVID-19 vaccination available | 84 (13.6) | 219 (35.4) | 237 (38.3) | 45 (7.3) | 34 (5.5) | 3.44 (1.00) |
| Total | - | - | - | - | - | 18.62 (2.85) |
3.1. Knowledge of COVID-19 and Vaccine Hesitancy
Overall, participants in this study demonstrated high levels of knowledge of COVID-19 disease (mean (SD) = 18.62 (2.85), range: 5-25) (Table 2) but exhibited limited knowledge of COVID-19 vaccination (average number of correct answers = 2.03 (1.12), range: 0-4) (Table 3).
When asked about COVID-19 as a disease, most of the participants agreed or strongly agreed that COVID-19 exists (78.5%) and that it is life-threatening and can cause death (80.3%). However, a relatively small percentage of the participants (27.5%) disagreed or strongly disagreed with the statement that COVID-19 is like other viruses and does not need this media hype.
When asked about COVID-19 vaccination, a high percentage of respondents (63.6%) provided incorrect answers to questions about the resemblances of the available vaccines regarding manufacturing and action and their capacity to protect from COVID-19 (57.1%).
| - |
Correct Answer |
Incorrect Answer |
|---|---|---|
| n (%) | ||
| • Do you think that COVID-19 vaccines are safe? | 285 (45.7) | 338 (54.3) |
| • Do you think that the available vaccines can protect from COVID-19? | 268 (42.9) | 357 (57.1) |
| • In terms of manufacturing and action, do you think all vaccines are the same? | 227 (36.4) | 396 (63.6) |
| • What are the possible side effects of the vaccines? | 448 (75.2) | 148 (24.8) |
| Total | 2.03 (1.12) | |
| - | Strongly Agree | Agree | Neutral | Disagree | Strongly Disagree | - |
|---|---|---|---|---|---|---|
| n (%) | Mean (SD)* | |||||
| • Not getting vaccinated will affect your job | 178 (29.9) | 208 (34.9) | 125 (21.0) | 49 (8.2) | 36 (6.0) | 2.26 (1.15) |
| • Do you believe that a booster dose in Jordan will be available to a selected group rather than to the community? | 76 (12.9) | 145 (24.6) | 270 (45.8) | 56 (9.5) | 42 (7.1) | 2.73 (1.04) |
| • You may have severe complications and side effects from the COVID-19 vaccine | 100 (17.2) | 184 (31.6) | 216 (37.1) | 61 (10.5) | 21 (3.6) | 2.52 (1.01) |
| • COVID-19 vaccine may be faulty or fake | 93 (15.9) | 150 (25.6) | 252 (43.0) | 59 (10.1) | 32 (5.5) | 2.64 (1.04) |
| • COVID-19 vaccine is being promoted for the commercial gains of the pharmaceutical companies | 115 (19.7) | 159 (27.2) | 245 (41.9) | 40 (6.8) | 26 (4.4) | 2.49 (1.02) |
| Total | - | - | - | - | - | 12.64 (3.64) |
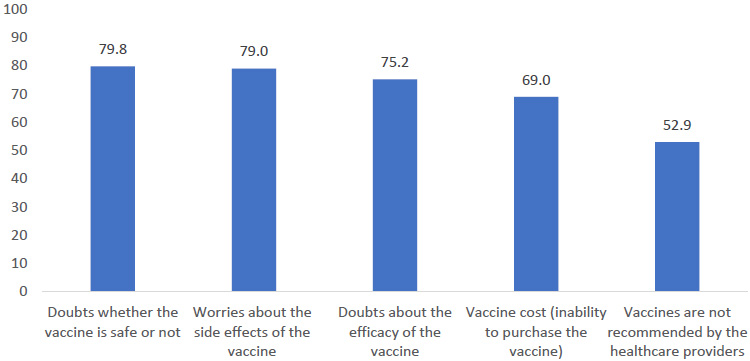
Reasons for hesitancy to take the COVID-19 vaccine.
3.2. Attitude and Perception towards COVID-19 and Vaccine Hesitancy
Participants presented a moderate attitude and perception toward COVID-19 vaccination (mean (SD) = 12.64 (3.64), range: 5-25) (Table 4). A majority strongly agreed or agreed that not getting vaccinated would affect their job (64.8%). Moreover, a high proportion considered that severe complications and side effects may happen after taking the COVID-19 vaccine (48.8%) and that the vaccine is being promoted for the commercial gains of pharmaceutical companies (46.9%).
Participants reported that some factors may justify their hesitancy to take the COVID-19 vaccine. Those factors included doubts about whether the vaccine is safe (79.8%), worries about the vaccine's side effects (79.0%), and doubts about the vaccine's efficacy (75.2%) (Fig. 1).
3.3. Factors associated with COVID-19 Disease Knowledge
Higher knowledge of COVID-19 disease was found among those who have ever been infected with COVID-19 compared to those who have not been infected (B= 0.537; p=0.037) (Table 5). No other sociodemographic or health characteristics appeared to be associated with knowledge of COVID-19 disease in this study.
| - | - | Coefficient | 95% CI | p-value |
|---|---|---|---|---|
| Gender | Female | 1 | - | - |
| Male | -0.131 | -0.675 to 0.414 | 0.638 | |
| Age (years) | 18-29 | 1 | - | - |
| 50-60 | -0.085 | -1.044 to 0.874 | 0.862 | |
| Place of residence | Urban | 1 | - | - |
| Rural area or village | 0.454 | -0.101 to 1.009 | 0.109 | |
| Marital status | Single, divorced, widowed | 1 | - | - |
| Married | -0.359 | -1.232 to 0.515 | 0.421 | |
| Monthly family income (JOD) | <500 | 1 | - | - |
| ≥500 | 0.463 | -0.076 to 1.003 | 0.092 | |
| Educational level | Undergraduate | 1 | - | - |
| Postgraduate | 0.470 | -0.336 to 1.275 | 0.253 | |
| Employment status | Employed | 1 | - | - |
| Unemployed/retired | 0.021 | -0.590 to 0.633 | 0.946 | |
| Smoking status | No | 1 | - | - |
| Yes | -0.344 | --0.938 to 0.250 | 0.256 | |
| Chronic diseases | None | 1 | - | - |
| At least one | 0.627 | -1.129 to 1.384 | 0.104 | |
| Influenza vaccination (yearly) | Yes | 1 | - | - |
| No | 0.046 | -0.705 to 0.798 | 0.904 | |
| COVID-19 vaccination (ever) | Yes | 1 | - | - |
| No | -0.329 | -1.166 to 0.507 | 0.440 | |
| Ever been infected with COVID-19? | No | 1 | - | - |
| Yes | 0.537 | 0.033 to 1.040 | 0.037 |
| - | - | Coefficient | 95% CI | p-value |
|---|---|---|---|---|
| Gender | Female | 1 | - | - |
| Male | 0.170 | -0.046 to 0.387 | 0.122 | |
| Age (years) | 18-29 | 1 | - | - |
| 50-60 | -0.245 | -0.616 to 0.126 | 0.196 | |
| Place of residence | Urban | 1 | - | - |
| Rural area or village | 0.089 | -0.129 to 0.306 | 0.425 | |
| Marital status | Single, divorced, widowed | 1 | - | - |
| Married | -0.079 | -0.416 to 0.259 | 0.649 | |
| Monthly family income (JOD) | <500 | 1 | - | - |
| ≥500 | 0.232 | 0.020 to 0.444 | 0.032 | |
| Educational level | Undergraduate | 1 | - | - |
| Postgraduate | 0.405 | 0.083 to 0.727 | 0.014 | |
| Employment status | Employed | 1 | - | - |
| Unemployed/retired | -0.116 | -0.356 to 0.125 | 0.347 | |
| Smoking status | No | 1 | - | - |
| Yes | -0.285 | -0.517 to -0.054 | 0.016 | |
| Chronic diseases | None | 1 | - | - |
| At least one | 0.171 | -0.126 to 0.468 | 0.259 | |
| Influenza vaccination (yearly) | Yes | 1 | - | - |
| No | 0.180 | -0.108 to 0.468 | 0.221 | |
| COVID-19 vaccination (ever) | Yes | 1 | - | - |
| No | -0.704 | -1.035 to -0.373 | <0.001 | |
| Ever been infected with COVID-19? | No | 1 | - | - |
| Yes | -0.078 | -0.277 to 0.121 | 0.444 |
| - | - | Coefficient | 95% CI | p-value |
|---|---|---|---|---|
| Gender | Female | 1 | - | - |
| Male | -0.060 | -0.777 to 0.656 | 0.869 | |
| Age (years) | 18-29 | 1 | - | - |
| 50-60 | -0.713 | -1.976 to 0.550 | 0.269 | |
| Place of residence | Urban | 1 | - | - |
| Rural area or village | 0.444 | -0.275 to 1.164 | 0.226 | |
| Marital status | Single, divorced, widowed | 1 | - | - |
| Married | 0.641 | -0.513 to 1.795 | 0.276 | |
| Monthly family income (JOD) | <500 | 1 | - | - |
| ≥500 | 0.183 | -0.527 to 0.893 | 0.614 | |
| Educational level | Undergraduate | 1 | - | - |
| Postgraduate | 1.160 | 0.119 to 2.200 | 0.029 | |
| Employment status | Employed | 1 | - | - |
| Unemployed/retired | -0.075 | -0.889 to 0.739 | 0.857 | |
| Smoking status | No | 1 | - | - |
| Yes | -0.677 | -1.455 to 0.101 | 0.088 | |
| Chronic diseases | None | 1 | - | - |
| At least one | 0.314 | -0.680 to 1.309 | 0.535 | |
| Influenza vaccination (yearly) | Yes | 1 | - | - |
| No | -0.715 | -1.713 to 0.284 | 0.161 | |
| COVID-19 vaccination (ever) | Yes | 1 | - | - |
| No | -0.585 | -1.679 to 0.508 | 0.294 | |
| Ever been infected with COVID-19? | No | 1 | - | - |
| Yes | -0.758 | -1.418 to -0.098 | 0.024 |
3.4. Factors associated with COVID-19 Vaccination Knowledge
Having a higher monthly income (B= 0.232; p=0.032) and a postgraduate educational level (B= 0.405; p=0.014) were associated with higher COVID-19 vaccination knowledge (Table 6). Those who had never taken the COVID-19 vaccination and those who were smokers were likely to present less vaccination knowledge (B= -0.704; p<0.001 and B= -0.285; p=0.016, respectively).
3.5. Factors associated with Attitudes/Perception of COVID-19 Vaccination
A postgraduate educational level (B= 1.160; p=0.029) was associated with more positive attitudes and perceptions toward COVID-19 vaccination (Table 7). Those infected with COVID-19 were more likely to present fewer positive attitudes and perceptions toward COVID-19 vaccination (B= -0.758; p=0.024).
4. DISCUSSION
Assessing Knowledge, Attitudes, and Practices (KAP) towards COVID-19 vaccination remains pertinent as the vaccination landscape is dynamic, with the emergence of new variants and ongoing research. Understanding the current state of public knowledge helps tailor communication strategies to address misconceptions. Additionally, assessing attitudes towards vaccination is crucial for identifying barriers and facilitators to vaccine acceptance. This information aids in developing targeted interventions to improve vaccine uptake. As vaccination campaigns evolve, regular assessments of practices provide insights into the implementation of vaccination programs and identify areas for improvement. Moreover, monitoring KAP over time enables researchers and healthcare professionals to gauge the effectiveness of public health initiatives, adapt strategies based on changing circumstances, and ensure ongoing community engagement.
Unlike previous studies (at the time of generating this questionnaire in late 2021) [13, 17], the current study gathered the latest information and facts about the COVID-19 disease, including myths, complications, signs, and symptoms, the right actions to take when suspicious about being infected, being infected, or when other family members got infected, and the recently used protective measures. It also included the latest information about the available vaccines, their known actions, side effects, myths about them, fears of them, attitudes and perceptions toward the booster dose, and some known or anticipated causes for vaccination hesitancy.
This information is a foundation for public education, enabling individuals to recognize the importance of preventive measures and take appropriate actions when suspicious of infection. The findings of this study contribute to informed decision-making regarding personal health and safety by addressing misconceptions and providing accurate information. Moreover, by understanding and implementing the latest protective measures, individuals contribute to the collective effort to curb the transmission of the virus.
This study gathered information on the KAP of mainly young adults living in cities. The vast majority reported earning less than JOD 1000 per month, being employed, and holding a higher degree. This is comparable to several previous studies on adults from Jordan [17-20]. The findings also showed a lack of significance in knowledge about the COVID-19 disease across most demographic variables. This is expected given that this disease has been the central issue in our lives in recent years.
Yet, more knowledge of COVID-19 disease was found among those infected with COVID-19 compared to those who have not been infected. Moreover, having a higher monthly income and a postgraduate educational level were associated with higher COVID-19 vaccination knowledge, which is in line with recent studies in Jordan [20], where higher incomes were found to be linked to higher education levels, and younger adults may be more knowledgeable, as mentioned previously [21, 22]. Another possibility is that postgraduate education could be correlated with more general knowledge, an ability to learn about new things and a better understanding of life matters. For example, a previous study reported that people with higher education are more likely to take vaccinations because they have more medical knowledge, greater access to pertinent information sources, and fully understand their importance for good health [23-33]. Moreover, the UCL COVID-19 social study of the UK reported that distrustful attitudes towards vaccination were higher amongst individuals with lower levels of education [34].
On the other hand, those who had never taken the COVID-19 vaccination and those who were smokers were likely to present less vaccination knowledge. A postgraduate educational level was associated with more positive attitudes and perceptions toward COVID-19 vaccination. As COVID-19 becomes endemic in 2024, our findings on vaccination knowledge, attitudes, and practices (KAP) can inform public health strategies. The weaker vaccination comprehension of unvaccinated people and smokers contrasts with the more positive sentiments of postgraduates. These demographic differences highlight the need for sophisticated public health responses to COVID-19 and future pandemics.
Our findings suggest specialized educational initiatives to meet various requirements. These campaigns should target individuals with lower vaccine literacy and provide clear, accessible information to dispel myths and promote immunization safety. Initiatives that improve knowledge within these populations can boost vaccination uptake, which is essential for outbreak control and public health. Segmented communication techniques are needed since educational attainment affects vaccination attitudes. Tailoring messaging to demographic segments' informational requirements and communication preferences can improve public involvement and compliance. More precise scientific facts can be employed in advertisements targeting higher-educated populations, whereas simplicity and direct communication should be favored for people with less formal education. These behavioral findings could also inform policy changes to encourage or incentivize vaccine-hesitant communities. Our work can help policymakers anticipate public health issues and improve vaccine coverage and crisis management. These insights can also be integrated into national pandemic preparedness strategies to enable timely, targeted responses to future health crises, optimizing public health response.
The same study reported that most sampled participants believed developing vaccines would end the pandemic [20]. However, around half of them reported having inadequate information on the benefits of COVID-19 vaccination. To elaborate on the importance of educational campaigns to increase knowledge about COVID-19, another study reported that fears of using vaccines and their accompanying side effects are the leading causes of vaccination hesitancy [17].
Furthermore, our study showed that those with positive attitudes and perceptions toward the vaccination process and, more specifically, those who believe in the vaccine's safety and efficacy in protecting against COVID-19 infection [23, 24], as well as those who receive the flu vaccine [25, 26], had a significantly better understanding of the vaccination and higher knowledge about the COVID-19 vaccines. These results agreed with a previous study on populations from Saudi Arabia, Jordan, Lebanon, and Iraq, showing that higher monthly income, medical degree, and prior reception of influenza vaccine are predictors of acceptance of the vaccines [27]. The results also showed that participants' knowledge about the COVID-19 vaccines can affect their actions or decisions upon suspicion of being infected with COVID-19.
Regarding the attitudes of the participants toward recommending the COVID-19 vaccination to particular groups, elderly and healthy middle-aged adults received high-ranked recommendations, while children [24, 28], patients with chronic or autoimmune diseases, and pregnant or lactating women all received a medium-ranked recommendation. It is worth mentioning that when asked about recommending the vaccine to the whole population, a medium-ranked recommendation was also suggested. This can be considered a shift in the attitudes toward accepting the vaccination of the public and even vulnerable groups, such as pregnant women and patients with an autoimmune disease, which was not the case at the beginning of the COVID-19 pandemic.
Moreover, the findings of this study showed that the participant’s acceptance of administering the COVID-19 vaccine to a particular population was significantly higher among participants with postgraduate or professional degrees, which was expected and in agreement with previous studies [27, 29]. This willingness to administer COVID-19 vaccines to a particular population was also significantly correlated with the knowledge of COVID-19 vaccines [23, 30]. This is also expected as participants with higher postgraduate and professional degrees may have more knowledge about the COVID-19 vaccines. As previously reported, greater knowledge about COVID-19 vaccines is associated with decreased vaccination hesitancy [18]
Regarding the attitudes and perceptions of participants about the COVID-19 vaccine, there was a high agreeing attitude toward many items. For instance, the participants agreed that not vaccinating would affect their jobs. This is true as it may be influenced by the recent Jordanian laws mandating vaccination for work. Nevertheless, this external pressure could potentially inflate positive attitudes as individuals may comply due to legal obligations rather than genuine personal conviction.
Most participants also agreed that the priority of getting the booster dose should be directed toward the elderly, patients with chronic diseases, and healthcare providers. This positive attitude indicates the current high level of knowledge about the COVID-19 vaccines among Jordanians and the association between risk perception and vaccination acceptance, as reported in other studies [31]. Moreover, the participants showed trust in the government's ability to bring enough vaccines, which may be understood as the government of Jordan bringing more vaccines than what the people needed this year, 2022, to the level that they could force everyone to take them. Moreover, it is worth mentioning that Jordanians believe that being vaccinated will never stigmatize them, which also may be considered a positive shift in the perception of COVID-19 vaccination compared to previous studies [32]. Enhanced national monitoring systems with regular KAP surveys are also critical. Health officials can swiftly identify and address vaccine reluctance by regularly monitoring public attitudes regarding immunization. In addition, intersectoral coordination between health authorities, educational institutions, and community organizations will increase vaccine literacy and preventive health practices. These partnerships are crucial to establishing a robust public health infrastructure that meets current requirements and prepares for future calamities. Our study uses COVID-19 lessons to help policymakers plan for and respond to pandemics. This proactive approach prepares our healthcare institutions and society for future health emergencies, creating a more informed and responsive public health environment in 2024 and beyond.
CONCLUSION
We developed a validated dual-lingual questionnaire to assess the knowledge, attitudes, and perceptions about COVID-19 vaccination among adult Jordanians after one year of vaccination experience. Our testing showed that Jordanians have good knowledge and a positive attitude or perception toward the vaccination process. Importantly, in such severe pandemics, it should always be considered that the environment, knowledge, attitudes, and public perceptions can be shifted dramatically with time. Therefore, studies should be conducted and reported more rapidly to be of greater help to policymakers. Based on the findings of the present study, various lines of future research would be useful in further developing the research on post-vaccination KAP in Jordan. Longitudinal studies are beneficial due to their ability to monitor changes in KAP over time and provide information on stability and trends. This would expand to create a broad geographic scope across regions in Jordan. Further qualitative research could be used to explore in depth the reasons behind these attitudes and practices, which may come from cultural, social, and personal factors. Other investigational efforts may relate to interventional studies that look at different educational strategies to improve vaccination KAP. Comparative studies with other countries, especially those in comparable health contexts, may yield useful contrasts and benchmarks. Informing on misinformation issues affecting vaccination efforts and tailoring research to specific demographic segments will serve to sharpen public health strategies and interventions. Finally, the evaluation of the impact of recent health policies on vaccination KAP can be a route for essential feedback with respect to policymaking and implementation. These recommended research routes extend the present study's findings and cover relevant gaps, thus serving as a guide for specific yet efficient public health interventions.
STUDY LIMITATIONS
The findings regarding COVID-19 vaccination attitude in Jordan may be limited by the use of an online questionnaire, given that this method might exclude individuals who do not have access to the internet, overrepresenting younger, more urban, and educated populations. Moreover, self-reported data are subject to social desirability biases when reporting sensitive issues, such as vaccination, as people may overreport vaccine acceptance. Although the purposive sample methodology captures its targeted groups, the methodology does not ensure that the sample is representative of the greater Jordanian population. These limitations should be considered when interpreting findings from this study and supporting future research efforts.
AUTHORS’ CONTRIBUTION
M.M., N.A., and S.H.: Study conception and design; M.M.: Data collection; M.M., N.A., and S.H.: Analysis and interpretation of results; M.M., N.A., and S.H.: Draft manuscript. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| CVI | = Content Validity Index |
| JEPeM-USM | = Jawatankuasa Etika Penyelidikan Manusia Universiti Sains Malaysia |
| KAP | = Knowledge, Attitudes, And Practices |
| SD | = Standard Deviation |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study received approval for implementation by the Jawatankuasa Etika Penyelidikan Manusia Universiti Sains Malaysia (JEPeM-USM) and has been assigned a study protocol code (USM/JEPeM/21110726). The study protocol also received approval from the Institutional Review Board (IRB) committee at Jordan University of Science and Technology and has been assigned a study protocol code (156/147/2022).
HUMAN AND ANIMAL RIGHTS
This research was conducted on humans by the Helsinki Declaration of 1975, as revised in 2013 (http://ethics.iit.edu/ecodes/node/3931).
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article will be available from the corresponding author [M.M.] upon reasonable request.
ACKNOWLEDGEMENTS
Declared none.


