All published articles of this journal are available on ScienceDirect.
Correlation between Biopsychosocial Factors and Quality of Life in Individuals with Hypertension: A Cross-sectional Study in Indonesia
Abstract
Background
The quality of life for those with a medical history of chronic illnesses such as hypertension is influenced by various factors. In addition to physical health, the biopsychosocial model underscores that hypertension arises from a multifaceted interplay of biological, psychological, and social elements. This study aims to determine the correlation between biopsychosocial factors and the quality of life of hypertensive individuals.
Methods
A total of 204 participants who met the inclusion criteria at Medan City Health Center were included in this study. Modified PSS-10, MSPSS, Bortner Rating Scale, and WHOQOL-BREF questionnaires were used to support variable assessment. Variables were tested with chi-square and logistic regression analyses to assess the association between biopsychosocial factors such as age, education level, occupation, income, social support, stress level, and others on the quality of life of hypertensive patients.
Results
The majority of respondents had a good quality of life (52.5%). There was an association between sports activities (0.004), stress level (0.013), social support (0.023), education level (p=0.045), and income (p=0.036) with quality of life. Patients with income >3,000,000 (OR 2.9; CI 95%), moderate stress level (OR 2.7; CI 95%), working as an employee (OR 2.7; CI 95%), high social support (OR 2.2; CI 95%) and exercise >3x a week/1>50 minutes a week (OR 2.1; CI 95%) had better quality of life.
Conclusion
Stress levels, income, social support, exercise activities, and occupation contribute to an improved quality of life.
1. INTRODUCTION
Hypertension or high blood pressure is a common health issue worldwide, including in Indonesia. According to the World Health Organisation (WHO), more than one billion people worldwide suffered from hypertension in 2020, and this number is likely to continue growing for the next decades [1]. According to data from the Indonesian Ministry of Health, the prevalence of hypertension in the country seems to be on the rise year after year. Factors such as lifestyle changes, unhealthy diet, stress, and lack of physical activity contribute to the increase in hypertension cases [2].
As defined by the World Health Organization (WHO), quality of life is an individual's perception of their circumstances, shaped by their cultural and value systems. This perception is further contextualized by the individual's personal goals, aspirations, and concerns [3]. This clearly indicates that the parameters of quality of life are determined by perceptions of physical health, psychological aspects, level of independence, and social relationships [4, 5]. Patients with hypertension are often associated with lower health-related quality of life than healthy people [6, 7]. However, aside from medical conditions, several other studies have found other factor variables that affect the quality of life of the hypertension population [8, 9]. While it is well-known that lifestyle contributes to hypertension outcomes, there is less clarity on how factors from other domains (such as emotional, socio-economic, and cultural aspects) potentially determine hypertension outcomes, which impact quality of life [10, 11].
In 1977, George Engel introduced a new idea in the treatment of medical disorders with the biopsychosocial concept. The approach emphasizes that the interaction of biological, psychological (which includes thoughts, emotions, and behaviors), and social (e.g., socioeconomic, socioenvironmental, and cultural) factors play an important role in health and illness. Therefore, health and disease are not only related to the physical medical aspects alone but involve a combination of all three factors [10, 11]. Traditional understanding of hypertension is often limited to physical factors alone, such as genetics, diet, and exercise habits. However, the biopsychosocial approach emphasizes that hypertension is the result of a complex interaction between biological, psychological, and social factors [12-14].
The goal of hypertension management is not only to control blood pressure within normal limits but also to enhance the quality of life of sufferers. Consequently, it is essential to discuss the relationship between biopsychosocial factors and quality of life in hypertensive patients. The main objective of our study was to ascertain the association between biopsychosocial factors and quality of life in hypertensive patients at Medan City Health Center. The specific objectives of our study were to describe the characteristics of the majority of respondents, which were observed based on age, gender, ethnicity, marital status, education level, employment status, income, body mass index, smoking habit, family history of hypertension, duration of hypertension, hypertension medication consumption, comorbidities, salt intake pattern, exercise activities, personality type, stress level, social support, and quality of life in hypertensive patients at Medan City Health Center. Additionally, it was interested in finding the relationship between biopsychosocial characteristics and quality of life in this population.
2. METHODS
2.1. Participants
Our study utilized a non-probability sampling technique adopting purposive sampling, resulting in a sample of 204 individuals with hypertension from Medan City Health Center who met the inclusion criteria: (1) diagnosed with hypertension; (2) consented to complete the research questionnaire and sign the informed consent form. The respondents' characteristics are listed in Table 1.
| Characteristics | (n = 204) | (%) | |||
|---|---|---|---|---|---|
| Age | |||||
| 18 - 41 years | 25 | 12,3 | |||
| 42 - 65 years | 179 | 87,7 | |||
| Gender | |||||
| Male | 61 | 29,9 | |||
| Women | 143 | 70,1 | |||
| Nationality | |||||
| Sumatra | 128 | 62,7 | |||
| Outside Sumatra | 76 | 37,3 | |||
| Marital Status | |||||
| Not married | 8 | 3,9 | |||
| Married | 196 | 96,1 | |||
| Education Level | |||||
| Not in school - Elementary school graduate | 41 | 20,1 | |||
| Junior/high school graduate/equivalent | 115 | 56,4 | |||
| Bachelor/Diploma Graduates | 48 | 23,5 | |||
| Jobs | |||||
| Not working | 63 | 30,9 | |||
| Housewife | 41 | 20,1 | |||
| Employee | 100 | 49 | |||
| Income | |||||
| IDR < 1.000.000 | 109 | 53,4 | |||
| IDR 1.000.000 - 3.000.000 | 57 | 28,0 | |||
| IDR ≥ 3.000.000 | 38 | 18,6 | |||
| Body Mass Index | |||||
| ≤23 (Normal) | 55 | 27 | |||
| 23-24,9 (Overweight) | 35 | 17,1 | |||
| ≥ 25 (Obese) | 114 | 55,9 | |||
| Blood Pressure | |||||
| Normal-High | 4 | 2 | |||
| Grade 1 Hypertension | 143 | 70,1 | |||
| Grade 2 Hypertension | 57 | 27,9 | |||
| Smoking Habit | |||||
| No smoking | 171 | 83,8 | |||
| Smoking | 33 | 16,2 | |||
| Family History of Hypertension | |||||
| No history of hypertension | 114 | 55,9 | |||
| History of Hypertension | 90 | 44,1 | |||
| Duration of Hypertension | |||||
| 1 - 10 years | 184 | 90,2 | |||
| ≥ 10 years | 20 | 9,8 | |||
| Consumption of Hypertension Medication | |||||
| No | 86 | 42,2 | |||
| Yes | 118 | 57,8 | |||
| Non-compliant | 46 | 39,0 | |||
| Compliant | 72 | 61,0 | |||
| Comorbidities | |||||
| No | 133 | 65,2 | |||
| Yes | 71 | 34,8 | |||
| Salt Intake Pattern | |||||
| <1 teaspoon | 96 | 47,1 | |||
| ≥ 1 teaspoon | 108 | 52,9 | |||
| Sports Activities | |||||
| <3x a week/<150 minutes a week | 149 | 73,0 | |||
| ≥ 3x a week/ >150 minutes a week | 55 | 27,0 | |||
| Personality Type | |||||
| Type A | 118 | 57,8 | |||
| Type B | 86 | 42,2 | |||
| Stress Level | |||||
| Low stress | 53 | 26,0 | |||
| Moderate stress | 119 | 58,3 | |||
| High stress | 32 | 15,7 | |||
| Social Support | |||||
| Low | 41 | 20,1 | |||
| High | 163 | 79,9 | |||
| Quality of Life | |||||
| Bad | 97 | 47,5 | |||
| Good | 107 | 52,5 | |||
2.2. Data Collection and Ethical Considerations
Primary data was collected by questionnaires filled out directly by respondents. The questionnaire used to assess patients' quality of life in our study was the WHOQOL-BREF, which includes biological, psychological, and social variables. A more detailed assessment of psychological variables was conducted using a modified Perceived Stress Scale (PSS-10) questionnaire to assess stress levels, a modified Bortner Rating Scale questionnaire to assess personality type, and a modified Multidimensional Scale of Perceived Social Support (MSPSS) questionnaire to evaluate the status of social support in patients (Suppl. Material).
The implementation of the research has considered ethical aspects such as voluntary, informed consent, confidentiality, potential for harm, and results communication. Our research has also been approved by the University of Sumatera Utara Research Ethics Commission (NO.701/KEPK/USU/2024).
2.3. Research Instruments
The instrument to assess the quality of life was developed based on WHO recommendations, namely WHOQOL-BREF, consisting of 26 items and assessed on a 5-point Likert scale, then divided into five domains, namely physical health, psychological, social relationships, environment, and quality of life. Scoring for each question from 1-5 according to the measurement scale response, the higher the score obtained, the better the respondent's quality of life. The questionnaire was valid with Cronbach's ɑ coefficient (r=0.89 - 0.95) and reliable (0.66-0.87) [15].
Stress levels were assessed using the Perceived Stress Scale (PSS-10), which consists of 10 questions designed to evaluate the stress experienced by the research subject in the past month. The PSS score ranges from 0 to 40. A higher score signifies an elevated stress level. Scoring interpretations consist of low (0-13), moderate (14-26), and severe stress (≥26) [16]. According to the Greek study, the results of df = 35 and r count = 0.4 (p < 0.05), and the scale reliability of the Perceived Stress Scale was 0.82 [17].
Assessment of personality type using the Bortner questionnaire: this scale consists of 24 pairs of items, and each item consists of two statements. The responses were then summed and categorized into type A and type B personalities. Personality type A includes individuals who are ambitious, impatient, hardworking, multitasking, and uncomfortable with delay and uncertainty. In contrast, type B personalities include people who live with lower stress levels and generally work consistently, enjoying their achievements without feeling distressed if the results are not as expected [18]. Personality interpretation with scores 29-56 Personality Type A, Score = 0-28 Personality Type B. Item validity coefficients moved between 0.307 to 0.493. The alpha reliability coefficient of the Personality Type A and B Scale is 0.763, so the results of the scale are valid and reliable [19].
A more detailed assessment of social support was conducted using the Multidimensional Scale of Perceived Social Support (MSPSS) questionnaire. This measuring tool employs a Likert Scale with seven response alternatives, ranging from one (strongly disagree) to seven (strongly agree). Scores ranging from 12 to 35 indicate low social support, 36 to 60 indicate moderate social support, and scores between 61 and 84 indicate great social support. Consequently, these three classifications can be consolidated into two categories: low social support (12-48) and high social support (49-84) [20].
2.4. Statistical Analysis
The research variables were analyzed descriptively to obtain an overview of the frequency distribution of respondents. The subsequent phase involved bivariate analysis to assess the impact of independent variables on the dependent variable. Chi-square tests were employed in our analysis to assess the influence of biopsychosocial factors on the quality of life of patients with hypertension. Additionally, multivariable analysis will be conducted utilizing logistic regression.
3. RESULTS
Correlation analysis between biopsychosocial factors and quality of life found a significant relationship between quality of life and education level (p=0.045), income (p=0.036), sports activities (p=0.004), stress level (p=0.013), and social support (0.023) Table 2.
Based on the 18 biopsychosocial variables studied, 10 variables were found to be candidates for logistic regression models and multivariate analysis, with the condition that p < 0.25, namely age, ethnicity, education level, occupation, income, body mass index, smoking habits, sports activities, stress levels, and social support. Multivariate logistic regression tests were applied to identify the most prevalent biopsychosocial factors that influence the quality of life of hypertensive patients.
Out of the ten biopsychosocial factors, five factors were with a p-value less than 0.05. These factors include the stress level factor (p-value = 0.02), the occupation factor (p-value = 0.02), the income factor (p-value = 0.02), the sports activities factor (p-value = 0.02), and the social support factor (p-value = 0.03) Table 3. Respondents with moderate stress levels had an odds ratio that was 2.6 times greater for having a better quality of life than respondents with high stress levels. Furthermore, respondents who worked as housewives had an odds ratio of 2.7 times higher to have a good quality of life compared to those who did not work. Respondents with an income exceeding Rp.3,000,000 demonstrated a 2.9-fold higher likelihood of having a good quality of life compared to those with an income below Rp.500,000. In addition, people who exercise >3x a week / <150 minutes a week have an odds ratio of 2.1 greater to have a quality of life that is classified as good compared to respondents who exercise <3x a week / <150 minutes a week. In addition, respondents with high social support had an odds ratio that was 2.2 times greater for having a good quality of life than those with low social support. These results were then made into a logistic regression model as follows:
| Characteristics | Good Quality of Life | Bad Quality of Life | p-value | ||
|---|---|---|---|---|---|
| N = 204 | % | N = 204 | % | ||
| Age | 0.217 | ||||
| 18 - 41 years | 16 | 15,0 | 9 | 9,3 | |
| 42 - 65 years | 91 | 85 | 88 | 90,7 | |
| Gender | 0.999 | ||||
| Male | 32 | 29,9 | 29 | 29,9 | |
| Women | 75 | 70,1 | 68 | 70,1 | |
| Nationality | 0.159 | ||||
| Sumatra | 72 | 67,3 | 56 | 57,7 | |
| Outside Sumatra | 35 | 32,7 | 41 | 42,3 | |
| Marital Status | 0.887 | ||||
| Not married | 4 | 3,7 | 4 | 4,1 | |
| Married | 103 | 96,3 | 93 | 95,9 | |
| Education Level | 0.045 | ||||
| Unschooled - elementary school graduate | 15 | 14 | 26 | 26,8 | |
| Junior/high school graduate | 62 | 57,9 | 53 | 54,6 | |
| Bachelor/diploma graduates | 30 | 28 | 18 | 18,6 | |
| Jobs | 0.151 | ||||
| Not working | 27 | 25,2 | 36 | 37,1 | |
| Housewife | 25 | 23,4 | 16 | 16,5 | |
| Employee | 55 | 51,4 | 45 | 46,4 | |
| Income | 0.036 | ||||
| IDR < 1.000.000 | 49 | 45,8 | 60 | 61,8 | |
| IDR 1.000.000 - 3.000.000 | 32 | 29,9 | 25 | 25,8 | |
| IDR ≥3.000.000 | 26 | 24,3 | 12 | 12,4 | |
| Body Mass Index | 0.029 | ||||
| < 23 (Normal) | 47 | 30,5 | 8 | 27 | |
| 23-24.9 (Overweight) | 29 | 18,8 | 6 | 17,1 | |
| ≥ 25 (Overweight - Obese) | 78 | 50,6 | 36 | 55,9 | |
| Smoking Habit | 0.101 | ||||
| No smoking | 94 | 87,9 | 77 | 79,4 | |
| Smoking | 13 | 12,1 | 20 | 20,6 | |
| Family History of hypertension | 0.533 | ||||
| No history of hypertension | 62 | 57,9 | 52 | 53,6 | |
| History of Hypertension | 45 | 42,1 | 45 | 46,4 | |
| Duration of Hypertension | 0.482 | ||||
| 1 - 10 years | 98 | 91,6 | 86 | 88,7 | |
| ≥10 years | 9 | 8,4 | 11 | 11,3 | |
| Consumption of Hypertension Medication | 0.550 | ||||
| Yes | 64 | 59,8 | 54 | 55,7 | |
| No | 43 | 40,2 | 43 | 44,3 | |
| Comorbidities | 0.605 | ||||
| Yes | 39 | 36,4 | 32 | 33 | |
| No | 68 | 63,6 | 65 | 67 | |
| Salt Intake Pattern | 0.921 | ||||
| <1 teaspoon | 50 | 46,7 | 46 | 47,4 | |
| ≥1 teaspoon | 57 | 53,3 | 51 | 52,6 | |
| Sports Activities | 0.004 | ||||
| <3x a week/<150 minutes a week | 69 | 64,5 | 80 | 82,5 | |
| ≥3x a week/ >150 minutes a week | 38 | 35,5 | 17 | 17,5 | |
| Personality Type | 0.753 | ||||
| Type A | 63 | 58,9 | 55 | 56,7 | |
| Type B | 44 | 41,1 | 42 | 43,3 | |
| Stress Level | 0.013 | ||||
| Low stress | 37 | 34,6 | 16 | 16,5 | |
| Moderate stress | 56 | 52,3 | 63 | 64,9 | |
| High stress | 14 | 13,1 | 18 | 18,6 | |
| Social Support | 0.023 | ||||
| Low | 15 | 14 | 26 | 26,8 | |
| High | 92 | 86 | 71 | 73,2 | |
| Variable Characteristics | B | Standard Error | p-value | OR | 95% CI |
|---|---|---|---|---|---|
| Sports Activities | |||||
| ≥ 3 times / 150 minutes in a week | 0,784 | 0,360 | 0,02 | 2,190 | 1-4,4 |
| Income | |||||
| IDR 1,000,000 - 3,000,000 | 0,631 | 0,394 | 0,10 | 1,879 | 0,8-4 |
| > IDR 3,000,000 | 1,066 | 0,481 | 0,02 | 2,903 | 1,1-7,4 |
| Stress Level | |||||
| Medium | 0,959 | 0,502 | 0,05 | 2,610 | 0,9-6,9 |
| High | 0,082 | 0,422 | 0,84 | 1,086 | 0,4-2,4 |
| Jobs | |||||
| Housewife | 0,998 | 0,442 | 0,02 | 2,713 | 1,1-6,4 |
| Employees & others | 0,039 | 0,401 | 0,92 | 1,040 | 0,4-2,2 |
| Social support | |||||
| High social support | 0,805 | 0,382 | 0,03 | 2,237 | 1-4,7 |
| Constant | -1,615 | 0,549 | 0,03 | 0,199 | |
Linear Regression Modelling
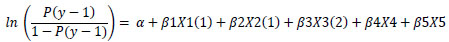 |
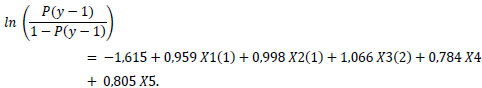 |
4. DISCUSSION
Our study proved that the quality of life of patients with hypertension is determined by five biopsychosocial factors, namely stress level, occupational, income, physical activity, and social support. Our results showed that stress levels were associated with quality of life (p-value 0.02). Our findings are consistent with a prior study that demonstrated the substantial influence of stress on quality of life and the management of hypertension [21, 22]. Biological systems, including the sympathetic adrenomedullary circuit and the hypothalamic-pituitary-adrenal axis, are involved in the body's reaction to stress [23]. Long-term pressure and stress also impact many physiological systems, such as metabolic pathways and the immune system, causing impaired function and cellular aging [24]. Increased stress levels are associated with decreased performance and impaired quality of life [25]. Some studies reported a positive correlation between hypertension and significant psychological distress, where this significant psychological distress increases the risk of hypertension and cerebrovascular disease and vice versa [26, 27]. Furthermore, several medical and mental conditions, including depression, metabolic syndrome, and cardiovascular disease, are also at risk due to high levels of stress [28].
Occupation is one of the factors that significantly affect the quality of life [29]. Occupation with higher job strain is linked to greater rates of hypertension, particularly among young white adults [30]. Our results showed that occupation had an impact on quality of life, with a p-value of 0.024. This aligns with previous research, which states that an individual's job has a significant role and influence in improving a person's quality of life [31, 32]. Our study proves that housewives have a better quality of life with an Odds Ratio of 2.7. Housewives may have some beneficial effects on health, in contrast to workers with inflexible work schedules, long working hours, and a lack of accessible childcare facilities for those with young children, dissatisfaction may be imminent, and quality of life may be negatively affected [33]. Working women, unlike working males, experiencing job pressure exhibited a higher prevalence of hypertension compared to individuals with relaxed psychosocial work characteristics [34].
Higher levels of physical exercise are strongly linked to happier and more contented lives in young, middle-aged, and older adults [35, 36]. Our study found those with hypertension who exercised more than three times a week or for less than 150 minutes a week were found to have a favourable quality of life 2.1 times more frequently. People who engage in physical activity or exercise report feeling better or healthier, and the effects in our study occurred across the life span [37]. Accordingly, a meta-analysis and systematic review carried out on college students revealed that physical activity has a favorable correlation with both emotional and physical well-being, among other dimensions of quality of life [38]. Another study found that physical activity during leisure time positively impacts people's quality of life, especially in improving subjective vitality and reducing stress symptoms [39]. Engaging in physical activity can prevent the emergence of diseases, particularly non-communicable diseases, make the body fitter and healthier, and prevent the onset of depression to improve quality of life [40].
Income has a significant impact on life quality [41, 42]. With a p-value of 0.027 and an odds ratio of 2.9, our study found a relationship between hypertension patients' income and quality of life. These results align with prior research conducted in Iran that shows income variable, which is socio-economic status, was identified as the primary factor influencing the quality of life due to its impact on health behaviors, access to healthcare services, opportunities for acquiring health-related information, and resources available for engaging in physical activities [43]. In the socioeconomic factor, the statistical test results showed that respondents with income below the regional minimum wage (below IDR 3.000.000) had a lower total score of the physical health component compared to respondents with income above the regional minimum wage. Respondents with high income tend to have better mean scores in the physical health component than low-income respondents due to easy access to medical care when there is a decline in physical health, which allows them to remain active [44].
A previous study that examined 600 hypertensive patients in China who were selected by RCT and examined several variables such as gender, marital status, latest education, income, and several others showed that the income variable significantly influenced the quality of life in terms of mental health [45]. Hypertensive patients with higher incomes tend to have better mental health compared to those with lower incomes. Access to mental health resources, the ability to manage stress, and financial freedom to obtain necessary treatment may support a better quality of life for patients with higher incomes [46].
Social support was significantly correlated with quality of life in our study, with a p-value of 0.035 and an odds ratio of 2.2. It aligns with the findings of a previous study, which reported a p-value of 0.003 and a 95% confidence interval (CI) of 1.53 for the correlation. With the support of the closest people, such as family, a patient's psychology can be positively affected to be more enthusiastic about living life and related disease therapy, thereby improving the patient’s quality of life [47]. Other studies have shown that those who received support from friends or family members (caring about their illness and reminding them about treatment) showed better treatment adherence than those who did not receive social support [48]. High social support leads to pleasure, a better sense of life, and satisfaction [49].
CONCLUSION
Five biopsychosocial factors influence the quality of life of hypertensive patients, including social support, stress level, employment status, income, and exercise. Our findings are expected to be considered in the care and health management of hypertensive patients by prioritizing the most influential biopsychosocial factors. By addressing biopsychosocial factors, practitioners can apply comprehensive care tailored to specific community needs. Good stress management and social support are expected to be achieved through the role of family and relatives in obtaining a better quality of life. Since our study was conducted in a primary health facility, further research with a larger sample in other health facilities and other variables that can be assessed is recommended to be carried out in order to obtain more comprehensive results.
AUTHORS’ CONTRIBUTION
The authors confirm their contribution to the paper as follows: study conception and design: AW, KR, PE; data collection: KA, AL, KH; analysis and interpretation of results: MI, MM; draft manuscript: DC. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| WHO | = World Health Organisation |
| MSPSS | = Multidimensional Scale of Perceived Social Support |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The study was approved by the University of Sumatera Utara, Indonesia Research Ethics Commission (NO.701/KEPK/USU/2024).
HUMAN AND ANIMAL RIGHTS
All procedures performed in studies involving human participants were in accordance with the ethical standards of institutional and/or research committees and with the 1975 Declaration of Helsinki, as revised in 2013.
AVAILABILITY OF DATA AND MATERIAL
All data generated or analyzed during this study are included in this published article.
FUNDING
This study is funded by the Directorate of Research, Technology, and Community Service and the Institute for Research and Community Service (DRTPM) of the Ministry of Education and Culture for the fiscal year 2024 through the Universitas Sumatera Utara Fundamental Research Programme, Indonesia grant, number 28/UN5.4.10.S/ PPM/KP-DRTPM/2024.
ACKNOWLEDGEMENTS
The authors would like to thank Universitas Sumatera Utara, Indonesia for supporting this study.


