All published articles of this journal are available on ScienceDirect.
Factors Influencing Japanese Nursery School Teachers’ Practical Skills in Pediatric Basic Life Support (PBLS)
Abstract
Aim
This study aimed to identify factors related to practical Pediatric Basic Life Support (PBLS) skills among nursery school teachers in regional Japanese cities.
Background
Reducing the mortality rate of infants and young children owing to unintentional injuries is a critical issue in every country. Nursery school teachers, caring for preschool children should possess accurate knowledge and confidence in their responses to emergencies. However, their practical skills in this area have yet to be investigated.
Methods
This study was conducted with 608 nursery school teachers from 45 nursery schools in Niigata Prefecture, Japan. Data were collected using the PBLS practical skills questionnaire created by the authors and the Utrecht Work Engagement Scale-Japanese version (UWESJ17). Multiple regression analysis extracted factors related to PBLS practical skills. Analysis was conducted using SPSS Statistics version 29.0, with the significance level set at less than 5%.
Results
Among participants, 57.8% were in their 40s or older, and 61.8% had over 10 years of nursery school teaching experience. Multiple regression analysis resulted in a model with six predictors, including experience taking a PBLS course, UWESJ17 score, and regular PBLS training at nursery school.
Conclusion
Factors related to the PBLS practical skills of nursery school teachers included personal and facility factors. Employers should establish regular and effective PBLS training programs, mandatory for all nursery school teachers. Injury prevention and response manuals should be distributed to all schools, ensuring consistency and preparedness. This study focused on one region of Japan; therefore, further research in diverse contexts is needed.
1. INTRODUCTION
According to the WISQARS™ database of the US Centers for Disease Control and Prevention, unintentional injury continued to be ranked high as a cause of children’s death in 2022 [1], and its prevention has been an important issue for many years. In Japan, statistics from 2017 to 2021 show that preventable injuries, such as death in bed (34%) and aspiration of gastric contents (22%), will account for the majority of choking-related deaths [2]. It has also been reported that 8.0- 10.8% of children survived one month after out-of-hospital cardiac arrest (OHCA) [3, 4] and that 3.0-3.8% of patients have favorable Cerebral Performance Categories (CPC) [3, 5], indicating a generally poor prognosis for OHCA.
By contrast, an epidemiological survey in Australia reported that approximately a quarter of children who had undergone resuscitation by emergency services showed a return of spontaneous circulation (ROSC) before arriving at a hospital and that older children had more favorable CPC [6]. In this context, ROSC is essential for increasing survival rates, and practical skills in pediatric basic life support (PBLS) are important for those working closely with their children. However, lack of awareness and training in cardiopulmonary resuscitation (CPR) among parents has become a serious issue globally [7], and a study in Japan indicated that only a small proportion of parents of 3-year-old children (20.8% of mothers and 20.4% of fathers) knew how to perform CPR, raising serious safety concerns [8].
In Japan, nursery schools play a crucial role, with 54.1% of 0– 5-year-old children attending these institutions in which licensed teachers care for several children [9]. However, the number of unintentional injuries in nursery schools has been increasing, reaching a record high of 2,772 cases in 2023, including nine deaths reported through the Child Death Review (CDR) [10]. Many of these injuries, such as suffocation or drowning, lead to out-of-hospital cardiac arrest (OHCA) [11]. However, a hearing survey on CDR revealed that recommended procedures for responding to OHCA, as outlined in the American Heart Association (AHA) guidelines, are often insufficiently implemented in nursery schools [12]. While nursery school teachers in Japan are required to undergo PBLS training during their licensing education or at their workplace [13], their practical skills in PBLS and the factors influencing their proficiency remain unexplored. This gap is critical because nursery school teachers are the first responders in childcare emergencies, and their ability to perform PBLS effectively can significantly impact children’s survival outcomes [14]. Furthermore, burnout among nursery school teachers, exacerbated by the COVID-19 pandemic, has raised concerns about their capacity to handle emergencies and maintain high standards of childcare [15, 16].
Therefore, this study focuses on understanding the practical PBLS skills of nursery school teachers, the factors influencing these skills, and the role of facility-level crisis management systems. Hence, by selecting a region in Japan that reflects the realities of PBLS practices, this study aims to provide foundational insights for improving PBLS training programs and enhancing emergency preparedness in nursery schools. Particularly, PBLS encompasses not only the execution of actions but also the precise application of critical components such as the depth of chest compressions and the speed of cardiac massage. These actions require a comprehensive understanding of the underlying principles to ensure effective delivery. Despite the critical nature of these skills, no standardized scale currently exists to measure the practical application of PBLS techniques objectively. Therefore, this study was designed as a pilot survey to facilitate the development of a reliable and valid scale for assessing practical PBLS skills.
2. MATERIALS AND METHODS
2.1. Study Design and Participants
This study conducted a questionnaire survey of nursery school teachers working on remote islands or in core regional cities outside the metropolitan areas of Japan. The participants had a nursery teacher’s license. Those with no nursery teacher’s license, dietitians, and nurses were excluded. Moreover, because a previous study showed that the learning outcomes of PBLS differ by region, the present study covered two regions with different medical situations. Specifically, we targeted nursery school teachers working in rural areas without emergency or critical care centers, as well as those working in major regional cities with multiple advanced treatment hospitals and emergency medical service systems.
Niigata Prefecture, where the present study was conducted, has a variety of regions: a major regional city with a population of over 500,000, which is one of the Institutes of Metropolitan Policy, as well as low-density provincial cities and rural areas [17]. Thus, the prefecture has diverse environments surrounding its nursery schools. In addition, Niigata Prefecture has no issues related to the number of nursery schools and children on enrollment waitlists [9, 18] and represents an average region outside major metropolitan areas in Japan. Therefore, this prefecture was selected for the survey.
In Japan, significant disparities exist in medical resources and emergency medical systems between urban and rural areas [19, 20]. To examine the influence of regional characteristics on PBLS skills in greater detail, we incorporated two distinct regions: an urban area represented by Chuo City, a regional core city with a population of 173,153 (11.5% aged 0–14) and a land area of 14.59 square miles, where tertiary emergency medical facilities are located within 10 km, and a rural area represented by a remote island with a population of 49,336 (10.1% aged 0–14) and a land area of 330.21 square miles, where emergency medical facilities are absent and overall medical resources are severely limited [17]. This comparative approach aimed to elucidate the impact of urban-rural disparities in the practical implementation of PBLS. Furthermore, we deemed it essential to elucidate the factors influencing the advanced level of pragmatic competence required for PBLS, which inherently demands a combination of both knowledge and technical skills.
2.2. Sampling
Niigata prefecture has urban areas with tertiary emergency medical facilities within 10 km, and the rural areas with no emergency medical facilities and extremely limited overall medical resources. Therefore, we extracted a total of 608 nursery school teachers taking care of 05 year old children. The sample included 223 teachers at 24 public and private nursery schools in rural areas and 385 teachers at 21 public and private nursery schools in urban areas with emergency and critical care centers within 10 km Fig. (1).
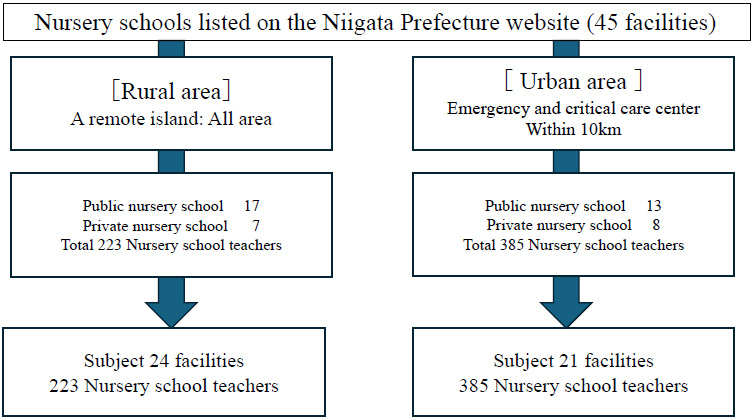

Flow diagram of Niigata prefecture.
The sample size required for the statistical analyses was calculated using the power analysis software Raosoft [21], with an error ratio of 5%, a confidence level of 95%, and a response distribution of 50%. This resulted in an effective sample size of 236 participants for a total population of 608 participants. We estimated that the number of participants required for the statistical analyses would be secured by expecting a response rate of 40%.
2.3. Instrument
The following basic characteristics of the participants were collected through descriptions or multiple-choice questions: age, years of experience as a nursery school teacher, educational background, employment type, and experience of taking a PBLS course. Moreover, responses were obtained regarding the region where the participants’ school was located, the number of children in the school, and school crisis management (the existence of a PBLS course, injury prevention, and injury occurrence manuals, installation of an AED, the presence of nurses, delay before ambulance arrival, and the travel time from the school to a hospital).
Practical skills: Of the 23 questionnaire items (consisting of six items from the PBLS knowledge questionnaire and 17 items from the PBLS confidence questionnaire), 23 items were selected based on the PBLS protocol for lay people outlined in the AHA BLS Guidelines 2020 [22] and reference to the 29 question items [23] published by previous studies [24–26] and the authors. The internal consistency was confirmed with a Cronbach’s α of .950.
Seventeen items from the Japanese version of the Utrecht Work Engagement Scale (UWESJ17) were used to measure the participants’ sense of fulfillment in their work. This scale, developed by Schaufeli and Bakker [27], measures whether a person feels proud, fulfilled, and energized by work. Shimazu et al. [28] developed a Japanese version and verified its reliability and validity. The UWESJ17 consists of three subscales (vigor, dedication, and absorption). The work engagement score was calculated as the average score for all 17 items.
2.4. Data Collection
For data collection, a survey was conducted anonymously by mail after obtaining written permission for the study from the Department of Nursery School Management of the municipalities and directors of the nursery schools.
The survey period was from March to June 2023.
Table 1.
| Characteristic | Item | Variable | n | % |
|---|---|---|---|---|
| Personal | Contract type | Full-time | 180 | 80.0 |
| Part-time | 45 | 20.0 | ||
| Ages | 20S | 33 | 14.7 | |
| 30S | 62 | 27.6 | ||
| over 40 | 130 | 57.8 | ||
| Years of experience as a nursery schoolteacher | with in10 years | 86 | 38.2 | |
| with in20 years | 87 | 38.7 | ||
| 21 years over | 52 | 23.1 | ||
| Education | College | 30 | 13.3 | |
| Junior College | 124 | 55.1 | ||
| Vocation or correspondence school | 71 | 31.6 | ||
| Participation in PBLS | Yes | 174 | 77.3 | |
| No | 51 | 22.7 | ||
| Number of times taking PBLS | None | 49 | 21.8 | |
| Once | 65 | 28.9 | ||
| More than twice | 111 | 49.3 | ||
| PBLS Training within the past one year | Yes | 65 | 28.9 | |
| No | 160 | 71.1 | ||
| Self-paid in PBLS Training | Yes | 17 | 7.6 | |
| No | 208 | 92.4 | ||
| UWESJ17 | High | 126 | 56.0 | |
| Low | 99 | 44.0 | ||
| Facility | Areas | Rural | 96 | 42.7 |
| Urban | 129 | 57.3 | ||
| Scale in Nursery schools | Small :19 children or less | 15 | 6.7 | |
| Medium:20-99 children | 135 | 60.0 | ||
| Large: more than 100 children | 75 | 33.3 | ||
| Regularly PBLS Training at the nursery school | For over once a year | 89 | 39.6 | |
| Not quite sure | 136 | 60.4 | ||
| Travel to a conference on injury prevention and resuscitation | Yes | 141 | 62.7 | |
| No | 84 | 37.3 | ||
| Nursery school nurse | Yes | 80 | 35.6 | |
| No | 145 | 64.4 | ||
| Injury Prevention Manual | Yes | 164 | 72.9 | |
| No | 61 | 27.1 | ||
| Injury Occurrence Manual | Yes | 181 | 80.4 | |
| No | 44 | 19.6 | ||
| AED (for child) | Yes | 209 | 92.9 | |
| No | 16 | 7.1 | ||
| Ambulance arrival | within10 minutes | 128 | 56.9 | |
| 10 minutes over | 97 | 43.1 | ||
| Time from school to hospital | within15 minutes | 140 | 62.2 | |
| 15 minutes over | 85 | 37.8 |
UWESJ17: Japanese version of the Utrecht Work Engagement Scale
2.5. Statistical Analysis
The data were analyzed using SPSS Statistics version 29.0. Prior to analysis, the data were screened for normality and outliers. Descriptive statistics were reported as means and standard deviations (SD) and standard error (SE) for all outcome variables. The demographic and facility-related characteristics of the participants are also presented.
To assess “PBLS knowledge,” participants completed a six-item questionnaire, where each correct response was assigned one point, yielding a possible score range of 0–6. For “PBLS confidence,” participants responded to a 17-item questionnaire. Responses of “5. Confident” and “4. Slightly confident” were categorized as “Confident” and assigned one point, while responses of “3. Neither,” “2. Not very confident,” and “1. Not confident” were categorized as “Not confident” and assigned zero points, resulting in a possible score range of 0–17. A significant positive correlation was observed between “PBLS knowledge” (range: 0–6) and “PBLS confidence” (range: 0–17), as determined by Pearson’s correlation coefficient (R = 0.409, p < 0.001). The sum of these scores was designated as “PBLS practical skills,” with a total possible range of 0–23.
2.6. Ethical Considerations
This study was reviewed by the Niigata College of Nursing (Japan) ethics committee and was conducted with the approval of the Niigata College of Nursing president (approval number: 022-12). Explanatory documents containing information on human rights protection in accordance with the Helsinki Declaration (1975, revised 2013; http://ethics.iit.edu/ecodes/node/3931) were provi-ded to the study participants, and informed consent was obtained. Free will was respected through anonymous mail. Prior to the start of the study, we confirmed with the developers of the UWESJ17 that the scale could be applied. (Appendix)
3. RESULTS
3.1. Subjects Characteristics
Of the 608 nursery school teachers working in the 45 nursery schools surveyed, 250 responded (response rate = 41.1%). Of these, 225 participants with no missing data on PBLS knowledge, PBLS confidence, UWESJ17 score, age, years of experience as a nursery school teacher, or educational background were included in the analysis (valid response rate: 90.0%). The basic attributes of the participants are presented in Table 1.
Regarding age, those in their 40s or older were the most common at 57.8%. Regarding the years of experience as a nursery school teacher, 38.7% had 10–20 years of experience. Regarding educational background, junior college was the most common (55.1%), followed by vocation or correspondence school (31.6%) and college (13.3%). Regarding residence, 96 participants (42.7%) lived in rural areas, and 129 (57.3%) lived in urban areas.
3.2. Intergroup Comparison of PBLS Practical Skills and each Item
The statistics of the PBLS practical skills are shown in Table 2. Furthermore, the correct answer rates for the six-item PBLS knowledge questionnaire (KQ) and the 17-item PBLS confidence questionnaire (CQ) are shown in Figs. (2 and 3), respectively. Among the items of PBLS knowledge, the correct answer rate was highest for “How much does the rib cage sink during chest compressions?” at 73.8% and lowest for “At what interval (in minutes) should AED be reanalyzed?” at 25.3%. Among the items of PBLS confidence, the correct answer rate was highest for “Unresponsive: Able to ask nearby nursery school teachers to call 119 and perform AED” at 78.7% and lowest for “Release of choking: Able to alternate between five chest compressions and five back taps (infants)” at 12.9%.
| S.No. | Item | Mean | SD | SE | Skewness | Kurtosis | Response Frequencies (%) | |
|---|---|---|---|---|---|---|---|---|
| 0 | 1 | |||||||
| 1 | Does a child have a voice when choking? | 0.67 | 0.47 | 0.04 | -0.712 | -1.507 | 32.9 | 67.1 |
| 2 | What is the ratio of chest compressions to ventilation? | 0.51 | 0.50 | 0.05 | -0.045 | -2.016 | 51.1 | 48.9 |
| 3 | How fast should chest compressions be (per minute)? | 0.52 | 0.50 | 0.05 | -0.081 | -2.011 | 47.1 | 52.9 |
| 4 | How much does the rib cage sink during chest compressions? | 0.74 | 0.44 | 0.03 | -1.088 | -0.823 | 26.2 | 73.8 |
| 5 | At what age can an AED be used? | 0.45 | 0.50 | 0.06 | 0.189 | -1.982 | 55.6 | 44.4 |
| 6 | How many minutes should the AED be reanalyzed every minute? | 0.23 | 0.42 | 0.06 | 1.284 | -0.354 | 74.7 | 25.3 |
| 1 | Choking or SIDS: Can ensure the safety of the surrounding area | 0.32 | 0.47 | 0.07 | 0.755 | -1.443 | 67.6 | 32.4 |
| 2 | Release of choking: Is able to perform the Heimlich maneuver (child) | 0.18 | 0.39 | 0.07 | 1.657 | 0.754 | 81.8 | 18.2 |
| 3 | Release of choking: Five chest compressions and five back taps alternately (infant) | 0.13 | 0.34 | 0.06 | 2.230 | 2.999 | 87.1 | 12.9 |
| 4 | Response: Tap on the shoulder to check for reactions (child) | 0.71 | 0.46 | 0.07 | -0.914 | -1.175 | 29.3 | 70.7 |
| 5 | Response: Stimulate the soles of the feet and check for reactions (infant) | 0.54 | 0.50 | 0.08 | -0.153 | -2.000 | 46.2 | 53.8 |
| 6 | Unresponsive: AED and call an ambulance with 119 | 0.79 | 0.41 | 0.06 | -1.409 | -0.015 | 21.3 | 78.7 |
| 7 | Unresponsive: Can be laid flat | 0.60 | 0.49 | 0.07 | -0.430 | -1.831 | 39.6 | 60.4 |
| 8 | Breathing: Can check respiratory arrest or agonal respiration *1 | 0.23 | 0.42 | 0.08 | 1.314 | -0.275 | 77.3 | 22.7 |
| 9 | Circulation: Chest compressions with one or both hands (child) | 0.27 | 0.44 | 0.07 | 1.062 | -0.879 | 73.3 | 26.7 |
| 10 | Circulation: Chest compressions with two fingers (infant) | 0.22 | 0.41 | 0.07 | 1.377 | -0.106 | 78.2 | 21.8 |
| 11 | Airway: Can perform head-tilt chin-lift maneuvers *2 | 0.33 | 0.47 | 0.08 | 0.733 | -1.475 | 67.1 | 32.9 |
| 12 | Airway: Can perform jaw thrust maneuver | 0.20 | 0.40 | 0.08 | 1.510 | 0.283 | 80.0 | 20.0 |
| 13 | AED: Can attach correctly | 0.46 | 0.50 | 0.07 | 0.171 | -1.989 | 54.2 | 45.8 |
| 14 | AED: Able to follow voice commands | 0.60 | 0.49 | 0.07 | -0.392 | -1.863 | 40.4 | 59.6 |
| 15 | Use of injury occurrence manual | 0.24 | 0.43 | 0.07 | 1.226 | -0.502 | 76.0 | 24.0 |
| 16 | Choking or aspiration: Able to observe their surroundings | 0.38 | 0.49 | 0.06 | 0.488 | -1.778 | 61.8 | 38.2 |
| 17 | Instructions: Ensure the safety of other children | 0.69 | 0.46 | 0.06 | -0.822 | -1.337 | 31.1 | 68.9 |
| PBLS Practical Skills | 10.00 | 5.65 | 0.38 | Range | PBLS Knowledge PBLS Confidence | |||
| 0-23 | 0-6 0-17 | |||||||
PBLS Confidence: “Strongly agree” or “Agree”=1; “Strongly disagree,” “Disagree,” or “Neutral”=0.
*1 Agonal respiration is a state of breathing that is gasping, fast, shallow, and not fully oxygenated.
*2 Head tilt chin-lift maneuver in which the airway is secured by placing one hand on the forehead, tilting the head back, and raising the chin. PBLS: Pediatric Basic Life Support; AED: automated external defibrillator; SIDS: sudden infant death syndrome.
SD: standard deviation; SE: standard error.
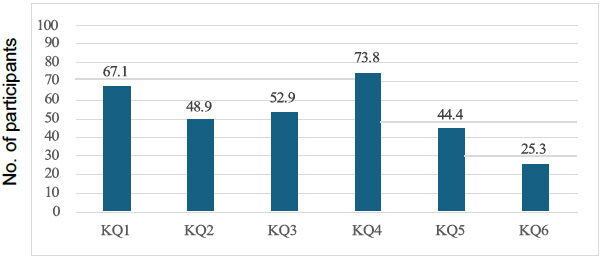
PBLS Knowledge questionnaire correct answer rate.
Note: KQ: PBLS knowledge questionnaire 6 items.
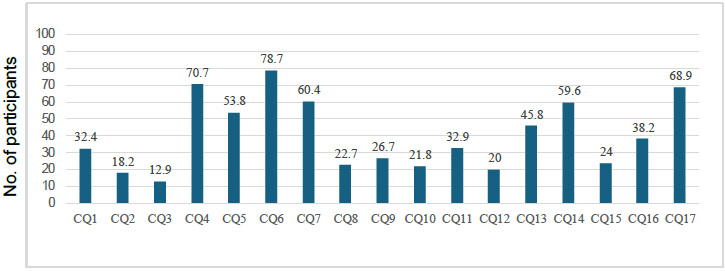
PBLS Confidence questionnaire correct answer rate.
Note: CQ: PBLS Confidence questionnaire 17 items.
| Item | Variable | n | mean | SD | t | df | p | 95%CI | |
|---|---|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||||
| Areas | Rural | 96 | 10.57 | 5.598 | 1.328 | 206.11 | .186 | -0.488 | 2.502 |
| Urban | 129 | 9.57 | 5.665 | ||||||
| Contract type | Full-time | 180 | 10.65 | 5.503 | 3.565 | 67.67 | .001** | 1.441 | 5.104 |
| Part-time | 45 | 7.38 | 5.507 | ||||||
| Participation in PBLS | Yes | 174 | 11.19 | 5.272 | 6.559 | 85.64 | .001** | 3.671 | 6.865 |
| No | 51 | 5.92 | 4.975 | ||||||
| PBLS Training within the past one year | Yes | 65 | 11.89 | 5.489 | 3.294 | 119.72 | .001** | 1.064 | 4.270 |
| No | 160 | 9.23 | 5.542 | ||||||
| Self-paid in PBLS Training | Yes | 17 | 13.71 | 5.632 | 2.828 | 18.63 | .011* | 1.039 | 6.988 |
| No | 208 | 9.69 | 5.552 | ||||||
| UWESJ17 | High | 126 | 11.09 | 5.791 | 3.392 | 219.46 | .001** | 1.040 | 3.923 |
| Low | 99 | 8.61 | 5.158 | ||||||
| Periodical PBLS Training at the nursery school | For over once a year | 89 | 11.89 | 5.714 | 4.144 | 177.26 | .001** | 1.640 | 4.621 |
| No Rure | 136 | 8.76 | 5.264 | ||||||
| Travel to a conference on injury prevention and resuscitation | Yes | 141 | 10.51 | 5.462 | 1.749 | 164.64 | .082 | -0.178 | 2.940 |
| No | 84 | 9.13 | 5.874 | ||||||
| Nursery school Nurse | Yes | 80 | 9.34 | 5.396 | -1.326 | 172.37 | .187 | -2.541 | 0.499 |
| No | 145 | 10.36 | 5.766 | ||||||
| Injury Prevention Manual | Yes | 164 | 10.95 | 5.612 | 4.555 | 121.29 | .001** | 1.980 | 5.025 |
| No | 61 | 7.44 | 4.935 | ||||||
| Injury Occurrence Manual | Yes | 181 | 10.65 | 5.600 | 3.826 | 70.85 | .001** | 1.594 | 5.063 |
| No | 44 | 7.32 | 5.066 | ||||||
| AED (for child) | Yes | 209 | 10.20 | 5.485 | 1.588 | 16.39 | .131 | -0.960 | 6.737 |
| No | 16 | 7.31 | 7.115 | ||||||
| Ambulance arrival | within10minutes | 128 | 11.16 | 5.502 | 3.639 | 207.02 | .001** | 1.234 | 4.151 |
| 10 minutes over | 97 | 8.46 | 5.493 | ||||||
| Time from nursery to hospital | within15minutes | 140 | 10.49 | 5.680 | 1.689 | 181.21 | .093 | -0.218 | 2.813 |
| 15 minutes over | 85 | 9.19 | 5.528 | ||||||
Levene test p<.001 homogeneity of variance.
PBLS: Pediatric Basic Life Support; AED: automated external defibrillator; UWESJ17: Japanese version of the Utrecht Work Engagement Scale;
CI: confidence interval; SD: standard deviation; SE: standard error
The mean ± SD of the 23 PBLS practical skills items was 10.00 ± 5.646, with a SE of 0.38.
An intergroup comparison of PBLS practical skills and each item is shown in Table 3. Intergroup comparisons revealed a significant difference between the nine items. Regarding employment type, practical PBLS skills were significantly higher among full-time employees than part-time employees (p<.001, 95% CI [1.441 5.104]). Regarding experience taking a PBLS course, PBLS practical skills were significantly higher in those with experience taking a course (p<.001, 95% CI [3.671 6.865]), and those who had taken a course within the past year, than in others (p<.001, 95% CI [1.064 4.270]). Furthermore, PBLS practical skill levels were significantly higher in the group with higher UWESJ17 scores than in the group with lower scores (p<.001, 95% CI [1.040 3.923]). They were significantly higher in facilities that conducted PBLS training at least once a year than in those that did so irregularly (p<.001, 95% CI [1.640 4.621]). In addition, PBLS practical skill levels were significantly higher in facilities with injury prevention manuals (p<.001, 95% CI [1.980 5.025]) and injury occurrence manuals (p<.001, 95% CI [1.594 5.063]) than in those without these factors. Furthermore, PBLS practical skills were significantly higher in facilities for which an ambulance could arrive in less than 10 minutes than in those for which an ambulance would require more than 10 minutes to arrive (p<.001, 95% CI [1.234 4.151]).
3.3. Multiple Regression Analysis with PBLS Practical Skills as a Dependent Variable
The results of the multiple regression analysis are presented in Table 4. The multiple regression analysis was performed using the step-down method. The dependent variable was “PBLS practical skills.” The independent variables were six of the nine items that showed a significant difference in the intergroup comparison of PBLS practical skills and each item (excluding three items that were considered to have multicollinearity), as well as one item that showed a significant difference in the simple
| - | Model 2 | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Regression Statistics | - | - | - | 95% CI | - | ||||
| Item | Variable | B | SE | β | t | p | Lower | Upper | VIF |
| (Constant) | - | -1.880 | 1.363 | - | -1.379 | .169 | -4.566 | .807 | - |
| Participation in PBLS | 1: Yes 0: No | 3.802 | .795 | .283 | 4.781 | .001** | 2.235 | 5.369 | 1.129 |
| UWESJ17 | - | 1.227 | .301 | .231 | 4.075 | .001** | .634 | 1.820 | 1.038 |
| Ambulance arrival | 1: <10 minutes 0: >10 minutes | 2.312 | .642 | .203 | 3.602 | .001** | 1.047 | 3.578 | 1.029 |
| Regular PBLS training at the nursery school | 1: Yes 0: No | 1.594 | .677 | .138 | 2.355 | .019* | .260 | 2.929 | 1.116 |
| Employment type | 1: Full-time 0: Part-time | 1.775 | .806 | .126 | 2.202 | .029* | .187 | 3.363 | 1.058 |
| Injury occurrence manual | 1: Yes 0: No | 1.694 | .831 | .119 | 2.038 | .043* | .056 | 3.331 | 1.106 |
| Coefficient of determination R2 | .325 | ||||||||
| Adjusted R2 | .307 | ||||||||
Dependent variable: PBLS Practical Skills; multiple correlation coefficient: R=.570
Independent variable: Participation in PBLS, UWESJ17, Ambulance arrival, Regular PBLS training at the nursery school, Employment type, and injury occurrence manual. Forced entry: Exclusion criteria=AED (for child); p<.001** and p<.05*.
PBLS: Pediatric Basic Life Support; AED: automated external defibrillator; UWESJ17: Japanese version of the Utrecht Work Engagement Scale SE: standard error; VIF: variance inflation factor.
regression analysis. The results showed that the regression of Model 2, which excluded the presence of AED, was significant, and that the prediction could be performed with an accuracy of 30.7%. A significant difference was observed for the following six predictive factors: Participation in PBLS (t(6)=4.781, p<.001, 95% CI [2.235 5.369]), average of the UWESJ17 scores (t(6)=4.075, p<.001, 95% CI [.634 1.820]), arrival of an ambulance within/over 10 minutes (t(6)=3.602, p<.001 95% CI [1.0473.578]), regular PBLS training at nursery school (t(6)=2.355, p<.05, 95% CI [.260 2.929]), employment type (full-time/part time; t(6)=2.202, p<.05, 95% CI [.187 3.363]), and injury occurrence manuals (t(6)=2.038,p<.05, 95% CI [.056 3.331]). In addition, the VIF of the independent variables applied was less than 5 for all models, and no multicollinearity was observed.
4. DISCUSSION
The results of this study showed that the following factors influenced the practical skills of nursery school teachers: experience taking a PBLS course, UWESJ17 score, and a nursery school location where it takes less than 10 minutes for an ambulance to arrive. Among these factors, the experience of taking a PBLS course had the strongest influence on practical PBLS skills.
Previous studies have reported that PBLS training is an important factor in acquiring practical PBLS skills. Moreover, a comparison before and after PBLS training revealed knowledge retention among nursing students [29], and a survey of elementary and junior high school teachers indicated that skills could be acquired through training [30]. Our results support the findings of these studies and reaffirm the importance of PBLS training in acquiring practical PBLS skills.
In contrast, while 80% of the subjects had experience taking a PBLS course, over 70% answered that the most recent course they had taken was over a year ago, indicating that most of the subjects had not taken the course for years. An intergroup comparison showed that those who had taken a PBLS course within the past year and those who attended PBLS training regularly, at least once a year, had higher PBLS practical skills.
A survey conducted in Saudi Arabia showed that those who had not received training for two years or more had a decline in knowledge and skills [30], and it has been reported that even the PBLS practical skills of pediatricians decline within three to six months if they do not receive regular training [31]. The subjects of the present study were nursery school teachers. Our results suggest that a system that allows them to receive PBLS training regularly, without gaps in time and with sufficient frequency, is necessary for maintaining their PBLS practical skills, similar to healthcare workers.
Interestingly, work engagement was associated with practical PBLS skills. Work engagement is defined as a psychological state in which a person feels proud, fulfilled, and energized by their work [32]. The finding that those who feel proud and fulfilled in their work have higher PBLS practical skills is similar to a recent focus on re-killing and re-upskilling in the industrial sector. These findings suggest that opportunities for reskilling and re-upskilling related to crisis management in nursery schools are useful for developing human resources with superior adaptability. Additionally, this study revealed that nursery school teachers PBLS practical skills were influenced by their employment type. This suggests that nursery school teachers’ pride and fulfillment in their work are also influenced by their employment type (full-time or part-time).To this end, PBLS training should be improved to allow remote training and include programs that elevate pride in one’s work rather than simply increasing the number of sessions. Furthermore, employers must establish a crisis management system that does not rely only on each person’s motivation but also on regular PBLS training as part of job training, regardless of employment type.
In Japan, securing human resources to provide childcare outside the home has become a social issue because of the serious decline in the population and birthrate. In addition, previous studies on schoolteachers have shown that many of them are concerned about not having appropriate knowledge and skills and that they hope to participate in PBLS training if it is free of charge, indicating that they have high expectations for improving their PBLS practical skills [30, 33]. Our results suggest that improving practical PBLS skills can alleviate the concerns mentioned above and may aid in securing human resources for nursery school teaching.
Furthermore, the location of a nursery school with a 10-minute ambulance arrival time was found to relate to practical PBLS skills, but our results did not reveal the reason for this significant difference. Early arrival of an ambulance at a nursery school indicates that a fire station equipped with an ambulance is located near the school. This may make it easier for nursery school teachers to receive PBLS training. Next, we discuss the practical skills of PBLS by subdividing their contents.
Among the items of PBLS knowledge, which is a part of PBLS practical skills, the correct answer rate was the lowest for the frequency of AED reanalysis. In addition, no questions had a correct answer rate of 80% or higher, and the overall correct answer rate was low. As many participants in this study had taken the course months or years ago, they might have forgotten the knowledge that they had previously learned.
Among the 17 items on PBLS confidence, the lowest confidence scores were found for the relief of airway obstruction in infants, the Heimlich maneuver in children, the jaw elevation maneuver, and chest compressions in infants. Regarding emergency resuscitation training, the method of resuscitation for children is relatively similar to that for adults. However, because the position and strength required for thoracic compressions in infants differ, it is likely that knowledge has not been firmly established and that nursery school teachers lack confidence in the technique. Recently, educational materials that do not rely on group training, such as infant BLS self-learning kits, have been widely used, and the effectiveness of these techniques has been demonstrated [34]. In the future, it will be necessary to not only solidify knowledge but also develop products that allow repeated and simple self-training, as a requirement of workplace training, on the resuscitation of infants and small children whose physical constitution differs from that of adults, as well as a system for evaluating training.
Finally, we discuss the issues in strengthening practical PBLS skills. Regarding personal factors, full-time nursery school teachers with high work engagement scores had high PBLS practical skills. Moreover, regarding employer factors, nursery school teachers in facilities that have manuals for a crisis management system and provide regular PBLS training had high PBLS practical skills. Thus, our results suggest the need to strengthen the crisis management system. Such a system should also consider the in-facility education provided by employers, such as the implementation of PBLS training for all employees, including part-time staff, regardless of employment conditions, as well as the preparation of injury prevention and injury occurrence manuals.
Currently, PBLS training is examined in the form of e-learning [35], online training [36], simulation-based training [29], and instructor-led training. To make it feasible to hold PBLS training regularly, at least once a year, it is hoped that training programs will be developed that can be undertaken by the entire facility by considering methods and schedule adjustments that make it easier for part-time employees to participate.
The strength of this study is that we extracted factors related to the knowledge of PBLS and the confidence in skills as “PBLS practical skills.” This led to the finding that personal factors, such as the effectiveness of receiving PBLS training and pride and fulfillment in one’s work, influenced PBLS practical skills. Facility factors, such as regular PBLS training at school and injury prevention and injury occurrence manuals, were extracted as factors related to PBLS practical skills. This study had limitations. This study conducted a survey that collected self-reported information that may have affected the responses of nursery school teachers, and it used a questionnaire. Moreover, a larger sample size is required to ensure the generalizability of the findings. As this study targeted only certain regions of Japan, the samples collected may not represent the actual situation of nursery school teachers across Japan.
CONCLUSION
This study found that factors influencing practical PBLS skills include personal factors, such as prior experience with PBLS courses and a sense of pride and fulfillment in one’s work, as well as facility-related factors, such as regular PBLS training at schools, injury prevention measures, and injury response manuals. However, no regional differences between rural and urban areas were found.
To address these findings, employers should establish regular and effective PBLS training programs, making participation mandatory for all nursery school teachers. Additionally, injury prevention and response manuals should be distributed to all schools to ensure consistency and preparedness.
One notable limitation of this study is the small sample size. This was primarily due to challenges in recruiting a sufficient number of participants, as the survey was conducted during the coronavirus pandemic. Consequently, the generalizability of the findings is limited, and caution should be exercised when applying the study’s conclusions to populations with different backgrounds or circumstances.
AUTHORS’ CONTRIBUTION
K.Y.: Study conception and design; K.Y.: Data collection; K.Y. and T.S.: Analysis and interpretation of results; K.Y. and T.S.: Draft manuscript. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| AED | Automated External Defibrillator |
| CDR | Child Death Review |
| CPC | Cerebral Performance Category |
| CPR | Cardio Pulmonary Resuscitation |
| OHCA | Out-of-hospital cardiac arrest |
| PBLS | Pediatric Basic Life Support |
| UWESJ17 | Japanese version of Utrecht Work Engagement Scale 17 |
| WISQARS™ | Web-based Injury Statistics Query and Reporting System |
| KQ | Knowledge Questionnaire |
| CQ | Confidence Questionnaire |
| SD | Standard Deviations |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study was reviewed by the Niigata College of Nursing Japan ethics committee and conducted with the approval of the Niigata College of Nursing president, Japan (approval number: 022-12).
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013. The study complies with all relevant ethical guidelines for research, and no animals were used at any stage.
CONSENT FOR PUBLICATION
The participants consented by ticking the consent box in the questionnaire, which was provided with the consent document, and the data collector recorded their consent.
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article is solely housed within the institution’s archive and not currently accessible through an online data repository.
FUNDING
This study was supported by JSPS Grant in Aid for Scientific Research, Grant number: JP22K10389.
ACKNOWLEDGEMENTS
We are deeply grateful to the Children and Youth Division of Sado City, Niigata Prefecture; the Chief of the Health and Welfare Section of Chuo Ward, Niigata City; and the nursery school teachers at the public-private nursery schools for their generous support and cooperation in this study.
APPENDIX
| Regression Statistics | - | 95%CI | |||||||
|---|---|---|---|---|---|---|---|---|---|
| - | B | SE | β | t | P | Lower | Upper | ||
| Employment type | 3.272 | 0.917 | 0.232 | 3.567 | .001** | 1.464 | 5.08 | ||
| Age (years) | -0.137 | 0.514 | -0.018 | -0.266 | 0.79 | -1.15 | 0.876 | ||
| Years of experience as a nursery | 0.864 | 0.488 | 0.118 | 1.773 | 0.078 | -0.096 | 1.825 | ||
| school teacher Education | -0.351 | 0.585 | -0.04 | -0.6 | 0.549 | -1.503 | 0.801 | ||
| Participation in PBLS | 5.268 | 0.829 | 0.392 | 6.354 | .001** | 3.634 | 6.902 | ||
| Number of times PBLS is taken | 2.045 | 0.453 | 0.289 | 4.513 | .001** | 1.152 | 2.938 | ||
| PBLS training in the past | 2.667 | 0.813 | 0.215 | 3.281 | .001** | 1.065 | 4.269 | ||
| one year Self-paid PBLS training |
4.014 | 1.402 | 0.188 | 2.863 | .005** | 1.251 | 6.776 | ||
| UWESJ17 | 1.653 | 0.338 | 0.311 | 4.891 | .001** | 0.987 | 2.319 | ||
| Area | -1.007 | 0.76 | -0.088 | -1.325 | 0.186 | -2.504 | 0.49 | ||
| The scale of nursery school | -1.05 | 0.654 | -0.107 | -1.606 | 0.11 | -2.339 | 0.238 | ||
| Regular PBLS training at the | 3.13 | 0.743 | 0.272 | 4.216 | .001** | 1.667 | 4.594 | ||
| Nursery school Travel to the conference on injury |
1.38 | 0.774 | 0.118 | 1.781 | 0.076 | -0.147 | 2.906 | ||
| Prevention and resuscitation Nursery school nurse | -1.021 | 0.785 | -0.087 | -1.301 | 0.195 | -2.568 | 0.526 | ||
| Injury prevention manuals | 3.502 | 0.816 | 0.276 | 4.294 | .001** | 1.895 | 5.11 | ||
| Injury occurrence manuals | 3.328 | 0.925 | 0.234 | 3.599 | .001** | 1.506 | 5.15 | ||
| Near miss sharing | -0.235 | 1.357 | -0.012 | -0.173 | 0.863 | -2.908 | 2.439 | ||
| Near miss scrutiny | 1.617 | 0.895 | 0.12 | 1.808 | 0.072 | -0.146 | 3.38 | ||
| AED (for child) | 2.888 | 1.455 | 0.132 | 1.985 | .048* | 0.021 | 5.756 | ||
| Ambulance arrival | 2.692 | 0.74 | 0.237 | 3.638 | .001** | 1.234 | 4.151 | ||
| Time from school to hospital | 1.297 | 0.773 | 0.112 | 1.678 | 0.095 | -0.226 | 2.821 | ||
Single regression analysis (forced entry) *p<.05 **p<.01.
B= unstandardized partial regression coefficient β=standardized partial regression coefficient.


