All published articles of this journal are available on ScienceDirect.
The Post-pandemic Prevalence of Refractive Errors among Elementary School Children in Jakarta
Abstract
Purpose:
To evaluate the prevalence of refractive errors among elementary school-aged children in Jakarta, particularly in post-pandemic situations.
Aim:
A cross-sectional study was conducted on 284 children in grades 4th to 6th in two elementary schools in Jakarta.
Methods:
Ophthalmological examination consisted of uncorrected visual acuity (UCVA) examination by trained teachers using a modified and simplified Snellen chart, followed by a slit lamp examination for anterior and posterior segment evaluation and best-corrected visual acuity (BCVA) examination using auto-refractometer and subjective refraction using a full Snellen chart. Demographic data were obtained via anamnesis and pre-questionnaire from the school database. Correlation between variables, the prevalence of refractive errors and characteristic demographics were analyzed through bivariate or multivariate analysis.
Results:
From a total of 284 children, 9 of the total screened children (4%) were already corrected with eyeglasses. However, the refractive screening result showed that 111 subjects (40%) were diagnosed with ametropic conditions, either with myopia and/or astigmatism. Further bivariate analysis to explore the correlation between the prevalence and subject characteristic shows that there was no statistical correlation between school grade and age of subjects toward ametropic diagnosis, even though the majority of the subjects diagnosed with ametropia were populated in younger aged children (less than 12 years old), which was as high as 62% of the total ametropic subjects, therefore clinically correlated.
Conclusion
The significantly increasing prevalence number of refractive errors post-pandemic among elementary school-aged children in Jakarta proved the worrying impact of excessive use of gadgets, online schooling and lack of outdoor activities during the last three years of social restriction in Indonesia. This high prevalence of refractive errors (generally more than 30%) was considered a public health problem. Therefore, these results will encourage the government and healthcare providers to mitigate and accelerate the screening, prevention and treatment of refractive errors in children, in a way to reduce the potential risks of future health, social, and economic problems.
1. INTRODUCTION
Refractive errors remain a leading and major contributor globally to visual impairment and overall visual problems in children. World Health Organization (WHO) estimated that more than ten million children, specifically the school-aged population, all over the world suffer from uncorrected refractive errors, mostly living in middle- to low-income countries, including Indonesia [1]. Refractive error is a vision problem that occurs when the shape of the eye prevents light transport from being focused directly on the retina. This condition can cause blurry vision and other related eye problems. In children, refractive errors can be easily corrected with optical treatments such as eyeglasses and contact lenses. The most frequent diagnoses of refractive errors in children are myopia and astigmatism. Myopia can result in blurred distance vision, while astigmatism causes distorted vision at any distance [1, 2].
The latest study in 2018 showed that the overall prevalence of refractive errors among elementary to junior high school children in Indonesia was around 28%, with myopia as the most common diagnosis [3]. Another study from Bandung in 2020 mentioned that the estimated prevalence of refractive error in children reached 22% [4]. Studies indicated an increased trend of refractive error among children in Indonesia, with one longitudinal study showing an almost two-fold increase in myopia among elementary school children between 2008 to 2016 [5].
It is commonly studied that the high prevalence of refractive errors in Indonesian children can be attributed to lifestyle changes, environmental factors, not to mention the role of prolonged screen time and lack of outdoor activities. This condition is worsened by the lack of access to eye care services and eyeglasses that are potentially limited [6]. A study in Makassar also mentioned that the knowledge and attitude toward eye care in parents and caregivers play a role in the high prevalence of refractive error in Indonesia [7].
During the pandemic, many reviews confirmed that the significant impact of limited eye care access, extremely high usage and frequent utilization of electronic gadgets has brought negative consequences on the development and progressivity of refractive errors among children [2, 8]. Therefore, this study aimed to evaluate the prevalence of refractive errors among elementary school-aged children in Jakarta, particularly in post-pandemic situations. Our hypothesis is the increasing duration of screen time during online school in confinement period during COVID-19 will increase the prevalence number of refractive errors in children, especially elementary school children.
2. METHODS
2.1. Ethical Approval
A cross-sectional study was conducted after receiving ethical approval from the Medical Faculty of Unika Atmajaya’s institutional ethics. All methods were performed according to the relevant guidelines and regulations of the Declaration of Helsinki.
2.2. Statistical Analysis
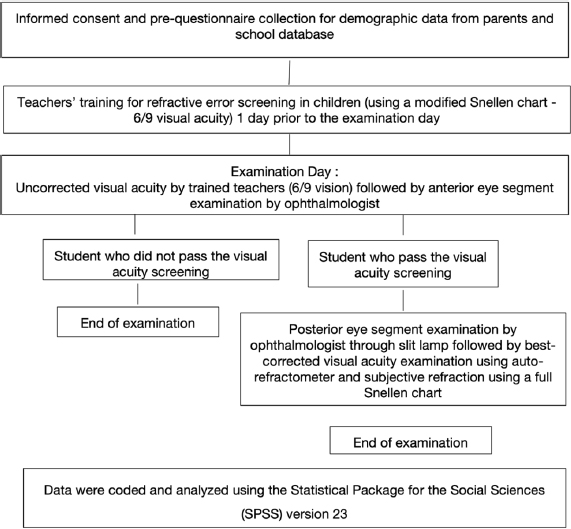
This study was conducted in two elementary school-based settings in Jakarta's urban area. This study included students of grades 4th to 6th at the time of screening performed, purposively sampling by covering all children who received written informed consent from their parents collected through google-form, a few days before the examination in-class examination process. As described in Fig. (1), the ophthalmological examination consisted of uncorrected visual acuity (UCVA) examination by trained teachers using a modified and simplified Snellen chart, followed by a slit lamp examination for anterior and posterior segment evaluation and best-corrected visual acuity (BCVA) examination using auto-refractometer and subjective refraction using a full Snellen chart. Demographic data was obtained via anamnesis and pre-questionnaire from the school database. Data were coded and analyzed using the Statistical Package for the Social Sciences (SPSS) version 23 (SPSS Inc., Chicago, IL, USA). Correlation between variables, the prevalence of refractive errors and characteristic demographics were analyzed through bivariate or multivariate analysis. The statistical significance was set at p < 0,05.
3. RESULTS
A total of 284 children of grades 4th to 6th from two elementary schools in the Jakarta urban area were screened from February to March 2023. As shown in Table 1, the subjects ranged in age from 9 to 15 years with the majority (69%) of them being 11-12 years old. Based on the refractive examination, two subjects showed exotropia, one with congenital malformation of the eyelid (epiblepharon) and no major anatomical disorder for the rest of the subjects. Before the refractive examination had been done, there were 9 of the total screened children (4%) already corrected with eyeglasses.
| Variable | Subject | |
|---|---|---|
| n (284) | % | |
| Grade in elementary school | ||
| 4th | 64 | 22 |
| 5th | 104 | 37 |
| 6th | 116 | 41 |
| Age (Years) | - | - |
| 9 | 7 | 3 |
| 10 | 64 | 23 |
| 11 | 112 | 39 |
| 12 | 86 | 30 |
| 13 | 9 | 4 |
| 14 | 3 | 0.5 |
| 15 | 3 | 0.5 |
| Eyeglasses or spectacles | - | - |
| Yes | 9 | 4 |
| No | 275 | 96 |
| Diagnosis | Subject | |
|---|---|---|
| n (284) | % | |
| Ametropia (Myopia and Astigmatism) | 111 | 40 |
| Emmetropia | 173 | 60 |
| Variable | Diagnosis | OR | 95% CI | p | |||
|---|---|---|---|---|---|---|---|
| Ametropia | Emetropia | ||||||
| N (111) | % | N (173) | % | ||||
| Grade in school | |||||||
| 6th | 47 | 42% | 70 | 42% | - | - | 0,492 |
| 5th | 40 | 36% | 63 | 36% | - | - | - |
| 4th | 24 | 22% | 40 | 22% | - | - | - |
| Age | - | - | - | - | - | - | - |
| ≥12 years | 42 | 38% | 53 | 31% | 1,10 | 0,72 – 1,67 | 0,657 |
| <12 years | 69 | 62% | 120 | 69% | - | - | - |
| Eyeglasses ^ | - | - | - | - | - | - | - |
| Yes | 9 | 8% | 0 | 0% | 3,10 | 2,52 – 3,81 | 0,001* |
| No | 102 | 92% | 173 | 100% | - | - | - |
The refractive screening result showed that 111 subjects were diagnosed with ametropic conditions, either with myopia and/or astigmatism, hence the prevalence of refractive error in this study is 40% (Table 2). We performed a bivariate analysis to further explore the correlation between the prevalence and subject characteristics, as described in Table 3. It shows that there was no statistical correlation between school grade and age of the subject toward ametropic diagnosis, even though the majority of the subjects diagnosed with ametropia were populated in younger aged children (less than 12 years old), which was as high as 62% of the total ametropic subjects, therefore clinically correlated. However, the eyeglasses correction significantly correlated with the prevalence of refractive errors causing ametropia, either myopia and/or astigmatism [OR (95%CI):3,1 (2,52–3,810; P=0,001].
4. DISCUSSION
This present study is the first research that evaluated the prevalence of refractive errors in elementary school-aged children in Jakarta post-COVID-19 pandemic. As we learned from many literature reviews in the field of vision health, during the pandemic, the excessive use of gadgets and prolonged online learning activities may have a significant impact on the development of refractive errors in children [9]. A cross-sectional survey in Jordan concluded the negative effect of COVID-19 home confinement with eye problems due to a significant increase in usage time of digital devices [9]. Another study in India also showed a three- to six-fold rise in myopia post-home confinement among public school children [10]. Our finding supports these studies and confirms our hypothesis. The prevalence of refractive errors in our study, which was as high as 40%, both myopia and astigmatism, is considered significantly high especially when we compare it with the prevalence of a pre-pandemic study performed by Halim et al. from Bandung in 2020 [4]. This high prevalence number reflected that 1 out of 4 elementary children in Jakarta suffered from refractive errors.
What we found during eye examinations in two urban elementary schools was the inconvenient fact that there was only 4% of children have had previous eyeglasses correction. This rate is enormously lower compared to the findings of the corrected rate in Vietnam [11]. Knowing that only 4% of children have received eyeglasses correction before our eye screening shows a huge potential vision health problem in this city. One study also showed that a high prevalence of refractive errors (generally more than 30%) was considered a public health problem [12]. Our causative hypothesis of these unfortunate findings is not dominantly because of the lack of knowledge from the parents and caregiver side, but also other variables including the healthcare system during the pandemic. With so many changes and challenges COVID-19 brought, during the initial wave of COVID-19, in-hospital mortality rates were high and viable treatment options were scarce. This major disruption in healthcare services during the COVID-19 pandemic forced government and healthcare providers to deprioritize non-emergency medical services, including eye care [1, 13]. This condition might have influenced the behaviors of parents with eye problems and children to not seek medical advice and help. It is worsened by the already low-knowledge-parents attitude to postpone or even cancel the visual examination, leading to delays in detecting and treating refractive errors in their children.
Even though most of the uncorrected refractive errors can be easily treated with glasses or contact lenses, our study provides new insights that there is a gap in routine eye care services in Jakarta during the pandemic. This phenomenon is inevitable during the initial wave, however, starting from the second wave onward, many countries began utilizing telemedicine for retinopathy screening, particularly in specific populations [12, 14]. Unfortunately, telemedicine may not have been considered urgent for young children, especially eye problems, potentially leading to delayed diagnosis and delayed treatment. Consequently, the increased percentage of diagnosed children might partly reflect the postponed evaluations that should have occurred in previous years.
When this figure is found in the school-aged children population, the scorching problem is even bigger. Various researchers have confirmed that children with uncorrected refractive errors will potentially have reduced visual acuity affecting their academic performances, reading abilities and overall learning process [2, 15, 16]. Uncorrected refractive errors in children also can cause visual discomfort and chronic consequences leading to a decreased passing grade in school [15, 16]. The children's daily activities and sports playing performance with uncorrected refractive errors were also hindered [17].
The long-term impact brings social and economic consequences as well. Children with uncorrected refractive errors may experience social isolation, stigmatization and bullying due to their reduced visual acuity. In the long run, many longitudinal cohort studies figured out that uncorrected refractive errors manifested in productivity loss, and increased healthcare costs due to the development of comorbidities such as amblyopia or lazy eye and other forms of eye disorders [14, 18].
Therefore, a clear mitigation plan and community refractive error correction initiative must be activated to reduce potential future risks to our children’s vision health and overall wellness. Access to eyeglasses as the golden standard corrective method is deemed necessary and should be widely and easily accessible at the household level. The learning from our study is undebatable that the prevalence of uncorrected refractive errors among elementary school-aged children in Jakarta is tremendously high and potentially can cause future public health impact. Referring to previous pre-pandemic studies resulted in a lower rate of eye problems [2], it reiterates our hypothesis that the distance-learning method with online-gadget medium, majorly contributes to the high prevalence of refractive errors (myopia and astigmatism) in children in Jakarta. Serious intervention is required to accelerate eye screening programs in school, as we had done in our study, to screen, diagnose and treat refractive errors in children, and eventually to stop the progressivity of future health, social and economic problems that can be caused by uncorrected refractive errors.
5. LIMITATIONS OF THE STUDY
In reporting the outcome of this study, three limitations of this study should be highlighted. One limitation of this study is the small sample size unable to ensure a representative distribution of the population to be considered representative of groups of elementary school children in Jakarta. Additionally, information regarding the types of devices used at home and the duration of screen time are not provided. Many newer laptops incorporate special features to reduce the strain on the eyes, such as adjusting screen brightness based on ambient light conditions and the time of day. Thirdly, the light intensity of the examination room when conducting this study is not measured. Certain light intensity should be ensured to make sure that the room is appropriate to conduct eye examinations. Further studies with bigger sample sizes in more distributive areas in Jakarta’s elementary school should be conducted.
CONCLUSION
The post-pandemic prevalence of refractive errors among elementary school-aged children in Jakarta is 40%, higher than the pre-pandemic study, which proved the worrying impact of excessive use of gadgets, online schooling and lack of outdoor activities during the last three years of social restriction in Indonesia. The correction rate is even lower, only reaching as low as 4% of children with myopia and astigmatism, which leaves a major piecework to the government and healthcare providers to mitigate and accelerate the screening, prevention and treatment of refractive errors in children, in a way to reduce the potential risks of future health, social, and economic problems.
LIST OF ABBREVIATIONS
| WHO | = World Health Organization |
| BCVA | = best-corrected visual acuity |
| SPSS | = Statistical Package for the Social Sciences |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The study was approved by the Institutional Review Board of Unika Atmajaya’s Medical Faculty.
HUMAN AND ANIMAL RIGHTS
No animals were used in this research. All procedures performed in studies involving human participants were in accordance with the ethical standards of institutional and/or research committee and with the 1975 Declaration of Helsinki, as revised in 2013.
CONSENT FOR PUBLICATION
Written informed consent has been obtained from the parents’ subjects to publish this paper.
STANDARDS OF REPORTING
STROBE guidelines were followed.
AVAILABILITY OF DATA AND MATERIALS
The data and supportive information are available within the article.
FUNDING
This research received no external funding.
CONFLICT OF INTEREST
The authors declare no conflict of interest.
ACKNOWLEDGEMENTS
We would like to extend our gratitude and appreciation to the teachers, parents and children in two elementary schools in Cikini and Kayu Putih for the operational support of our study. Also, appreciate the contribution of Ibu Anindiarti in field work of this study and project.


