All published articles of this journal are available on ScienceDirect.
Prevalence and Risk Factors of Hypertension among Young Adults: An Indonesian Basic Health Survey
Abstract
Introduction
Hypertension patients aged under 40 years have low awareness and under-diagnosis, hence poor blood pressure control. The prevalence of undiagnosed hypertension in men and women aged 26 to 35 years is 55% and 44%, respectively. This study aimed to provide information on the prevalence and risk factors for hypertension among young adults based on the basic health survey (Riset Kesehatan Dasar; RISKESDAS) in Indonesia.
Methods
This cross-sectional study utilized secondary data from the RISKESDAS 2018 with a total of 140,073 subjects aged 26-35 years. The characteristics of the subjects were presented as proportion. This study performed a chi-square test and involved multivariate analysis using binary logistic regression for all parameters with p-value <0.25 in the chi-square test.
Results
This study reports the prevalence of hypertension among young adults to be 4.1%. A study also found that female (POR:=1.225 95% confidence interval (CI): 1.119-1.341), unmarried (POR=0.711; 95% CI:0.556-0.908), low-level education (POR=1.286; 95% CI:1.195-1.384), unemployed (POR=1.267; 95% CI:1.166-1.377), BMI≥25 (POR=2.472 (2.295-2.662), diabetes mellitus (POR=3.688; 95% CI:2.630-5.173), emotional mental disorder (POR=2.041; 95% CI:1.856-2.244), instant food consumption (POR=1.108; 95% CI:1.025-1.197) were related to the occurrence of hypertension among young adults.
Conclusion
The prevalence of hypertension among young adults was 4.1%. Females, married, low level of education, unemployed, BMI≥25, diabetes mellitus, having a mental disorder, and consumption of instant food altogether increase the risk of getting hypertension among young adults aged 26-35 years old.
1. INTRODUCTION
Hypertension is a condition in which repeated examination results in a systolic blood pressure (SBP) of more than 140 mm Hg in the clinic or health center and a diastolic blood pressure (DBP) of at least 90 mm Hg. These definitions apply to all individuals (>18 years old) [1]. It develops when the arterioles put too much pressure on the vessel walls from the blood, making the heart work harder to keep the pressure [2]. Hypertension can trigger other non-communicable diseases [3]. The number of hypertension patients continues to increase every year. In 2025, there will be 1.5 billion people with hypertension [4]. Every year, it is estimated that there will be 9.4 million deaths due to hypertension and its complications [2]. Worldwide, there are 54% of adults diagnosed with hypertension [5]. An estimated 46% of adults with hypertension are in ignorance [2]. A rise in blood pressure increases the risk of heart attack, heart failure, stroke, and kidney diseases [6]. Hypertension patients have a 2.6 times greater risk of developing coronary heart disease compared to non-hypertensive individuals [7]. The goal for individuals with hypertension is to maintain BP at <140/90 mm Hg to prevent complications [6].
The prevalence of hypertension in Indonesia has increased, based on the basic health survey (Riset Kesehatan Dasar; RISKESDAS). In 2013, hypertension was 25.8%, while the in 2018 increased to 34.1%. Moreover, there are plenty of unreported cases; merely 1/3 of hypertension cases in Indonesia are diagnosed [8]. Based on a systematic review study in 90 countries, only 46.5% of adults aged ≥20 years old with hypertension were aware of their BP [9]. Hypertension patients aged under 40 years have low awareness, under-diagnosis, and poor blood pressure control [10]. The prevalence of undiagnosed hypertension in men and women aged 26 to 35 years is 55% and 44%, respectively. The prevalence of undiagnosed hypertension in young adults is higher than in people aged ≥75 years [11].
It is important to identify and manage modifiable risk factors for hypertension. Since the determinants may vary across different age groups, examining the factors specifically among young adults in Indonesia is essential. A limited number of studies have been conducted to investigate the factors contributing to high blood pressure in young adults, especially in Indonesia's 26-35 age group. This study aimed to provide information on the prevalence and risk factors for hypertension among young adults based on the RISKESDAS 2018 in Indonesia.
2. MATERIALS AND METHODS
2.1. Design and Study Population
This cross-sectional study utilized secondary data from the RISKESDAS 2018. RISKESDAS is a population health study conducted by the National Institute for Health Development Policy, Ministry of Health, Republic Indonesia. RISKESDAS aims to monitor public health status and services that provide information on key health indicators such as health status, nutritional status, environmental health, health behaviors, and various aspects of health care. RISKESDAS data provides health data at district/city and national levels. This report included subjects aged 26–35 who were interviewed by the RISKESDAS 2018 enumerator, with a total of 140,073 subjects aged 26–35. Of the 140,073 subjects, 78,300 met the criteria to be analyzed (Fig. 1). Complete detailed reports of the survey methods, including data collection, ethical issues, and other related steps, were published in the RISKESDAS 2018 report [12].
2.2. Data Collection and Variables
This study conformed to the ethical criteria based on the Helsinki Declaration of 1975 and its revised in 2013 and approved by the Ethical Review Board, Faculty of Medicine, Universitas Negeri Semarang, under the approval ID number 169/KEPK/FK/KLE/2024. The National Institute for Health Development Policy, Ministry of Health, Republic Indonesia, approved the RISKESDAS data for this report. This study used certain parameters from RISKESDAS 2018, which were analyzed in this study. These include their weight and height, sociodemographic data, hypertension status, diabetes mellitus status, emotional mental disorder status, smoking status, physical activity status, alcohol consumption, body mass index, salt food consumption, fat food consumption, and instant food consumption.
Sociodemographic factors in this study included age, sex, marital status, residence area, education level, and working status. Hypertension was categorized as previously diagnosed as hypertension by a doctor and having a history of under-hypertension medication. The subjects diagnosed with diabetes mellitus (DM) were classified as having a plasma glucose level of at least 126 mg/dL during fasting or two hours postprandial and a random plasma glucose level of at least 200 mg/dL or a previous medical diagnosis. Moreover, to reduce the possibility of bias concerning the inquiry of “previously had been diagnosed with diabetes mellitus by a physician,” inquiries concerning the DM medication and plasma glucose test were asked.
This study used the Ministry of Health of the Republic of Indonesia age category, which young adults defined as someone between 26 and 35 years old [13]. Marital status was divided into three categories: unmarried, married, and widow. The residence areas were divided into two categories: urban and rural. Education level was divided into two categories: low (less than senior high school) and high (more than or equal to senior high school). Employment status was classified as either employed or unemployed.
BMI was acquired by calculating the result measurement of weight (in kilograms) divided by height (in meters square) and was categorized as ≥25 and <25. Emotional mental disorders were determined by a self-reporting questionnaire (SRQ) consisting of 20 questions invented by WHO with a cutoff point of 6 [14].
Lifestyle and eating behavior factors in this study included smoking, physical activity, alcohol consumption, salt food consumption, fat food consumption, and instant food consumption. Physical activity was categorized as sedentary and active based on the International Physical Questionnaire. Consumption of salt, fat, and instant food was counted as frequent if consumed≥3-6 times/week.
2.3. Statistical Analysis
The characteristics of the subjects were presented as proportion. This study performed a chi-square test to find out the risk factors associated with hypertension among young adults in Indonesia. The p-values <0.05 reflected as statistically significant. This study involved multivariate analysis using a binary logistic regression for all parameters with p-value <0.25 in the chi-square test. The statistical analysis was accomplished in this study using IBM SPSS Statistics software (for Windows, Version 22.0, Armonk, NY: IBM Corp.).
3. RESULTS
3.1. Characteristics of Subjects
Of the 140,073 subjects aged 26-35, 73,800 met the criteria and were included in the analysis. Among these, 3,225 (4.1%) young adults in Indonesia were identified as having hypertension. Tables 1 and 2 explain the characteristics of these subjects.
Based on the result of the chi-square test in Table 3, some parameters show p-value <0.005; it refers to evidence of influence hypertension among young adults, i.e. sex (POR=0.856; 95% CI: 0.794-0.924), education levels (POR=1.355; 95% CI: 1.262-1.454), marital status (POR=0.612; 95% CI: 0.481-0.777), working status (POR=1.358; 95% CI: 1.264-1.460).
It is also based on the result of the chi-square test in Table 4, body mass index (POR=2.424; 95% CI: 2.255-2.606), diabetes mellitus (POR=4.257; 95% CI: 3.059-5.924), emotional mental disorder (POR=2.105; 95% CI: 1.919-2.311), smoking (POR=0.876; 95% CI: 0.808-0.949), and instant food consumption (POR=1.159; 95% CI: 1.074-1.251). Binary logistic regression will be used to continue analyzing the variables whose p-value is less than 0.25.
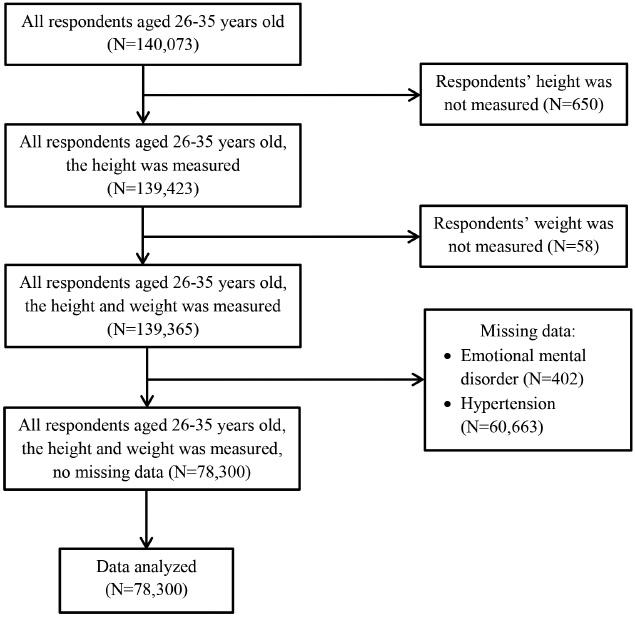
Subjects’ recruitment flow.
| Variables | Samples (N) | Percentages (%) |
|---|---|---|
| Sex | ||
| Male | 27227 | 34.8 |
| Female | 51073 | 65.2 |
| Marital Status | ||
| Unmarried | 8398 | 10.7 |
| Married | 67895 | 86.7 |
| Widowed | 2007 | 2.6 |
| Residence Area | ||
| Urban | 34367 | 43.9 |
| Rural | 43933 | 55.1 |
| Education Level | ||
| Low | 37482 | 33.6 |
| High | 51958 | 66.4 |
| Variables | Samples (N) | Percentages (%) |
|---|---|---|
| Working Status | ||
| Unemployed | 26342 | 33.6 |
| Employed | 51958 | 66.4 |
| Body Mass Index | ||
| BMI≥25 | 31430 | 40.1 |
| BMI>25 | 46870 | 59.9 |
| Diabetes Mellitus | ||
| Yes | 274 | 0.3 |
| No | 78026 | 99.7 |
| Emotional Mental Disorder | ||
| Yes | 7705 | 9.8 |
| No | 70595 | 90.2 |
| Smoking | ||
| Yes | 22245 | 28.4 |
| No | 56055 | 71.6 |
| Physical Activity | ||
| Sedentary | 7067 | 9.0 |
| Active | 71233 | 91.0 |
| Alcohol Consumption | ||
| Yes | 3540 | 4.5 |
| No | 74760 | 95.5 |
| Salt Food Consumption | ||
| Frequent (≥36 times/week) | 32153 | 41.1 |
| Rarely (<36 times/week) | 48147 | 58.9 |
| Fat Food Consumption | ||
| Frequent (≥36 times/week) | 47346 | 60.5 |
| Rarely (<36 times/week) | 30954 | 39.5 |
| Instant Food Consumption | ||
| Frequent (≥36 times/week) | 21864 | 27.9 |
| Rarely (<36 times/week) | 56436 | 72.1 |
| Hypertension | ||
| Yes | 3225 | 4.1 |
| No | 75075 | 95.9 |
Table 3.
| Variables | Hypertension | pvalue | POR (95% CI) | |||
|---|---|---|---|---|---|---|
| Yes | No | |||||
| N | % | N | % | |||
| Sex | ||||||
| Male | 1015 | 3.7 | 26212 | 96.3 | <0.001* | 0.856 (0.7940.924) |
| Female | 2210 | 4.3 | 48863 | 95.7 | ||
| Marital Status | ||||||
| Unmarried | 253 | 3.0 | 8145 | 97.0 | <0.001* | 0.612 (0.4810.777) |
| Married | 2875 | 4.2 | 65020 | 95.8 | 0.190 | 0.871 (0.7081.071) |
| Widowed | 97 | 4.8 | 1910 | 95.2 | ||
| Education Level | ||||||
| Low | 1778 | 4.7 | 35704 | 95.3 | <0.001* | 1.355 (1.2621.454) |
| High | 1447 | 3.5 | 39371 | 96.5 | ||
| Working Status | ||||||
| Unemployed | 1305 | 5.0 | 25037 | 95.0 | <0.001* | 1.358 (1.2641.460) |
| Employed | 1920 | 3.7 | 50038 | 96.3 | ||
| Variables | Hypertension | pvalue | POR (95% CI) | |||
|---|---|---|---|---|---|---|
| Yes | No | |||||
| N | % | N | % | |||
| Body Mass Index | ||||||
| BMI≥25 | 1968 | 6.3 | 29462 | 93.7 | <0.001* | 2.424 (2.2552.606) |
| BMI<25 | 1257 | 2.7 | 45613 | 97.3 | ||
| Diabetes Mellitus | ||||||
| Yes | 42 | 15.3 | 232 | 84.7 | <0.001* | 4.257 (3.0595.924) |
| No | 3183 | 4.1 | 74843 | 95.9 | ||
| Emotional Mental Disorder | ||||||
| Yes | 583 | 7.6 | 7122 | 92.4 | <0.001* | 2.105 (1.9192.311) |
| No | 2642 | 3.7 | 67953 | 96.3 | ||
| Smoking | ||||||
| Yes | 835 | 3.8 | 21410 | 96.2 | 0.001* | 0.876 (0.8080.949) |
| No | 2390 | 4.3 | 53665 | 95.7 | ||
| Physical Activity | ||||||
| Sedentary | 298 | 4.2 | 6769 | 95.8 | 0.663 | 1.027 (0.9101.160) |
| Active | 2927 | 4.1 | 68306 | 95.9 | ||
| Alcohol Consumption | ||||||
| Yes | 159 | 4.5 | 3381 | 95.5 | 0.260 | 1.100 (0.9341.294) |
| No | 3066 | 4.1 | 71694 | 95.9 | ||
| Salt Food Consumption | ||||||
| Frequent (≥36 times/week) | 1309 | 4.1 | 30844 | 95.9 | 0.583 | 0.980 (0.9121.053) |
| Rarely (<36 times/week) | 1916 | 4.2 | 44231 | 95.8 | ||
| Fat Food Consumption | ||||||
| Frequent (≥36 times/week) | 1954 | 4.1 | 45392 | 95.9 | 0.897 | 1.005 (0.9351.081) |
| Rarely (<36 times/week) | 1271 | 4.1 | 29683 | 95.9 | ||
| Instant Food Consumption | ||||||
| Frequent (≥36 times/week) | 995 | 4.6 | 20869 | 95.4 | <0.001* | 1.159 (1.0741.251) |
| Rarely (<36 times/week) | 2230 | 4.0 | 54206 | 96.0 | ||
| Variables | B | S.E | Wald | p-value | POR (95% CI) |
|---|---|---|---|---|---|
| Female | 0.203 | 0.046 | 19.368 | <0.001* | 1.225 (1.119-1.341) |
| Unmarried | -0.341 | 0.125 | 7.434 | 0.006* | 0.711 (0.556-0.908) |
| Low Level of Education | 0.251 | 0.037 | 45.177 | <0.001* | 1.286 (1.195-1.384) |
| Unemployed | 0.237 | 0.043 | 30.930 | <0.001* | 1.267 (1.166-1.377) |
| BMI≥25 | 0.905 | 0.038 | 573.050 | <0.001* | 2.472 (2.295-2.662) |
| Diabetes Mellitus | 1.305 | 0.173 | 57.182 | <0.001* | 3.688 (2.630-5.173) |
| Emotional Mental Disorder | 0.713 | 0.048 | 216.699 | <0.001* | 2.041 (1.856-2.244) |
| Instant Food Consumption | 0.102 | 0.040 | 6.722 | 0.010* | 1.108 (1.025-1.197) |
| Constant | -3.844 | 0.113 | 1165.952 | <0.001 | 0.021 |
Table 5 shows the final regression model results, i.e., female (POR:=1.225 95% confidence interval (CI): 1.119-1.341), unmarried (POR=0.711; 95% CI:0.556-0.908), low-level education (POR=1.286; 95% CI:1.195-1.384), unemployed (POR=1.267; 95% CI:1.166-1.377), BMI≥25 (POR=2.472 (2.295-2.662), diabetes mellitus (POR=3.688; 95% CI:2.630-5.173), emotional mental disorder (POR=2.041; 95% CI:1.856-2.244), instant food consumption (POR=1.108; 95% CI:1.025-1.197) were altogether related to the occurrence of hypertension among young adults.
4. DISCUSSION
This national scope study in Indonesia found that the prevalence of hypertension among young adults aged 26-35 was 4.1%. Previous studies reported different prevalences of hypertension among young adults; the CARDIA study reported that in the US, young adults was 9.6% [15]; the Framingham study discovered that the prevalence of hypertension was 12.9% in women and 14.2% in men aged 20 to 49 [16]; another study in the US reported the prevalence of hypertension among 20 to 44 years old was 9.3% [17]. Other studies consistently reported similar prevalence: Albania, aged 15-49, was 16.24% [18]; Zimbabwe, aged 18-25, was 7.4%; Lahore, Pakistan, aged 18-39, was 15.7% [19]; and India, aged 18-39, was 13.8% [20]. This study's findings indicate that the prevalence of hypertension in young adults was low compared to other studies. This is likely since the study only included participants who had received a medical diagnosis or had taken antihypertensive medication. In contrast, previous studies confirmed the diagnosis by blood pressure measurement; missing out on subjects unaware of hypertension was potentially a lot in this study. Most young adults are unaware of their abnormally high blood pressure and only realize its effects when they age [21]. Young adults are less sensitive to hypertension than older people because young adults visit doctors less often than older people [21]. Hypertension patients aged below 40 years have low awareness, under-diagnosis, and poor blood pressure control [10].
This study found that females were more susceptible to hypertension compared to females. Previous studies reported different conditions [18, 22-24], i.e., a study in Albania reported that males are more at risk of hypertension [18], and a study in Poland also showed similar results [22]. A cross-sectional study conducted in Varanasi revealed that males are at 1.97 times greater risk of hypertension [23]. A study of young adults in Zimbabwe also found that males were 1.53 times more likely to develop hypertension than females [25]. Generally, males have less favorable habits compared to females, such as excess consumption of instant food, smoking, and alcohol consumption, leading to hypertension [18, 26]. However, this study found that females have more risk. The low number of male visits to health services could be the reason for the lower rate of hypertension in males because of undetected cases. Females are more likely to visit health services for consultation regarding birth control and regular gynecological services, where every visit will check their blood pressure so that females’ blood pressure is more detected compared to males [21].
This study also found that married persons have a greater risk of hypertension, and unmarried persons have a lower risk. This finding is dissimilar from previous studies that found unmarried persons have a greater risk of hypertension [23, 26, 27]. Another study reported that early-married women have a higher risk of developing hypertension [28]. The present study also found that low-level education subjects possess a higher risk of developing hypertension. A Chinese study found that people with only an elementary education or less are more likely to develop hypertension than people with a middle or higher education [29]. Low knowledge which is a result of low education, influences an unhealthy lifestyle, and access to health information is more accessible for those with higher education levels. The degree of education affects how well they receive and absorb information, which affects their health [23, 30]. Other studies also show that a higher level of education is expected to increase good knowledge about hypertension and its treatment [31].
This study also found that unemployed subjects have a greater risk of hypertension. A previous study concluded similarly that unemployed subjects risk developing hypertensive disease more than employed people [32-34]. A systematic review and meta-analysis study in Southeast Asian Countries also stated that the unemployed have a greater risk of hypertension [34]. Unemployed people are 1.39 more at risk of hypertension compared to employed people [35]. The results of a nationwide study in China state that unemployment conditions are a high risk of hypertension because of the relationship with economic capacity. Therefore, unemployment will indirectly make someone less aware of hypertension treatment and control [36, 37]. Unemployment is more at risk of hypertension because of low income; a person will have a limited variety of food, and the health services received are more limited [32].
The current study also concluded that subjects with a BMI≥25 have a 2.47 times greater risk of hypertension. This finding is consistent with previous studies, including a study in Poland, which states that having a BMI above average is a greater risk of hypertension [22]. Other studies, i.e., Nagpur and South Asia, state the same conclusion [38]. A cohort study conducted in Thailand over four years showed that BMI was significantly associated with an increased risk of hypertension [26]. A study conducted among young adults in Tenwek Mission Hospital, Bomet County, Kenya, in 2018 stated that having a BMI≥25 had a 3.05 more significant risk of hypertension [39]. A Malaysian study stated that obese people have a 4.29 times risk of developing hypertension [40]. Likened to people with normal BMI, people with BMI≥25 are more likely to have metabolic disorders, such as fat metabolism disorder and insulin antibody disorder. Metabolic disorders can trigger cardiovascular disease, including hypertension [41]. Apart from other risk factors, BMI directly affects blood pressure. Nevertheless, the mechanism of BMI's influence on blood pressure is still unclear [42]. Several studies show that BMI is a critical and sensitive indicator for predicting high blood pressure [43, 44].
In developing countries, diabetes mellitus can be a significant factor in the development of cardiovascular disease [45]. This study showed that diabetes mellitus has a significant association with hypertension. People with diabetes mellitus are more at risk of developing hypertension [23, 26, 40, 46]. Hypertension and diabetes mellitus are interrelated because hypertension can also cause diabetes mellitus [47]. A previous study reported that the presence of diabetes mellitus puts a person at twice the risk of hypertension [48]. A prospective cohort study conducted over four years in a national Thai Cohort Study showed similar results, where diabetes mellitus was strongly associated with hypertension [26]. Diabetes mellitus is also a variable that affects hypertension, as demonstrated by a study conducted in Malaysia [40]. Research conducted in South Korea through The Fourth Korea National Health and Nutrition Examination Survey (KNHANES IV) states that hypertension is more prevalent in adults with diabetes mellitus in the general population and for both sexes [49]. Hypertension occurs due to complex metabolic disorders caused by diabetes mellitus. Increased circulating fluid volume and peripheral vascular resistance in patients with diabetes mellitus occur due to insulin resistance, which increases body fluid volume. This condition is closely related to increased blood pressure [50].
This study found that emotional mental disorder has a higher risk of getting hypertension. Psychologically, distress that occurs causes an increased risk of hypertension, 1.53 greater than a person without a mental disorder [51]. A study in China concluded that stress was significantly related to hypertension, where stressful conditions put a person 1.2 times more at risk of hypertension [52]. Emotional mental disorders, e.g., stress, will trigger endothelial dysfunction that allows for an increase in blood pressure [53].
The present study also found that instant food consumption leads to hypertension condition. A prospective cohort study in Spanish revealed that high consumption of ultra-processed food creates a greater risk of hypertension [54]. An 8-year cohort study in Thailand showed that dietary patterns are associated with hypertension. An unhealthy diet includes consuming processed foods, including instant foods that are low in fiber, high in carbohydrates, saturated fat, and high in sodium [55]. Generally, the combinations contained in instant food are carbohydrates, fat, and salt [26]. Frequent consumption of instant food will trigger cardiometabolic, which causes an increase in blood pressure [56].
Since the study used secondary data regarding the data available in RISKESDAS, certain factors that influence the development of hypertension in young adults have yet to be identified. Future research is therefore anticipated to incorporate these characteristics, along with genetics and other factors, including modifiable factors and certain prevention efforts.
CONCLUSION
The prevalence of hypertension among young adults in this study was 4.1%, which showed lower numbers compared to other studies. This low prevalence might be due to a lack of awareness, low hypertension case detection, and underdiagnosis conditions, suggesting increasing early detection and screening efforts in the community.
Females, married, low-level education, unemployed, BMI≥25, diabetes mellitus, having an emotional mental disorder, and consumption of instant food altogether increase the risk of getting hypertension among young adults aged 26-35 years old.
AUTHORS' CONTRIBUTION
L.R.P. and M.A.: Study conception and design; L.R.P. and A.I.F.: Data collection; L.R.P., M.A., A.A.N.: Analysis and interpretation of results. manuscript draft: LRP, MA, AIF, PK, and SAS. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| SRQ | = Self-reporting questionnaire |
| DBP | = Diastolic Blood Pressure |
| SBP | = Systolic Blood Pressure |
| DM | = Diabetes Mellitus |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study was approved by the Ethical Review Board, Faculty of Medicine, Universitas Negeri Semarang, Indonesia under the approval ID number 169/KEPK/FK/KLE/2024.
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
AVAILABILITY OF DATA AND MATERIAL
The data supporting the findings of the article is available at https://doi.org/10.6084/m9.figshare.2754294 6.v1 .
FUNDING
This work was financially supported by the Ministry of Education and Culture, Republic of Indonesia, and the Institute of Research and Community Service, Universitas Negeri Semarang (Grant number SP DIPA- 023.17.1.690523/2024).
ACKNOWLEDGEMENTS
We also thank the National Institute for Health Development Policy, Ministry of Health, Republic Indonesia, for providing data from the Indonesian Basic Health Survey (Riset Kesehatan Dasar; RISKESDAS).


