All published articles of this journal are available on ScienceDirect.
Utilization of Cervical Cancer Screening Services among Women in Vhembe District, South Africa: A Cross-Sectional Study
Abstract
Aim:
Screening for early detection and treatment of cervical cancer is a cornerstone of prevention. The purpose of this study was to assess the awareness in women about the utilization of cervical cancer screening services in Vhembe District, South Africa.
Methods:
This cross-sectional study involved a random selection of 500 women aged 20-59 years in Vhembe District, Limpopo Province, South Africa. Data was collected via a self-structured questionnaire on the demographic variables, provision, utilization and awareness of cervical cancer screening services.
Results:
The majority of the participants agreed to have cervical cancer screening services in their clinics (79.2%), and never had a Pap smear (58.6%). Most women would not go for cervical cancer screening, mainly because of a lack of facilities (30.0%), fear of pain (24.4%), and embarrassment (15.2%). Most participants indicated that Pap smear test meant scraping the cervix to detect abnormal cancerous cells (39.2%) and 34.2% did not know a Pap smear. Majority of the participants indicated Pap smears should be done every 10 years (65.8%); Pap smears could detect cervical cancer earlier (66.8%), and had heard about cervical cancer (71.6%). The majority of the participants considered cervical cancer as a serious problem to warrant considerable attention (59.4%); and some perceived cervical cancer as transmittable through multiple sexual partners (22.2%). The majority of the participants were aware of a vaccine against cervical cancer for girls at school (69.0%), and it was indicated that government should use health education to encourage women to attend cervical screening services (51.6%).
Conclusion:
Despite the free availability of cervical cancer screening services and awareness, the utilization of cervical cancer screening services is low. There is a need to intensify cervical screening health talks and campaigns, and to provide alternative accessible options for screening services for women in rural areas.
1. INTRODUCTION
Globally, cervical cancer, a public health problem is the second most common cancer among women, with an estimated 528, 000 new cases and 266,000 deaths among women each year [1]. It is estimated that yearly, between 20,000 to 30,000 women, mostly in poor countries, die of cervical cancer [2]. The prevention, control and treatment of cervical cancer are a public health priority [3]. Cervical cancer is a killer disease and is incurable, if it is at an advanced stage [4, 5]. Early screening is a proven, cost-effective, cervical cancer control strategy [6]; and thus, early screening of cervical cancer is an important preventative strategy.
Cervical cancer mortality rates in low resource countries are nearly three times higher than the rates experienced in high resource settings [1, 7, 8]. For example, in developed countries like the USA, 40% of women diagnosed with cervical cancer die from it, whereas in Africa, the equivalent death rate is 78% [9]. In the United Kingdom (UK), there was a 42% reduction in cervical cancer after the National Health System implemented cervical cancer programmes successfully [2]. In India, cervical cancer accounts for one-fifth of the world burden of the disease because there are no cervical cancer screening programmes [10]. In Australia, the number of women diagnosed with cervical cancer dropped on average by 4.5% each year, which was attributed to a comprehensive cervical cancer programme’s impact that dropped cervical cancer to the 18th most common cause of cancer death in women [3]. In Sub-Saharan Africa, cervical cancer comprises 20-25% of all cancers among women. The estimate doubles that of women worldwide. Its incidence ranges from 30-40 per 100,000 women [10]. Cervical cancer is the most incident cancer and the leading cause of cancer mortality in Ghanaian women [11]. Therefore, in countries where there are no cervical cancer screening services, cervical cancer becomes a public health burden.
Cervical cancer screening was introduced in 2000 in South Africa. A projected 70% coverage of cervical cancer by 2010 was targeted, but to date, only 13.6% coverage has been reached [3]; the cervical cancer mortality rate is still high. For the vast majority of women in South Africa, screening services are neither available nor function effectively, or, they are inaccessible to those who need them, thus affecting the utilization of cervical cancer services negatively [12].
In South Africa, the cervical cancer screening services are provided by Primary Health Care Nurses (PHCNs) in the clinics and in the private sector; and screening is done mostly when guidelines recommend or when people have symptoms [10]. The National Department of Health, South Africa [12] is committed to reducing the incidence, morbidity and mortality rate of cervical cancer in South Africa by performing cervical cancer screening for about 15% of women at the age of 30 years and above, and by reducing the cervical cancer incidence in women 30 years and older.
Although cervical cancer motivational talks, campaigns and cervical cancer screening services are provided for women in all the clinics in Vhembe District [13], generally, there are very few women who voluntarily present themselves for cervical screening services. Women who utilize the cervical cancer screening services, do so because they have been referred by other health facilities or the women are presenting with symptoms. Factors associated with poor utilisation of cervical cancer screening services are fear of embarrassment, pain and stigmatisation [14, 15], time constraint [11, 16], lack of awareness about where to get screening [11, 17], the associated costs [11, 14, 18], the attitudes of health workers [19] and delays in hospitals cancer screening [11]. Cervical cancer screening services could be utilised better if cervical cancer screening awareness campaigns were sustained and the services accessible, affordable and available [20]. The objective of this study, therefore, was to assess the awareness of women on the utilisation of cervical cancer screening services in Vhembe District, South Africa.
2. METHODS
2.1. Setting
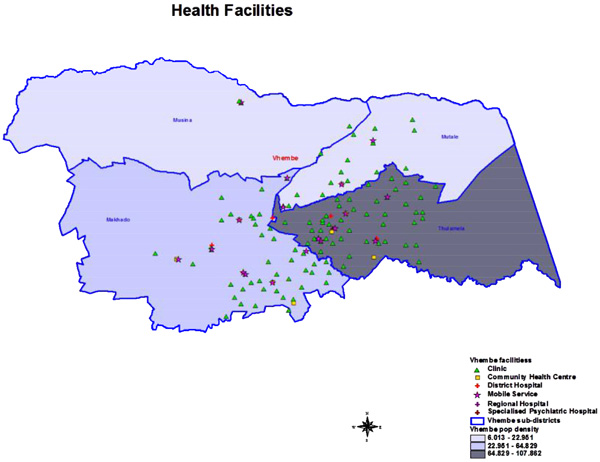
The study was conducted in Vhembe District, which is divided into four municipalities: Thulamela, Makhado, Mutale and Musina. Thohoyandou, is the current capital of Vhembe District. The people are mostly black Africans and Vhavenda speaking; however, the majority of the health facilities offering cervical cancer screening services are advertised by posters written mostly in English, Afrikaans, Sesotho, Zulu or Xhosa. Vhembe District is predominantly rural and most households are female-headed. The poor roads affect ambulances, mobile clinics and transportation in general. Most people are unemployed (18.6%) and illiterate, as they cannot read and write in English or read their own local language in health services advertisements [21]. Fig. (1) shows areas where PHCNs provide cervical cancer screening in the four municipalities, that is, it displays the physical location of clinics, community health centres and mobile clinics.
2.2. Design
Cross-sectional, quantitative research was conducted to assess the awareness of women on the utilization of cervical screening services in the Vhembe District of the Limpopo Province.
2.3. Population and Sampling
The target population was women aged 20-59 years; women who were attending health clinics in the Vhembe District. The statistics of women visiting the selected clinics for various health problems in the past period of four months before data collection was 5000 women as follows: 1650 (Thulamela), 1210 (Makhado), 1190 (Mutale), and 950 (Musina). The appropriate sample size was estimated using the following formula:
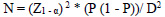 |
Where Z is the confidence level, P is the expected population of women visiting the clinics due to health reasons, and D is the margin of error. P was set at 5000 and D at 0.045. The calculation was performed at 95% confidence level. The required sample size for the study was 433 participants. However, 500 participants were included in the study to address possible incomplete and missing responses. The probability proportional to the size of women visiting each study site was selected: 165 in Thulamela, 121 in Mkhado, 119 in Mutale and 95 in Musina. Inclusion criteria were women aged between 20-59 years, because cervical cancer commonly affects women in this age group [4]; and it included women who had previously received cervical cancer screening services.
2.4. Data Collection
A self-administered questionnaire was used for data collection. The questionnaire contained closed-ended items. The questionnaire was divided into four sections, namely, the demographical variables (age, educational level, source of income, marital status, employment); perceptions regarding the provision, utilisation and awareness of cervical cancer screening services. Participants who could not read and write in English or Tshivenda (local language) were assisted by the research assistants. Participants were interviewed using the questionnaire in a private space, without friends, family members or husbands.
2.5. Ethical Considerations
The University of Venda Ethics Committee granted ethical clearance for the study (Ref: SHS/14/PDC/02/1908). Permission to conduct the study was also obtained from the Limpopo Provincial Health Department and the Vhembe District Department of Health. Furthermore, permission was granted to access the facilities and utilise selected clinics and PHCNs. Informed consent was obtained from the participants, prior to data collection. Anonymity and privacy were maintained throughout the study. Participants were allowed to withdraw from the study, at any point of the research process, without prejudice or penalty. The consent form and the questionnaire were written in English and Tshivenda. Participants who could not write and read were briefed about the aim and nature of the study and were asked to thumbprint as an indicator of consenting to participate in the study.
3. DATA ANALYSIS
Descriptive statistics (frequencies and percentages) were used to summarise the data. Data sets were analyzed using the Statistical Package for Social Sciences (SPSS) version 22.0.
4. RESULTS
Most participants were 30-39 years old (29.6%), followed by 50-59 years (24.4%), had grade 1-7 (25.2%) and a tertiary education (11.2%). Their sources of income were mainly pension (51.0%) and a monthly salary (28.8%), while 57 women (11.4%) had no income. Most of the participants were married (40.2%), single (37.0%) or widowed (13.2%) and unemployed (146=29.2%) (Table 1).
| Variables | n(%) |
|---|---|
| Age (years) | |
| 20-29 | 117(23.4) |
| 30-39 | 148(29.6) |
| 40-49 | 113(22.6) |
| 50-59 | 122(24.4) |
| Level of education | |
| No formal schooling | 230(46.0) |
| Grade 1-7 | 126(25.2) |
| Grade 8-12 | 88(17.6) |
| Tertiary | 56(11.2) |
| Source of income | |
| Monthly salary | 144(28.8) |
| Pension | 255(51.0) |
| Business | 44(8.8) |
| No income | 57(11.4) |
| Whether income is enough to cater for the family | |
| Enough | 113 (26.6) |
| Not enough | 387 (77.4) |
| Marital status | |
| Single | 185(37.0) |
| Married | 201(40.2) |
| Divorced | 48(9.6) |
| Widowed | 66(13.2) |
| Type of employment | |
| Employed | 46(9.2) |
| Non-government employment | 195(39.0) |
| Self-employed | 57(11.4) |
| Student | 19(3.8) |
| Unemployed | 146(29.2) |
| Retired | 37(7.4) |
The majority of the participants indicated having received cervical cancer screening services in their clinics (396/79.2%); some of the clinics were 5 km away from their homes (236/47.2%). Majority of the participants never had a Pap smear done (293/58.6%); and for some participants, their husbands did not support Pap smear screening (141/28.2%). Most of the participants agreed that being ill (153/30.6%) was the reason for having a Pap smear. However, most women would not go for cervical cancer screening mostly because of a lack of facilities (150/30%), fear of pain (122/24.4%) and embarrassment (76/15.2%). Most participants indicated having followed-up on their Pap smear results after screening (224/44.8). The majority of the participants indicated that the community health workers (301/60.2%), and others maintained that stockvel (140/28.0%) groups were available to provide cervical cancer services (Table 2).
| Statements | n(%) |
|---|---|
| Clinic having cervical cancer screening services | |
| Yes | 396(79.2) |
| No | 104(20.8) |
| Distance of clinic from home | |
| Within 5 km | 264(52.8) |
| 5 km and more | 236(47.2) |
| Mode of transport to the clinic from your home | |
| Public transport | 184(36.8) |
| Own transport | 35(7.0) |
| On foot | 281(56.2) |
| Ever had a Pap smear | |
| Yes | 207(41.4) |
| No | 293(58.6) |
| Husband supportive of a Pap smear | |
| Yes | 60(12) |
| No | 141(28.2) |
| Reason for a Pap smear | |
| Illness | 153(30.6) |
| Cervical cancer screening | 92(18.4) |
| Voluntary | 59((11.8) |
| Family planning | 88(17.6) |
| Postnatal care | 108(21.6) |
| Reasons for not doing a Pap smear | |
| Embarrassment | 76(15.2) |
| Painful | 122(24.4) |
| Long queues | 40(8.0) |
| Long procedure | 10(2.0) |
| Hatred | 41(8.2) |
| No equipment | 150(30) |
| If you had once done a Pap smear, did you return for the results? | |
| Yes | 224(44.8) |
| No | 95(19.0) |
| Do you have a problem with a Pap smear being administered by male? | |
| Yes | 281(56.2) |
| No | 219(43.8) |
| If employed, is it mandatory for the staff at your workplace to have cervical cancer screening? | |
| Yes | 92(18.4) |
| No | 149(29.8) |
| Availability of community groups | |
| Cancer groups | 5(1.0) |
| Community health workers | 301(60.2) |
| Stockvel groups | 140(28.0) |
| Football group | 54(10.8) |
With regard to awareness of the utilisation of cervical cancer screening services (Table 3), most participants indicated that a Pap smear test meant scraping of the cervix to detect abnormal cancerous cells (196/39.2%) and 171 participants (34.2%) did not know Pap smear. The majority of the participants indicated that a Pap smear should be done every 10 years (329/65.8%); Pap smears could detect cervical cancer earlier (334/66.8%); and had heard about cervical cancer (358/71.6%). Most participants indicated hearing about cervical cancer mostly at the clinic (247/49.4%) and on the radio (161/32.2%). The majority of the participants considered cervical cancer as a serious problem that warranted considerable attention (297/59.4%). They perceived cervical cancer to be transmittable by having multiple sexual partners (111/22.2%). Most participants got information on cervical cancer in public areas (86/17.2%) and at schools (57/11.4%). The majority of the participants were aware of a vaccine against cervical cancer for girls at school (345/69.0%).
| Statements | n(%) |
|---|---|
| What is a Pap smear test? | |
| A scraping of the cervix to look for abnormal cancerous cells | 196(39.2) |
| Treatment of cancer | 93(18.6) |
| Test for sexually transmitted infections | 40(8.0) |
| Don’t know | 171(34.2) |
| How frequently should a Pap smear be done? | |
| Yearly | 105(21.0) |
| Every 2 years | 27(5.4) |
| Every 5 years | 39(7.8) |
| Every 10 years | 329(65.8) |
| Do you perceive that a Pap smear can detect cervical cancer earlier? | |
| Yes | 334(66.8) |
| No | 166(33.2) |
| Have you ever heard about cervical cancer? | |
| Yes | 358(71.6) |
| No | 142(28.4) |
| Where have you heard about cancer? | |
| Radio | 161(32.2) |
| Television | 39(7.8) |
| Clinic | 247(49.4) |
| Church | 53(10.6) |
| Do you regard yourself as vulnerable to cervical cancer? | |
| Yes | 134(26.8) |
| No | 366(73.2) |
| Do you consider cervical cancer as a serious problem to warrant consideration? | |
| Yes | 297(59.4) |
| No | 203(40.6) |
| Which of the following do you think increases your chance of having cervical cancer? | |
| Multiple sexual relationships | 111(22.2) |
| If your partner has a sexual relationship with many women | 42(8.4) |
| Being sexually active at a young age | 60(12.0) |
| Using the same bath as somebody who has cervical cancer | 23(4.6) |
| Failure to use condoms | 69(13.8) |
| Don’t know | 195(39.0) |
| Have you ever come across information related to cervical cancer written on: | |
| Refrigerator magnets | 26(5.2) |
| Plastic grocery bags | 19(3.8) |
| Public areas | 86(17.2) |
| Bill boards along the road | 27(5.4) |
| Schools | 57(11.4) |
| Sanitary pads | 67(13.4) |
| None | 218 (43.6) |
| Are you aware that there is a vaccine against cervical cancer provided to girls at school? | |
| Yes | 345(69.0) |
| No | 155(31.0) |
| Are you aware of other health professionals, like a doctor, social worker or dietician working in this clinic? | |
| Yes | 490(98.0) |
| No | 10(2.0) |
Table 4 concerns the interventions to promote utilisation of cervical cancer screening services. Participants indicated that health education (258/51.6%) and campaigns (148/29.6%) should be used mostly by the government to encourage women to attend cervical screening services.
| Statements | n(%) |
|---|---|
| Strategies used by the government to encourage women to attend cervical cancer screening services | |
| Health education | 258(51.6) |
| Cervical screening campaigns | 148(29.6) |
| Cell phone reminders | 1(0.2) |
| What else can be done to encourage women to attend cervical cancer screening? | |
| 24-hour services | 1(0.8) |
| Advertisement | 5(1.2) |
| Don’t know | 10(2) |
| Teaching | 26(5.2) |
| Awareness campaign | 7(1.4) |
| Groups | 6(1.2) |
| Door-to-door | 10(2) |
| School | 1(0.8) |
| Compulsory screening | 6(1.2) |
| Give caps | 2(0.4) |
| Give T-shirt | 3(0.6) |
| Give flag | 3(0.6) |
| Develop magazines | 4(0.5) |
| Give pamphlets | 7(1.4) |
| Encourage women to go for screening | 1(0.8) |
| Offer free services | 1(0.8) |
| Encourage use of condoms | 2(1.4) |
| Use of radio | 1(0.8) |
| Poster | 2(1.4) |
| Build clinics | 1(0.8) |
| Threaten women to go for screening | 1(0.8) |
| Use community health workers | 6(1.2) |
| Use special women at clinics | 1(0.8) |
| Use letters | 1(0.8) |
| Use cell phone reminders | 2(0.4) |
| Use community members | 1(0.8) |
| Use civic organizations | 1(0.8) |
| Services to be provided by competent professionals | 1(0.8) |
| Use of chiefs | 1(0.8) |
5. DISCUSSION
The present study assessed the awareness of women concerning the utilisation of cervical cancer screening services in the Vhembe District, South Africa. Most participants were aware of the cervical cancer services provided by other multidisciplinary health team members. Strategies to be used to encourage women to utilise cervical cancer screening services effectively needed the involvement of other multidisciplinary health team members. This would facilitate the use of multiple strategies since each member of the multidisciplinary team would interact with the patient in different ways. The key sources of information should include other women who are well-informed about cervical cancer or have been screened, leaders or members of women’s groups, midwives, PHCNs, traditional healers, community health workers, community leaders and doctors [22, 23]. These categories of people have an influence on how women perceive cervical cancer screening which reflects one of the tenets of the Health Belief Model (HBM) regarding behavioural change [24].
The majority of the participants did not view themselves as being vulnerable to cervical cancer (73.2%); this would influence their utilisation of cervical cancer screening services. The main elements of the HBM are that, in order for people to change behavior, people must feel personally vulnerable to a health threat, view the possible effects as severe, and see that taking serious action is likely to either prevent or reduce the health risk. When individuals perceive a threat as not serious or themselves as not vulnerable, they are unlikely to adopt mitigating behaviors [25]. In this study, although the majority of the participants were aware that a Pap smear could detect cervical cancer earlier (66.8%), others had contrary opinions or were uncertain. These categories of participants obviously lacked knowledge about cervical cancer and, as such, might not utilise cervical cancer screening services. Although 65.8% of the participants knew what a Pap smear test was, 34.2% did not understand a Pap smear and would feel reluctant to subject themselves to one. It, therefore, became clear that a lack of knowledge about Pap smears would impact negatively on the utilisation of cervical cancer screening [26].
The findings of this study revealed that most of the women were aware of the cervical cancer screening services provided at the five clinics (49.4%). This service location knowledge was encouraging and should be sustained by creating awareness. Knowledge of cervical cancer is important for early detection and subsequent treatment. Cervical cancer screening services could be utilized better if cervical cancer screening awareness campaigns were sustained and the services were accessible, affordable and available [20]. Previous findings revealed that women in this setting, lacked knowledge about cervical cancer and the prevention thereof, but displayed positive attitudes to the utilisation of cervical cancer screening services [27]. Women who did not know what a Pap smear was would not even know that with any gynecological complaints, such as, pain, bleeding, offensive discharges or loss of weight, a Pap smear would be required as part of the routine gynecological examination [28].
The study indicated that most women would not go for cervical cancer screening mostly because of fear of pain, embarrassment and a lack of facilities for screening. Feelings of fear that cervical cancer screening would result in discomfort, harm or pain, constituted a hindrance to the utilisation of cervical cancer screening services. Embarrassment and fear of pain, or the detection of cancer were barriers to the utilisation of cervical cancer screening services [11, 29-31]; furthermore, those feelings were worse if the woman did not have prior knowledge about cancer and screening.
Access to various modes of transport is an important matter for someone who is wanting to access cervical cancer screening services, especially in rural areas where the travel distances are great and access to alternative modes of transport is limited. This study found that transportation and geographical location impacted negatively on the utilisation of cervical cancer screening services, as some women had needed to travel more than five kilometres on moutainous roads to access cervical cancer screening. This scenario was not in accordance with the Batho Pele principles and Patients’ Rights Charter which prescribe that a patient should have access to health care, and that the acceptable distance should be less than five kilometres [32]. The long distances of more than five kilometres to a clinic show that the clinics are still too few and far between; that the National DoH’s prescribed clinic-distance is unattainable in this setting. This present study indicated that the communities stayed more than five kilometres from most clinics. Notably, the rugged and mountainous terrain in the setting was and is a big challenge when trying to access health facilities, which are far away from the people. This supports Ntekim’s findings [22] who indicated that high rates of invasive cervical cancer can be attributed to the difficulty of accessing cervical cancer screening services in most countries of Sub-Sahara Africa, because of the difficult-to-reach terrain associated with mountainous topography. Besides, in poor and developing countries, women did not avail themselves for cervical cancer screening [33] because of transportation problems [34] and distances to the clinics [35].
The finding that failure to use a condom increases the chances of cervical cancer, raised a concern about poor knowledge of cervical cancer. However, the majority of the participants considered cervical cancer as a serious health problem to be addressed. This thought might have originated from seeing patients experiencing pain and dying due to cancer. In a study conducted by Ndlovu et al. [30], a lack of sufficient knowledge was demonstrated by more than half (57%) of women who were not aware of the risk factors for cervical cancer. According to the HBM, knowledge about cancer-related matters is a structural variable which affects women’s perceptions of the seriousness of cervical cancer, whether it be a threat or not and whether it should be prevented or not [24]. This is confirmed by Kim et al. [36] who revealed that knowledge and low-risk perceptions of cervical cancer were the most important barriers to screening; these barriers discourage women from utilising cervical cancer screening services. In order to change the attitude of women, health messages should be formulated to address specific areas [27, 37].
Unlike women, men with higher levels of education demonstrated significantly greater knowledge about cervical cancer [38]. In this present study, men were not supportive of women’s partners attending Pap smear screening. According to Wright et al. [39], men should be involved in cervical cancer screening services in order to understand, motivate and support their women to utilise cervical cancer screening services. Cultural factors were identified as barriers to male involvement in female-orientated services [40]. The man as the head of the family is the main person whose support has more impact on whether cervical cancer screening is done or not, especially because cervical cancer screening affects the reproductive structures. The failure to support women may be because men lack specific knowledge: they are not included in health education relating to cervical cancer screening services. Some male partners do have an interest in reproductive health education and are willing to get more involved in their partner’s reproductive health care. Some are involved in family planning and antenatal care [41]. Male partners should be included in counseling before the women are screened. If women and men understood that treatment is offered during the same visit as screening, husbands would be more likely to accompany their wives for screening or to sign a form ahead of time that would permit cryotherapy, if needed [36]. Factors facilitating cancer treatment are social support from husbands, relatives, friends, the encouragement and role modelling of health workers and peers [36]. It is more effective to gain men’s co-operation prior to screening, by directing information, education, and advocacy at both men and women [36].
Financial constraints are major problems for women attending cervical cancer screening services. Women with lower socioeconomic status are less likely to go to clinics for cervical cancer screening because they do not have money for traveling to the nearest clinic. The situation exposes them to dying from conditions that could have been prevented or cured, if diagnosed earlier. More than 70% of all cancer deaths occurred in low- and middle-income countries [42]. Most women are poor, they do not have money to pay the costs. Although the PHC services, including screening services, are provided free in South Africa, women still fail to utilise these services. The poverty rate in this setting is rife. Most women in the Vhembe District are unemployed (18.6%) [21]; the unemployment rate is high, resulting in many families surviving on the monthly social grant money from the government and from their self-employment earnings through menial jobs. The situation is worsened by the fact that most of them are neither educated nor skilled. Poverty causes dependency [43]. Poverty could make men undecided about women going for cervical cancer screening. Sayem et al. [44] support this by indicating that economic dependency lessens the women’s power to be heard. This means that women have no power to decide for themselves as they do not have the means to decide where to seek health service.
In this study, the participants had heard about cancer from the clinics (49.4%) and radio (32.2%). Media and telephone communications could be used to reach as many women as possible [45, 46]. Online social networking site use has also been found to be convenient, effective and easily accessible [47].
The findings of the study revealed the availability of different groups in the community to perform cervical cancer services. Women who received information from multiple sources were more likely to present themselves for cervical cancer screening, irrespective of their ability to estimate whether cervical cancer was a problem sufficiently serious to be worthy of prevention and treatment or not [48]. However, such information should be presented in a non-stigmatising manner during health education in order to promote utilisation of cervical cancer screening services [49].
In this study, 31.0% participants were not aware of the HPV vaccination for girls. Vaccinations are one of the most commonly used public health strategies to reduce the risk of infection and minimise the prevalence of disease-causing agents (HPV) in the environment [50]. South Africa is one of the few low to middle-income countries in Africa that has introduced national HPV vaccines, in response to the WHO recommendation to include HPV vaccination in national immunisation programmes. Limited knowledge/awareness of the relationship between HPV and cervical cancer [45, 51-53] has been reported, even among healthcare workers [50]. The increasing rates of cervical cancer warrant a greater commitment to expanding cervical cancer screening and HPV vaccination of girls to prevent future cases [54].
Participants in this present study suggested the use of health education and cervical cancer campaigns as the main strategies to create cancer awareness and encourage women to attend cervical cancer screening services. Cervical screening campaign is most commonly used to reach people who stay far from clinics. However, there are limited educational campaigns and materials to raise awareness of the need to utilise cervical cancer screening services in the communities [55]. Health care services in the Vhembe District are still more inclined to offer curative rather than preventive health care services. Women present for screnning when they feel lower abdominal pains or when cervical cancer has already progressed to an advanced stage [55].
5.1. Limitations
This study was conducted in selected health clinics in the Vhembe District. Therefore, the sample may not be representative of the Limpopo Province nor South Africa. Also, given that the awareness and utilisation of the cervical cancer screening questionnaire were via self-reporting, the possibility of recall bias could not be overruled. Furthermore, only women who came to the clinic at the time of data collection were included in the study, which suggests a selection bias as women who did not attend the clinic during that period were excluded.
CONCLUSION AND RECOMMENDATIONS
Notwithstanding, the free availability of cervical cancer screening services in the Vhembe District, the awareness and utilisation of cervical cancer screening services in this setting are low. There is a need to intensify cervical screening campaigns among women, and/or to provide alternative means to make the cancer screening services far more accessible to the women in rural, difficult-to-reach regions. Also, it is important to include more languages on posters, and to teach midwives to do breast and cervical screening. There is an urgent need for different educational and organizational strategies to be used in order to improve the reproductive health of women [48]. Accessibility of screening services, including the provision of preventative and promotional health education to individuals, could be improved through planning and implementation of screening programmes involving community leaders and by designing culturally relevant messages [56].
AUTHORS’ CONTRIBUTIONS
Elisa Naledzani Vhuromu, Daniel Ter Goon, Maria Sonto Maputle and Rachel T Lebese contributed to the conceptualisation of the study and manuscript preparation. Elisa Naledzani Vhuromu contributed to the collection of data, Benedine Uchenna Okafor and Daniel Ter Goon contributed to data analysis and manuscript preparation. All authors read and approved the final manuscript before submission.
ETHICAL APPROVAL AND CONSENT TO PARTICIPATE
The University of Venda Ethics Committee granted ethical clearance for the study (Ref: SHS/14/PDC/02/1908). Permission to conduct the study was also obtained from the Limpopo Provincial Health Department and the Vhembe District Department of Health. Furthermore, permission was granted to access the facilities and utilise selected clinics and PHCNs.
HUMAN AND ANIMAL RIGHTS
No animals/ humans were used for the studies that are bases of this research.
CONSENT FOR PUBLICATION
Informed consent was obtained from the participants, prior to data collection.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


