All published articles of this journal are available on ScienceDirect.
Spatial Analysis of Perceived Health System Capability and Actual Health System Capacity for COVID-19 in South Africa
Abstract
Introduction:
People’s confidence in the health system's capability in managing the COVID-19 pandemic can determine public support, risk perceptions, and compliance to the required behaviors during the pandemic. Therefore, this paper investigated people’s perception of health system capability to manage the COVID-19 pandemic in different spatial areas across the country using data from an online survey.
Methods:
Multivariate logistic regression models were used to examine factors associated with people’s perception of the health system capability to manage the COVID-19 pandemic at the national and provincial levels. Spatial comparative analysis was conducted to contrast spatial density indicators of the number of hospitals, hospital beds, and ICU beds per given population across various provinces.
Results:
Findings showed that South Africans had low confidence in the health system capability, with only two in five (40.7%) reporting that they thought that the country’s health system was able to manage the COVID-19 pandemic. Sex and knowledge on COVID-19 were significantly associated with the people’s perception of the health system capability to manage the pandemic at the national level and in four of the nine provinces.
Conclusion:
Overall, the findings of this study clearly highlight challenges facing the country’s health system, both perceived or real, that needed to be addressed as part of the preparation for the COVID-19 pandemic. Timeous implementation of a countrywide National Health Insurance (NHI) system is now more critical than ever in improving healthcare outcomes of the South African population beyond the existence of the COVID-19 epidemic.
1. INTRODUCTION
Coronavirus Disease 2019 (COVID-19) is a novel coronavirus caused by the Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV2). This novel coronavirus first emerged as a causative agent that led to a respiratory disease outbreak in December 2019 in Wuhan, China [1]. South Africa recorded its first confirmed case of COVID-19 on the 5th March 2020. Since then the number of confirmed cases has grown exponentially, and as of the 7th of July 2021 South Africa has recorded 2.09 million cases. Globally, health systems have been scrutinized for their capability to manage the COVID-19 pandemic. Clinically, the COVID-19 disease is characterised by a dry cough, fever, fatigue and shortness of breath. In severe cases, patients present with severe respiratory illness such as pneumonia or acute respiratory distress syndrome (ARDS), both of which could be fatal and requires hospitalization [2]. According to a presentation made to Members of the South African Parliament by the Director-General of the National Department of Health at the early days of the pandemic, there were a total of 119 416 hospital beds available from both private and public hospitals across South Africa [3, 4]. There were also 3 318 Intensive Care Unit (ICU) beds available. However, it was projected that ICU beds could exceed 14 700 at the highest peak of the COVID-19 pandemic.
In South Africa, inequalities exist in access to health services between the public and private sectors, as well as within the public sector itself, especially between urban and rural areas [5-11]. The public health system supports around 84% of the population (those who are uninsured), while the private sector only services 16% of the population (those with medical insurance). However, the annual per capita healthcare expenditure of the private sector is almost 10 times more than that of the public sector [6]. Those who can afford medical insurance are predominantly from the White population group and those who cannot afford it are mainly Black Africans. The inequalities in access to healthcare in South Africa are inherited from the racial segregation policies of the apartheid government [12]. The COVID-19 outbreak has dramatically highlighted the necessity for a more integrated healthcare system [13]. The COVID-19 pandemic presents a significant opportunity for the National Health Insurance (NHI) to be piloted in real-time. In March 2020, the Competition Commission had published a COVID-19 block exemption for the health sector for promoting better coordination, sharing of information and standardisation of practice across the entire healthcare sector, as well as promoting agreements between the National Department of Health and the private healthcare sector [14]. Spatial accessibility of healthcare facilities is also an important factor in the fight against the COVID-19 outbreak. Spatial accessibility is often concerned with the complex relationship between the spatial separation of the population and the supply of healthcare facilities and thus has a strong underlying geographic component [15-18]. Spatial accessibility is regarded as a primary deciding factor of access to healthcare and healthcare utilization [19, 20].
In addition, people’s confidence in the capability of the health system to manage the COVID-19 pandemic is also crucial. For instance, in India, it was reported that some people escaped from hospitals or quarantine mainly due to the confidence deficit in the public health system in many parts of the country [21]. Therefore, this paper explores South Africans’ perceptions of the country’s health system capability to manage the COVID-19 pandemic. It further assesses the country’s health system capacity in various geographic areas and draws comparisons with perceptions of the health system capability to manage the COVID-19 pandemic.
2. MATERIALS AND METHODS
2.1. Data
This paper utilised data from the Human Sciences Research Council’s (HSRC) COVID-19 online survey conducted in South Africa from 27 March 2020 to 2 April 2020. The survey was open to all adults (18 years and older) residing in South Africa, regardless of race, sex or nationality. Targeted minimum sample size was not pre-determined for this online survey. The questionnaire development was done through a consultative process with socio-behavioral scientists, public health scientists and epidemiologists both locally and internationally [22, 23]. The questionnaire development was further informed by work on public opinions and reactions to the coronavirus emergency prior to the survey as COVID-19 was an emerging pandemic at that time [24, 25]. The self-administered structured questionnaire (48 items) included socio-demographic, knowledge and infection control measures regarding COVID-19, risk of contracting COVID-19, perception of health system capability, hygiene practices, preparedness for self-isolation/quarantine, preparedness for lockdown and the use of social media in accessing the information on COVID-19. Cronbach's alpha analysis was undertaken for the six items used to create the knowledge score. Cronbach's alpha was 0.628. An alpha between 0.6-0.7 indicates an acceptable level of reliability. The survey alerts were distributed and broadcasted via various platforms, and these included a data-free messaging platform, various social media platforms, the HSRC organisational website, as well as local and national radio and television stations.
2.2. Measures
Socio-demographic variables used included sex, age, race, employment, knowledge score (continuous variable), risk perception and self-isolation or quarantine possibility. These variables were categorized as follows; age groups in years (18-29, 30-39, 40-49, 50-59, 60+), sex (male or female), race groups (Black African, Coloured, White, Indian/Asian), employment status (employed full-time, employed informal/part-time, student, unemployed, self-employed), and dwelling type (formal dwelling or informal dwelling). A knowledge score was developed from six knowledge variables about COVID-19, four of which were variables related to knowledge about the transmission (COVID-19 is spread by direct contact with the virus from (Select all that apply)) with options being (infected people coughing/sneezing, pets, touching face after being in contact with an infected person, contact in a public gathering with an infected person, contaminated surfaces and I don’t know); one variable related to knowledge about incubation (After how long will an infected person show signs of being sick?) with options being (immediately, after 1-2 days, after 2-14 days, after 15-20 days, and I don’t know); and one variable related to knowledge about symptoms (Which of the following best describes the symptoms of COVID-19: (Select all that apply)) with options being (shortness of breath, body pain, sweating, headaches, coughs, sneezing, red-itchy eyes, runny nose, fever, and I don’t know). Respondents were assigned a value of 1 for each of the four transmission modes identified, for correct identification of the incubation period of 2-14 days and for correct identification of fever, cough and shortness of breath as the main symptoms. The final knowledge sum score ranged from 0 to 6. For risk perception, self-perceived risk of contracting coronavirus was assessed using the question “How do you rate your personal risk of contracting COVID-19?” with response options being 1=very high risk, 2=high risk, 3=moderate risk, 4=low risk and 5= very low risk. These responses were recoded into 1=low risk (very low risk, and low risk), 2=moderate risk and 3=high risk (very high risk and high risk). For the perception of self-isolation or quarantine possibility, this was assessed using the question “Do you think you may end up in a situation of self-isolation or quarantine?” with response options being 1=yes, 2=no and 3=don’t know. These responses were recoded into 0=no (no and don’t know) and 1=yes (yes). The primary outcome variable, people’s perception of health system capability in dealing with the COVID-19 pandemic, was assessed using the following question “Do you feel each of the following are able to manage the South African COVID-19 outbreak? SA health system” with options being 1=yes, 2=no and 3=don’t know. These were dichotomised into 0=no (no and don’t know) and 1=yes (yes) for logistic regression models.
2.3. Statistical Analysis
Data were analysed using Stata version 15.0 [26]. The data were benchmarked using Statistics South Africa 2019’s mid-year adult population estimates for the generalisability of the findings [27]. Differences in estimates between the socio-demographic variables were compared using Chi-squared tests with a statistical significance level of p ≤ 0.05. Multivariate logistic regression was performed to determine factors associated with the perception that the country’s health system was capable of managing the COVID-19 pandemic. Odds ratio (OR) with 95% CIs and p ≤ 0.05 were reported for the level of statistical significance. This was done at both national and provincial levels to determine differences across provinces. Race group and dwelling type were excluded from the logistic regression analyses due to low response rates from Indian/Asian and Coloured groups in three provinces, namely Northern Cape, Limpopo and Mpumalanga.
2.4. Spatial Analysis
Spatial density indicators were developed using secondary data for the numbers of hospitals, hospital beds and ICU beds gathered from several sources [4, 28, 29]. The 2019 population estimates from Statistics South Africa (Stats SA) were used to calculate spatial density indicators of the number of hospitals, hospital beds and ICU beds per given population. Spatial comparative analysis was employed to generate maps showing the perception of health system capability and density indicators of the health system across various provinces using ArcGIS 10. The health facilities earmarked by the national government to focus on COVID-19 were also geocoded and mapped for spatial analysis of their distribution and geographic accessibility.
3. RESULTS
3.1. Demographics of Respondents
The study sample comprised 53 488 respondents. After benchmarking against population demographics, females constituted 53.9% and Black Africans accounted for 76.4% followed by Whites at 10.8%. In terms of age composition, 29.9% were 18-29 years old followed by those aged between 30 and 39 years old (25.7%).
3.2. Perception of Health System Capability in Managing COVID-19
Table 1 highlights people’s perceptions towards health system capability to manage the COVID-19 pandemic across different socio-demographic variables and provinces. Overall, two in five South Africans (40.7%) reported that they thought that the country’s health system was able to manage the COVID-19 outbreak. The people’s perception of the health system capability to manage COVID-19 varied significantly across all socio-demographic variables (p < 0.01 for age and p < 0.001 for all other variables). Males had a significantly higher prevalence of perceiving the health system as capable than females. The older persons (70 years and older) had the lowest confidence in the health system capability (29.0%) compared to other age groups. Black Africans had the highest confidence in the health system capability (46.9%), while participants from the White population group had the lowest (13.4%).
Those employed part-time or informally had the highest confidence (44.8%) in the health system capability and self-employed adults had the lowest (34.4%). The confidence in the health system capability was less prevalent among those who thought they were at moderate and high risk of contracting COVID-19 (around 38% each) and among those who thought they might end up in self-isolation or quarantine (34.1%). People residing in informal dwellings had a higher confidence in the health system capability (55.7%) than those who lived in formal dwellings (40.0%).
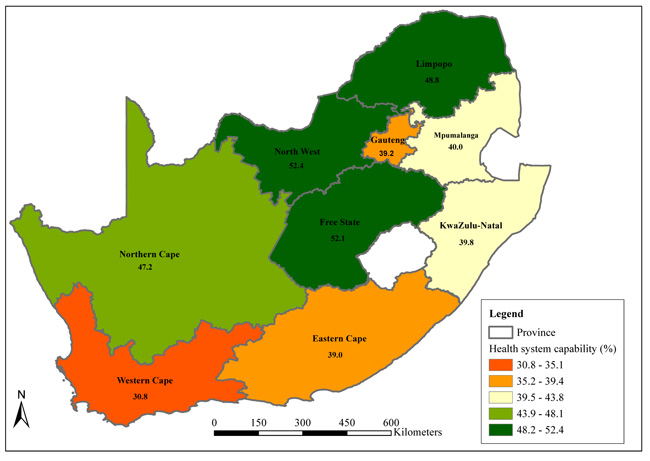
Fig. (1) highlights that the Western Cape had the lowest percentage (30.8%) of people who felt that the national health system was capable of dealing with the COVID-19 pandemic. Gauteng and Eastern Cape were under the second-lowest category of 35.2% to 39.4%. North West and Free State had the highest percentages of people (more than half each) who had confidence in the health system’s capability in managing the COVID-19 pandemic. These were followed by Limpopo, with 48.8% of people having confidence in the country’s health system to deal with the COVID-19 pandemic.
| Socio-Demographics | Total | % | 95% CI | P-Value |
|---|---|---|---|---|
| Sex | - | - | - | - |
| Male | 15 476 | 44.4 | [42.3-46.5] | <0.001 |
| Female | 33 721 | 37.6 | [36.0-39.1] | - |
| Age Group | - | - | - | - |
| 18-29 | 8 794 | 43.0 | [40.8-45.2] | <0.01 |
| 30-39 | 13 074 | 39.6 | [37.5-41.7] | - |
| 40-49 | 13 089 | 40.7 | [38.3-43.2] | - |
| 50-59 | 10 683 | 43.0 | [39.8-46.3] | - |
| 60-69 | 5 887 | 40.7 | [35.8-45.9] | - |
| 70+ | 1 864 | 29.0 | [19.0-41.5] | - |
| Race Group | - | - | - | - |
| Black African | 7 883 | 46.9 | [45.2-48.5] | <0.001 |
| Coloured | 4 376 | 30.1 | [28.3-31.9] | - |
| White | 36 322 | 13.4 | [12.8-14.1] | - |
| Indian/Asian | 3 878 | 17.8 | [16.1-19.6] | - |
| Employment Status | - | - | - | - |
| Employed full-time | 28 204 | 40.0 | [38.4-41.6] | <0.001 |
| Employed informal/part-time | 3 774 | 44.8 | [40.3-49.3] | - |
| Student | 2 932 | 43.3 | [39.6-47.0] | - |
| Unemployed | 8 131 | 43.4 | [39.7-47.2] | - |
| Self-employed | 10 339 | 34.4 | [30.1-39.0] | - |
| Risk Perception | - | - | - | - |
| Low | 22 917 | 44.7 | [42.9-46.6] | <0.001 |
| Moderate | 21 110 | 38.1 | [35.8-40.4] | - |
| High | 9 458 | 38.3 | [35.6-41.0] | - |
| Self-Isolation/Quarantine Possibility | - | - | - | - |
| Yes | 24 546 | 34.1 | [32.3-36.0] | <0.001 |
| No | 11 593 | 50.9 | [48.3-53.4] | - |
| I don’t know | 17 264 | 40.2 | [37.9-42.6] | - |
| Dwelling Type | - | - | - | - |
| Formal dwelling | 52 878 | 40.0 | [38.7-41.3] | <0.001 |
| Informal dwelling | 599 | 55.7 | [49.6-61.6] | - |
| Province | - | - | - | - |
| Eastern Cape | 2 462 | 39.0 | [34.7-43.6] | <0.001 |
| Free State | 1 254 | 52.1 | [46.2-58.0] | - |
| Gauteng | 24 543 | 39.2 | [37.7-40.7] | - |
| KwaZulu-Natal | 6 399 | 39.8 | [36.9-42.7] | - |
| Limpopo | 1 020 | 48.8 | [42.1-55.6] | - |
| Mpumalanga | 957 | 40.0 | [33.9-46.4] | - |
| North West | 971 | 52.4 | [44.9-59.8] | - |
| Northern Cape | 478 | 47.2 | [39.0-55.6] | - |
| Western Cape | 15 404 | 30.8 | [29.1-32.5] | - |
| Total | 53 488 | 40.7 | [39.4-42.0] | - |
| - | National | EC | FS | GP | KZN | LP | MP | NW | NC | WC |
|---|---|---|---|---|---|---|---|---|---|---|
| Socio-Demographics | OR | OR | OR | OR | OR | OR | OR | OR | OR | OR |
| Sex | - | - | - | - | - | - | - | - | - | - |
| Male | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Female | 0.75* | 0.96 | 0.61* | 0.78* | 0.94 | 0.61 | 0.80 | 0.36* | 0.60 | 0.77* |
| Age Group | - | - | - | - | - | - | - | - | - | - |
| 18-29 | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| 30-39 | 0.92 | 0.88 | 2.12* | 0.88 | 0.76 | 1.33 | 1.10 | 0.73 | 0.90 | 0.80 |
| 40-49 | 0.97 | 0.53* | 1.21 | 1.09 | 0.98 | 0.95 | 2.10 | 0.75 | 1.00 | 0.80 |
| 50-59 | 1.07 | 1.13 | 2.07 | 1.08 | 0.85 | 1.01 | 3.00 | 0.73 | 1.40 | 0.81 |
| 60+ | 0.76* | 1.14 | 2.37 | 0.76 | 0.67 | 1.26 | 0.40 | 0.45 | 0.90 | 0.49* |
| Employment Status | - | - | - | - | - | - | - | - | - | - |
| Employed full-time | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Employed informally/part-time | 1.21 | 1.20 | 0.55 | 1.21 | 1.40 | 0.62 | 1.50 | 1.35 | 3.50 | 1.31 |
| Student | 1.07 | 0.82 | 0.81 | 1.24 | 1.04 | 0.71 | 2.00 | 1.16 | 0.70 | 1.22 |
| Unemployed | 1.21* | 0.90 | 0.84 | 1.16 | 1.32 | 0.76 | 2.40 | 1.70 | 2.00 | 1.17 |
| Self-employed | 0.78* | 0.75 | 0.54 | 0.85 | 0.76 | 0.33* | 1.00 | 1.03 | 2.00 | 0.74* |
| Knowledge | - | - | - | - | - | - | - | - | - | - |
| Knowledge score | 0.89* | 0.89 | 0.68* | 0.88* | 0.90* | 0.99 | 0.90 | 1.04 | 0.80 | 0.86* |
| Risk Perception | - | - | - | - | - | - | - | - | - | - |
| Low | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Moderate | 0.82* | 1.02 | 0.62 | 0.81* | 0.75* | 0.73 | 0.80 | 0.97 | 0.50 | 0.94 |
| High | 0.87 | 0.94 | 0.59 | 0.90 | 0.82 | 0.64 | 0.90 | 0.9 | 0.50 | 0.95 |
| Self-Isolation or Quarantine Possibility | - | - | - | - | - | - | - | - | - | - |
| No | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Yes | 0.65* | 0.54* | 0.9 | 0.60* | 0.86 | 0.76 | 0.60 | 0.41* | 0.60 | 0.69* |
Multivariate logistic regression models shows that at the national level age (compared with 18-29 years: 60 years and older, OR=0.76, 95% CI: [0.59-0.99]), being female (OR=0.75 [0.67-0.83]), employment status (compared with full-time employed: unemployed, OR=1.21 [1.02-1.44] and self-employed, OR=0.78 [0.64-0.96]), knowledge score (OR=0.89 [0.85-0.93]), risk perception (compared with low risk perception: moderate, OR=0.82 [0.72-0.93]), and perception of self-isolation or quarantine possibility (OR=0.65 [0.58-0.72]) were significantly associated with the perception that the health system was capable of managing the COVID-19 pandemic (Table 2).
| Province | Total Population | Public Hospitals | Private Hospitals | Total Hospitals | Public Hospital Beds | Private Hospitals Beds | Total Hospital Beds | Public ICU Beds | Private ICU Beds | Total ICU Beds |
|---|---|---|---|---|---|---|---|---|---|---|
| Eastern Cape | 6 712 276 | 91 | 17 | 108 | 13 200 | 1 723 | 14 923 | 93 | 110 | 203 |
| Free State | 2 887 465 | 34 | 13 | 47 | 4 798 | 2 337 | 7 135 | 109 | 114 | 223 |
| Gauteng | 15 176 116 | 39 | 83 | 122 | 16 656 | 14 278 | 30 934 | 330 | 1 132 | 1 462 |
| KwaZulu-Natal | 11 289 086 | 77 | 12 | 89 | 22 048 | 4 514 | 26 562 | 273 | 305 | 578 |
| Limpopo | 5 982 584 | 42 | 10 | 52 | 7 745 | 600 | 8 345 | 34 | 28 | 62 |
| Mpumalanga | 4 592 187 | 33 | 13 | 46 | 4 745 | 1 252 | 5 997 | 25 | 63 | 88 |
| North West | 4 027 160 | 22 | 14 | 36 | 5 132 | 1 685 | 6 817 | 54 | 87 | 141 |
| Northern Cape | 1 263 875 | 16 | 2 | 18 | 1 523 | 293 | 1 816 | 21 | 27 | 48 |
| Western Cape | 6 844 272 | 53 | 39 | 92 | 12 241 | 4 385 | 16 626 | 222 | 291 | 513 |
| South Africa | 58 775 021 | 407 | 203 | 610 | 85 362 | 31 067 | 119 155 | 1 178 | 2 140 | 3 318 |
At provincial level, the models show that in the Eastern Cape, perception of self-isolation or quarantine possibility (OR=0.54 [0.37-0.8]) and age 40-49 years (OR=0.53 [0.31-0.91] compared to 18-29 years) were significantly associated with decreased odds of perceiving that the health system was capable. In the Free State, females (OR=0.61 [0.37-0.99]) and knowledge score (OR=0.68 [0.55-0.85]) were significantly associated with decreased odds of perceiving that the health system was capable while age 30-39 years (OR=2.12 [1.05-4.28] compared to 18-29 years) was significantly associated with increased odds of this perception. In Gauteng, females (OR=0.78 [0.69-0.89]), knowledge score (OR=0.88 [0.83-0.94]) and moderate risk perception (OR=0.81 [0.7-0.93] compared to low risk perception) were significantly associated with decreased odds of the perception. In KwaZulu-Natal, knowledge score (OR=0.90 [0.82-0.99]) and moderate risk perception (OR=0.75 [0.56-1.0] compared to low risk perception) were significantly associated with decreased odds of perception. In Limpopo being self-employed (OR=0.33 [0.13-0.81] compared with being in full-time employment) was significantly associated with decreased odds of perception. In the North West, females (OR=0.36 [0.20-0.67]) and perception of self-isolation or quarantine possibility (OR=0.41 [0.23-0.72]) were significantly associated with decreased odds of perception. In the Western Cape, females (OR=0.77 [0.65-0.92]), 60 years and older (OR=0.49 [0.35-0.68] compared to 18-29 years), being self-employed (OR=0.74 [0.56-0.97] compared to being in full-time employment), knowledge score (OR=0.86 [0.80-0.93]) and perception of self-isolation or quarantine possibility (OR=0.69 [0.58-0.81]) were significantly associated with decreased odds of perceiving that the health system was capable of managing the COVID-19 pandemic.
3.3. Health System Capacity
Table 3 shows secondary data on total population, hospitals, hospital beds, and ICU beds by province. Gauteng, the most populated province (smallest by geographic area) had the highest number of hospitals, however, these were mainly private hospitals (83) compared to 39 public hospitals. There were more hospital beds in public hospitals than in private hospitals, whereas the opposite was the case with regard to ICU beds across the country.
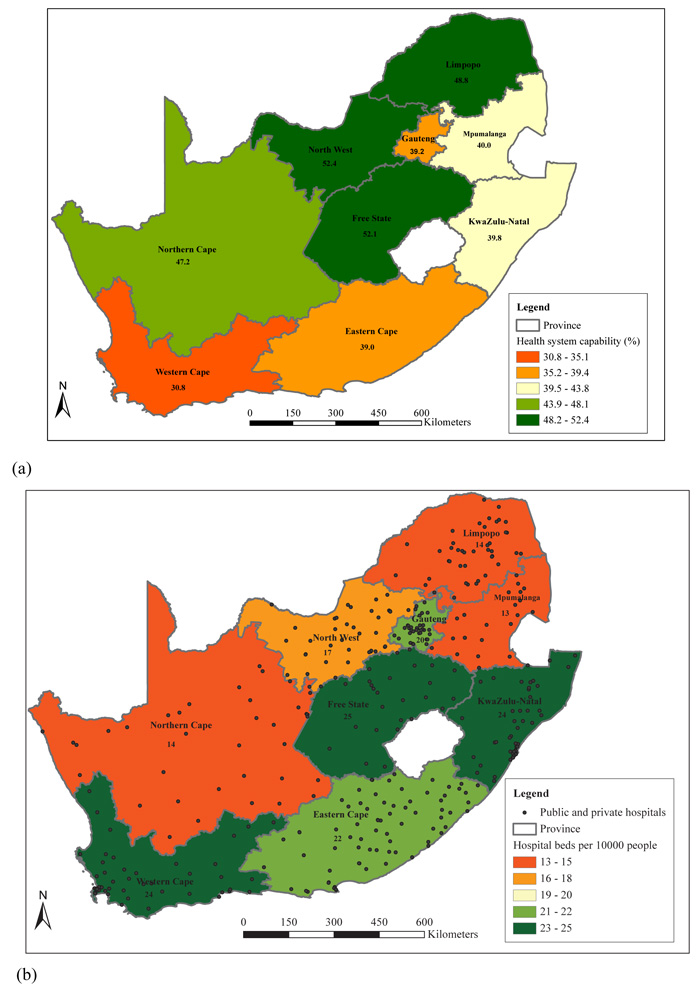
Fig. (2) shows the results from the spatial density analysis of hospitals and hospital beds per population. KwaZulu-Natal, Gauteng, Limpopo and North West had the lowest number of hospitals per 100 000 people with 0.79, 0.80, 0.87 and 0.89 respectively (Fig. 2a). All the remaining provinces had more than one hospital per 100 000 people. Free State had the highest with 1.63 hospitals per 100 000 people. Gauteng had the highest number of hospital beds, followed by Western Cape, KwaZulu-Natal and Eastern Cape, with more than 10 000 beds in their hospitals. Mpumalanga, Limpopo and Northern Cape had the lowest number of hospital beds per 10 000 people (Fig. 2b). Gauteng, which was among those with the lowest number of hospitals per 100 000 people, fell under the second-highest category with 20 hospital beds per 10 000 people. Free State, KwaZulu-Natal and Western Cape had the highest number of hospital beds per 10 000 people with 25, 24 and 24 respectively. Fig. (2b) also shows the broad spatial distribution of private and public hospitals across different provinces.
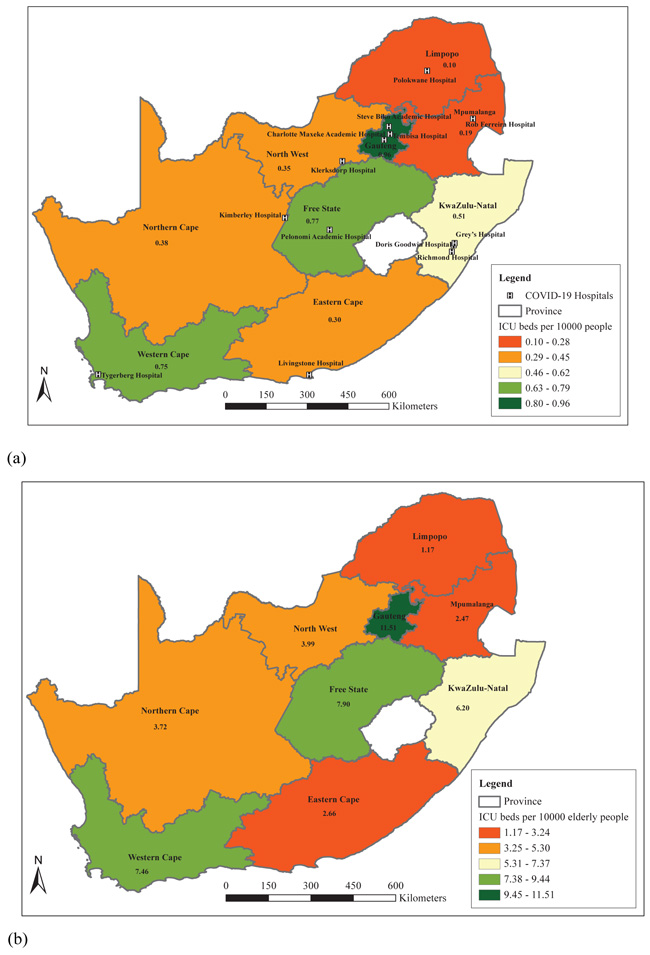
With regard to the number of ICU beds per 10 000 people, Limpopo and Mpumalanga fell in the lowest category of 0.10 to 0.28 ICU beds per 10 000 people (Fig. 3a). Gauteng, Free State and Western Cape, had the highest ICU beds per 10 000 people. Fig. (3a) further depicts the spatial distribution of hospitals earmarked to attend to COVID-19 patients. Almost all provinces, except Gauteng, seems to have an unbalanced location of the COVID-19 hospitals. The authors are not aware of the factors that were considered when selecting the current COVID-19 hospitals. From a geographic point of view, it appears that the hospitals in each province are often located in some major cities which are not necessarily centrally located within their province. Therefore, these hospitals are not easily accessible to a large proportion of a province’s population, especially if the patients will be transported by road. Hence, at least two hospitals per province could have resolved the skewness of this spatial distribution. KwaZulu-Natal in particular, has all three COVID-19 hospitals around Pietermaritzburg, which raises some spatial concern in terms of physical accessibility of these COVID-19 hospitals. For the vulnerable population, the elderly, a similar pattern was noticed, except for the Eastern Cape, which ranked in the second-lowest category of numbers of ICU beds per 10 000 people but had one of the lowest numbers of ICU beds per 10 000 elderly people. Limpopo, Mpumalanga and the Eastern Cape had between 1.17 and 3.24 ICU beds per 10 000 elderly people (Fig. 3b).
4. DISCUSSION
Overall the study findings show that people had low confidence in the South African health system, with only two out of five people indicating they thought the health system would be able to manage the COVID-19 pandemic. In similar studies conducted in Denmark and Finland, respondents reported high rates of confidence in their health systems capability to manage COVID-19 with 86% and 78% respectively [30, 31]. Black Africans, those employed part-time or informally and informal dwellers had higher confidence in the health system capability while the White population group, self-employed and those residing in formal dwellings had lower confidence in health system capability to manage the COVID-19 pandemic. This demonstrates clear divisions based on socio-economic status, geolocation as well as some racial differences in peoples’ perceptions. The majority of the Black Africans rely on the public health system almost exclusively, therefore, this increased confidence could well be due to the fact that they would not have alternative options in terms of access to healthcare, traditional forms of treatments aside. The lower confidence shown here by White respondents could be directed at the public health system and not the private which is usually very well resourced. The majority of the White population group have access to medical insurance and, therefore private medical care.
Furthermore, the older persons (70 years and above), those who perceived themselves at high risk of contracting COVID-19 and those who thought they might end up in self-isolation or quarantine had the lowest confidence in the health system capacity to manage the COVID-19 pandemic. This is concerning since people in older age groups are among those that are classified as highly vulnerable to the COVID-19 pandemic around the world, both in terms of infections and fatalities [32].
Sex and knowledge on COVID-19 were significantly associated with the perception of the health system’s capability to manage the pandemic at the national level and in four of the nine provinces. Females were less likely to have confidence in the health system capability to manage the COVID-19 pandemic than their male counterparts. The finding that men have more confidence in the healthcare system is surprising since previous studies reported that men generally access healthcare services much less than women do [33]. It is possible that women lacking confidence in the health system’s capability could be associated with how they perceive the quality thereof. Future research needs to examine people’s perceptions of health system capability in conjunction with the quality of care received. Age and self-isolation or quarantine possibility were key factors at the national level and in three provinces, while employment and risk perception were significant predictors at the national level and in two provinces. The vulnerable group, elderly (60 years and older), was a key determinant of people’s confidence in the health system capability to manage the COVID-19 pandemic at the national level and in the Western Cape. People’s risk perceptions (which are influenced by age and degree of perceived vulnerability) and knowledge about a public health problem often result in lower confidence in managing the problem.
Spatial accessibility has been previously reported to represent an important barrier to accessing healthcare services [17]. Spatial access to COVID-19 hospitals in our findings raises some concerns regarding the readiness to manage the COVID-19 pandemic, especially considering that most patients might have to be transported by road. These could be addressed by at least adding extra temporary hospitals earmarked for COVID-19 in each province that has only one COVID-19 hospital. Provinces have already started setting up additional healthcare facilities in preparation for the expected surge in the number of cases and the potential need for hospitalisation across the country. Predominantly rural provinces such as the Eastern Cape and KwaZulu-Natal should also undertake special context-specific planning for the provision which addresses challenges such as long distances between villages and available hospitals as well as poor road infrastructure. These extra hospitals should be allocated based on the geographic location and population distribution as well as the emerging trends of the pandemic whereby the number of cases and epicentres have been shifting since the outbreak of the COVID-19 pandemic. The Western Cape initially only had one hospital earmarked for COVID-19 in the early stages of the epidemic when our study was conducted. This later changed dramatically, with the province now being regarded as one of the epicentres for the pandemic with a high number of confirmed cases and number of deaths. This had to be revisited and more hospitals were allocated, as well as temporary hospitals being setup at the Cape Town International Convention Centre in the fight against the COVID-19 pandemic. Other provinces with big urban metros such as the Eastern Cape, Gauteng, and KwaZulu-Natal had to also readjust their plans as they all initially had three hospitals each that were earmarked for the response.
Our study findings show that the number of hospitals per population and the number of hospital beds per population across the country are generally lower compared to some international statistics from both public and private hospitals in Canada, Italy and Japan [34]. The current national average of 5.6 ICU beds per 100 000 in South Africa is slightly lower compared to those of some European countries such as the United Kingdom (6.6), France (9.7) and Italy (12.5). Turkey and Germany had the highest reported numbers with 46 and 29.2 ICU beds per 100 000 population [32].
Findings from this paper show that there were some similarities between people’s perceptions of health system capability and the actual health system capacity to manage the COVID-19 pandemic in some provinces. For instance, Free State was predominantly at the upper band in terms of the proportion of people who had confidence in the health systems capability and the actual health system capacity to manage the pandemic. Eastern Cape, on the other hand was at the lower end with regard to people’s confidence in health systems capability and health system capacity. Eastern Cape appeared at the upper bound only on the number of hospitals per 100 000 population and the number of hospital beds per 10 000 population. Surprisingly, Western Cape had the lowest score of people’s confidence in the health system capability to manage the COVID-19 pandemic, yet it was among the top for almost all density indicators of health system capacity except for the density on number of ICU beds per 10 000 elderly people where it was in the middle range. Western Cape also had the highest significant proportion of elderly people based on the online survey results. In addition, results showed that the elderly (60 years and above) was a significant predictor of people’s confidence in health system capability. This might have attributed to the lowest confidence in the health system capability in this province. Although North West and Limpopo had the highest proportions of people who felt that the health system was capable to deal with the COVID-19 pandemic, they were among the lowest in all health system capacity indicators.
The COVID-19 pandemic demonstrated and highlighted the urgency and the importance of the implementation of the NHI, especially in addressing the inequity of access to healthcare that exists between private and public health care. The COVID-19 pandemic has laid bare the health disparities that exists between different communities in the country due to historical structural systems brought about by both colonialism and the apartheid race based spatial planning and service provision. This pandemic provides the first and best opportunity for South Africa to reengineer the country’s health system to be united and integrated as much as possible between the public and private health systems. The COVID-19 block exemption for the health sector is an important step towards the testing the implementation of NHI. The government and all role players in the country should embrace this opportunity by ensuring that all systems that are necessary for the implementation of the NHI are put in place and expanded upon.
This study does have some limitations. One of the main limitations was that there was no clarity in the online questionnaire on whether the definition of the South African health system included both private and public sector. The survey relied on self-report which is prone to social desirability bias, which could have led to underestimation or overestimation of the people’s confidence in health systems capability to deal with the COVID-19 pandemic depending on how they understood and experience the health system. Respondents may also have been responding on their perceptions of the health system regardless of whether they utilise those services or not. Other than the above mentioned limitations, findings from this study contributes to the body of evidence on people’s perceptions about the South African health system capability and the state of health system capacity to manage the COVID-19 pandemic across the country.
CONCLUSION
To the best of our knowledge, this paper was the first to investigate people’s perception of the South African health system capability and the actual health system capacity to respond to the COVID-19 pandemic and its subsequent spread. Overall, most people had low confidence in the health system capability in managing the COVID-19 pandemic and that may be due to having the wrong perceptions or may be due to prior poor experiences in their interaction with healthcare facilities and/or services. Sex and knowledge on COVID-19 were significantly associated with the perception of the health system’s capability to manage the pandemic at the national level and in four of the nine provinces. Females were less likely to have confidence in the health system capability to manage the COVID-19 outbreak pandemic as compared to their male counterparts. Overall, the findings of this study clearly highlights the challenges of the country’s health system, both perceived or real that needed to be addressed as part of the preparation for the COVID-19 pandemic. Urgent policy interventions and implementations are recommended for continued increase in the number of ICU beds across the country with particular focus in Western Cape, Eastern Cape, KwaZulu-Natal and Gauteng. Timeous implementation of a countrywide NHI system is now more critical than ever in improving healthcare outcomes of the South African population even beyond the existence of the COVID-19 pandemic. Future research need to examine people’s perception of health system capability in conjunction with the quality of care received. Future research should also explore the country’s readiness for NHI implementation as well as preparedness for future waves of COVID-19 and other pandemics. People’s perception of NHI should also be explored, especially during and after the COVID-19 pandemic.
AUTHORS’ CONTRIBUTIONS
SPR conceived the study and TM conceptualised the paper. TM and RS conducted the analysis and interpreted the results. TM drafted the manuscript. TM, RS, SS, GWS, SD, TMa, IN, WP, ND, SJ, SP, KZ, MMo, MM, SPR contributed to interpreting the results and editing the manuscript. All authors read and approved the final manuscript before submission.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Ethics approval was received from the Human Sciences Research Council (HSRC) Research Ethics Committee (REC); (REC 5/03/20).
HUMAN AND ANIMAL RIGHTS
No Animals were used in this research. All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICATION
All participants provided electronic informed consent.
FUNDING
This research received no external funding.
AVAILABILITY OF DATA AND MATERIALS
All data generated or analysed during this study are available on request from the corresponding author [TM].
CONFLICTS OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Big thanks to all South African residents who participated in the HSRC COVID-19 Online Survey. Thanks to Ms. Yolande Shean for logistical and administrative support while Prof Leickness Simbayi and Prof Crain Soudien are credited for their executive support of the HSRC COVID-19 Online Survey.


